User login
The four questions you should ask about sexual health
This transcript has been edited for clarity.
When I went to med school, we were taught to take a sexual history. Do you smoke? Do you drink? Do you do drugs? Do you have sex? Men, women, or both? And that was it. We’re telling patients that sex is a vice, something that is dangerous and that you should feel bad about. But sex is how we’re all here and how we even continue as a species. We must get comfortable as doctors talking to our patients about sexual medicine.
What if we move away from sex being in the vice category – the part of the social history that’s the bad stuff you shouldn’t be doing? Maybe we should bring it into the review of systems.
As a very basic first step, I like to ask patients four things. As a sexual medicine doctor, I deal with these four things: libido, arousal, orgasm, and pain.
Why are these important? These are the things our patients really care about; 2.3 of every 1,000 people got divorced in 2021.
Libido. Women who have distressing low sexual desire have sex on average two and a half times per month. We call this mercy sex or duty sex. I don’t know what the half time per month looks like, but people genuinely care about desire and their doctors don’t really know that.
We have a biopsychosocial toolbox to help our patients. Let me give you an example: Antidepressants can have sexual side effects. Could there be medications in our toolbox that can help our patients? Of course there can, and there are. What about education or talk therapy? We should be asking our patients what they care about and why they care about it so we can help them achieve their quality-of-life goals.
Arousal. What about arousal? Did you know that erections are a marker of cardiovascular disease in men? We know this to be true for men, and I’m certain the research would be no different for women. We know that there are many biological causes for decrease in arousal, including sleep apnea, diabetes, hypertension, and smoking. I can convince a lot of men to quit smoking because I tell them it’s bad for their penis. We have to understand what our patients care about and then advise them on why we think we can help improve these issues.
Orgasm. How about orgasm? Have you ever been asked whether you can orgasm? Have you ever been asked whether you have questions about orgasm? About 15%-20% of women report having an orgasm disorder, and we rarely talk about this in an exam room. I’ve certainly never been asked, and everybody knows what I do for a living. Not to mention all the men that I and my colleagues see who have really distressing premature ejaculation or delayed orgasm. This is pathophysiology at its finest and most complex. It is so interesting, and we have so much to learn and understand about orgasm in general.
Pain. Finally, ask about pain. It seems obvious that we should be asking our patients about their pain, which includes pelvic pain, but oftentimes we avoid talking about private parts. Pain affects not just our patients, but also their partners and their families, when our patients can’t sit without discomfort, if they can’t go and perform the daily activities that bring them joy and belonging. We have to really work with our toolbox in a biopsychosocial manner to help our patients. I often use the incredible rehabilitation specialists called pelvic floor physical therapists.
Remember, we’re talking about libido, arousal, orgasm, and pain. Sex is important to us as a species. It’s important to our patients. Ask nonjudgmental and open-ended questions. You actually may be the only doctor to ever do so.
Dr. Rubin is an assistant clinical professor, department of urology, Georgetown University, Washington. She reported conflicts of interest with Sprout, Maternal Medical, Absorption Pharmaceuticals, GSK, and Endo.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
When I went to med school, we were taught to take a sexual history. Do you smoke? Do you drink? Do you do drugs? Do you have sex? Men, women, or both? And that was it. We’re telling patients that sex is a vice, something that is dangerous and that you should feel bad about. But sex is how we’re all here and how we even continue as a species. We must get comfortable as doctors talking to our patients about sexual medicine.
What if we move away from sex being in the vice category – the part of the social history that’s the bad stuff you shouldn’t be doing? Maybe we should bring it into the review of systems.
As a very basic first step, I like to ask patients four things. As a sexual medicine doctor, I deal with these four things: libido, arousal, orgasm, and pain.
Why are these important? These are the things our patients really care about; 2.3 of every 1,000 people got divorced in 2021.
Libido. Women who have distressing low sexual desire have sex on average two and a half times per month. We call this mercy sex or duty sex. I don’t know what the half time per month looks like, but people genuinely care about desire and their doctors don’t really know that.
We have a biopsychosocial toolbox to help our patients. Let me give you an example: Antidepressants can have sexual side effects. Could there be medications in our toolbox that can help our patients? Of course there can, and there are. What about education or talk therapy? We should be asking our patients what they care about and why they care about it so we can help them achieve their quality-of-life goals.
Arousal. What about arousal? Did you know that erections are a marker of cardiovascular disease in men? We know this to be true for men, and I’m certain the research would be no different for women. We know that there are many biological causes for decrease in arousal, including sleep apnea, diabetes, hypertension, and smoking. I can convince a lot of men to quit smoking because I tell them it’s bad for their penis. We have to understand what our patients care about and then advise them on why we think we can help improve these issues.
Orgasm. How about orgasm? Have you ever been asked whether you can orgasm? Have you ever been asked whether you have questions about orgasm? About 15%-20% of women report having an orgasm disorder, and we rarely talk about this in an exam room. I’ve certainly never been asked, and everybody knows what I do for a living. Not to mention all the men that I and my colleagues see who have really distressing premature ejaculation or delayed orgasm. This is pathophysiology at its finest and most complex. It is so interesting, and we have so much to learn and understand about orgasm in general.
Pain. Finally, ask about pain. It seems obvious that we should be asking our patients about their pain, which includes pelvic pain, but oftentimes we avoid talking about private parts. Pain affects not just our patients, but also their partners and their families, when our patients can’t sit without discomfort, if they can’t go and perform the daily activities that bring them joy and belonging. We have to really work with our toolbox in a biopsychosocial manner to help our patients. I often use the incredible rehabilitation specialists called pelvic floor physical therapists.
Remember, we’re talking about libido, arousal, orgasm, and pain. Sex is important to us as a species. It’s important to our patients. Ask nonjudgmental and open-ended questions. You actually may be the only doctor to ever do so.
Dr. Rubin is an assistant clinical professor, department of urology, Georgetown University, Washington. She reported conflicts of interest with Sprout, Maternal Medical, Absorption Pharmaceuticals, GSK, and Endo.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
When I went to med school, we were taught to take a sexual history. Do you smoke? Do you drink? Do you do drugs? Do you have sex? Men, women, or both? And that was it. We’re telling patients that sex is a vice, something that is dangerous and that you should feel bad about. But sex is how we’re all here and how we even continue as a species. We must get comfortable as doctors talking to our patients about sexual medicine.
What if we move away from sex being in the vice category – the part of the social history that’s the bad stuff you shouldn’t be doing? Maybe we should bring it into the review of systems.
As a very basic first step, I like to ask patients four things. As a sexual medicine doctor, I deal with these four things: libido, arousal, orgasm, and pain.
Why are these important? These are the things our patients really care about; 2.3 of every 1,000 people got divorced in 2021.
Libido. Women who have distressing low sexual desire have sex on average two and a half times per month. We call this mercy sex or duty sex. I don’t know what the half time per month looks like, but people genuinely care about desire and their doctors don’t really know that.
We have a biopsychosocial toolbox to help our patients. Let me give you an example: Antidepressants can have sexual side effects. Could there be medications in our toolbox that can help our patients? Of course there can, and there are. What about education or talk therapy? We should be asking our patients what they care about and why they care about it so we can help them achieve their quality-of-life goals.
Arousal. What about arousal? Did you know that erections are a marker of cardiovascular disease in men? We know this to be true for men, and I’m certain the research would be no different for women. We know that there are many biological causes for decrease in arousal, including sleep apnea, diabetes, hypertension, and smoking. I can convince a lot of men to quit smoking because I tell them it’s bad for their penis. We have to understand what our patients care about and then advise them on why we think we can help improve these issues.
Orgasm. How about orgasm? Have you ever been asked whether you can orgasm? Have you ever been asked whether you have questions about orgasm? About 15%-20% of women report having an orgasm disorder, and we rarely talk about this in an exam room. I’ve certainly never been asked, and everybody knows what I do for a living. Not to mention all the men that I and my colleagues see who have really distressing premature ejaculation or delayed orgasm. This is pathophysiology at its finest and most complex. It is so interesting, and we have so much to learn and understand about orgasm in general.
Pain. Finally, ask about pain. It seems obvious that we should be asking our patients about their pain, which includes pelvic pain, but oftentimes we avoid talking about private parts. Pain affects not just our patients, but also their partners and their families, when our patients can’t sit without discomfort, if they can’t go and perform the daily activities that bring them joy and belonging. We have to really work with our toolbox in a biopsychosocial manner to help our patients. I often use the incredible rehabilitation specialists called pelvic floor physical therapists.
Remember, we’re talking about libido, arousal, orgasm, and pain. Sex is important to us as a species. It’s important to our patients. Ask nonjudgmental and open-ended questions. You actually may be the only doctor to ever do so.
Dr. Rubin is an assistant clinical professor, department of urology, Georgetown University, Washington. She reported conflicts of interest with Sprout, Maternal Medical, Absorption Pharmaceuticals, GSK, and Endo.
A version of this article first appeared on Medscape.com.
An STI upsurge requires a nimble approach to care
Except for a drop in the number of sexually transmitted infections (STIs) early in the COVID-19 pandemic (March and April 2020), the incidence of STIs has been rising throughout this century.1 In 2018, 1 in 5 people in the United States had an STI; 26 million new cases were reported that year, resulting in direct costs of $16 billion—85% of which was for the care of HIV infection.2 Also that year, infection with Chlamydia trachomatis (chlamydia), Trichomonas vaginalis (trichomoniasis), herpesvirus type 2 (genital herpes), and/or human papillomavirus (condylomata acuminata) constituted 97.6% of all prevalent and 93.1% of all incident STIs.3 Almost half (45.5%) of new cases of STIs occur in people between the ages of 15 and 24 years.3
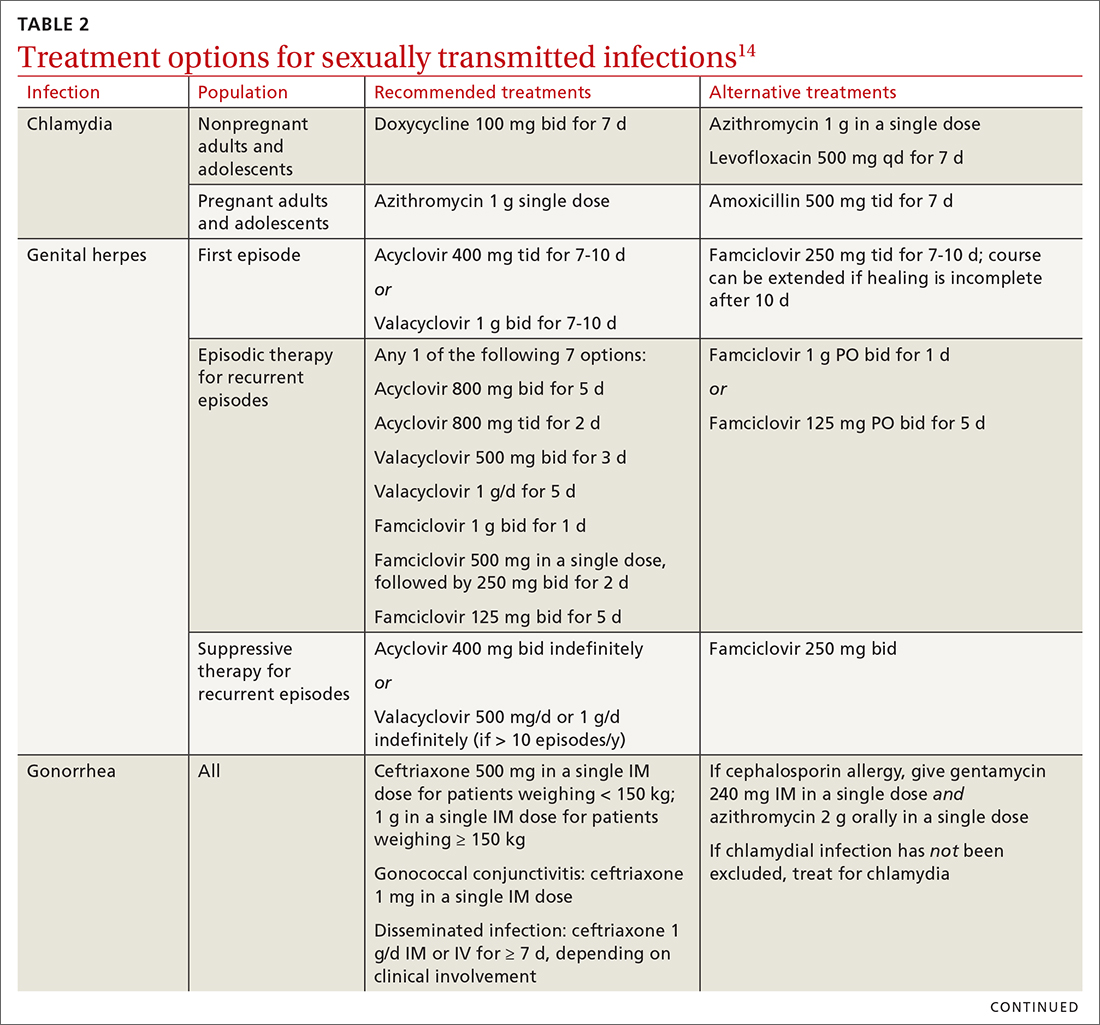
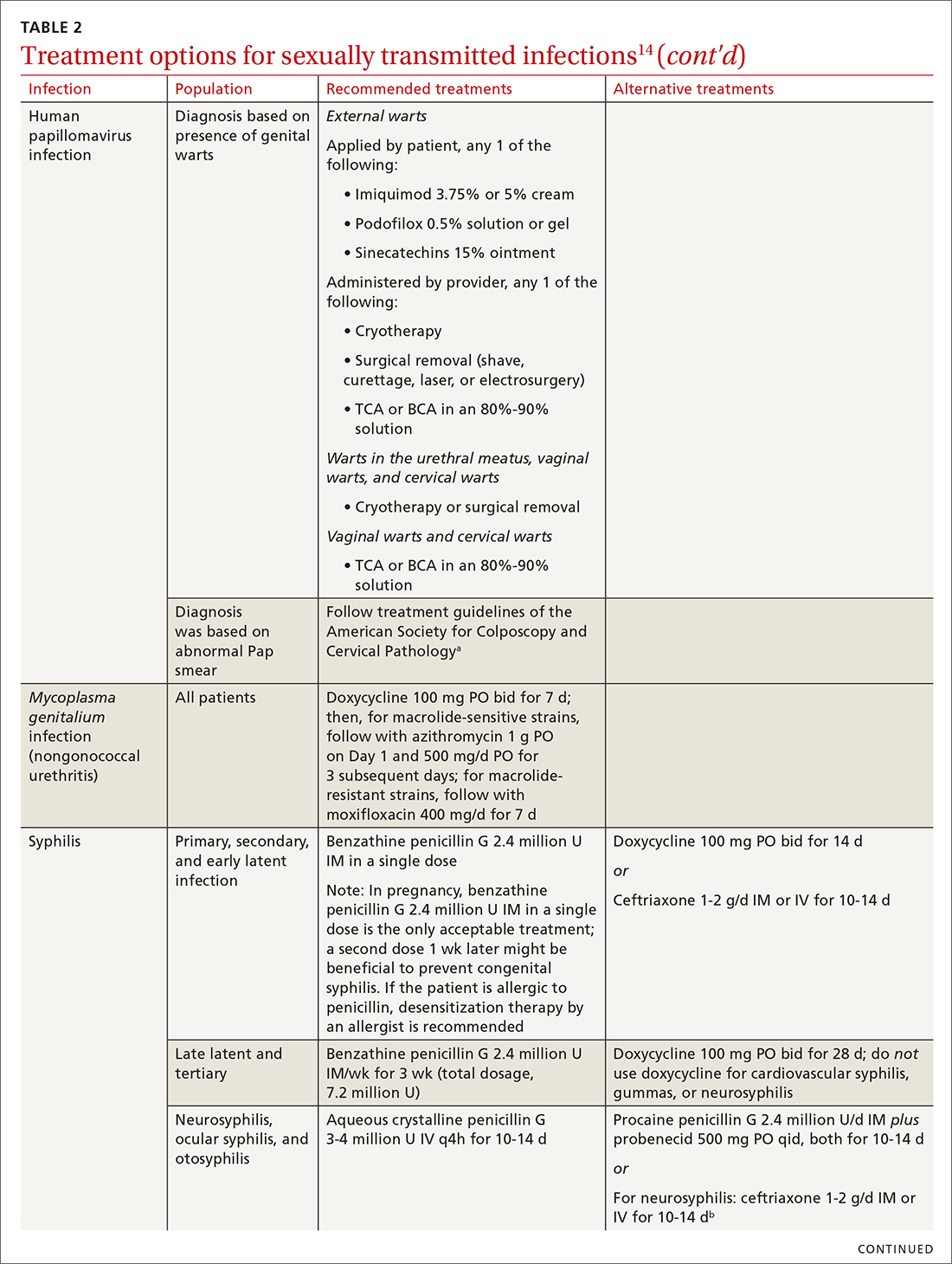
Three factors—changing social patterns, including the increase of social networking; the ability of antiviral therapy to decrease the spread of HIV, leading to a reduction in condom use; and increasing antibiotic resistance—have converged to force changes in screening and treatment recommendations. In this article, we summarize updated guidance for primary care clinicians from several sources—including the Centers for Disease Control and Prevention (CDC), the US Preventive Services Task Force (USPSTF), and the American Society for Colposcopy and Cervical Pathology (ASCCP)—on diagnosing STIs (TABLE 14-13) and providing guideline-based treatment (Table 214). Because of the breadth and complexity of HIV disease, it is not addressed here.

Chlamydia
Infection with Chlamydia trachomatis—the most commonly reported bacterial STI in the United States—primarily causes cervicitis in women and proctitis in men, and can cause urethritis and pharyngitis in men and women. Prevalence is highest in sexually active people younger than 24 years.15
Because most infected people are asymptomatic and show no signs of illness on physical exam, screening is recommended for all sexually active women younger than 25 years and all men who have sex with men (MSM).4 No studies have established proper screening intervals; a reasonable approach, therefore, is to repeat screening for patients who have a sexual history that confers a new or persistent risk for infection since their last negative result.
Depending on the location of the infection, symptoms of chlamydia can include vaginal or penile irritation or discharge, dysuria, pelvic or rectal pain, and sore throat. Breakthrough bleeding in a patient who is taking an oral contraceptive should raise suspicion for chlamydia.
Untreated chlamydia can lead to pelvic inflammatory disease (PID), tubo-ovarian abscess, tubal factor infertility, ectopic pregnancy, and chronic pelvic pain. Infection can be transmitted vertically (mother to baby) antenatally, which can cause ophthalmia neonatorum and pneumonia in these newborns.
Diagnosis. The diagnosis of chlamydia is made using nucleic acid amplification testing (NAAT). Specimens can be collected by the clinician or the patient (self collected) using a vaginal, rectal, or oropharyngeal swab, or a combination of these, and can be obtained from urine or liquid-based cytology material.16
Continue to: Treatment
Treatment. Recommendations for treating chlamydia were updated by the CDC in its 2021 treatment guidelines (Table 214). Doxycycline 100 mg bid for 7 days is the preferred regimen; alternative regiments are (1) azithromycin 1 g in a single dose and (2) levofloxacin 500 mg daily for 7 days.4 A meta-analysis17 and a Cochrane review18 showed that the rate of treatment failure was higher among men when they were treated with azithromycin instead of doxycycline; furthermore, a randomized controlled trial demonstrated that doxycycline is more effective than azithromycin (cure rate, 100%, compared to 74%) at treating rectal chlamydia in MSM.19
Azithromycin is efficacious for urogenital infection in women; however, there is concern that the 33% to 83% of women who have concomitant rectal infection (despite reporting no receptive anorectal sexual activity) would be insufficiently treated. Outside pregnancy, the CDC does not recommend a test of cure but does recommend follow-up testing for reinfection in 3 months. Patients should abstain from sexual activity until 7 days after all sexual partners have been treated.
Expedited partner therapy (EPT) is the practice of treating sexual partners of patients with known chlamydia (and patients with gonococcal infection). Unless prohibited by law in your state, offer EPT to patients with chlamydia if they cannot ensure that their sexual partners from the past 60 days will seek timely treatment.a
Evidence to support EPT comes from 3 US clinical trials, whose subjects comprised heterosexual men and women with chlamydia or gonorrhea.21-23 The role of EPT for MSM is unclear; data are limited. Shared decision-making is recommended to determine whether EPT should be provided, to ensure that co-infection with other bacterial STIs (eg, syphilis) or HIV is not missed.24-26
a Visit www.cdc.gov/std/ept to read updated information about laws and regulations regarding EPT in your state.20
Gonorrhea
Gonorrhea is the second most-reported bacterial communicable disease.5 Infection with Neisseria gonorrhoeae causes urethral discharge in men, leading them to seek treatment; infected women, however, are often asymptomatic. Infected men and women might not recognize symptoms until they have transmitted the disease. Women have a slower natural clearance of gonococcal infection, which might explain their higher prevalence.27 Delayed recognition of symptoms can result in complications, including PID.5
Diagnosis. Specimens for NAAT can be obtained from urine, endocervical, vaginal, rectal, pharyngeal, and male urethral specimens. Reported sexual behaviors and exposures of women and transgender or gender-diverse people should be taken into consideration to determine whether rectal or pharyngeal testing, or both, should be performed.28 MSM should be screened annually at sites of contact, including the urethra, rectum, and pharynx.28 All patients with urogenital or rectal gonorrhea should be asked about oral sexual exposure; if reported, pharyngeal testing should be performed.5
NAAT of urine is at least as sensitive as testing of an endocervical specimen; the same specimen can be used to test for chlamydia and gonorrhea. Patient-collected specimens are a reasonable alternative to clinician-collected swab specimens.29
Continue to: Treatment
Treatment is complicated by the ability of gonorrhea to develop resistance. Intramuscular ceftriaxone 500 mg in a single dose cures 98% to 99% of infections in the United States; however, monitoring local resistance patterns in the community is an important component of treatment.28 (See Table 214 for an alternative regimen for cephalosporin-allergic patients and for treating gonococcal conjunctivitis and disseminated infection.)
In 2007, the CDC identified widespread quinolone-resistant gonococcal strains; therefore, fluoroquinolones no longer are recommended for treating gonorrhea.30 Cefixime has demonstrated only limited success in treating pharyngeal gonorrhea and does not attain a bactericidal level as high as ceftriaxone does; cefixime therefore is recommended only if ceftriaxone is unavailable.28 The national Gonococcal Isolate Surveillance Project is finding emerging evidence of the reduced susceptibility of N gonorrhoeae to azithromycin—making dual therapy for gonococcal infection no longer a recommendation.28
Patients should abstain from sex until 7 days after all sex partners have been treated for gonorrhea. As with chlamydia, the CDC does not recommend a test of cure for uncomplicated urogenital or rectal gonorrhea unless the patient is pregnant, but does recommend testing for reinfection 3 months after treatment.14 For patients with pharyngeal gonorrhea, a test of cure is recommended 7 to 14 days after initial treatment, due to challenges in treatment and because this site of infection is a potential source of antibiotic resistance.28
Trichomoniasis
T vaginalis, the most common nonviral STI worldwide,31 can manifest as a yellow-green vaginal discharge with or without vaginal discomfort, dysuria, epididymitis, and prostatitis; most cases, however, are asymptomatic. On examination, the cervix might be erythematous with punctate lesions (known as strawberry cervix).
Unlike most STIs, trichomoniasis is as common in women older than 24 years as it is in younger women. Infection is associated with a lower educational level, lower socioeconomic status, and having ≥ 2 sexual partners in the past year.32 Prevalence is approximately 10 times as high in Black women as it is in White women.
T vaginalis infection is associated with an increase in the risk for preterm birth, premature rupture of membranes, cervical cancer, and HIV infection. With a lack of high-quality clinical trials on the efficacy of screening, women with HIV are the only group for whom routine screening is recommended.6
Diagnosis. NAAT for trichomoniasis is now available in conjunction with gonorrhea and chlamydia testing of specimens on vaginal or urethral swabs and of urine specimens and liquid Pap smears.
Continue to: Treatment
Treatment. Because of greater efficacy, the treatment recommendation for women has changed from a single 2-g dose of oral metronidazole to 500 mg twice daily for 7 days. The 2-g single oral dose is still recommended for men7 (Table 214 lists alternative regimens).
Mycoplasma genitalium
Infection with M genitalium is common and often asymptomatic. The disease causes approximately 20% of all cases of nongonococcal and nonchlamydial urethritis in men and about 40% of persistent or recurrent infections. M genitalium is present in approximately 20% of women with cervicitis and has been associated with PID, preterm delivery, spontaneous abortion, and infertility.
There are limited and conflicting data regarding outcomes in infected patients other than those with persistent or recurrent infection; furthermore, resistance to azithromycin is increasing rapidly, resulting in an increase in treatment failures. Screening therefore is not recommended, and testing is recommended only in men with nongonococcal urethritis.33,34
Diagnosis. NAAT can be performed on urine or on a urethral, penile meatal, endocervical, or vaginal swab; men with recurrent urethritis or women with recurrent cervicitis should be tested. NAAT also can be considered in women with PID. Testing the specimen for the microorganism’s resistance to macrolide antibiotics is recommended (if such testing is available).
Treatment is initiated with doxycycline 100 mg twice daily for 7 days. If the organism is macrolide sensitive, follow with azithromycin 1 g orally on Day 1, then 500 mg/d for 3 more days. If the organism is macrolide resistant or testing is unavailable, follow doxycycline with oral moxifloxacin 400 mg/d for 7 days.33
Genital herpes (mostly herpesvirus type 2)
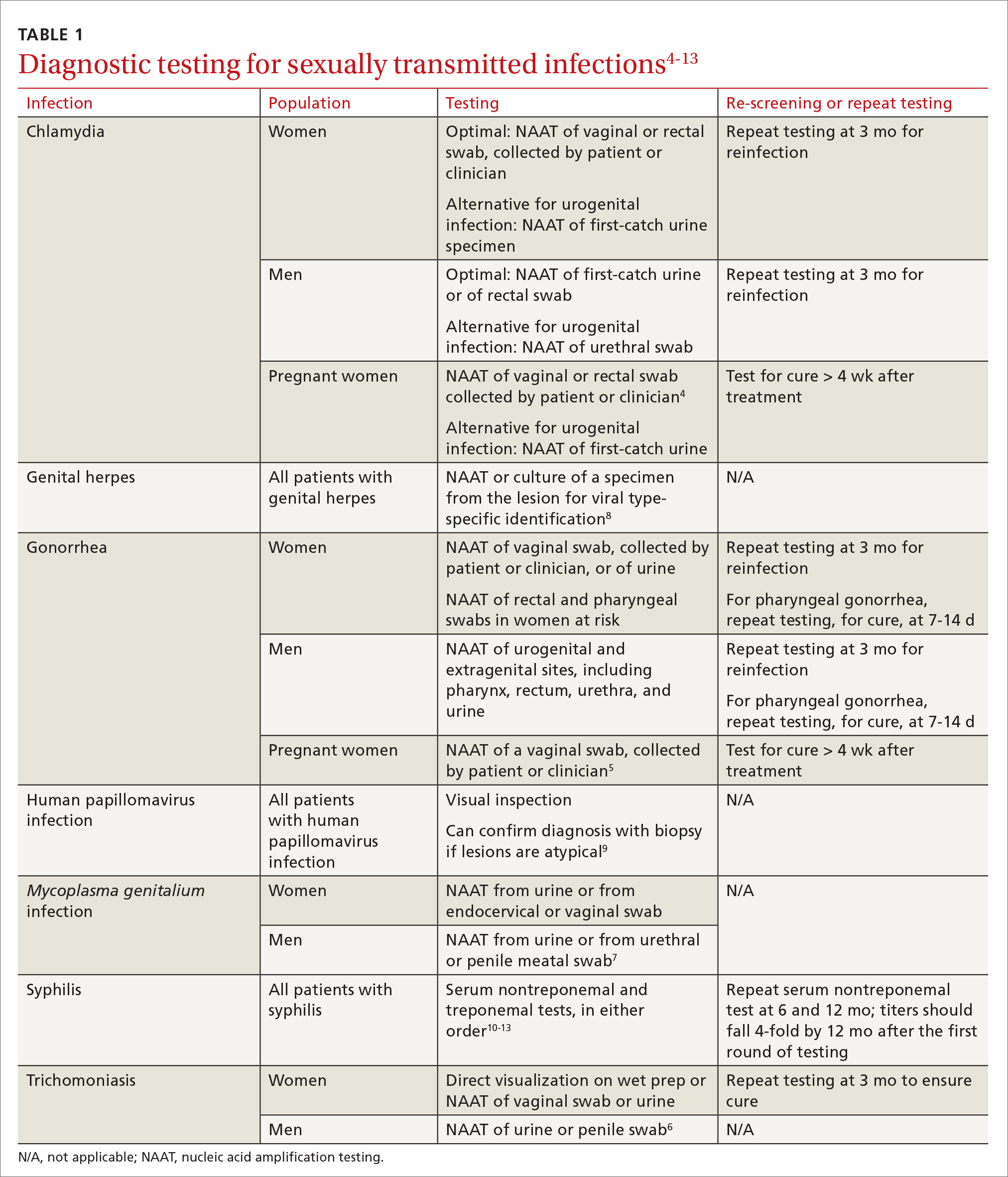
Genital herpes, characterized by painful, recurrent outbreaks of genital and anal lesions,35 is a lifelong infection that increases in prevalence with age.8 Because many infected people have disease that is undiagnosed or mild or have unrecognizable symptoms during viral shedding, most genital herpes infections are transmitted by people who are unaware that they are contagious.36 Herpesvirus type 2 (HSV-2) causes most cases of genital herpes, although an increasing percentage of cases are attributed to HSV type 1 (HSV-1) through receptive oral sex from a person who has an oral HSV-1 lesion.
Importantly, HSV-2–infected people are 2 to 3 times more likely to become infected with HIV than people who are not HSV-2 infected.37 This is becauseCD4+ T cells concentrate at the site of HSV lesions and express a higher level of cell-surface receptors that HIV uses to enter cells. HIV replicates 3 to 5 times more quickly in HSV-infected tissue.38
Continue to: HSV can become disseminated...
HSV can become disseminated, particularly in immunosuppressed people, and can manifest as encephalitis, hepatitis, and pneumonitis. Beyond its significant burden on health, HSV carries significant psychosocial consequences.9
Diagnosis. Clinical diagnosis can be challenging if classic lesions are absent at evaluation. If genital lesions are present, HSV can be identified by NAAT or culture of a specimen of those lesions. False-negative antibody results might be more frequent in early stages of infection; repeating antibody testing 12 weeks after presumed time of acquisition might therefore be indicated, based on clinical judgment. HSV-2 antibody positivity implies anogenital infection because almost all HSV-2 infections are sexually acquired.
HSV-1 antibody positivity alone is more difficult to interpret because this finding does not distinguish between oral and genital lesions, and most HSV-1 seropositivity is acquired during childhood.36 HSV polymerase chain reaction (PCR) testing of blood should not be performed to diagnose genital herpes infection, except in settings in which there is concern about disseminated infection.
Treatment. Management should address the acute episode and the chronic nature of genital herpes. Antivirals will not eradicate latent
- attenuate current infection
- prevent recurrence
- improve quality of life
- suppress the virus to prevent transmission to sexual partners.
All patients experiencing an initial episode of genital herpes should be treated, regardless of symptoms, due to the potential for prolonged or severe symptoms during recurrent episodes.9 Three drugs—acyclovir, valacyclovir, and famciclovir—are approved by the US Food and Drug Administration (FDA) to treat genital herpes and appear equally effective (TABLE 214).
Antiviral therapy for recurrent genital HSV infection can be administered either as suppressive therapy to reduce the frequency of recurrences or episodically to shorten the duration of lesions:
- Suppressive therapy reduces the frequency of recurrence by 70% to 80% among patients with frequent outbreaks. Long-term safety and efficacy are well established.
- Episodic therapy is most effective if started within 1 day after onset of lesions or during the prodrome.36
There is no specific recommendation for when to choose suppressive over episodic therapy; most patients prefer suppressive therapy because it improves quality of life. Use shared clinical decision-making to determine the best option for an individual patient.
Continue to: Human papillomavirus
Human papillomavirus
Condylomata acuminata (genital warts) are caused by human papillomavirus (HPV), most commonly types 6 and 11, which manifest as soft papules or plaques on the external genitalia, perineum, perianal skin, and groin. The warts are usually asymptomatic but can be painful or pruritic, depending on size and location.
Diagnosis is made by visual inspection and can be confirmed by biopsy if lesions are atypical. Lesions can resolve spontaneously, remain unchanged, or grow in size or number.
Treatment. The aim of treatment is relief of symptoms and removal of warts. Treatment does not eradicate HPV infection. Multiple treatments are available that can be applied by the patient as a cream, gel, or ointment or administered by the provider, including cryotherapy, surgical removal, and solutions. The decision on how to treat should be based on the number, size, and
HPV-associated cancers and precancers. This is a broad (and separate) topic. HPV types 16 and 18 cause most cases of cervical, penile, vulvar, vaginal, anal, and oropharyngeal cancer and precancer.39 The USPSTF, the American Cancer Society, and the American College of Obstetricians and Gynecologists all have recommendations for cervical cancer screening in the United States.40 Refer to guidelines of the ASCCP for recommendations on abnormal screening tests.41
Prevention of genital warts. The 9-valent HPV vaccine available in the United States is safe and effective and helps protect against viral types 6, 11, 16, 18, 31, 33, 45, 52, and 58. Types 6 and 11 are the principal causes of genital warts. Types 16 and 18 cause 66% of cervical cancer. The vaccination series can be started at age 9 years and is recommended for everyone through age 26 years. Only 2 doses are needed if the first dose is given prior to age 15 years; given after that age, a 3-dose series is utilized. Refer to CDC vaccine guidelines42 for details on the exact timing of vaccination.
Vaccination for women ages 27 to 45 years is not universally recommended because most people have been exposed to HPV by that age. However, the vaccine can still be administered, depending on clinical circumstances and the risk for new infection.42
Syphilis
Caused by the spirochete Treponema pallidum, syphilis manifests across a spectrum—from congenital to tertiary. The inability of medical science to develop a method for culturing the spirochete has confounded diagnosis and treatment.
Continue to: Since reaching a historic...
Since reaching a historic nadir of incidence in 2000 (5979 cases in the United States), there has been an increasingly rapid rise in that number: to 130,000 in 2020. More than 50% of cases are in MSM; however, the number of cases in heterosexual women is rapidly increasing.43
Routine screening for syphilis should be performed in any person who is at risk: all pregnant women in the first trimester (and in the third trimester and at delivery if they are at risk or live in a community where prevalence is high) and annually in sexually active MSM or anyone with HIV infection.10
Diagnosis. Examination by dark-field microscopy, testing by PCR, and direct fluorescent antibody assay for T pallidum from lesion tissue or exudate provide definitive diagnosis for early and congenital syphilis, but are often unavailable.
Presumptive diagnosis requires 2 serologic tests:
- Nontreponemal tests (the VDRL and rapid plasma reagin tests) identify anticardiolipin antibodies released during syphilis infection, although results also can be elevated in autoimmune disease or after certain immunizations, including the COVID-19 vaccine.
- Treponemal tests (the fluorescent treponemal antibody absorbed assay, T pallidum particulate agglutination assay, enzyme immunoassay, and chemiluminescence immunoassay) are specific antibody tests.
Historically, reactive nontreponemal tests, which are less expensive and easier to perform, were followed by a treponemal test to confirm the presumptive diagnosis. This method continues to be reasonable when screening patients in a low-prevalence population.11 The reverse sequence screening algorithm (ie, begin with a treponemal test) is now frequently used. With this method, a positive treponemal test must be confirmed with a nontreponemal test. If the treponemal test is positive and the nontreponemal test is negative, another treponemal test must be positive to confirm the diagnosis. This algorithm is useful in high-risk populations because it provides earlier detection of recently acquired syphilis and enhanced detection of late latent syphilis.12,13,44 The CDC has not stated a diagnostic preference.
Once the diagnosis is made, a complete history (including a sexual history and a history of syphilis testing and treatment) and a physical exam are necessary to confirm stage of disease.45
Special circumstances. Neurosyphilis, ocular syphilis, and otosyphilis refer to the site of infection and can occur at any stage of disease. The nervous system usually is infected within hours of initial infection, but symptoms might take weeks or years to develop—or might never manifest. Any time a patient develops neurologic, ophthalmologic, or audiologic symptoms, careful neurologic and ophthalmologic evaluation should be performed and the patient should be tested for HIV.
Continue to: Lumbar puncture is warranted...
Lumbar puncture is warranted for evaluation of cerebrospinal fluid if neurologic symptoms are present but is not necessary for isolated ocular syphilis or otosyphilis without neurologic findings. Treatment should not be delayed for test results if ocular syphilis is suspected because permanent blindness can develop. Any patient at high risk for an STI who presents with neurologic or ophthalmologic symptoms should be tested for syphilis and HIV.45
Pregnant women who have a diagnosis of syphilis should be treated with penicillin immediately because treatment ≥ 30 days prior to delivery is likely to prevent most cases of congenital syphilis. However, a course of penicillin might not prevent stillbirth or congenital syphilis in a gravely infected fetus, evidenced by fetal syphilis on a sonogram at the time of treatment. Additional doses of penicillin in pregnant women with early syphilis might be indicated if there is evidence of fetal syphilis on ultrasonography. All women who deliver a stillborn infant (≥ 20 weeks’ gestation) should be tested for syphilis at delivery.46
All patients in whom primary or secondary syphilis has been diagnosed should be tested for HIV at the time of diagnosis and treatment; if the result is negative, they should be offered preexposure prophylaxis (PrEP; discussed shortly). If the incidence of HIV in your community is high, repeat testing for HIV in 3 months. Clinical and serologic evaluation should be performed 6 and 12 months after treatment.47
Treatment. Penicillin remains the standard treatment for syphilis. Primary, secondary, and early tertiary stages (including in pregnancy) are treated with benzathine penicillin G 2.4 million units intramuscular (IM) in a single dose. For pregnant patients, repeating that dose in 1 week generally is recommended. Patients in the late latent (> 1 year) or tertiary stage receive the same dose of penicillin, which is then repeated weekly, for a total of 3 doses. Doxycycline and ceftriaxone are alternatives, except in pregnancy.
Warn patients of the Jarisch-Herxheimer reaction: fever, headache, and myalgias associated with initiation of treatment in the presence of the high bacterial load seen in early syphilis. Treatment is symptomatic, but the Jarisch-Herxheimer reaction can cause fetal distress in pregnancy.
Otosyphilis, ocular syphilis, and neurosyphilis require intravenous (IV) aqueous crystalline penicillin G 3 to 4 million U every 4 hours for 10 to 14 days.45 Alternatively, procaine penicillin G 2.4 million U/d IM can be given daily with oral probenecid 500 mg qid, both for 10 to 14 days (TABLE 214).
Screening andprevention of STIs
Screening recommendations
Follow USPSTF screening guidelines for STIs.10,48-54 Screen annually for:
- gonorrhea and chlamydia in women ages 15 to 24 years and in women older than 25 years if they are at increased risk
- gonorrhea, chlamydia, syphilis, and HIV in MSM, and hepatitis C if they are HIV positive
- trichomoniasis in women who are HIV positive.
Continue to: Consider the community in which...
Consider the community in which you practice when determining risk; you might want to consult local public health authorities for information about local epidemiology and guidance on determining which of your patients are at increased risk.
Preexposure prophylaxis
According to the CDC, all sexually active adults and adolescents should be informed about the availability of PrEP to prevent HIV infection. PrEP should be (1) available to anyone who requests it and (2) recommended for anyone who is sexually active and who practices sexual behaviors that place them at substantial risk for exposure to or acquisition of HIV, or both.
The recommended treatment protocol for men and women who have either an HIV-positive partner or inconsistent condom use or who have had a bacterial STI in the previous 6 months is oral emtricitabine 200 mg plus tenofovir disoproxil fumarate 300 mg/d (sold as Truvada-F/TDF). Men and transgender women (ie, assigned male at birth) with at-risk behaviors also can use emtricitabine plus tenofovir alafenamide 25 mg/d (sold as Descovy-F/TAF).
In addition, cabotegravir plus rilpirivine (sold as Cabenuva), IM every 2 months, was approved by the FDA for PrEP in 2021.
Creatinine clearance should be assessed at baseline and yearly (every 6 months for those older than 50 years) in patients taking PrEP. All patients must be tested for HIV at initiation of treatment and every 3 months thereafter (every 4 months for cabotegravir plus rilpirivine). Patients should be screened for bacterial STIs every 6 months (every 3 months for MSM and transgender women); screening for chlamydia should be done yearly. For patients being treated with emtricitabine plus tenofovir alafenamide, weight and a lipid profile (cholesterol and triglycerides) should be assessed annually.55
Postexposure prophylaxis
The sharp rise in the incidence of STIs in the past few years has brought renewed interest in postexposure prophylaxis (PEP) for STIs. Although PEP should be standard in cases of sexual assault, this protocol also can be considered in other instances of high-risk exposure.
CDC recommendations for PEP in cases of assault are56:
- ceftriaxone 500 mg IM in a single dose (1 g if weight is ≥ 150 kg) plus
- doxycycline 100 mg bid for 7 days plus
- metronidazole 2 g bid for 7 days (for vaginal exposure)
- pregnancy evaluation and emergency contraception
- hepatitis B risk evaluation and vaccination, with or without hepatitis B immune globulin
- HIV risk evaluation, based on CDC guidelines, and possible HIV prophylaxis (PrEP)
- HPV vaccination for patients ages 9 to 26 years if they are not already fully vaccinated.
CORRESPONDENCE
Belinda Vail, MD, 3901 Rainbow Boulevard, Mail Stop 4010, Kansas City, KS 66160; bvail@kumc.edu
1. Pagaoa M, Grey J, Torrone E, et al. Trends in nationally notifiable sexually transmitted disease case reports during the US COVID-19 pandemic, January to December 2020. Sex Transm Dis. 2021;48:798-804. doi: 10.1097/OLQ.0000000000001506
2. Chesson HW, Spicknall IH; Bingham A, et al. The estimated direct lifetime medical costs of sexually transmitted infections acquired in the United States in 2018. Sex Transm Dis. 2021;48:215-221. doi: 10.1097/OLQ.0000000000001380
3. Kreisel KM, Spicknall IH, Gargano JW, et al. Sexually transmitted infections among US women and men: prevalence and incidence estimates, 2018. Sex Transm Dis. 2021;48:208-214. doi: 10.1097/OLQ.0000000000001355
4. CDC. Sexually transmitted infections treatment guidelines, 2021: Chlamydial infections among adolescents and adults. US Department of Health and Human Services. July 21, 2021. Accessed April 19, 2023. www.cdc.gov/std/treatment-guidelines/chlamydia.htm
5. CDC. Sexually transmitted infections treatment guidelines, 2021: Gonococcal infections among adolescents and adults. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/gonorrhea-adults.htm
6. Van Gerwen OT, Muzny CA. Recent advances in the epidemiology, diagnosis, and management of Trichomonas vaginalis infection. F1000Res. 2019;
7. CDC. Sexually transmitted infections treatment guidelines, 2021. Trichomoniasis. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. December 27, 2021. www.cdc.gov/std/treatment-guidelines/trichomoniasis.htm
8. Spicknall IH, Flagg EW, Torrone EA. Estimates of the prevalence and incidence of genital herpes, United States, 2018. Sex Transm Dis. 2021;48:260-265. doi: 10.1097/OLQ.0000000000001375
9. Mark H, Gilbert L, Nanda J. Psychosocial well-being and quality of life among women newly diagnosed with genital herpes. J Obstet Gynecol Neonatal Nurs.
10. Bibbins-Domingo K, Grossman DC, Curry SJ, et al; US Preventive Services Task Force. Screening for syphilis infection in nonpregnant adults and adolescents: US Preventive Services Task Force recommendation statement. JAMA. 2016;315:2321-2327. doi: 10.1001/jama.2016.5824
11. Ricco J, Westby A. Syphilis: far from ancient history. Am Fam Physician. 2020;102:91-98.
12. Goza M, Kulwicki B, Akers JM, et al. Syphilis screening: a review of the Syphilis Health Check rapid immunochromatographic test. J Pharm Technol. 2017;33:53-59. doi:10.1177/8755122517691308
13. Henao- AF, Johnson SC. Diagnostic tests for syphilis: new tests and new algorithms. Neurol Clin Pract. 2014;4:114-122. doi: 10.1212/01.CPJ.0000435752.17621.48
14. Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021;70:1-187. doi:10.15585/mmwr.rr7004a1
15. CDC. Sexually Transmitted Disease Surveillance 2021. National overview of STDs. US Department of Health and Human Services. April 2023. Accessed May 9, 2023. www.cdc.gov/std/statistics/2021/overview.htm#Chlamydia
16. CDC. Recommendations for the laboratory-based detection of Chlamydia trachomatis and Neisseria gonorrhoeae—2014. MMWR Recomm Rep. 2014;63:1-19.
17. Kong FYS, Tabrizi SN, Law M, et al. Azithromycin versus doxycycline for the treatment of genital chlamydia infection: a meta-analysis of randomized controlled trials. Clin Infect Dis. 2014;59:193-205. doi: 10.1093/cid/ciu220
18. Páez-Canro C, Alzate JP, González LM, et al. Antibiotics for treating urogenital Chlamydia trachomatis infection in men and non-pregnant women. Cochrane Database Syst Rev. 2019;1:CD010871. doi: 10.1002/14651858.CD010871.pub2
19. Dombrowski JC, Wierzbicki MR, Newman LM, et al. Doxycycline versus azithromycin for the treatment of rectal chlamydia in men who have sex with men: a randomized controlled trial. Clin Infect Dis. 2021;73:824-831. doi: 10.1093/cid/ciab153
20. CDC. Sexually transmitted infections treatment guidelines, 2021: Expedited partner therapy. US Department of Health and Human Services. July 22, 2021. Accessed April 19, 2023. www.cdc.gov/std/treatment-guidelines/clinical-EPT.htm
21. Golden MR, Whittington WLH, Handsfield HH, et al. Effect of expedited treatment of sex partners on recurrent or persistent gonorrhea or chlamydial infection. N Engl J Med. 2005;352:676-685. doi: 10.1056/NEJMoa041681
22. Schillinger JA, Kissinger P, Calvet H, et al. Patient-delivered partner treatment with azithromycin to prevent repeated Chlamydia trachomatis infection among women: a randomized, controlled trial. Sex Transm Dis. 2003;30:49-56. doi: 10.1097/00007435-200301000-00011
23. Cameron ST, Glasier A, Scott G, et al. Novel interventions to reduce re-infection in women with chlamydia: a randomized controlled trial. Hum Reprod. 2009;24:888-895. doi: 10.1093/humrep/den475
24. McNulty A, Teh MF, Freedman E. Patient delivered partner therapy for chlamydial infection—what would be missed? Sex Transm Dis. 2008;35:834-836. doi: 10.1097/OLQ.0b013e3181761993
25. Stekler J, Bachmann L, Brotman RM, et al. Concurrent sexually transmitted infections (STIs) in sex partners of patients with selected STIs: implications for patient-delivered partner therapy. Clin Infect Dis. 2005;40:787-793. doi: 10.1086/428043
26. Schillinger JA, Kissinger P, Calvet H, et al. Patient-delivered partner treatment with azithromycin to prevent repeated Chlamydia trachomatis infection among women: a randomized, controlled trial. Sex Transm Dis. 2003;30:49-56. doi: 10.1097/00007435-200301000-00011
27. Stupiansky NW, Van der Pol B, Williams JA, et al. The natural history of incident gonococcal infection in adolescent women. Sex Transm Dis. 2011;38:750-754. doi: 10.1097/OLQ.0b013e31820ff9a4
28. CDC. Sexually transmitted infections treatment guidelines, 2021: Screening recommendations and considerations referenced in treatment guidelines and original sources. US Department of Health and Human Services. June 6, 2022. Accessed May 9, 2023. www.cdc.gov/std/treatment-guidelines/screening-recommen dations.htm
29. Cantor A, Dana T, Griffen JC, et al. Screening for chlamydial and gonococcal infections: a systematic review update for the US Preventive Services Task Force. Evidence Synthesis No. 206. AHRQ Report No. 21-05275-EF-1. Agency for Healthcare Research and Quality. September 2021. www.ncbi.nlm.nih.gov/books/NBK574045
30. CDC. Update to CDC’s sexually transmitted diseases treatment guidelines, 2006: fluoroquinolones no longer recommended for treatment of gonococcal infections. MMWR Morb Mortal Wkly Rep. 2007;56:332-336.
31. Rowley J, Vander Hoorn S, Korenromp E, et al. Chlamydia, gonorrhoea, trichomoniasis and syphilis: global prevalence and incidence estimates, 2016. Bull World Health Organ. 2019:97:548-562P. doi: 10.2471/BLT.18.228486
32. Patel EU, Gaydos CA, Packman ZR, et al. Prevalence and correlates of Trichomonas vaginalis infection among men and women in the United States. Clin Infect Dis. 2018;67:211-217. doi: 10.1093/cid/ciy079
33. CDC. Sexually transmitted infections treatment guidelines, 2021. Mycoplasma genitalium. US Department of Health and Human Services. July 22, 2021. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/mycoplasmagenitalium.htm
34. Manhart LE, Broad JM, Bolden MR. Mycoplasma genitalium: should we treat and how? Clin Infect Dis. 2011;53(suppl 3):S129-S142. doi:10.1093/cid/cir702.
35. Corey L, Wald A. Genital herpes. In: Holmes KK, Sparling PF, Stamm WE, et al, eds. Sexually Transmitted Diseases. 4th ed. McGraw-Hill; 2008:399-437.
36. CDC. Sexually transmitted infections treatment guidelines, 2021: Genital herpes. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/herpes.htm
37. Looker KJ, Elmes JAR, Gottlieb SL, et al. Effect of HSV-2 infection on subsequent HIV acquisition: an updated systematic review and meta-analysis. Lancet Infect Dis. 2017;17:1303-1316. doi: 10.1016/S1473-3099(17)30405-X
38. Rollenhagen C, Lathrop M, Macura SL, et al. Herpes simplex virus type-2 stimulates HIV-1 replication in cervical tissues: implications for HIV-1 transmission and efficacy of anti-HIV-1 microbicides. Mucosal Immunol. 2014;7:1165-1174. doi: 10.1038/mi.2014.3
39. Cogliano V, Baan R, Straif K, et al; WHO International Agency for Research on Cancer. Carcinogenicity of human papillomaviruses. Lancet Oncol.
40. Simon MA, Tseng CW, Wong JB. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320:674-686. doi:10.1001/jama.2018.10897
41. Perkins RB, Guido RS, Castle PE, et al; . 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors. J Low Genit Tract Dis. 2020;24:102-131. doi: 10.1097/LGT.0000000000000525
42. Meites E, Szilagyi PG, Chesson HW, et al. Human papillomavirus vaccination for adults: updated recommendations of the Advisory Committee on Immunization Practices. MMWR Morb Mortal Wkly Rep. 2019;68:698-702. doi: 10.15585/mmwr.mm6832a3
43. Schmidt R, Carson PJ, Jansen RJ. Resurgence of syphilis in the United States: an assessment of contributing factors. Infect Dis (Auckl). 2019;12:1178633719883282. doi: 10.1177/1178633719883282
44. Boog GHP, Lopes JVZ, Mahler JV, et al. Diagnostic tools for neurosyphilis: a systematic review. BMC Infect Dis. 2021;21:568. doi: 10.1186/s12879-021-06264-8
45. CDC. Sexually transmitted infections treatment guidelines, 2021. Syphilis. US Department of Health and Human Services. April 20, 2023. Accessed April 24, 2023. www.cdc.gov/std/treatment-guidelines/syphilis.htm
46. Matthias JM, Rahman MM, Newman DR, et al. Effectiveness of prenatal screening and treatment to prevent congenital syphilis, Louisiana and Florida, 2013-2014. Sex Transm Dis. 2017;44:498-502. doi: 10.1097/OLQ.0000000000000638
47. Clement ME, Okeke NL, Hicks CB. Treatment of syphilis: a systematic review. JAMA. 2014;312:1905-1917. doi: 10.1001/jama.2014.13259
48. Davidson KW, Barry MJ, Mangione CM, et al; US Preventive Services Task Force. Screening for chlamydia and gonorrhea: US Preventive Services Task Force recommendation statement. JAMA. 2021;326:949-956. doi: 10.1001/jama.2021.14081
49. Krist AH, Davidson KW, Mangione CM, et al; US Preventive Services Task Force. Screening for hepatitis B virus infection in adolescents and adults: US Preventive Services Task Force recommendation statement. JAMA. 2020;324:2415-2422. doi: 10.1001/jama.2020.22980
50. Owens DK, Davidson KW, Krist AH, et al; US Preventive Services Task Force. Screening for hepatitis C virus infection in adolescents and adults: US Preventive Services Task Force recommendation statement. JAMA. 2020;323:970-975. doi: 10.1001/jama.2020.1123
51. Bibbins-Domingo K, Grossman DC, Curry SJ, et al; US Preventive Services Task Force. Serologic screening for genital herpes infection: US Preventive Services Task Force recommendation statement. JAMA. 2016;316:2525-2530. doi: 10.1001/jama.2016.16776
52. Curry SJ, Krist AH, Owens DK, et al; US Preventive Services Task Force. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320:674-686. doi: 10.1001/jama.2018.10897
53. Owens DK, Davidson KW, Krist AH, et al; US Preventive Services Task Force. Screening for HIV infection: US Preventive Services Task Force recommendation statement. JAMA. 2019;321:2326-2336. doi: 10.1001/jama.2019.6587
54. Farley TA, Cohen DA, Elkins W. Asymptomatic sexually transmitted diseases: the case for screening. Prev Med. 2003;36:502-509. doi: 10.1016/s0091-7435(02)00058-0
55. US Public Health Service. Preexposure prophylaxis for the prevention of HIV infection in the United States—2021 update. A clinical practice guideline. Centers for Disease Control and Prevention. Accessed April 24, 2023. www.cdc.gov/hiv/pdf/risk/prep/cdc-hiv-prep-guidelines-2021.pdf
56. CDC. Sexually transmitted infections treatment guidelines, 2021: Sexual assault and abuse and STIs—adolescents and adults, 2021. US Department of Health and Human Services. July 22, 2021. Accessed April 24, 2023. www.cdc.gov/std/treatment-guidelines/sexual-assault-adults.htm
Except for a drop in the number of sexually transmitted infections (STIs) early in the COVID-19 pandemic (March and April 2020), the incidence of STIs has been rising throughout this century.1 In 2018, 1 in 5 people in the United States had an STI; 26 million new cases were reported that year, resulting in direct costs of $16 billion—85% of which was for the care of HIV infection.2 Also that year, infection with Chlamydia trachomatis (chlamydia), Trichomonas vaginalis (trichomoniasis), herpesvirus type 2 (genital herpes), and/or human papillomavirus (condylomata acuminata) constituted 97.6% of all prevalent and 93.1% of all incident STIs.3 Almost half (45.5%) of new cases of STIs occur in people between the ages of 15 and 24 years.3

Three factors—changing social patterns, including the increase of social networking; the ability of antiviral therapy to decrease the spread of HIV, leading to a reduction in condom use; and increasing antibiotic resistance—have converged to force changes in screening and treatment recommendations. In this article, we summarize updated guidance for primary care clinicians from several sources—including the Centers for Disease Control and Prevention (CDC), the US Preventive Services Task Force (USPSTF), and the American Society for Colposcopy and Cervical Pathology (ASCCP)—on diagnosing STIs (TABLE 14-13) and providing guideline-based treatment (Table 214). Because of the breadth and complexity of HIV disease, it is not addressed here.



Chlamydia
Infection with Chlamydia trachomatis—the most commonly reported bacterial STI in the United States—primarily causes cervicitis in women and proctitis in men, and can cause urethritis and pharyngitis in men and women. Prevalence is highest in sexually active people younger than 24 years.15
Because most infected people are asymptomatic and show no signs of illness on physical exam, screening is recommended for all sexually active women younger than 25 years and all men who have sex with men (MSM).4 No studies have established proper screening intervals; a reasonable approach, therefore, is to repeat screening for patients who have a sexual history that confers a new or persistent risk for infection since their last negative result.
Depending on the location of the infection, symptoms of chlamydia can include vaginal or penile irritation or discharge, dysuria, pelvic or rectal pain, and sore throat. Breakthrough bleeding in a patient who is taking an oral contraceptive should raise suspicion for chlamydia.
Untreated chlamydia can lead to pelvic inflammatory disease (PID), tubo-ovarian abscess, tubal factor infertility, ectopic pregnancy, and chronic pelvic pain. Infection can be transmitted vertically (mother to baby) antenatally, which can cause ophthalmia neonatorum and pneumonia in these newborns.
Diagnosis. The diagnosis of chlamydia is made using nucleic acid amplification testing (NAAT). Specimens can be collected by the clinician or the patient (self collected) using a vaginal, rectal, or oropharyngeal swab, or a combination of these, and can be obtained from urine or liquid-based cytology material.16
Continue to: Treatment
Treatment. Recommendations for treating chlamydia were updated by the CDC in its 2021 treatment guidelines (Table 214). Doxycycline 100 mg bid for 7 days is the preferred regimen; alternative regiments are (1) azithromycin 1 g in a single dose and (2) levofloxacin 500 mg daily for 7 days.4 A meta-analysis17 and a Cochrane review18 showed that the rate of treatment failure was higher among men when they were treated with azithromycin instead of doxycycline; furthermore, a randomized controlled trial demonstrated that doxycycline is more effective than azithromycin (cure rate, 100%, compared to 74%) at treating rectal chlamydia in MSM.19
Azithromycin is efficacious for urogenital infection in women; however, there is concern that the 33% to 83% of women who have concomitant rectal infection (despite reporting no receptive anorectal sexual activity) would be insufficiently treated. Outside pregnancy, the CDC does not recommend a test of cure but does recommend follow-up testing for reinfection in 3 months. Patients should abstain from sexual activity until 7 days after all sexual partners have been treated.
Expedited partner therapy (EPT) is the practice of treating sexual partners of patients with known chlamydia (and patients with gonococcal infection). Unless prohibited by law in your state, offer EPT to patients with chlamydia if they cannot ensure that their sexual partners from the past 60 days will seek timely treatment.a
Evidence to support EPT comes from 3 US clinical trials, whose subjects comprised heterosexual men and women with chlamydia or gonorrhea.21-23 The role of EPT for MSM is unclear; data are limited. Shared decision-making is recommended to determine whether EPT should be provided, to ensure that co-infection with other bacterial STIs (eg, syphilis) or HIV is not missed.24-26
a Visit www.cdc.gov/std/ept to read updated information about laws and regulations regarding EPT in your state.20
Gonorrhea
Gonorrhea is the second most-reported bacterial communicable disease.5 Infection with Neisseria gonorrhoeae causes urethral discharge in men, leading them to seek treatment; infected women, however, are often asymptomatic. Infected men and women might not recognize symptoms until they have transmitted the disease. Women have a slower natural clearance of gonococcal infection, which might explain their higher prevalence.27 Delayed recognition of symptoms can result in complications, including PID.5
Diagnosis. Specimens for NAAT can be obtained from urine, endocervical, vaginal, rectal, pharyngeal, and male urethral specimens. Reported sexual behaviors and exposures of women and transgender or gender-diverse people should be taken into consideration to determine whether rectal or pharyngeal testing, or both, should be performed.28 MSM should be screened annually at sites of contact, including the urethra, rectum, and pharynx.28 All patients with urogenital or rectal gonorrhea should be asked about oral sexual exposure; if reported, pharyngeal testing should be performed.5
NAAT of urine is at least as sensitive as testing of an endocervical specimen; the same specimen can be used to test for chlamydia and gonorrhea. Patient-collected specimens are a reasonable alternative to clinician-collected swab specimens.29
Continue to: Treatment
Treatment is complicated by the ability of gonorrhea to develop resistance. Intramuscular ceftriaxone 500 mg in a single dose cures 98% to 99% of infections in the United States; however, monitoring local resistance patterns in the community is an important component of treatment.28 (See Table 214 for an alternative regimen for cephalosporin-allergic patients and for treating gonococcal conjunctivitis and disseminated infection.)
In 2007, the CDC identified widespread quinolone-resistant gonococcal strains; therefore, fluoroquinolones no longer are recommended for treating gonorrhea.30 Cefixime has demonstrated only limited success in treating pharyngeal gonorrhea and does not attain a bactericidal level as high as ceftriaxone does; cefixime therefore is recommended only if ceftriaxone is unavailable.28 The national Gonococcal Isolate Surveillance Project is finding emerging evidence of the reduced susceptibility of N gonorrhoeae to azithromycin—making dual therapy for gonococcal infection no longer a recommendation.28
Patients should abstain from sex until 7 days after all sex partners have been treated for gonorrhea. As with chlamydia, the CDC does not recommend a test of cure for uncomplicated urogenital or rectal gonorrhea unless the patient is pregnant, but does recommend testing for reinfection 3 months after treatment.14 For patients with pharyngeal gonorrhea, a test of cure is recommended 7 to 14 days after initial treatment, due to challenges in treatment and because this site of infection is a potential source of antibiotic resistance.28
Trichomoniasis
T vaginalis, the most common nonviral STI worldwide,31 can manifest as a yellow-green vaginal discharge with or without vaginal discomfort, dysuria, epididymitis, and prostatitis; most cases, however, are asymptomatic. On examination, the cervix might be erythematous with punctate lesions (known as strawberry cervix).
Unlike most STIs, trichomoniasis is as common in women older than 24 years as it is in younger women. Infection is associated with a lower educational level, lower socioeconomic status, and having ≥ 2 sexual partners in the past year.32 Prevalence is approximately 10 times as high in Black women as it is in White women.
T vaginalis infection is associated with an increase in the risk for preterm birth, premature rupture of membranes, cervical cancer, and HIV infection. With a lack of high-quality clinical trials on the efficacy of screening, women with HIV are the only group for whom routine screening is recommended.6
Diagnosis. NAAT for trichomoniasis is now available in conjunction with gonorrhea and chlamydia testing of specimens on vaginal or urethral swabs and of urine specimens and liquid Pap smears.
Continue to: Treatment
Treatment. Because of greater efficacy, the treatment recommendation for women has changed from a single 2-g dose of oral metronidazole to 500 mg twice daily for 7 days. The 2-g single oral dose is still recommended for men7 (Table 214 lists alternative regimens).
Mycoplasma genitalium
Infection with M genitalium is common and often asymptomatic. The disease causes approximately 20% of all cases of nongonococcal and nonchlamydial urethritis in men and about 40% of persistent or recurrent infections. M genitalium is present in approximately 20% of women with cervicitis and has been associated with PID, preterm delivery, spontaneous abortion, and infertility.
There are limited and conflicting data regarding outcomes in infected patients other than those with persistent or recurrent infection; furthermore, resistance to azithromycin is increasing rapidly, resulting in an increase in treatment failures. Screening therefore is not recommended, and testing is recommended only in men with nongonococcal urethritis.33,34
Diagnosis. NAAT can be performed on urine or on a urethral, penile meatal, endocervical, or vaginal swab; men with recurrent urethritis or women with recurrent cervicitis should be tested. NAAT also can be considered in women with PID. Testing the specimen for the microorganism’s resistance to macrolide antibiotics is recommended (if such testing is available).
Treatment is initiated with doxycycline 100 mg twice daily for 7 days. If the organism is macrolide sensitive, follow with azithromycin 1 g orally on Day 1, then 500 mg/d for 3 more days. If the organism is macrolide resistant or testing is unavailable, follow doxycycline with oral moxifloxacin 400 mg/d for 7 days.33
Genital herpes (mostly herpesvirus type 2)
Genital herpes, characterized by painful, recurrent outbreaks of genital and anal lesions,35 is a lifelong infection that increases in prevalence with age.8 Because many infected people have disease that is undiagnosed or mild or have unrecognizable symptoms during viral shedding, most genital herpes infections are transmitted by people who are unaware that they are contagious.36 Herpesvirus type 2 (HSV-2) causes most cases of genital herpes, although an increasing percentage of cases are attributed to HSV type 1 (HSV-1) through receptive oral sex from a person who has an oral HSV-1 lesion.
Importantly, HSV-2–infected people are 2 to 3 times more likely to become infected with HIV than people who are not HSV-2 infected.37 This is becauseCD4+ T cells concentrate at the site of HSV lesions and express a higher level of cell-surface receptors that HIV uses to enter cells. HIV replicates 3 to 5 times more quickly in HSV-infected tissue.38
Continue to: HSV can become disseminated...
HSV can become disseminated, particularly in immunosuppressed people, and can manifest as encephalitis, hepatitis, and pneumonitis. Beyond its significant burden on health, HSV carries significant psychosocial consequences.9
Diagnosis. Clinical diagnosis can be challenging if classic lesions are absent at evaluation. If genital lesions are present, HSV can be identified by NAAT or culture of a specimen of those lesions. False-negative antibody results might be more frequent in early stages of infection; repeating antibody testing 12 weeks after presumed time of acquisition might therefore be indicated, based on clinical judgment. HSV-2 antibody positivity implies anogenital infection because almost all HSV-2 infections are sexually acquired.
HSV-1 antibody positivity alone is more difficult to interpret because this finding does not distinguish between oral and genital lesions, and most HSV-1 seropositivity is acquired during childhood.36 HSV polymerase chain reaction (PCR) testing of blood should not be performed to diagnose genital herpes infection, except in settings in which there is concern about disseminated infection.
Treatment. Management should address the acute episode and the chronic nature of genital herpes. Antivirals will not eradicate latent
- attenuate current infection
- prevent recurrence
- improve quality of life
- suppress the virus to prevent transmission to sexual partners.
All patients experiencing an initial episode of genital herpes should be treated, regardless of symptoms, due to the potential for prolonged or severe symptoms during recurrent episodes.9 Three drugs—acyclovir, valacyclovir, and famciclovir—are approved by the US Food and Drug Administration (FDA) to treat genital herpes and appear equally effective (TABLE 214).
Antiviral therapy for recurrent genital HSV infection can be administered either as suppressive therapy to reduce the frequency of recurrences or episodically to shorten the duration of lesions:
- Suppressive therapy reduces the frequency of recurrence by 70% to 80% among patients with frequent outbreaks. Long-term safety and efficacy are well established.
- Episodic therapy is most effective if started within 1 day after onset of lesions or during the prodrome.36
There is no specific recommendation for when to choose suppressive over episodic therapy; most patients prefer suppressive therapy because it improves quality of life. Use shared clinical decision-making to determine the best option for an individual patient.
Continue to: Human papillomavirus
Human papillomavirus
Condylomata acuminata (genital warts) are caused by human papillomavirus (HPV), most commonly types 6 and 11, which manifest as soft papules or plaques on the external genitalia, perineum, perianal skin, and groin. The warts are usually asymptomatic but can be painful or pruritic, depending on size and location.
Diagnosis is made by visual inspection and can be confirmed by biopsy if lesions are atypical. Lesions can resolve spontaneously, remain unchanged, or grow in size or number.
Treatment. The aim of treatment is relief of symptoms and removal of warts. Treatment does not eradicate HPV infection. Multiple treatments are available that can be applied by the patient as a cream, gel, or ointment or administered by the provider, including cryotherapy, surgical removal, and solutions. The decision on how to treat should be based on the number, size, and
HPV-associated cancers and precancers. This is a broad (and separate) topic. HPV types 16 and 18 cause most cases of cervical, penile, vulvar, vaginal, anal, and oropharyngeal cancer and precancer.39 The USPSTF, the American Cancer Society, and the American College of Obstetricians and Gynecologists all have recommendations for cervical cancer screening in the United States.40 Refer to guidelines of the ASCCP for recommendations on abnormal screening tests.41
Prevention of genital warts. The 9-valent HPV vaccine available in the United States is safe and effective and helps protect against viral types 6, 11, 16, 18, 31, 33, 45, 52, and 58. Types 6 and 11 are the principal causes of genital warts. Types 16 and 18 cause 66% of cervical cancer. The vaccination series can be started at age 9 years and is recommended for everyone through age 26 years. Only 2 doses are needed if the first dose is given prior to age 15 years; given after that age, a 3-dose series is utilized. Refer to CDC vaccine guidelines42 for details on the exact timing of vaccination.
Vaccination for women ages 27 to 45 years is not universally recommended because most people have been exposed to HPV by that age. However, the vaccine can still be administered, depending on clinical circumstances and the risk for new infection.42
Syphilis
Caused by the spirochete Treponema pallidum, syphilis manifests across a spectrum—from congenital to tertiary. The inability of medical science to develop a method for culturing the spirochete has confounded diagnosis and treatment.
Continue to: Since reaching a historic...
Since reaching a historic nadir of incidence in 2000 (5979 cases in the United States), there has been an increasingly rapid rise in that number: to 130,000 in 2020. More than 50% of cases are in MSM; however, the number of cases in heterosexual women is rapidly increasing.43
Routine screening for syphilis should be performed in any person who is at risk: all pregnant women in the first trimester (and in the third trimester and at delivery if they are at risk or live in a community where prevalence is high) and annually in sexually active MSM or anyone with HIV infection.10
Diagnosis. Examination by dark-field microscopy, testing by PCR, and direct fluorescent antibody assay for T pallidum from lesion tissue or exudate provide definitive diagnosis for early and congenital syphilis, but are often unavailable.
Presumptive diagnosis requires 2 serologic tests:
- Nontreponemal tests (the VDRL and rapid plasma reagin tests) identify anticardiolipin antibodies released during syphilis infection, although results also can be elevated in autoimmune disease or after certain immunizations, including the COVID-19 vaccine.
- Treponemal tests (the fluorescent treponemal antibody absorbed assay, T pallidum particulate agglutination assay, enzyme immunoassay, and chemiluminescence immunoassay) are specific antibody tests.
Historically, reactive nontreponemal tests, which are less expensive and easier to perform, were followed by a treponemal test to confirm the presumptive diagnosis. This method continues to be reasonable when screening patients in a low-prevalence population.11 The reverse sequence screening algorithm (ie, begin with a treponemal test) is now frequently used. With this method, a positive treponemal test must be confirmed with a nontreponemal test. If the treponemal test is positive and the nontreponemal test is negative, another treponemal test must be positive to confirm the diagnosis. This algorithm is useful in high-risk populations because it provides earlier detection of recently acquired syphilis and enhanced detection of late latent syphilis.12,13,44 The CDC has not stated a diagnostic preference.
Once the diagnosis is made, a complete history (including a sexual history and a history of syphilis testing and treatment) and a physical exam are necessary to confirm stage of disease.45
Special circumstances. Neurosyphilis, ocular syphilis, and otosyphilis refer to the site of infection and can occur at any stage of disease. The nervous system usually is infected within hours of initial infection, but symptoms might take weeks or years to develop—or might never manifest. Any time a patient develops neurologic, ophthalmologic, or audiologic symptoms, careful neurologic and ophthalmologic evaluation should be performed and the patient should be tested for HIV.
Continue to: Lumbar puncture is warranted...
Lumbar puncture is warranted for evaluation of cerebrospinal fluid if neurologic symptoms are present but is not necessary for isolated ocular syphilis or otosyphilis without neurologic findings. Treatment should not be delayed for test results if ocular syphilis is suspected because permanent blindness can develop. Any patient at high risk for an STI who presents with neurologic or ophthalmologic symptoms should be tested for syphilis and HIV.45
Pregnant women who have a diagnosis of syphilis should be treated with penicillin immediately because treatment ≥ 30 days prior to delivery is likely to prevent most cases of congenital syphilis. However, a course of penicillin might not prevent stillbirth or congenital syphilis in a gravely infected fetus, evidenced by fetal syphilis on a sonogram at the time of treatment. Additional doses of penicillin in pregnant women with early syphilis might be indicated if there is evidence of fetal syphilis on ultrasonography. All women who deliver a stillborn infant (≥ 20 weeks’ gestation) should be tested for syphilis at delivery.46
All patients in whom primary or secondary syphilis has been diagnosed should be tested for HIV at the time of diagnosis and treatment; if the result is negative, they should be offered preexposure prophylaxis (PrEP; discussed shortly). If the incidence of HIV in your community is high, repeat testing for HIV in 3 months. Clinical and serologic evaluation should be performed 6 and 12 months after treatment.47
Treatment. Penicillin remains the standard treatment for syphilis. Primary, secondary, and early tertiary stages (including in pregnancy) are treated with benzathine penicillin G 2.4 million units intramuscular (IM) in a single dose. For pregnant patients, repeating that dose in 1 week generally is recommended. Patients in the late latent (> 1 year) or tertiary stage receive the same dose of penicillin, which is then repeated weekly, for a total of 3 doses. Doxycycline and ceftriaxone are alternatives, except in pregnancy.
Warn patients of the Jarisch-Herxheimer reaction: fever, headache, and myalgias associated with initiation of treatment in the presence of the high bacterial load seen in early syphilis. Treatment is symptomatic, but the Jarisch-Herxheimer reaction can cause fetal distress in pregnancy.
Otosyphilis, ocular syphilis, and neurosyphilis require intravenous (IV) aqueous crystalline penicillin G 3 to 4 million U every 4 hours for 10 to 14 days.45 Alternatively, procaine penicillin G 2.4 million U/d IM can be given daily with oral probenecid 500 mg qid, both for 10 to 14 days (TABLE 214).
Screening andprevention of STIs
Screening recommendations
Follow USPSTF screening guidelines for STIs.10,48-54 Screen annually for:
- gonorrhea and chlamydia in women ages 15 to 24 years and in women older than 25 years if they are at increased risk
- gonorrhea, chlamydia, syphilis, and HIV in MSM, and hepatitis C if they are HIV positive
- trichomoniasis in women who are HIV positive.
Continue to: Consider the community in which...
Consider the community in which you practice when determining risk; you might want to consult local public health authorities for information about local epidemiology and guidance on determining which of your patients are at increased risk.
Preexposure prophylaxis
According to the CDC, all sexually active adults and adolescents should be informed about the availability of PrEP to prevent HIV infection. PrEP should be (1) available to anyone who requests it and (2) recommended for anyone who is sexually active and who practices sexual behaviors that place them at substantial risk for exposure to or acquisition of HIV, or both.
The recommended treatment protocol for men and women who have either an HIV-positive partner or inconsistent condom use or who have had a bacterial STI in the previous 6 months is oral emtricitabine 200 mg plus tenofovir disoproxil fumarate 300 mg/d (sold as Truvada-F/TDF). Men and transgender women (ie, assigned male at birth) with at-risk behaviors also can use emtricitabine plus tenofovir alafenamide 25 mg/d (sold as Descovy-F/TAF).
In addition, cabotegravir plus rilpirivine (sold as Cabenuva), IM every 2 months, was approved by the FDA for PrEP in 2021.
Creatinine clearance should be assessed at baseline and yearly (every 6 months for those older than 50 years) in patients taking PrEP. All patients must be tested for HIV at initiation of treatment and every 3 months thereafter (every 4 months for cabotegravir plus rilpirivine). Patients should be screened for bacterial STIs every 6 months (every 3 months for MSM and transgender women); screening for chlamydia should be done yearly. For patients being treated with emtricitabine plus tenofovir alafenamide, weight and a lipid profile (cholesterol and triglycerides) should be assessed annually.55
Postexposure prophylaxis
The sharp rise in the incidence of STIs in the past few years has brought renewed interest in postexposure prophylaxis (PEP) for STIs. Although PEP should be standard in cases of sexual assault, this protocol also can be considered in other instances of high-risk exposure.
CDC recommendations for PEP in cases of assault are56:
- ceftriaxone 500 mg IM in a single dose (1 g if weight is ≥ 150 kg) plus
- doxycycline 100 mg bid for 7 days plus
- metronidazole 2 g bid for 7 days (for vaginal exposure)
- pregnancy evaluation and emergency contraception
- hepatitis B risk evaluation and vaccination, with or without hepatitis B immune globulin
- HIV risk evaluation, based on CDC guidelines, and possible HIV prophylaxis (PrEP)
- HPV vaccination for patients ages 9 to 26 years if they are not already fully vaccinated.
CORRESPONDENCE
Belinda Vail, MD, 3901 Rainbow Boulevard, Mail Stop 4010, Kansas City, KS 66160; bvail@kumc.edu
Except for a drop in the number of sexually transmitted infections (STIs) early in the COVID-19 pandemic (March and April 2020), the incidence of STIs has been rising throughout this century.1 In 2018, 1 in 5 people in the United States had an STI; 26 million new cases were reported that year, resulting in direct costs of $16 billion—85% of which was for the care of HIV infection.2 Also that year, infection with Chlamydia trachomatis (chlamydia), Trichomonas vaginalis (trichomoniasis), herpesvirus type 2 (genital herpes), and/or human papillomavirus (condylomata acuminata) constituted 97.6% of all prevalent and 93.1% of all incident STIs.3 Almost half (45.5%) of new cases of STIs occur in people between the ages of 15 and 24 years.3

Three factors—changing social patterns, including the increase of social networking; the ability of antiviral therapy to decrease the spread of HIV, leading to a reduction in condom use; and increasing antibiotic resistance—have converged to force changes in screening and treatment recommendations. In this article, we summarize updated guidance for primary care clinicians from several sources—including the Centers for Disease Control and Prevention (CDC), the US Preventive Services Task Force (USPSTF), and the American Society for Colposcopy and Cervical Pathology (ASCCP)—on diagnosing STIs (TABLE 14-13) and providing guideline-based treatment (Table 214). Because of the breadth and complexity of HIV disease, it is not addressed here.



Chlamydia
Infection with Chlamydia trachomatis—the most commonly reported bacterial STI in the United States—primarily causes cervicitis in women and proctitis in men, and can cause urethritis and pharyngitis in men and women. Prevalence is highest in sexually active people younger than 24 years.15
Because most infected people are asymptomatic and show no signs of illness on physical exam, screening is recommended for all sexually active women younger than 25 years and all men who have sex with men (MSM).4 No studies have established proper screening intervals; a reasonable approach, therefore, is to repeat screening for patients who have a sexual history that confers a new or persistent risk for infection since their last negative result.
Depending on the location of the infection, symptoms of chlamydia can include vaginal or penile irritation or discharge, dysuria, pelvic or rectal pain, and sore throat. Breakthrough bleeding in a patient who is taking an oral contraceptive should raise suspicion for chlamydia.
Untreated chlamydia can lead to pelvic inflammatory disease (PID), tubo-ovarian abscess, tubal factor infertility, ectopic pregnancy, and chronic pelvic pain. Infection can be transmitted vertically (mother to baby) antenatally, which can cause ophthalmia neonatorum and pneumonia in these newborns.
Diagnosis. The diagnosis of chlamydia is made using nucleic acid amplification testing (NAAT). Specimens can be collected by the clinician or the patient (self collected) using a vaginal, rectal, or oropharyngeal swab, or a combination of these, and can be obtained from urine or liquid-based cytology material.16
Continue to: Treatment
Treatment. Recommendations for treating chlamydia were updated by the CDC in its 2021 treatment guidelines (Table 214). Doxycycline 100 mg bid for 7 days is the preferred regimen; alternative regiments are (1) azithromycin 1 g in a single dose and (2) levofloxacin 500 mg daily for 7 days.4 A meta-analysis17 and a Cochrane review18 showed that the rate of treatment failure was higher among men when they were treated with azithromycin instead of doxycycline; furthermore, a randomized controlled trial demonstrated that doxycycline is more effective than azithromycin (cure rate, 100%, compared to 74%) at treating rectal chlamydia in MSM.19
Azithromycin is efficacious for urogenital infection in women; however, there is concern that the 33% to 83% of women who have concomitant rectal infection (despite reporting no receptive anorectal sexual activity) would be insufficiently treated. Outside pregnancy, the CDC does not recommend a test of cure but does recommend follow-up testing for reinfection in 3 months. Patients should abstain from sexual activity until 7 days after all sexual partners have been treated.
Expedited partner therapy (EPT) is the practice of treating sexual partners of patients with known chlamydia (and patients with gonococcal infection). Unless prohibited by law in your state, offer EPT to patients with chlamydia if they cannot ensure that their sexual partners from the past 60 days will seek timely treatment.a
Evidence to support EPT comes from 3 US clinical trials, whose subjects comprised heterosexual men and women with chlamydia or gonorrhea.21-23 The role of EPT for MSM is unclear; data are limited. Shared decision-making is recommended to determine whether EPT should be provided, to ensure that co-infection with other bacterial STIs (eg, syphilis) or HIV is not missed.24-26
a Visit www.cdc.gov/std/ept to read updated information about laws and regulations regarding EPT in your state.20
Gonorrhea
Gonorrhea is the second most-reported bacterial communicable disease.5 Infection with Neisseria gonorrhoeae causes urethral discharge in men, leading them to seek treatment; infected women, however, are often asymptomatic. Infected men and women might not recognize symptoms until they have transmitted the disease. Women have a slower natural clearance of gonococcal infection, which might explain their higher prevalence.27 Delayed recognition of symptoms can result in complications, including PID.5
Diagnosis. Specimens for NAAT can be obtained from urine, endocervical, vaginal, rectal, pharyngeal, and male urethral specimens. Reported sexual behaviors and exposures of women and transgender or gender-diverse people should be taken into consideration to determine whether rectal or pharyngeal testing, or both, should be performed.28 MSM should be screened annually at sites of contact, including the urethra, rectum, and pharynx.28 All patients with urogenital or rectal gonorrhea should be asked about oral sexual exposure; if reported, pharyngeal testing should be performed.5
NAAT of urine is at least as sensitive as testing of an endocervical specimen; the same specimen can be used to test for chlamydia and gonorrhea. Patient-collected specimens are a reasonable alternative to clinician-collected swab specimens.29
Continue to: Treatment
Treatment is complicated by the ability of gonorrhea to develop resistance. Intramuscular ceftriaxone 500 mg in a single dose cures 98% to 99% of infections in the United States; however, monitoring local resistance patterns in the community is an important component of treatment.28 (See Table 214 for an alternative regimen for cephalosporin-allergic patients and for treating gonococcal conjunctivitis and disseminated infection.)
In 2007, the CDC identified widespread quinolone-resistant gonococcal strains; therefore, fluoroquinolones no longer are recommended for treating gonorrhea.30 Cefixime has demonstrated only limited success in treating pharyngeal gonorrhea and does not attain a bactericidal level as high as ceftriaxone does; cefixime therefore is recommended only if ceftriaxone is unavailable.28 The national Gonococcal Isolate Surveillance Project is finding emerging evidence of the reduced susceptibility of N gonorrhoeae to azithromycin—making dual therapy for gonococcal infection no longer a recommendation.28
Patients should abstain from sex until 7 days after all sex partners have been treated for gonorrhea. As with chlamydia, the CDC does not recommend a test of cure for uncomplicated urogenital or rectal gonorrhea unless the patient is pregnant, but does recommend testing for reinfection 3 months after treatment.14 For patients with pharyngeal gonorrhea, a test of cure is recommended 7 to 14 days after initial treatment, due to challenges in treatment and because this site of infection is a potential source of antibiotic resistance.28
Trichomoniasis
T vaginalis, the most common nonviral STI worldwide,31 can manifest as a yellow-green vaginal discharge with or without vaginal discomfort, dysuria, epididymitis, and prostatitis; most cases, however, are asymptomatic. On examination, the cervix might be erythematous with punctate lesions (known as strawberry cervix).
Unlike most STIs, trichomoniasis is as common in women older than 24 years as it is in younger women. Infection is associated with a lower educational level, lower socioeconomic status, and having ≥ 2 sexual partners in the past year.32 Prevalence is approximately 10 times as high in Black women as it is in White women.
T vaginalis infection is associated with an increase in the risk for preterm birth, premature rupture of membranes, cervical cancer, and HIV infection. With a lack of high-quality clinical trials on the efficacy of screening, women with HIV are the only group for whom routine screening is recommended.6
Diagnosis. NAAT for trichomoniasis is now available in conjunction with gonorrhea and chlamydia testing of specimens on vaginal or urethral swabs and of urine specimens and liquid Pap smears.
Continue to: Treatment
Treatment. Because of greater efficacy, the treatment recommendation for women has changed from a single 2-g dose of oral metronidazole to 500 mg twice daily for 7 days. The 2-g single oral dose is still recommended for men7 (Table 214 lists alternative regimens).
Mycoplasma genitalium
Infection with M genitalium is common and often asymptomatic. The disease causes approximately 20% of all cases of nongonococcal and nonchlamydial urethritis in men and about 40% of persistent or recurrent infections. M genitalium is present in approximately 20% of women with cervicitis and has been associated with PID, preterm delivery, spontaneous abortion, and infertility.
There are limited and conflicting data regarding outcomes in infected patients other than those with persistent or recurrent infection; furthermore, resistance to azithromycin is increasing rapidly, resulting in an increase in treatment failures. Screening therefore is not recommended, and testing is recommended only in men with nongonococcal urethritis.33,34
Diagnosis. NAAT can be performed on urine or on a urethral, penile meatal, endocervical, or vaginal swab; men with recurrent urethritis or women with recurrent cervicitis should be tested. NAAT also can be considered in women with PID. Testing the specimen for the microorganism’s resistance to macrolide antibiotics is recommended (if such testing is available).
Treatment is initiated with doxycycline 100 mg twice daily for 7 days. If the organism is macrolide sensitive, follow with azithromycin 1 g orally on Day 1, then 500 mg/d for 3 more days. If the organism is macrolide resistant or testing is unavailable, follow doxycycline with oral moxifloxacin 400 mg/d for 7 days.33
Genital herpes (mostly herpesvirus type 2)
Genital herpes, characterized by painful, recurrent outbreaks of genital and anal lesions,35 is a lifelong infection that increases in prevalence with age.8 Because many infected people have disease that is undiagnosed or mild or have unrecognizable symptoms during viral shedding, most genital herpes infections are transmitted by people who are unaware that they are contagious.36 Herpesvirus type 2 (HSV-2) causes most cases of genital herpes, although an increasing percentage of cases are attributed to HSV type 1 (HSV-1) through receptive oral sex from a person who has an oral HSV-1 lesion.
Importantly, HSV-2–infected people are 2 to 3 times more likely to become infected with HIV than people who are not HSV-2 infected.37 This is becauseCD4+ T cells concentrate at the site of HSV lesions and express a higher level of cell-surface receptors that HIV uses to enter cells. HIV replicates 3 to 5 times more quickly in HSV-infected tissue.38
Continue to: HSV can become disseminated...
HSV can become disseminated, particularly in immunosuppressed people, and can manifest as encephalitis, hepatitis, and pneumonitis. Beyond its significant burden on health, HSV carries significant psychosocial consequences.9
Diagnosis. Clinical diagnosis can be challenging if classic lesions are absent at evaluation. If genital lesions are present, HSV can be identified by NAAT or culture of a specimen of those lesions. False-negative antibody results might be more frequent in early stages of infection; repeating antibody testing 12 weeks after presumed time of acquisition might therefore be indicated, based on clinical judgment. HSV-2 antibody positivity implies anogenital infection because almost all HSV-2 infections are sexually acquired.
HSV-1 antibody positivity alone is more difficult to interpret because this finding does not distinguish between oral and genital lesions, and most HSV-1 seropositivity is acquired during childhood.36 HSV polymerase chain reaction (PCR) testing of blood should not be performed to diagnose genital herpes infection, except in settings in which there is concern about disseminated infection.
Treatment. Management should address the acute episode and the chronic nature of genital herpes. Antivirals will not eradicate latent
- attenuate current infection
- prevent recurrence
- improve quality of life
- suppress the virus to prevent transmission to sexual partners.
All patients experiencing an initial episode of genital herpes should be treated, regardless of symptoms, due to the potential for prolonged or severe symptoms during recurrent episodes.9 Three drugs—acyclovir, valacyclovir, and famciclovir—are approved by the US Food and Drug Administration (FDA) to treat genital herpes and appear equally effective (TABLE 214).
Antiviral therapy for recurrent genital HSV infection can be administered either as suppressive therapy to reduce the frequency of recurrences or episodically to shorten the duration of lesions:
- Suppressive therapy reduces the frequency of recurrence by 70% to 80% among patients with frequent outbreaks. Long-term safety and efficacy are well established.
- Episodic therapy is most effective if started within 1 day after onset of lesions or during the prodrome.36
There is no specific recommendation for when to choose suppressive over episodic therapy; most patients prefer suppressive therapy because it improves quality of life. Use shared clinical decision-making to determine the best option for an individual patient.
Continue to: Human papillomavirus
Human papillomavirus
Condylomata acuminata (genital warts) are caused by human papillomavirus (HPV), most commonly types 6 and 11, which manifest as soft papules or plaques on the external genitalia, perineum, perianal skin, and groin. The warts are usually asymptomatic but can be painful or pruritic, depending on size and location.
Diagnosis is made by visual inspection and can be confirmed by biopsy if lesions are atypical. Lesions can resolve spontaneously, remain unchanged, or grow in size or number.
Treatment. The aim of treatment is relief of symptoms and removal of warts. Treatment does not eradicate HPV infection. Multiple treatments are available that can be applied by the patient as a cream, gel, or ointment or administered by the provider, including cryotherapy, surgical removal, and solutions. The decision on how to treat should be based on the number, size, and
HPV-associated cancers and precancers. This is a broad (and separate) topic. HPV types 16 and 18 cause most cases of cervical, penile, vulvar, vaginal, anal, and oropharyngeal cancer and precancer.39 The USPSTF, the American Cancer Society, and the American College of Obstetricians and Gynecologists all have recommendations for cervical cancer screening in the United States.40 Refer to guidelines of the ASCCP for recommendations on abnormal screening tests.41
Prevention of genital warts. The 9-valent HPV vaccine available in the United States is safe and effective and helps protect against viral types 6, 11, 16, 18, 31, 33, 45, 52, and 58. Types 6 and 11 are the principal causes of genital warts. Types 16 and 18 cause 66% of cervical cancer. The vaccination series can be started at age 9 years and is recommended for everyone through age 26 years. Only 2 doses are needed if the first dose is given prior to age 15 years; given after that age, a 3-dose series is utilized. Refer to CDC vaccine guidelines42 for details on the exact timing of vaccination.
Vaccination for women ages 27 to 45 years is not universally recommended because most people have been exposed to HPV by that age. However, the vaccine can still be administered, depending on clinical circumstances and the risk for new infection.42
Syphilis
Caused by the spirochete Treponema pallidum, syphilis manifests across a spectrum—from congenital to tertiary. The inability of medical science to develop a method for culturing the spirochete has confounded diagnosis and treatment.
Continue to: Since reaching a historic...
Since reaching a historic nadir of incidence in 2000 (5979 cases in the United States), there has been an increasingly rapid rise in that number: to 130,000 in 2020. More than 50% of cases are in MSM; however, the number of cases in heterosexual women is rapidly increasing.43
Routine screening for syphilis should be performed in any person who is at risk: all pregnant women in the first trimester (and in the third trimester and at delivery if they are at risk or live in a community where prevalence is high) and annually in sexually active MSM or anyone with HIV infection.10
Diagnosis. Examination by dark-field microscopy, testing by PCR, and direct fluorescent antibody assay for T pallidum from lesion tissue or exudate provide definitive diagnosis for early and congenital syphilis, but are often unavailable.
Presumptive diagnosis requires 2 serologic tests:
- Nontreponemal tests (the VDRL and rapid plasma reagin tests) identify anticardiolipin antibodies released during syphilis infection, although results also can be elevated in autoimmune disease or after certain immunizations, including the COVID-19 vaccine.
- Treponemal tests (the fluorescent treponemal antibody absorbed assay, T pallidum particulate agglutination assay, enzyme immunoassay, and chemiluminescence immunoassay) are specific antibody tests.
Historically, reactive nontreponemal tests, which are less expensive and easier to perform, were followed by a treponemal test to confirm the presumptive diagnosis. This method continues to be reasonable when screening patients in a low-prevalence population.11 The reverse sequence screening algorithm (ie, begin with a treponemal test) is now frequently used. With this method, a positive treponemal test must be confirmed with a nontreponemal test. If the treponemal test is positive and the nontreponemal test is negative, another treponemal test must be positive to confirm the diagnosis. This algorithm is useful in high-risk populations because it provides earlier detection of recently acquired syphilis and enhanced detection of late latent syphilis.12,13,44 The CDC has not stated a diagnostic preference.
Once the diagnosis is made, a complete history (including a sexual history and a history of syphilis testing and treatment) and a physical exam are necessary to confirm stage of disease.45
Special circumstances. Neurosyphilis, ocular syphilis, and otosyphilis refer to the site of infection and can occur at any stage of disease. The nervous system usually is infected within hours of initial infection, but symptoms might take weeks or years to develop—or might never manifest. Any time a patient develops neurologic, ophthalmologic, or audiologic symptoms, careful neurologic and ophthalmologic evaluation should be performed and the patient should be tested for HIV.
Continue to: Lumbar puncture is warranted...
Lumbar puncture is warranted for evaluation of cerebrospinal fluid if neurologic symptoms are present but is not necessary for isolated ocular syphilis or otosyphilis without neurologic findings. Treatment should not be delayed for test results if ocular syphilis is suspected because permanent blindness can develop. Any patient at high risk for an STI who presents with neurologic or ophthalmologic symptoms should be tested for syphilis and HIV.45
Pregnant women who have a diagnosis of syphilis should be treated with penicillin immediately because treatment ≥ 30 days prior to delivery is likely to prevent most cases of congenital syphilis. However, a course of penicillin might not prevent stillbirth or congenital syphilis in a gravely infected fetus, evidenced by fetal syphilis on a sonogram at the time of treatment. Additional doses of penicillin in pregnant women with early syphilis might be indicated if there is evidence of fetal syphilis on ultrasonography. All women who deliver a stillborn infant (≥ 20 weeks’ gestation) should be tested for syphilis at delivery.46
All patients in whom primary or secondary syphilis has been diagnosed should be tested for HIV at the time of diagnosis and treatment; if the result is negative, they should be offered preexposure prophylaxis (PrEP; discussed shortly). If the incidence of HIV in your community is high, repeat testing for HIV in 3 months. Clinical and serologic evaluation should be performed 6 and 12 months after treatment.47
Treatment. Penicillin remains the standard treatment for syphilis. Primary, secondary, and early tertiary stages (including in pregnancy) are treated with benzathine penicillin G 2.4 million units intramuscular (IM) in a single dose. For pregnant patients, repeating that dose in 1 week generally is recommended. Patients in the late latent (> 1 year) or tertiary stage receive the same dose of penicillin, which is then repeated weekly, for a total of 3 doses. Doxycycline and ceftriaxone are alternatives, except in pregnancy.
Warn patients of the Jarisch-Herxheimer reaction: fever, headache, and myalgias associated with initiation of treatment in the presence of the high bacterial load seen in early syphilis. Treatment is symptomatic, but the Jarisch-Herxheimer reaction can cause fetal distress in pregnancy.
Otosyphilis, ocular syphilis, and neurosyphilis require intravenous (IV) aqueous crystalline penicillin G 3 to 4 million U every 4 hours for 10 to 14 days.45 Alternatively, procaine penicillin G 2.4 million U/d IM can be given daily with oral probenecid 500 mg qid, both for 10 to 14 days (TABLE 214).
Screening andprevention of STIs
Screening recommendations
Follow USPSTF screening guidelines for STIs.10,48-54 Screen annually for:
- gonorrhea and chlamydia in women ages 15 to 24 years and in women older than 25 years if they are at increased risk
- gonorrhea, chlamydia, syphilis, and HIV in MSM, and hepatitis C if they are HIV positive
- trichomoniasis in women who are HIV positive.
Continue to: Consider the community in which...
Consider the community in which you practice when determining risk; you might want to consult local public health authorities for information about local epidemiology and guidance on determining which of your patients are at increased risk.
Preexposure prophylaxis
According to the CDC, all sexually active adults and adolescents should be informed about the availability of PrEP to prevent HIV infection. PrEP should be (1) available to anyone who requests it and (2) recommended for anyone who is sexually active and who practices sexual behaviors that place them at substantial risk for exposure to or acquisition of HIV, or both.
The recommended treatment protocol for men and women who have either an HIV-positive partner or inconsistent condom use or who have had a bacterial STI in the previous 6 months is oral emtricitabine 200 mg plus tenofovir disoproxil fumarate 300 mg/d (sold as Truvada-F/TDF). Men and transgender women (ie, assigned male at birth) with at-risk behaviors also can use emtricitabine plus tenofovir alafenamide 25 mg/d (sold as Descovy-F/TAF).
In addition, cabotegravir plus rilpirivine (sold as Cabenuva), IM every 2 months, was approved by the FDA for PrEP in 2021.
Creatinine clearance should be assessed at baseline and yearly (every 6 months for those older than 50 years) in patients taking PrEP. All patients must be tested for HIV at initiation of treatment and every 3 months thereafter (every 4 months for cabotegravir plus rilpirivine). Patients should be screened for bacterial STIs every 6 months (every 3 months for MSM and transgender women); screening for chlamydia should be done yearly. For patients being treated with emtricitabine plus tenofovir alafenamide, weight and a lipid profile (cholesterol and triglycerides) should be assessed annually.55
Postexposure prophylaxis
The sharp rise in the incidence of STIs in the past few years has brought renewed interest in postexposure prophylaxis (PEP) for STIs. Although PEP should be standard in cases of sexual assault, this protocol also can be considered in other instances of high-risk exposure.
CDC recommendations for PEP in cases of assault are56:
- ceftriaxone 500 mg IM in a single dose (1 g if weight is ≥ 150 kg) plus
- doxycycline 100 mg bid for 7 days plus
- metronidazole 2 g bid for 7 days (for vaginal exposure)
- pregnancy evaluation and emergency contraception
- hepatitis B risk evaluation and vaccination, with or without hepatitis B immune globulin
- HIV risk evaluation, based on CDC guidelines, and possible HIV prophylaxis (PrEP)
- HPV vaccination for patients ages 9 to 26 years if they are not already fully vaccinated.
CORRESPONDENCE
Belinda Vail, MD, 3901 Rainbow Boulevard, Mail Stop 4010, Kansas City, KS 66160; bvail@kumc.edu
1. Pagaoa M, Grey J, Torrone E, et al. Trends in nationally notifiable sexually transmitted disease case reports during the US COVID-19 pandemic, January to December 2020. Sex Transm Dis. 2021;48:798-804. doi: 10.1097/OLQ.0000000000001506
2. Chesson HW, Spicknall IH; Bingham A, et al. The estimated direct lifetime medical costs of sexually transmitted infections acquired in the United States in 2018. Sex Transm Dis. 2021;48:215-221. doi: 10.1097/OLQ.0000000000001380
3. Kreisel KM, Spicknall IH, Gargano JW, et al. Sexually transmitted infections among US women and men: prevalence and incidence estimates, 2018. Sex Transm Dis. 2021;48:208-214. doi: 10.1097/OLQ.0000000000001355
4. CDC. Sexually transmitted infections treatment guidelines, 2021: Chlamydial infections among adolescents and adults. US Department of Health and Human Services. July 21, 2021. Accessed April 19, 2023. www.cdc.gov/std/treatment-guidelines/chlamydia.htm
5. CDC. Sexually transmitted infections treatment guidelines, 2021: Gonococcal infections among adolescents and adults. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/gonorrhea-adults.htm
6. Van Gerwen OT, Muzny CA. Recent advances in the epidemiology, diagnosis, and management of Trichomonas vaginalis infection. F1000Res. 2019;
7. CDC. Sexually transmitted infections treatment guidelines, 2021. Trichomoniasis. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. December 27, 2021. www.cdc.gov/std/treatment-guidelines/trichomoniasis.htm
8. Spicknall IH, Flagg EW, Torrone EA. Estimates of the prevalence and incidence of genital herpes, United States, 2018. Sex Transm Dis. 2021;48:260-265. doi: 10.1097/OLQ.0000000000001375
9. Mark H, Gilbert L, Nanda J. Psychosocial well-being and quality of life among women newly diagnosed with genital herpes. J Obstet Gynecol Neonatal Nurs.
10. Bibbins-Domingo K, Grossman DC, Curry SJ, et al; US Preventive Services Task Force. Screening for syphilis infection in nonpregnant adults and adolescents: US Preventive Services Task Force recommendation statement. JAMA. 2016;315:2321-2327. doi: 10.1001/jama.2016.5824
11. Ricco J, Westby A. Syphilis: far from ancient history. Am Fam Physician. 2020;102:91-98.
12. Goza M, Kulwicki B, Akers JM, et al. Syphilis screening: a review of the Syphilis Health Check rapid immunochromatographic test. J Pharm Technol. 2017;33:53-59. doi:10.1177/8755122517691308
13. Henao- AF, Johnson SC. Diagnostic tests for syphilis: new tests and new algorithms. Neurol Clin Pract. 2014;4:114-122. doi: 10.1212/01.CPJ.0000435752.17621.48
14. Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021;70:1-187. doi:10.15585/mmwr.rr7004a1
15. CDC. Sexually Transmitted Disease Surveillance 2021. National overview of STDs. US Department of Health and Human Services. April 2023. Accessed May 9, 2023. www.cdc.gov/std/statistics/2021/overview.htm#Chlamydia
16. CDC. Recommendations for the laboratory-based detection of Chlamydia trachomatis and Neisseria gonorrhoeae—2014. MMWR Recomm Rep. 2014;63:1-19.
17. Kong FYS, Tabrizi SN, Law M, et al. Azithromycin versus doxycycline for the treatment of genital chlamydia infection: a meta-analysis of randomized controlled trials. Clin Infect Dis. 2014;59:193-205. doi: 10.1093/cid/ciu220
18. Páez-Canro C, Alzate JP, González LM, et al. Antibiotics for treating urogenital Chlamydia trachomatis infection in men and non-pregnant women. Cochrane Database Syst Rev. 2019;1:CD010871. doi: 10.1002/14651858.CD010871.pub2
19. Dombrowski JC, Wierzbicki MR, Newman LM, et al. Doxycycline versus azithromycin for the treatment of rectal chlamydia in men who have sex with men: a randomized controlled trial. Clin Infect Dis. 2021;73:824-831. doi: 10.1093/cid/ciab153
20. CDC. Sexually transmitted infections treatment guidelines, 2021: Expedited partner therapy. US Department of Health and Human Services. July 22, 2021. Accessed April 19, 2023. www.cdc.gov/std/treatment-guidelines/clinical-EPT.htm
21. Golden MR, Whittington WLH, Handsfield HH, et al. Effect of expedited treatment of sex partners on recurrent or persistent gonorrhea or chlamydial infection. N Engl J Med. 2005;352:676-685. doi: 10.1056/NEJMoa041681
22. Schillinger JA, Kissinger P, Calvet H, et al. Patient-delivered partner treatment with azithromycin to prevent repeated Chlamydia trachomatis infection among women: a randomized, controlled trial. Sex Transm Dis. 2003;30:49-56. doi: 10.1097/00007435-200301000-00011
23. Cameron ST, Glasier A, Scott G, et al. Novel interventions to reduce re-infection in women with chlamydia: a randomized controlled trial. Hum Reprod. 2009;24:888-895. doi: 10.1093/humrep/den475
24. McNulty A, Teh MF, Freedman E. Patient delivered partner therapy for chlamydial infection—what would be missed? Sex Transm Dis. 2008;35:834-836. doi: 10.1097/OLQ.0b013e3181761993
25. Stekler J, Bachmann L, Brotman RM, et al. Concurrent sexually transmitted infections (STIs) in sex partners of patients with selected STIs: implications for patient-delivered partner therapy. Clin Infect Dis. 2005;40:787-793. doi: 10.1086/428043
26. Schillinger JA, Kissinger P, Calvet H, et al. Patient-delivered partner treatment with azithromycin to prevent repeated Chlamydia trachomatis infection among women: a randomized, controlled trial. Sex Transm Dis. 2003;30:49-56. doi: 10.1097/00007435-200301000-00011
27. Stupiansky NW, Van der Pol B, Williams JA, et al. The natural history of incident gonococcal infection in adolescent women. Sex Transm Dis. 2011;38:750-754. doi: 10.1097/OLQ.0b013e31820ff9a4
28. CDC. Sexually transmitted infections treatment guidelines, 2021: Screening recommendations and considerations referenced in treatment guidelines and original sources. US Department of Health and Human Services. June 6, 2022. Accessed May 9, 2023. www.cdc.gov/std/treatment-guidelines/screening-recommen dations.htm
29. Cantor A, Dana T, Griffen JC, et al. Screening for chlamydial and gonococcal infections: a systematic review update for the US Preventive Services Task Force. Evidence Synthesis No. 206. AHRQ Report No. 21-05275-EF-1. Agency for Healthcare Research and Quality. September 2021. www.ncbi.nlm.nih.gov/books/NBK574045
30. CDC. Update to CDC’s sexually transmitted diseases treatment guidelines, 2006: fluoroquinolones no longer recommended for treatment of gonococcal infections. MMWR Morb Mortal Wkly Rep. 2007;56:332-336.
31. Rowley J, Vander Hoorn S, Korenromp E, et al. Chlamydia, gonorrhoea, trichomoniasis and syphilis: global prevalence and incidence estimates, 2016. Bull World Health Organ. 2019:97:548-562P. doi: 10.2471/BLT.18.228486
32. Patel EU, Gaydos CA, Packman ZR, et al. Prevalence and correlates of Trichomonas vaginalis infection among men and women in the United States. Clin Infect Dis. 2018;67:211-217. doi: 10.1093/cid/ciy079
33. CDC. Sexually transmitted infections treatment guidelines, 2021. Mycoplasma genitalium. US Department of Health and Human Services. July 22, 2021. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/mycoplasmagenitalium.htm
34. Manhart LE, Broad JM, Bolden MR. Mycoplasma genitalium: should we treat and how? Clin Infect Dis. 2011;53(suppl 3):S129-S142. doi:10.1093/cid/cir702.
35. Corey L, Wald A. Genital herpes. In: Holmes KK, Sparling PF, Stamm WE, et al, eds. Sexually Transmitted Diseases. 4th ed. McGraw-Hill; 2008:399-437.
36. CDC. Sexually transmitted infections treatment guidelines, 2021: Genital herpes. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/herpes.htm
37. Looker KJ, Elmes JAR, Gottlieb SL, et al. Effect of HSV-2 infection on subsequent HIV acquisition: an updated systematic review and meta-analysis. Lancet Infect Dis. 2017;17:1303-1316. doi: 10.1016/S1473-3099(17)30405-X
38. Rollenhagen C, Lathrop M, Macura SL, et al. Herpes simplex virus type-2 stimulates HIV-1 replication in cervical tissues: implications for HIV-1 transmission and efficacy of anti-HIV-1 microbicides. Mucosal Immunol. 2014;7:1165-1174. doi: 10.1038/mi.2014.3
39. Cogliano V, Baan R, Straif K, et al; WHO International Agency for Research on Cancer. Carcinogenicity of human papillomaviruses. Lancet Oncol.
40. Simon MA, Tseng CW, Wong JB. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320:674-686. doi:10.1001/jama.2018.10897
41. Perkins RB, Guido RS, Castle PE, et al; . 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors. J Low Genit Tract Dis. 2020;24:102-131. doi: 10.1097/LGT.0000000000000525
42. Meites E, Szilagyi PG, Chesson HW, et al. Human papillomavirus vaccination for adults: updated recommendations of the Advisory Committee on Immunization Practices. MMWR Morb Mortal Wkly Rep. 2019;68:698-702. doi: 10.15585/mmwr.mm6832a3
43. Schmidt R, Carson PJ, Jansen RJ. Resurgence of syphilis in the United States: an assessment of contributing factors. Infect Dis (Auckl). 2019;12:1178633719883282. doi: 10.1177/1178633719883282
44. Boog GHP, Lopes JVZ, Mahler JV, et al. Diagnostic tools for neurosyphilis: a systematic review. BMC Infect Dis. 2021;21:568. doi: 10.1186/s12879-021-06264-8
45. CDC. Sexually transmitted infections treatment guidelines, 2021. Syphilis. US Department of Health and Human Services. April 20, 2023. Accessed April 24, 2023. www.cdc.gov/std/treatment-guidelines/syphilis.htm
46. Matthias JM, Rahman MM, Newman DR, et al. Effectiveness of prenatal screening and treatment to prevent congenital syphilis, Louisiana and Florida, 2013-2014. Sex Transm Dis. 2017;44:498-502. doi: 10.1097/OLQ.0000000000000638
47. Clement ME, Okeke NL, Hicks CB. Treatment of syphilis: a systematic review. JAMA. 2014;312:1905-1917. doi: 10.1001/jama.2014.13259
48. Davidson KW, Barry MJ, Mangione CM, et al; US Preventive Services Task Force. Screening for chlamydia and gonorrhea: US Preventive Services Task Force recommendation statement. JAMA. 2021;326:949-956. doi: 10.1001/jama.2021.14081
49. Krist AH, Davidson KW, Mangione CM, et al; US Preventive Services Task Force. Screening for hepatitis B virus infection in adolescents and adults: US Preventive Services Task Force recommendation statement. JAMA. 2020;324:2415-2422. doi: 10.1001/jama.2020.22980
50. Owens DK, Davidson KW, Krist AH, et al; US Preventive Services Task Force. Screening for hepatitis C virus infection in adolescents and adults: US Preventive Services Task Force recommendation statement. JAMA. 2020;323:970-975. doi: 10.1001/jama.2020.1123
51. Bibbins-Domingo K, Grossman DC, Curry SJ, et al; US Preventive Services Task Force. Serologic screening for genital herpes infection: US Preventive Services Task Force recommendation statement. JAMA. 2016;316:2525-2530. doi: 10.1001/jama.2016.16776
52. Curry SJ, Krist AH, Owens DK, et al; US Preventive Services Task Force. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320:674-686. doi: 10.1001/jama.2018.10897
53. Owens DK, Davidson KW, Krist AH, et al; US Preventive Services Task Force. Screening for HIV infection: US Preventive Services Task Force recommendation statement. JAMA. 2019;321:2326-2336. doi: 10.1001/jama.2019.6587
54. Farley TA, Cohen DA, Elkins W. Asymptomatic sexually transmitted diseases: the case for screening. Prev Med. 2003;36:502-509. doi: 10.1016/s0091-7435(02)00058-0
55. US Public Health Service. Preexposure prophylaxis for the prevention of HIV infection in the United States—2021 update. A clinical practice guideline. Centers for Disease Control and Prevention. Accessed April 24, 2023. www.cdc.gov/hiv/pdf/risk/prep/cdc-hiv-prep-guidelines-2021.pdf
56. CDC. Sexually transmitted infections treatment guidelines, 2021: Sexual assault and abuse and STIs—adolescents and adults, 2021. US Department of Health and Human Services. July 22, 2021. Accessed April 24, 2023. www.cdc.gov/std/treatment-guidelines/sexual-assault-adults.htm
1. Pagaoa M, Grey J, Torrone E, et al. Trends in nationally notifiable sexually transmitted disease case reports during the US COVID-19 pandemic, January to December 2020. Sex Transm Dis. 2021;48:798-804. doi: 10.1097/OLQ.0000000000001506
2. Chesson HW, Spicknall IH; Bingham A, et al. The estimated direct lifetime medical costs of sexually transmitted infections acquired in the United States in 2018. Sex Transm Dis. 2021;48:215-221. doi: 10.1097/OLQ.0000000000001380
3. Kreisel KM, Spicknall IH, Gargano JW, et al. Sexually transmitted infections among US women and men: prevalence and incidence estimates, 2018. Sex Transm Dis. 2021;48:208-214. doi: 10.1097/OLQ.0000000000001355
4. CDC. Sexually transmitted infections treatment guidelines, 2021: Chlamydial infections among adolescents and adults. US Department of Health and Human Services. July 21, 2021. Accessed April 19, 2023. www.cdc.gov/std/treatment-guidelines/chlamydia.htm
5. CDC. Sexually transmitted infections treatment guidelines, 2021: Gonococcal infections among adolescents and adults. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/gonorrhea-adults.htm
6. Van Gerwen OT, Muzny CA. Recent advances in the epidemiology, diagnosis, and management of Trichomonas vaginalis infection. F1000Res. 2019;
7. CDC. Sexually transmitted infections treatment guidelines, 2021. Trichomoniasis. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. December 27, 2021. www.cdc.gov/std/treatment-guidelines/trichomoniasis.htm
8. Spicknall IH, Flagg EW, Torrone EA. Estimates of the prevalence and incidence of genital herpes, United States, 2018. Sex Transm Dis. 2021;48:260-265. doi: 10.1097/OLQ.0000000000001375
9. Mark H, Gilbert L, Nanda J. Psychosocial well-being and quality of life among women newly diagnosed with genital herpes. J Obstet Gynecol Neonatal Nurs.
10. Bibbins-Domingo K, Grossman DC, Curry SJ, et al; US Preventive Services Task Force. Screening for syphilis infection in nonpregnant adults and adolescents: US Preventive Services Task Force recommendation statement. JAMA. 2016;315:2321-2327. doi: 10.1001/jama.2016.5824
11. Ricco J, Westby A. Syphilis: far from ancient history. Am Fam Physician. 2020;102:91-98.
12. Goza M, Kulwicki B, Akers JM, et al. Syphilis screening: a review of the Syphilis Health Check rapid immunochromatographic test. J Pharm Technol. 2017;33:53-59. doi:10.1177/8755122517691308
13. Henao- AF, Johnson SC. Diagnostic tests for syphilis: new tests and new algorithms. Neurol Clin Pract. 2014;4:114-122. doi: 10.1212/01.CPJ.0000435752.17621.48
14. Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021;70:1-187. doi:10.15585/mmwr.rr7004a1
15. CDC. Sexually Transmitted Disease Surveillance 2021. National overview of STDs. US Department of Health and Human Services. April 2023. Accessed May 9, 2023. www.cdc.gov/std/statistics/2021/overview.htm#Chlamydia
16. CDC. Recommendations for the laboratory-based detection of Chlamydia trachomatis and Neisseria gonorrhoeae—2014. MMWR Recomm Rep. 2014;63:1-19.
17. Kong FYS, Tabrizi SN, Law M, et al. Azithromycin versus doxycycline for the treatment of genital chlamydia infection: a meta-analysis of randomized controlled trials. Clin Infect Dis. 2014;59:193-205. doi: 10.1093/cid/ciu220
18. Páez-Canro C, Alzate JP, González LM, et al. Antibiotics for treating urogenital Chlamydia trachomatis infection in men and non-pregnant women. Cochrane Database Syst Rev. 2019;1:CD010871. doi: 10.1002/14651858.CD010871.pub2
19. Dombrowski JC, Wierzbicki MR, Newman LM, et al. Doxycycline versus azithromycin for the treatment of rectal chlamydia in men who have sex with men: a randomized controlled trial. Clin Infect Dis. 2021;73:824-831. doi: 10.1093/cid/ciab153
20. CDC. Sexually transmitted infections treatment guidelines, 2021: Expedited partner therapy. US Department of Health and Human Services. July 22, 2021. Accessed April 19, 2023. www.cdc.gov/std/treatment-guidelines/clinical-EPT.htm
21. Golden MR, Whittington WLH, Handsfield HH, et al. Effect of expedited treatment of sex partners on recurrent or persistent gonorrhea or chlamydial infection. N Engl J Med. 2005;352:676-685. doi: 10.1056/NEJMoa041681
22. Schillinger JA, Kissinger P, Calvet H, et al. Patient-delivered partner treatment with azithromycin to prevent repeated Chlamydia trachomatis infection among women: a randomized, controlled trial. Sex Transm Dis. 2003;30:49-56. doi: 10.1097/00007435-200301000-00011
23. Cameron ST, Glasier A, Scott G, et al. Novel interventions to reduce re-infection in women with chlamydia: a randomized controlled trial. Hum Reprod. 2009;24:888-895. doi: 10.1093/humrep/den475
24. McNulty A, Teh MF, Freedman E. Patient delivered partner therapy for chlamydial infection—what would be missed? Sex Transm Dis. 2008;35:834-836. doi: 10.1097/OLQ.0b013e3181761993
25. Stekler J, Bachmann L, Brotman RM, et al. Concurrent sexually transmitted infections (STIs) in sex partners of patients with selected STIs: implications for patient-delivered partner therapy. Clin Infect Dis. 2005;40:787-793. doi: 10.1086/428043
26. Schillinger JA, Kissinger P, Calvet H, et al. Patient-delivered partner treatment with azithromycin to prevent repeated Chlamydia trachomatis infection among women: a randomized, controlled trial. Sex Transm Dis. 2003;30:49-56. doi: 10.1097/00007435-200301000-00011
27. Stupiansky NW, Van der Pol B, Williams JA, et al. The natural history of incident gonococcal infection in adolescent women. Sex Transm Dis. 2011;38:750-754. doi: 10.1097/OLQ.0b013e31820ff9a4
28. CDC. Sexually transmitted infections treatment guidelines, 2021: Screening recommendations and considerations referenced in treatment guidelines and original sources. US Department of Health and Human Services. June 6, 2022. Accessed May 9, 2023. www.cdc.gov/std/treatment-guidelines/screening-recommen dations.htm
29. Cantor A, Dana T, Griffen JC, et al. Screening for chlamydial and gonococcal infections: a systematic review update for the US Preventive Services Task Force. Evidence Synthesis No. 206. AHRQ Report No. 21-05275-EF-1. Agency for Healthcare Research and Quality. September 2021. www.ncbi.nlm.nih.gov/books/NBK574045
30. CDC. Update to CDC’s sexually transmitted diseases treatment guidelines, 2006: fluoroquinolones no longer recommended for treatment of gonococcal infections. MMWR Morb Mortal Wkly Rep. 2007;56:332-336.
31. Rowley J, Vander Hoorn S, Korenromp E, et al. Chlamydia, gonorrhoea, trichomoniasis and syphilis: global prevalence and incidence estimates, 2016. Bull World Health Organ. 2019:97:548-562P. doi: 10.2471/BLT.18.228486
32. Patel EU, Gaydos CA, Packman ZR, et al. Prevalence and correlates of Trichomonas vaginalis infection among men and women in the United States. Clin Infect Dis. 2018;67:211-217. doi: 10.1093/cid/ciy079
33. CDC. Sexually transmitted infections treatment guidelines, 2021. Mycoplasma genitalium. US Department of Health and Human Services. July 22, 2021. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/mycoplasmagenitalium.htm
34. Manhart LE, Broad JM, Bolden MR. Mycoplasma genitalium: should we treat and how? Clin Infect Dis. 2011;53(suppl 3):S129-S142. doi:10.1093/cid/cir702.
35. Corey L, Wald A. Genital herpes. In: Holmes KK, Sparling PF, Stamm WE, et al, eds. Sexually Transmitted Diseases. 4th ed. McGraw-Hill; 2008:399-437.
36. CDC. Sexually transmitted infections treatment guidelines, 2021: Genital herpes. US Department of Health and Human Services. September 21, 2022. Accessed April 23, 2023. www.cdc.gov/std/treatment-guidelines/herpes.htm
37. Looker KJ, Elmes JAR, Gottlieb SL, et al. Effect of HSV-2 infection on subsequent HIV acquisition: an updated systematic review and meta-analysis. Lancet Infect Dis. 2017;17:1303-1316. doi: 10.1016/S1473-3099(17)30405-X
38. Rollenhagen C, Lathrop M, Macura SL, et al. Herpes simplex virus type-2 stimulates HIV-1 replication in cervical tissues: implications for HIV-1 transmission and efficacy of anti-HIV-1 microbicides. Mucosal Immunol. 2014;7:1165-1174. doi: 10.1038/mi.2014.3
39. Cogliano V, Baan R, Straif K, et al; WHO International Agency for Research on Cancer. Carcinogenicity of human papillomaviruses. Lancet Oncol.
40. Simon MA, Tseng CW, Wong JB. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320:674-686. doi:10.1001/jama.2018.10897
41. Perkins RB, Guido RS, Castle PE, et al; . 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors. J Low Genit Tract Dis. 2020;24:102-131. doi: 10.1097/LGT.0000000000000525
42. Meites E, Szilagyi PG, Chesson HW, et al. Human papillomavirus vaccination for adults: updated recommendations of the Advisory Committee on Immunization Practices. MMWR Morb Mortal Wkly Rep. 2019;68:698-702. doi: 10.15585/mmwr.mm6832a3
43. Schmidt R, Carson PJ, Jansen RJ. Resurgence of syphilis in the United States: an assessment of contributing factors. Infect Dis (Auckl). 2019;12:1178633719883282. doi: 10.1177/1178633719883282
44. Boog GHP, Lopes JVZ, Mahler JV, et al. Diagnostic tools for neurosyphilis: a systematic review. BMC Infect Dis. 2021;21:568. doi: 10.1186/s12879-021-06264-8
45. CDC. Sexually transmitted infections treatment guidelines, 2021. Syphilis. US Department of Health and Human Services. April 20, 2023. Accessed April 24, 2023. www.cdc.gov/std/treatment-guidelines/syphilis.htm
46. Matthias JM, Rahman MM, Newman DR, et al. Effectiveness of prenatal screening and treatment to prevent congenital syphilis, Louisiana and Florida, 2013-2014. Sex Transm Dis. 2017;44:498-502. doi: 10.1097/OLQ.0000000000000638
47. Clement ME, Okeke NL, Hicks CB. Treatment of syphilis: a systematic review. JAMA. 2014;312:1905-1917. doi: 10.1001/jama.2014.13259
48. Davidson KW, Barry MJ, Mangione CM, et al; US Preventive Services Task Force. Screening for chlamydia and gonorrhea: US Preventive Services Task Force recommendation statement. JAMA. 2021;326:949-956. doi: 10.1001/jama.2021.14081
49. Krist AH, Davidson KW, Mangione CM, et al; US Preventive Services Task Force. Screening for hepatitis B virus infection in adolescents and adults: US Preventive Services Task Force recommendation statement. JAMA. 2020;324:2415-2422. doi: 10.1001/jama.2020.22980
50. Owens DK, Davidson KW, Krist AH, et al; US Preventive Services Task Force. Screening for hepatitis C virus infection in adolescents and adults: US Preventive Services Task Force recommendation statement. JAMA. 2020;323:970-975. doi: 10.1001/jama.2020.1123
51. Bibbins-Domingo K, Grossman DC, Curry SJ, et al; US Preventive Services Task Force. Serologic screening for genital herpes infection: US Preventive Services Task Force recommendation statement. JAMA. 2016;316:2525-2530. doi: 10.1001/jama.2016.16776
52. Curry SJ, Krist AH, Owens DK, et al; US Preventive Services Task Force. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320:674-686. doi: 10.1001/jama.2018.10897
53. Owens DK, Davidson KW, Krist AH, et al; US Preventive Services Task Force. Screening for HIV infection: US Preventive Services Task Force recommendation statement. JAMA. 2019;321:2326-2336. doi: 10.1001/jama.2019.6587
54. Farley TA, Cohen DA, Elkins W. Asymptomatic sexually transmitted diseases: the case for screening. Prev Med. 2003;36:502-509. doi: 10.1016/s0091-7435(02)00058-0
55. US Public Health Service. Preexposure prophylaxis for the prevention of HIV infection in the United States—2021 update. A clinical practice guideline. Centers for Disease Control and Prevention. Accessed April 24, 2023. www.cdc.gov/hiv/pdf/risk/prep/cdc-hiv-prep-guidelines-2021.pdf
56. CDC. Sexually transmitted infections treatment guidelines, 2021: Sexual assault and abuse and STIs—adolescents and adults, 2021. US Department of Health and Human Services. July 22, 2021. Accessed April 24, 2023. www.cdc.gov/std/treatment-guidelines/sexual-assault-adults.htm
PRACTICE RECOMMENDATIONS
› Focus efforts to prevent sexually transmitted infections (STIs) on patients ages 15 to 24 years—because half of new STIs in the United States occur in this age group. A
› Screen for other STIs, including HIV infection, if a person tests positive for a single STI. A
› Treat STIs by following updated (2021) guidelines developed by the Centers for Disease Control and Prevention. A
Strength of recommendation (SOR)
A Good-quality patient-oriented evidence
B Inconsistent or limited-quality patient-oriented evidence
C Consensus, usual practice, opinion, disease-oriented evidence, case series
25 years of Viagra: A huge change in attitudes about ED
This transcript has been edited for clarity.
Incredibly, 25 years ago, Bob Dole, a senator from Kansas at the time and former presidential candidate, went on national television in a commercial and discussed the fact that he was sexually impotent. You might be thinking, “What was happening then? Was this an early Jerry Springer experience or reality TV gone haywire?” No. Viagra was approved as a treatment 25 years ago this year.
Bob Dole was recruited by Pfizer, the manufacturer of Viagra, to do commercials in which he discussed his sexual dysfunction. He was recruited for a very specific set of reasons. First, he was a distinguished, prominent, respected national figure. Second, he was conservative.
For those of you who don’t remember, when 25 years ago Viagra first appeared, Pfizer was terrified that they would get attacked for promoting promiscuity by introducing a sex pill onto the market. Bob Dole was basically saying, “I have a medical problem. It’s tough to talk about, but there is a treatment. I’m going to discuss the fact that I, among many other men, could use this to help that problem.”
He was used in a way to deflect conservative or religious critics worried about the promotion of sex outside of marriage. Bob Dole was also well known to be married to Elizabeth Dole. This wasn’t somebody who was out on the dating market. Bob Dole was a family man, and his selection was no accident. For all these reasons, Bob Dole was the first spokesperson for Viagra.
Now, as it happens, I had a role to play with this drug. Pfizer called me up and asked me to come and do a consult with them about the ethics of this brand-new treatment. I had never been asked by a drug company to do anything like this. I didn’t know what I was doing. I thought about it and said: “I’ll do it if you let me sit in on discussions and meetings at your New York headquarters about this drug. I want open access.”
I assume they gave me open access. I went to many meetings before the Food and Drug Administration approved Viagra, and many discussions took place about how to roll it out. Once I got there, the one thing I insisted upon was that they had to be treating a disease. If they didn’t want to get involved in criticisms about this new miracle solution to the age-old problem of sexual dysfunction, impotence wouldn’t do. It wasn’t a medical diagnosis, and it was kind of a very undefined situation.
Erectile dysfunction was the answer. They met with urologists, sex experts, and individuals within the company and came up with the idea that if you were unable to have an erection after trying for 6 months or more, you suffered from erectile dysfunction, and that was the group for whom they should market Viagra. I fully agreed with that.
What happened was that probably hundreds of millions of men worldwide came forward for the first time and said, “I’m ashamed and guilty. I feel stigmatized. Now, with something that might help me, I’m going to say to my doctor, I have this problem.”
It’s a very important lesson because 25 years later, it’s still difficult for people – men and women – to discuss sexual problems, sexual dysfunction, and unhappiness with their sex life. I know we’ve gotten better at asking about this, but it’s still difficult for patients to go into it, bring it up, and talk about it. It’s something that we have to think hard about how we bring forward, honest, frank conversation and make people comfortable so they can tell us.
One thing that Viagra proved to the world is that not only is there a large amount of sexual dysfunction – some numbers as high as 35% of men over age 65 – but that sexual dysfunction is related to diseases. It’s caused by hypertension, hardening of the arteries, and diabetes. It may be caused by psychological anxiety or even just a poor relationship where things are falling apart.
I think it’s important that, when Viagra first appeared, what Pfizer tried to do and with the marketing oriented around it was treating it as a disease, trying to treat erectile dysfunction as a symptom, and then trying to explore the underlying possible causes for that symptom.
Sadly, if we look today, we have come a long way – and not always a good way – from where Viagra started. Viagra is easily available online. Many companies say, just get online and a doctor will talk with you about a prescription. They do, but they don’t explore the underlying causes anymore online of what might be causing the erectile dysfunction. They certainly may have a checkbox and ask somebody about this or that, but I’ve gone and tested the sites, and you can get a prescription in about 30 seconds.
It’s not really gone with the old medical model that accompanied the appearance of Viagra. We now treat it as a recreational drug or an aphrodisiac, none of which is true. If your body is working properly, blood will flow where it’s going to go. Taking Viagra or any of the other treatments will not help improve that or enhance that.
The other problem I see today with where we are with these impotence and erectile dysfunction drugs is that we still have not developed a full array of interventions for women. It’s true that men have Viagra, and it’s true that that’s often reimbursed. We still have women complaining that they have sexual dysfunction or loss of interest or whatever the problem might be, and we haven’t been able to develop drugs that will help them.
Since Viagra’s approval 25 years ago until the patent ran out in 2019, $40 billion worth of the drug has been sold. Its advertising has shifted so that
Doctors always need to be thinking about exploring that and trying to get a vision or a view of the health of their patients. It’s still hard for many people to speak up and say if they’re having problems in bed, and we want to make sure that we try our best to make that happen.
Overall, I think the approval of Viagra 25 years ago was a very good thing. It brought a terrible problem out into the open. It helped enhance the quality of life for many men. Despite where we are today, I think the introduction of that pill was actually a major achievement in pharmacology.
Dr. Kaplan is director, division of medical ethics, New York University Langone Medical Center, New York. He reported conflicts of interest with Johnson & Johnson, Medscape, and Pfizer.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
Incredibly, 25 years ago, Bob Dole, a senator from Kansas at the time and former presidential candidate, went on national television in a commercial and discussed the fact that he was sexually impotent. You might be thinking, “What was happening then? Was this an early Jerry Springer experience or reality TV gone haywire?” No. Viagra was approved as a treatment 25 years ago this year.
Bob Dole was recruited by Pfizer, the manufacturer of Viagra, to do commercials in which he discussed his sexual dysfunction. He was recruited for a very specific set of reasons. First, he was a distinguished, prominent, respected national figure. Second, he was conservative.
For those of you who don’t remember, when 25 years ago Viagra first appeared, Pfizer was terrified that they would get attacked for promoting promiscuity by introducing a sex pill onto the market. Bob Dole was basically saying, “I have a medical problem. It’s tough to talk about, but there is a treatment. I’m going to discuss the fact that I, among many other men, could use this to help that problem.”
He was used in a way to deflect conservative or religious critics worried about the promotion of sex outside of marriage. Bob Dole was also well known to be married to Elizabeth Dole. This wasn’t somebody who was out on the dating market. Bob Dole was a family man, and his selection was no accident. For all these reasons, Bob Dole was the first spokesperson for Viagra.
Now, as it happens, I had a role to play with this drug. Pfizer called me up and asked me to come and do a consult with them about the ethics of this brand-new treatment. I had never been asked by a drug company to do anything like this. I didn’t know what I was doing. I thought about it and said: “I’ll do it if you let me sit in on discussions and meetings at your New York headquarters about this drug. I want open access.”
I assume they gave me open access. I went to many meetings before the Food and Drug Administration approved Viagra, and many discussions took place about how to roll it out. Once I got there, the one thing I insisted upon was that they had to be treating a disease. If they didn’t want to get involved in criticisms about this new miracle solution to the age-old problem of sexual dysfunction, impotence wouldn’t do. It wasn’t a medical diagnosis, and it was kind of a very undefined situation.
Erectile dysfunction was the answer. They met with urologists, sex experts, and individuals within the company and came up with the idea that if you were unable to have an erection after trying for 6 months or more, you suffered from erectile dysfunction, and that was the group for whom they should market Viagra. I fully agreed with that.
What happened was that probably hundreds of millions of men worldwide came forward for the first time and said, “I’m ashamed and guilty. I feel stigmatized. Now, with something that might help me, I’m going to say to my doctor, I have this problem.”
It’s a very important lesson because 25 years later, it’s still difficult for people – men and women – to discuss sexual problems, sexual dysfunction, and unhappiness with their sex life. I know we’ve gotten better at asking about this, but it’s still difficult for patients to go into it, bring it up, and talk about it. It’s something that we have to think hard about how we bring forward, honest, frank conversation and make people comfortable so they can tell us.
One thing that Viagra proved to the world is that not only is there a large amount of sexual dysfunction – some numbers as high as 35% of men over age 65 – but that sexual dysfunction is related to diseases. It’s caused by hypertension, hardening of the arteries, and diabetes. It may be caused by psychological anxiety or even just a poor relationship where things are falling apart.
I think it’s important that, when Viagra first appeared, what Pfizer tried to do and with the marketing oriented around it was treating it as a disease, trying to treat erectile dysfunction as a symptom, and then trying to explore the underlying possible causes for that symptom.
Sadly, if we look today, we have come a long way – and not always a good way – from where Viagra started. Viagra is easily available online. Many companies say, just get online and a doctor will talk with you about a prescription. They do, but they don’t explore the underlying causes anymore online of what might be causing the erectile dysfunction. They certainly may have a checkbox and ask somebody about this or that, but I’ve gone and tested the sites, and you can get a prescription in about 30 seconds.
It’s not really gone with the old medical model that accompanied the appearance of Viagra. We now treat it as a recreational drug or an aphrodisiac, none of which is true. If your body is working properly, blood will flow where it’s going to go. Taking Viagra or any of the other treatments will not help improve that or enhance that.
The other problem I see today with where we are with these impotence and erectile dysfunction drugs is that we still have not developed a full array of interventions for women. It’s true that men have Viagra, and it’s true that that’s often reimbursed. We still have women complaining that they have sexual dysfunction or loss of interest or whatever the problem might be, and we haven’t been able to develop drugs that will help them.
Since Viagra’s approval 25 years ago until the patent ran out in 2019, $40 billion worth of the drug has been sold. Its advertising has shifted so that
Doctors always need to be thinking about exploring that and trying to get a vision or a view of the health of their patients. It’s still hard for many people to speak up and say if they’re having problems in bed, and we want to make sure that we try our best to make that happen.
Overall, I think the approval of Viagra 25 years ago was a very good thing. It brought a terrible problem out into the open. It helped enhance the quality of life for many men. Despite where we are today, I think the introduction of that pill was actually a major achievement in pharmacology.
Dr. Kaplan is director, division of medical ethics, New York University Langone Medical Center, New York. He reported conflicts of interest with Johnson & Johnson, Medscape, and Pfizer.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
Incredibly, 25 years ago, Bob Dole, a senator from Kansas at the time and former presidential candidate, went on national television in a commercial and discussed the fact that he was sexually impotent. You might be thinking, “What was happening then? Was this an early Jerry Springer experience or reality TV gone haywire?” No. Viagra was approved as a treatment 25 years ago this year.
Bob Dole was recruited by Pfizer, the manufacturer of Viagra, to do commercials in which he discussed his sexual dysfunction. He was recruited for a very specific set of reasons. First, he was a distinguished, prominent, respected national figure. Second, he was conservative.
For those of you who don’t remember, when 25 years ago Viagra first appeared, Pfizer was terrified that they would get attacked for promoting promiscuity by introducing a sex pill onto the market. Bob Dole was basically saying, “I have a medical problem. It’s tough to talk about, but there is a treatment. I’m going to discuss the fact that I, among many other men, could use this to help that problem.”
He was used in a way to deflect conservative or religious critics worried about the promotion of sex outside of marriage. Bob Dole was also well known to be married to Elizabeth Dole. This wasn’t somebody who was out on the dating market. Bob Dole was a family man, and his selection was no accident. For all these reasons, Bob Dole was the first spokesperson for Viagra.
Now, as it happens, I had a role to play with this drug. Pfizer called me up and asked me to come and do a consult with them about the ethics of this brand-new treatment. I had never been asked by a drug company to do anything like this. I didn’t know what I was doing. I thought about it and said: “I’ll do it if you let me sit in on discussions and meetings at your New York headquarters about this drug. I want open access.”
I assume they gave me open access. I went to many meetings before the Food and Drug Administration approved Viagra, and many discussions took place about how to roll it out. Once I got there, the one thing I insisted upon was that they had to be treating a disease. If they didn’t want to get involved in criticisms about this new miracle solution to the age-old problem of sexual dysfunction, impotence wouldn’t do. It wasn’t a medical diagnosis, and it was kind of a very undefined situation.
Erectile dysfunction was the answer. They met with urologists, sex experts, and individuals within the company and came up with the idea that if you were unable to have an erection after trying for 6 months or more, you suffered from erectile dysfunction, and that was the group for whom they should market Viagra. I fully agreed with that.
What happened was that probably hundreds of millions of men worldwide came forward for the first time and said, “I’m ashamed and guilty. I feel stigmatized. Now, with something that might help me, I’m going to say to my doctor, I have this problem.”
It’s a very important lesson because 25 years later, it’s still difficult for people – men and women – to discuss sexual problems, sexual dysfunction, and unhappiness with their sex life. I know we’ve gotten better at asking about this, but it’s still difficult for patients to go into it, bring it up, and talk about it. It’s something that we have to think hard about how we bring forward, honest, frank conversation and make people comfortable so they can tell us.
One thing that Viagra proved to the world is that not only is there a large amount of sexual dysfunction – some numbers as high as 35% of men over age 65 – but that sexual dysfunction is related to diseases. It’s caused by hypertension, hardening of the arteries, and diabetes. It may be caused by psychological anxiety or even just a poor relationship where things are falling apart.
I think it’s important that, when Viagra first appeared, what Pfizer tried to do and with the marketing oriented around it was treating it as a disease, trying to treat erectile dysfunction as a symptom, and then trying to explore the underlying possible causes for that symptom.
Sadly, if we look today, we have come a long way – and not always a good way – from where Viagra started. Viagra is easily available online. Many companies say, just get online and a doctor will talk with you about a prescription. They do, but they don’t explore the underlying causes anymore online of what might be causing the erectile dysfunction. They certainly may have a checkbox and ask somebody about this or that, but I’ve gone and tested the sites, and you can get a prescription in about 30 seconds.
It’s not really gone with the old medical model that accompanied the appearance of Viagra. We now treat it as a recreational drug or an aphrodisiac, none of which is true. If your body is working properly, blood will flow where it’s going to go. Taking Viagra or any of the other treatments will not help improve that or enhance that.
The other problem I see today with where we are with these impotence and erectile dysfunction drugs is that we still have not developed a full array of interventions for women. It’s true that men have Viagra, and it’s true that that’s often reimbursed. We still have women complaining that they have sexual dysfunction or loss of interest or whatever the problem might be, and we haven’t been able to develop drugs that will help them.
Since Viagra’s approval 25 years ago until the patent ran out in 2019, $40 billion worth of the drug has been sold. Its advertising has shifted so that
Doctors always need to be thinking about exploring that and trying to get a vision or a view of the health of their patients. It’s still hard for many people to speak up and say if they’re having problems in bed, and we want to make sure that we try our best to make that happen.
Overall, I think the approval of Viagra 25 years ago was a very good thing. It brought a terrible problem out into the open. It helped enhance the quality of life for many men. Despite where we are today, I think the introduction of that pill was actually a major achievement in pharmacology.
Dr. Kaplan is director, division of medical ethics, New York University Langone Medical Center, New York. He reported conflicts of interest with Johnson & Johnson, Medscape, and Pfizer.
A version of this article first appeared on Medscape.com.
FDA approves new device for enlarged prostate treatment
Designed and marketed by Urotronic (Plymouth, Minn.), the Optilume BPH Catheter System employs mechanical dilation to relieve obstruction of the prostate and then delivers paclitaxel to aid in prostate healing. The device is used in an outpatient setting and is less invasive than other procedures.
“There’s nothing else like Optilume BPH that’s currently available, it’s the only treatment option that requires no cutting, burning, steaming, or implants,” said Urotronic President and CEO David Perry in a press release.
Two randomized trials, EVEREST-1 and PINNACLE, both showed that the Optilume BPH system improved urinary flow rate and decreased the amount of urine stored in the bladder following urination. Men who used the OPTILUME device were able to ejaculate normally and reported no sexual difficulties.
“Optilume BPH is the next generation of minimally invasive technology, creating a new drug device space among BPH therapies,” Steven A. Kaplan, MD, professor of urology at the Icahn School of Medicine at Mount Sinai, New York, said in the press release. Dr. Kaplan led the EVEREST-1 and PINNACLE studies, which Urotronic funded.
More than 80% of men older than age 70 have an enlarged prostate, based on autopsy analyses.
A version of this article first appeared on Medscape.com.
Designed and marketed by Urotronic (Plymouth, Minn.), the Optilume BPH Catheter System employs mechanical dilation to relieve obstruction of the prostate and then delivers paclitaxel to aid in prostate healing. The device is used in an outpatient setting and is less invasive than other procedures.
“There’s nothing else like Optilume BPH that’s currently available, it’s the only treatment option that requires no cutting, burning, steaming, or implants,” said Urotronic President and CEO David Perry in a press release.
Two randomized trials, EVEREST-1 and PINNACLE, both showed that the Optilume BPH system improved urinary flow rate and decreased the amount of urine stored in the bladder following urination. Men who used the OPTILUME device were able to ejaculate normally and reported no sexual difficulties.
“Optilume BPH is the next generation of minimally invasive technology, creating a new drug device space among BPH therapies,” Steven A. Kaplan, MD, professor of urology at the Icahn School of Medicine at Mount Sinai, New York, said in the press release. Dr. Kaplan led the EVEREST-1 and PINNACLE studies, which Urotronic funded.
More than 80% of men older than age 70 have an enlarged prostate, based on autopsy analyses.
A version of this article first appeared on Medscape.com.
Designed and marketed by Urotronic (Plymouth, Minn.), the Optilume BPH Catheter System employs mechanical dilation to relieve obstruction of the prostate and then delivers paclitaxel to aid in prostate healing. The device is used in an outpatient setting and is less invasive than other procedures.
“There’s nothing else like Optilume BPH that’s currently available, it’s the only treatment option that requires no cutting, burning, steaming, or implants,” said Urotronic President and CEO David Perry in a press release.
Two randomized trials, EVEREST-1 and PINNACLE, both showed that the Optilume BPH system improved urinary flow rate and decreased the amount of urine stored in the bladder following urination. Men who used the OPTILUME device were able to ejaculate normally and reported no sexual difficulties.
“Optilume BPH is the next generation of minimally invasive technology, creating a new drug device space among BPH therapies,” Steven A. Kaplan, MD, professor of urology at the Icahn School of Medicine at Mount Sinai, New York, said in the press release. Dr. Kaplan led the EVEREST-1 and PINNACLE studies, which Urotronic funded.
More than 80% of men older than age 70 have an enlarged prostate, based on autopsy analyses.
A version of this article first appeared on Medscape.com.
Men and women react differently to acute stress
Topline
Methodology
- The study included 80 healthy participants, mean age 24 years.
- Half the subjects immersed their nondominant hand (including the wrist) in ice water for up to 3 minutes; the other half, which served as the control group, immersed their hand in warm water for 3 minutes.
- Participants were asked to deliberately downregulate emotional responses to high-intensity negative pictures.
- Participants regularly provided saliva samples to check cortisol levels and were monitored for cardiovascular activity.
- Researchers assessed pupil dilation, which along with subject ratings of their affective state served as emotion regulation (ER) outcome measures.
Takeaway
- In men, stress rapidly improved the ability to downregulate emotional arousal via distraction that was fully mediated by cortisol.
- In women, sympathetic nervous system (SNS) reactivity was linked to decreased regulatory performances.
- Direct stress effects on ER were smaller than expected.
In practice
The study contributes to a “better understanding of the neuroendocrinological mechanisms of stress effects on ER that may help to develop adequate preventive and curative interventions of stress- and emotion-related disorders,” the researchers write.
Source
The study was conducted by Katja Langer, Valerie Jentsch, and Oliver Wolf from the Department of Cognitive Psychology, Ruhr University Bochum (Germany). It was published in the May 2023 issue of Psychoneuroendocrinology.
Limitations
The results have some inconsistencies. The ER paradigm is somewhat artificial and not fully comparable with emotional trigger and regulatory requirements in everyday life. The study did not directly assess levels of catecholamines such as adrenaline and noradrenaline.
Disclosures
The study received support from the German Research Foundation (DFG). The authors have no reported conflicts of interest.
A version of this article originally appeared on Medscape.com.
Topline
Methodology
- The study included 80 healthy participants, mean age 24 years.
- Half the subjects immersed their nondominant hand (including the wrist) in ice water for up to 3 minutes; the other half, which served as the control group, immersed their hand in warm water for 3 minutes.
- Participants were asked to deliberately downregulate emotional responses to high-intensity negative pictures.
- Participants regularly provided saliva samples to check cortisol levels and were monitored for cardiovascular activity.
- Researchers assessed pupil dilation, which along with subject ratings of their affective state served as emotion regulation (ER) outcome measures.
Takeaway
- In men, stress rapidly improved the ability to downregulate emotional arousal via distraction that was fully mediated by cortisol.
- In women, sympathetic nervous system (SNS) reactivity was linked to decreased regulatory performances.
- Direct stress effects on ER were smaller than expected.
In practice
The study contributes to a “better understanding of the neuroendocrinological mechanisms of stress effects on ER that may help to develop adequate preventive and curative interventions of stress- and emotion-related disorders,” the researchers write.
Source
The study was conducted by Katja Langer, Valerie Jentsch, and Oliver Wolf from the Department of Cognitive Psychology, Ruhr University Bochum (Germany). It was published in the May 2023 issue of Psychoneuroendocrinology.
Limitations
The results have some inconsistencies. The ER paradigm is somewhat artificial and not fully comparable with emotional trigger and regulatory requirements in everyday life. The study did not directly assess levels of catecholamines such as adrenaline and noradrenaline.
Disclosures
The study received support from the German Research Foundation (DFG). The authors have no reported conflicts of interest.
A version of this article originally appeared on Medscape.com.
Topline
Methodology
- The study included 80 healthy participants, mean age 24 years.
- Half the subjects immersed their nondominant hand (including the wrist) in ice water for up to 3 minutes; the other half, which served as the control group, immersed their hand in warm water for 3 minutes.
- Participants were asked to deliberately downregulate emotional responses to high-intensity negative pictures.
- Participants regularly provided saliva samples to check cortisol levels and were monitored for cardiovascular activity.
- Researchers assessed pupil dilation, which along with subject ratings of their affective state served as emotion regulation (ER) outcome measures.
Takeaway
- In men, stress rapidly improved the ability to downregulate emotional arousal via distraction that was fully mediated by cortisol.
- In women, sympathetic nervous system (SNS) reactivity was linked to decreased regulatory performances.
- Direct stress effects on ER were smaller than expected.
In practice
The study contributes to a “better understanding of the neuroendocrinological mechanisms of stress effects on ER that may help to develop adequate preventive and curative interventions of stress- and emotion-related disorders,” the researchers write.
Source
The study was conducted by Katja Langer, Valerie Jentsch, and Oliver Wolf from the Department of Cognitive Psychology, Ruhr University Bochum (Germany). It was published in the May 2023 issue of Psychoneuroendocrinology.
Limitations
The results have some inconsistencies. The ER paradigm is somewhat artificial and not fully comparable with emotional trigger and regulatory requirements in everyday life. The study did not directly assess levels of catecholamines such as adrenaline and noradrenaline.
Disclosures
The study received support from the German Research Foundation (DFG). The authors have no reported conflicts of interest.
A version of this article originally appeared on Medscape.com.
Methotrexate does not impair sperm quality, small study finds
TOPLINE:
Methotrexate (MTX) is not associated with testicular toxicity, so therapy can be safety started in men pursuing parenthood, a small study finds.
METHODOLOGY:
- Lack of evidence regarding MTX’s effect on sperm quality has resulted in inconsistent recommendations for men actively pursuing parenthood.
- Researchers enrolled 20 men aged 18 years or older with an immune-mediated inflammatory disease (IMID) who were about to begin MTX therapy and 25 healthy men as controls.
- Participants provided semen samples prior to beginning MTX therapy and 13 weeks after beginning therapy.
- Researchers tested samples in both groups for markers of testicular toxicity.
- Also evaluated whether MTX polyglutamates could be detected in sperm of seminal fluid, as a secondary outcome.
TAKEAWAY:
- Found no significant differences in conventional semen parameters, sperm DNA damage, or male reproductive endocrine axis between the MTX group and controls.
- The concentration of MTX polyglutamates is low in both sperm and seminal fluid and is particularly low in sperm.
IN PRACTICE:
“Therapy with MTX can be safely started or continued in men diagnosed with an IMID and with an active wish to become a father,” the authors write.
STUDY DETAILS:
Luis Fernando Perez-Garcia, MD, Erasmus Medical Center, Rotterdam, the Netherlands, led the research. The study was published online in Annals of the Rheumatic Diseases on June 1, 2023.
LIMITATIONS:
The small number of participants and that the study included only MTX starters and not those who have taken MTX longer term.
DISCLOSURES:
Grants from the Dutch Arthritis Foundation, The Netherlands Organization for Health Research and Development, and Consejo Nacional de Ciencia y Tecnologia funded the project. Researchers disclosed financial relationships with Galapagos NV and UCB.
A version of this article first appeared on Medscape.com.
TOPLINE:
Methotrexate (MTX) is not associated with testicular toxicity, so therapy can be safety started in men pursuing parenthood, a small study finds.
METHODOLOGY:
- Lack of evidence regarding MTX’s effect on sperm quality has resulted in inconsistent recommendations for men actively pursuing parenthood.
- Researchers enrolled 20 men aged 18 years or older with an immune-mediated inflammatory disease (IMID) who were about to begin MTX therapy and 25 healthy men as controls.
- Participants provided semen samples prior to beginning MTX therapy and 13 weeks after beginning therapy.
- Researchers tested samples in both groups for markers of testicular toxicity.
- Also evaluated whether MTX polyglutamates could be detected in sperm of seminal fluid, as a secondary outcome.
TAKEAWAY:
- Found no significant differences in conventional semen parameters, sperm DNA damage, or male reproductive endocrine axis between the MTX group and controls.
- The concentration of MTX polyglutamates is low in both sperm and seminal fluid and is particularly low in sperm.
IN PRACTICE:
“Therapy with MTX can be safely started or continued in men diagnosed with an IMID and with an active wish to become a father,” the authors write.
STUDY DETAILS:
Luis Fernando Perez-Garcia, MD, Erasmus Medical Center, Rotterdam, the Netherlands, led the research. The study was published online in Annals of the Rheumatic Diseases on June 1, 2023.
LIMITATIONS:
The small number of participants and that the study included only MTX starters and not those who have taken MTX longer term.
DISCLOSURES:
Grants from the Dutch Arthritis Foundation, The Netherlands Organization for Health Research and Development, and Consejo Nacional de Ciencia y Tecnologia funded the project. Researchers disclosed financial relationships with Galapagos NV and UCB.
A version of this article first appeared on Medscape.com.
TOPLINE:
Methotrexate (MTX) is not associated with testicular toxicity, so therapy can be safety started in men pursuing parenthood, a small study finds.
METHODOLOGY:
- Lack of evidence regarding MTX’s effect on sperm quality has resulted in inconsistent recommendations for men actively pursuing parenthood.
- Researchers enrolled 20 men aged 18 years or older with an immune-mediated inflammatory disease (IMID) who were about to begin MTX therapy and 25 healthy men as controls.
- Participants provided semen samples prior to beginning MTX therapy and 13 weeks after beginning therapy.
- Researchers tested samples in both groups for markers of testicular toxicity.
- Also evaluated whether MTX polyglutamates could be detected in sperm of seminal fluid, as a secondary outcome.
TAKEAWAY:
- Found no significant differences in conventional semen parameters, sperm DNA damage, or male reproductive endocrine axis between the MTX group and controls.
- The concentration of MTX polyglutamates is low in both sperm and seminal fluid and is particularly low in sperm.
IN PRACTICE:
“Therapy with MTX can be safely started or continued in men diagnosed with an IMID and with an active wish to become a father,” the authors write.
STUDY DETAILS:
Luis Fernando Perez-Garcia, MD, Erasmus Medical Center, Rotterdam, the Netherlands, led the research. The study was published online in Annals of the Rheumatic Diseases on June 1, 2023.
LIMITATIONS:
The small number of participants and that the study included only MTX starters and not those who have taken MTX longer term.
DISCLOSURES:
Grants from the Dutch Arthritis Foundation, The Netherlands Organization for Health Research and Development, and Consejo Nacional de Ciencia y Tecnologia funded the project. Researchers disclosed financial relationships with Galapagos NV and UCB.
A version of this article first appeared on Medscape.com.
Anabolic-steroid withdrawal regimens show promise in men
Men who illicitly used anabolic-androgenic steroids to bulk up and then turned to illegal, web-based regimens for treating their steroid withdrawal complications have provided important clues for new approaches to treating a growing worldwide population of men who abuse steroids.
A retrospective, observational study at one steroid addiction center in Glasgow examined 641 men who had stopped using steroids within the prior 3 years in 2015-2022 and who had self-administered certain agents, collectively known as post-cycle therapy (PCT) – within 3 months of stopping steroids.
They had a significant 3.8-fold increased rate of normalization of their levels of testosterone, luteinizing hormone (LH), and follicle-stimulating hormone (FSH), compared with men who either never used PCT or began it more than 3 months after stopping steroids, Channa N. Jayasena, PhD, MRCP, FRCPath, reported at the annual meeting of the Endocrine Society.
These testosterone, LH, and FSH levels served as a “surrogate marker of biochemical recovery from hypogonadism,” he explained. Normalization also occurred “slightly sooner” in men who began using PCT early after steroid cessation, added Dr. Jayasena, a reproductive endocrinologist at Imperial College, London.
When men recovered their endogenous testosterone-producing capacity, it occurred after an average of about 13 weeks on PCT and after an average of about 19 weeks without PCT, a significant difference.
“There is a vacuum of medical advice on what to do” when men stop taking steroids, said Dr. Jayasena during a press briefing at the meeting. “We can’t recommend anything yet because [our studies] have not proven causality” between the post-cycle therapy that many men start after stopping steroids and any symptom improvement they experience.”
The next step is to test the PCT agents in a prospective, controlled study, an investigation Dr. Jayasena and colleagues are eager to launch. The goal is to determine whether PCT is truly effective, the optimal doses, and whether the treatments are safe.
‘Incredibly sophisticated’ online community
The agents that constitute PCT include human chorionic gonadotropin (hCG, the “pregnancy hormone”), selective estrogen receptor modulators (SERMs), and aromatase inhibitors (AIs). SERMs and AIs are licensed only for use in women, the former for osteoporosis and breast cancer and the latter for breast cancer.
All of these agents, as well as others, are advertised by various illegal websites as treatments that can restore endogenous testosterone production in men whose native testosterone shut down during their steroid self-medication.
Restored testosterone resolves many of the adverse effects of steroid withdrawal such as diminished libido and erections, and depressed mood and energy.
Men buy PCT agents illegally from various websites. “There is an enormous, incredibly sophisticated community online that influences” PCT, and an “incredibly refined worldwide distribution network,” Dr. Jayasena explained.
His study included 410 men who turned to PCT after steroid cessation and 170 who did not.
Largest study of hormone recovery when men stop taking steroids
In a further multivariate analysis of the observational data, men who had used four or more different steroid treatments fared worse – with a significant 75% reduced rate of testosterone normalization with PCT – compared with men who had used a single steroid agent.
And men who had been on a steroid regimen for more than 6 months also fared badly – with a significant 66% reduced rate of testosterone normalization with PCT, compared with men on a steroid regimen for 3 months or less.
“This is the largest study of hormone recovery when men stop taking steroids,” Dr. Jayasena noted.
And the data “require corroboration within an interventional study to determine causality.”
“We need further studies to help doctors and other health care professionals advise men about the risks of anabolic steroid use and support those who are motivated to stop,” Dr. Jayasena said.
He cautioned that the study has several limitations: biases were potentially introduced based on recruitment and on recall by participants; clinicians drew blood specimens used to measure hormone levels at random times; and participants may have engaged in concealed drug use and used steroid and PCT agents that did not contain the substances advertised.
Nevertheless,, and they “may have important therapeutic implications for the future treatment of men who are motivated to stop” steroids.
The study received no commercial funding. Dr. Jayasena has received research funding from Logixx Pharma.
A version of this article first appeared on Medscape.com.
Men who illicitly used anabolic-androgenic steroids to bulk up and then turned to illegal, web-based regimens for treating their steroid withdrawal complications have provided important clues for new approaches to treating a growing worldwide population of men who abuse steroids.
A retrospective, observational study at one steroid addiction center in Glasgow examined 641 men who had stopped using steroids within the prior 3 years in 2015-2022 and who had self-administered certain agents, collectively known as post-cycle therapy (PCT) – within 3 months of stopping steroids.
They had a significant 3.8-fold increased rate of normalization of their levels of testosterone, luteinizing hormone (LH), and follicle-stimulating hormone (FSH), compared with men who either never used PCT or began it more than 3 months after stopping steroids, Channa N. Jayasena, PhD, MRCP, FRCPath, reported at the annual meeting of the Endocrine Society.
These testosterone, LH, and FSH levels served as a “surrogate marker of biochemical recovery from hypogonadism,” he explained. Normalization also occurred “slightly sooner” in men who began using PCT early after steroid cessation, added Dr. Jayasena, a reproductive endocrinologist at Imperial College, London.
When men recovered their endogenous testosterone-producing capacity, it occurred after an average of about 13 weeks on PCT and after an average of about 19 weeks without PCT, a significant difference.
“There is a vacuum of medical advice on what to do” when men stop taking steroids, said Dr. Jayasena during a press briefing at the meeting. “We can’t recommend anything yet because [our studies] have not proven causality” between the post-cycle therapy that many men start after stopping steroids and any symptom improvement they experience.”
The next step is to test the PCT agents in a prospective, controlled study, an investigation Dr. Jayasena and colleagues are eager to launch. The goal is to determine whether PCT is truly effective, the optimal doses, and whether the treatments are safe.
‘Incredibly sophisticated’ online community
The agents that constitute PCT include human chorionic gonadotropin (hCG, the “pregnancy hormone”), selective estrogen receptor modulators (SERMs), and aromatase inhibitors (AIs). SERMs and AIs are licensed only for use in women, the former for osteoporosis and breast cancer and the latter for breast cancer.
All of these agents, as well as others, are advertised by various illegal websites as treatments that can restore endogenous testosterone production in men whose native testosterone shut down during their steroid self-medication.
Restored testosterone resolves many of the adverse effects of steroid withdrawal such as diminished libido and erections, and depressed mood and energy.
Men buy PCT agents illegally from various websites. “There is an enormous, incredibly sophisticated community online that influences” PCT, and an “incredibly refined worldwide distribution network,” Dr. Jayasena explained.
His study included 410 men who turned to PCT after steroid cessation and 170 who did not.
Largest study of hormone recovery when men stop taking steroids
In a further multivariate analysis of the observational data, men who had used four or more different steroid treatments fared worse – with a significant 75% reduced rate of testosterone normalization with PCT – compared with men who had used a single steroid agent.
And men who had been on a steroid regimen for more than 6 months also fared badly – with a significant 66% reduced rate of testosterone normalization with PCT, compared with men on a steroid regimen for 3 months or less.
“This is the largest study of hormone recovery when men stop taking steroids,” Dr. Jayasena noted.
And the data “require corroboration within an interventional study to determine causality.”
“We need further studies to help doctors and other health care professionals advise men about the risks of anabolic steroid use and support those who are motivated to stop,” Dr. Jayasena said.
He cautioned that the study has several limitations: biases were potentially introduced based on recruitment and on recall by participants; clinicians drew blood specimens used to measure hormone levels at random times; and participants may have engaged in concealed drug use and used steroid and PCT agents that did not contain the substances advertised.
Nevertheless,, and they “may have important therapeutic implications for the future treatment of men who are motivated to stop” steroids.
The study received no commercial funding. Dr. Jayasena has received research funding from Logixx Pharma.
A version of this article first appeared on Medscape.com.
Men who illicitly used anabolic-androgenic steroids to bulk up and then turned to illegal, web-based regimens for treating their steroid withdrawal complications have provided important clues for new approaches to treating a growing worldwide population of men who abuse steroids.
A retrospective, observational study at one steroid addiction center in Glasgow examined 641 men who had stopped using steroids within the prior 3 years in 2015-2022 and who had self-administered certain agents, collectively known as post-cycle therapy (PCT) – within 3 months of stopping steroids.
They had a significant 3.8-fold increased rate of normalization of their levels of testosterone, luteinizing hormone (LH), and follicle-stimulating hormone (FSH), compared with men who either never used PCT or began it more than 3 months after stopping steroids, Channa N. Jayasena, PhD, MRCP, FRCPath, reported at the annual meeting of the Endocrine Society.
These testosterone, LH, and FSH levels served as a “surrogate marker of biochemical recovery from hypogonadism,” he explained. Normalization also occurred “slightly sooner” in men who began using PCT early after steroid cessation, added Dr. Jayasena, a reproductive endocrinologist at Imperial College, London.
When men recovered their endogenous testosterone-producing capacity, it occurred after an average of about 13 weeks on PCT and after an average of about 19 weeks without PCT, a significant difference.
“There is a vacuum of medical advice on what to do” when men stop taking steroids, said Dr. Jayasena during a press briefing at the meeting. “We can’t recommend anything yet because [our studies] have not proven causality” between the post-cycle therapy that many men start after stopping steroids and any symptom improvement they experience.”
The next step is to test the PCT agents in a prospective, controlled study, an investigation Dr. Jayasena and colleagues are eager to launch. The goal is to determine whether PCT is truly effective, the optimal doses, and whether the treatments are safe.
‘Incredibly sophisticated’ online community
The agents that constitute PCT include human chorionic gonadotropin (hCG, the “pregnancy hormone”), selective estrogen receptor modulators (SERMs), and aromatase inhibitors (AIs). SERMs and AIs are licensed only for use in women, the former for osteoporosis and breast cancer and the latter for breast cancer.
All of these agents, as well as others, are advertised by various illegal websites as treatments that can restore endogenous testosterone production in men whose native testosterone shut down during their steroid self-medication.
Restored testosterone resolves many of the adverse effects of steroid withdrawal such as diminished libido and erections, and depressed mood and energy.
Men buy PCT agents illegally from various websites. “There is an enormous, incredibly sophisticated community online that influences” PCT, and an “incredibly refined worldwide distribution network,” Dr. Jayasena explained.
His study included 410 men who turned to PCT after steroid cessation and 170 who did not.
Largest study of hormone recovery when men stop taking steroids
In a further multivariate analysis of the observational data, men who had used four or more different steroid treatments fared worse – with a significant 75% reduced rate of testosterone normalization with PCT – compared with men who had used a single steroid agent.
And men who had been on a steroid regimen for more than 6 months also fared badly – with a significant 66% reduced rate of testosterone normalization with PCT, compared with men on a steroid regimen for 3 months or less.
“This is the largest study of hormone recovery when men stop taking steroids,” Dr. Jayasena noted.
And the data “require corroboration within an interventional study to determine causality.”
“We need further studies to help doctors and other health care professionals advise men about the risks of anabolic steroid use and support those who are motivated to stop,” Dr. Jayasena said.
He cautioned that the study has several limitations: biases were potentially introduced based on recruitment and on recall by participants; clinicians drew blood specimens used to measure hormone levels at random times; and participants may have engaged in concealed drug use and used steroid and PCT agents that did not contain the substances advertised.
Nevertheless,, and they “may have important therapeutic implications for the future treatment of men who are motivated to stop” steroids.
The study received no commercial funding. Dr. Jayasena has received research funding from Logixx Pharma.
A version of this article first appeared on Medscape.com.
FROM ENDO 2023
Big trial reassures on heart safety of testosterone in men
CHICAGO – , long-awaited results from a major clinical trial show.
Among over 5,000 men aged 45-80 years randomized to daily transdermal testosterone gel or matching placebo gel for an average of 22 months, no increased risk was seen for a first occurrence of any component of a composite of death from cardiovascular causes, nonfatal myocardial infarction, or nonfatal stroke.
There was also no increased risk for prostate cancer over the 33-month follow-up period. However, there were increases in rates of atrial fibrillation, acute kidney injury, and pulmonary embolism in the testosterone group.
In terms of efficacy, testosterone therapy was associated with improved sexual function over two years of treatment and correction, or prevention, of anemia, but had no effect on progression to diabetes or glycemic parameters.
And, an unexpected finding was a significant and unexplained 43% increase in fractures with testosterone therapy.
The TRAVERSE study was mandated by the Food and Drug Administration in 2015 in response to concerns and conflicting data regarding the cardiovascular safety of testosterone replacement therapy in men. It was conducted by a consortium of five manufacturers of testosterone replacement products, led by AbbVie.
The results were presented during a symposium at the annual meeting of the Endocrine Society. The mandated safety data were published online in the New England Journal of Medicine. The efficacy outcomes, undertaken opportunistically due to the trial’s large sample size and relatively long followup time, will be published later this year.
Taken together, the TRAVERSE findings are expected to transform the risk–benefit discussions with patients about the use of testosterone therapy for hypogonadism, study coauthor Shalender Bhasin, MD, told this news organization.
“Testosterone deficiency doesn’t kill people as far as we know but it is really an important symptomatic condition that affects quality of life. Many middle-aged and older men seek assistance for these symptoms, so it’s an important condition and the treatment decisions are complicated,” said Dr. Bhasin, director of the research program in Men’s Health: Aging and Metabolism, at Brigham and Women’s Hospital in Boston.
These new data will be incorporated into future guidelines on testosterone therapy in men with hypoandrogenism, noted Dr. Bhasin, a coauthor of The Endocrine Society’s 2018 guidelines.
Findings apply only to men with bona fide testosterone deficiency
Asked to comment, endocrinologist Bradley D. Anawalt, MD, told this news organization that “the community of physicians who prescribe testosterone to men was waiting with bated breath” for the TRAVERSE results.
“Until now, we’ve had to say well, there might be a risk of strokes and heart attacks. This study does a lot to say that’s not a serious risk, in the first few years anyway, of testosterone therapy. We still need long-term follow-up in these patients, or others, to see what the long-term risks are, but it’s really reassuring,” added Dr. Anawalt, professor of medicine at the University of Washington, Seattle.
Both Dr. Bhasin and Dr. Anawalt said the TRAVERSE trial in men is similar in many ways to the Women’s Health Initiative (WHI). “[TRAVERSE] is not as big as [WHI], but it’s framed in a similar way to ask those safety questions and to weigh the risk and benefit,” Dr. Anawalt explained.
However, Dr. Anawalt stressed that the TRAVERSE safety data apply only to men with documented testosterone deficiency.
“It’s important to emphasize that this is a study of men with bona fide testosterone deficiency and symptoms. It doesn’t give carte blanche to prescribe to men with normal testosterone concentrations. It doesn’t tell us about the safety of that,” he noted.
Safety reassuring, but some concerns will require more investigation
TRAVERSE was a multicenter, randomized, double-blind, placebo-controlled noninferiority trial that enrolled 5246 men aged 45-80 years. Participants had pre-existing or were at high risk of cardiovascular disease, reported symptoms of hypogonadism, and had two fasting testosterone levels < 300 ng/dL. They were randomly assigned to receive daily transdermal 1.62% testosterone gel or placebo gel.
The primary safety endpoint event (first adjudicated major adverse cardiac event) occurred in 182 patients (7.0%) in the testosterone group and in 190 patients (7.3%) in the placebo group (hazard ratio, 0.96; P < .001 for noninferiority). Similar results were seen in sensitivity analyses.
Pulmonary embolism occurred in 0.9% of the testosterone group versus 0.5% of the placebo group, supporting current guidelines that testosterone should be used with caution in men who have had previous thromboembolic events, the authors note.
Prostate cancer occurred in 0.5% (n = 12) of patients in the testosterone group and 0.4% (n = 11) of patients in the placebo group, not a significant difference (P = .87).
There were, however, significant differences between the testosterone and placebo groups in terms of nonfatal arrhythmias warranting intervention (5.2% vs. 3.3%; P = .001), atrial fibrillation (3.5% vs. 2.4%; P = .02), and acute kidney injury (2.3% vs. 1.5%; P = .04).
“These adverse events were not expected,” the authors wrote.
Dr. Bhasin said that the team plans to investigate those cases further to look for possible risk factors, including whether COVID-19 played a role in these outcomes because the trial took place during the pandemic and some participants in both study groups contracted the virus.
Regarding acute kidney injury, Dr. Anawalt said: “I don’t know that I believe that ... It’s probably a statistical abnormality. It barely made ... significance.”
Finally, ‘real data on something we’ve been prescribing for decades’
Both Dr. Bhasin and Dr. Anawalt pointed out the deficiencies in the prior literature in terms of what has been known about testosterone’s effects. According to Dr. Bhasin, “In spite of all the folklore, there isn’t very much known about the efficacy of treatment beyond sexual function, and even there, the data are really limited. Most trials have been open-label and very small.”
He added that even among the few previous randomized clinical trials, only one, the TTrials series, had an adequate number of participants and used robust measures to assess sexual function, but that study only lasted a year.
Indeed, Dr. Anawalt noted, “[TRAVERSE] and its father study, the TTrials, were the first systematic studies to look at large groups of men getting testosterone versus placebo. We’re now starting to get real data on something that we’ve been prescribing for decades.”
At the ENDO symposium, Dr. Bhasin presented data showing significant improvements with testosterone compared to placebo in overall sexual activity (P = .011), sexual symptoms (P < .001), and sexual desire over one year, and maintained over two years in TRAVERSE. All were assessed by validated questionnaires.
“They confirmed that there’s an improvement in sexual function and that it’s sustained. That’s important because there had been doubt about that ... and it sounds like it’s clinically significant,” Dr. Anawalt said.
Testosterone therapy was also associated with lower rates of anemia among men who were not anemic at baseline, and lower incidence of anemia in those who were anemic to begin with. However, the rate of progression from prediabetes to diabetes didn’t differ significantly, nor did testosterone therapy improve glycemic control or remission in men who had diabetes at baseline, Dr. Bhasin reported.
‘Big surprise’ and a mystery: Testosterone increased fracture risk
The fracture data were presented by Peter J. Snyder, MD, of the University of Pennsylvania, who earlier in the session had received an Endocrine Society award for his work in the testosterone field.
“No prior trial of testosterone treatment of hypogonadal men has been large enough or long enough to assess its effect on fractures ... until the TRAVERSE trial,” he said.
The hypothesis going in was that testosterone would decrease the fracture incidence, since prior data had suggested it improves many parameters of bone quality in elderly men and in those with severe hypogonadism.
Instead, there were 91 confirmed and adjudicated clinical fractures in the testosterone group versus 64 in the placebo group, giving a hazard ratio of 1.43 (P = .03). The risk was seen across fracture types, increasing the likelihood that this finding was, in fact, real, Dr. Snyder said.
“We could speculate about a possible mechanism, but because we did not expect these results, we did not design the trial to evaluate a possible mechanism,” Dr. Snyder noted.
Dr. Anawalt told this news organization that the fracture finding “was a big surprise. None of us would have expected that there would be an increase in fractures.”
Clinically, Dr. Anawalt said it suggests consideration of expanding the use of anti-osteoporotic medication such as bisphosphonates to men with low testosterone and elevated fracture risk for whom clinicians may have assumed that just giving them testosterone replacement might also protect their bones.
“This begs the question should we reorient the way we’re thinking about these men.”
The study was funded by AbbVie, Acerus Pharmaceuticals Corporation/Aytu Biosciences, Allergan Sales, Endo Pharmaceuticals, and Upsher-Smith Laboratories. Dr. Bhasin has disclosed grants to his institution from Function Promoting Therapies and Metro International Biotech, and owns stock in XYone. Dr. Anawalt has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
This article was updated 6/19/23.
CHICAGO – , long-awaited results from a major clinical trial show.
Among over 5,000 men aged 45-80 years randomized to daily transdermal testosterone gel or matching placebo gel for an average of 22 months, no increased risk was seen for a first occurrence of any component of a composite of death from cardiovascular causes, nonfatal myocardial infarction, or nonfatal stroke.
There was also no increased risk for prostate cancer over the 33-month follow-up period. However, there were increases in rates of atrial fibrillation, acute kidney injury, and pulmonary embolism in the testosterone group.
In terms of efficacy, testosterone therapy was associated with improved sexual function over two years of treatment and correction, or prevention, of anemia, but had no effect on progression to diabetes or glycemic parameters.
And, an unexpected finding was a significant and unexplained 43% increase in fractures with testosterone therapy.
The TRAVERSE study was mandated by the Food and Drug Administration in 2015 in response to concerns and conflicting data regarding the cardiovascular safety of testosterone replacement therapy in men. It was conducted by a consortium of five manufacturers of testosterone replacement products, led by AbbVie.
The results were presented during a symposium at the annual meeting of the Endocrine Society. The mandated safety data were published online in the New England Journal of Medicine. The efficacy outcomes, undertaken opportunistically due to the trial’s large sample size and relatively long followup time, will be published later this year.
Taken together, the TRAVERSE findings are expected to transform the risk–benefit discussions with patients about the use of testosterone therapy for hypogonadism, study coauthor Shalender Bhasin, MD, told this news organization.
“Testosterone deficiency doesn’t kill people as far as we know but it is really an important symptomatic condition that affects quality of life. Many middle-aged and older men seek assistance for these symptoms, so it’s an important condition and the treatment decisions are complicated,” said Dr. Bhasin, director of the research program in Men’s Health: Aging and Metabolism, at Brigham and Women’s Hospital in Boston.
These new data will be incorporated into future guidelines on testosterone therapy in men with hypoandrogenism, noted Dr. Bhasin, a coauthor of The Endocrine Society’s 2018 guidelines.
Findings apply only to men with bona fide testosterone deficiency
Asked to comment, endocrinologist Bradley D. Anawalt, MD, told this news organization that “the community of physicians who prescribe testosterone to men was waiting with bated breath” for the TRAVERSE results.
“Until now, we’ve had to say well, there might be a risk of strokes and heart attacks. This study does a lot to say that’s not a serious risk, in the first few years anyway, of testosterone therapy. We still need long-term follow-up in these patients, or others, to see what the long-term risks are, but it’s really reassuring,” added Dr. Anawalt, professor of medicine at the University of Washington, Seattle.
Both Dr. Bhasin and Dr. Anawalt said the TRAVERSE trial in men is similar in many ways to the Women’s Health Initiative (WHI). “[TRAVERSE] is not as big as [WHI], but it’s framed in a similar way to ask those safety questions and to weigh the risk and benefit,” Dr. Anawalt explained.
However, Dr. Anawalt stressed that the TRAVERSE safety data apply only to men with documented testosterone deficiency.
“It’s important to emphasize that this is a study of men with bona fide testosterone deficiency and symptoms. It doesn’t give carte blanche to prescribe to men with normal testosterone concentrations. It doesn’t tell us about the safety of that,” he noted.
Safety reassuring, but some concerns will require more investigation
TRAVERSE was a multicenter, randomized, double-blind, placebo-controlled noninferiority trial that enrolled 5246 men aged 45-80 years. Participants had pre-existing or were at high risk of cardiovascular disease, reported symptoms of hypogonadism, and had two fasting testosterone levels < 300 ng/dL. They were randomly assigned to receive daily transdermal 1.62% testosterone gel or placebo gel.
The primary safety endpoint event (first adjudicated major adverse cardiac event) occurred in 182 patients (7.0%) in the testosterone group and in 190 patients (7.3%) in the placebo group (hazard ratio, 0.96; P < .001 for noninferiority). Similar results were seen in sensitivity analyses.
Pulmonary embolism occurred in 0.9% of the testosterone group versus 0.5% of the placebo group, supporting current guidelines that testosterone should be used with caution in men who have had previous thromboembolic events, the authors note.
Prostate cancer occurred in 0.5% (n = 12) of patients in the testosterone group and 0.4% (n = 11) of patients in the placebo group, not a significant difference (P = .87).
There were, however, significant differences between the testosterone and placebo groups in terms of nonfatal arrhythmias warranting intervention (5.2% vs. 3.3%; P = .001), atrial fibrillation (3.5% vs. 2.4%; P = .02), and acute kidney injury (2.3% vs. 1.5%; P = .04).
“These adverse events were not expected,” the authors wrote.
Dr. Bhasin said that the team plans to investigate those cases further to look for possible risk factors, including whether COVID-19 played a role in these outcomes because the trial took place during the pandemic and some participants in both study groups contracted the virus.
Regarding acute kidney injury, Dr. Anawalt said: “I don’t know that I believe that ... It’s probably a statistical abnormality. It barely made ... significance.”
Finally, ‘real data on something we’ve been prescribing for decades’
Both Dr. Bhasin and Dr. Anawalt pointed out the deficiencies in the prior literature in terms of what has been known about testosterone’s effects. According to Dr. Bhasin, “In spite of all the folklore, there isn’t very much known about the efficacy of treatment beyond sexual function, and even there, the data are really limited. Most trials have been open-label and very small.”
He added that even among the few previous randomized clinical trials, only one, the TTrials series, had an adequate number of participants and used robust measures to assess sexual function, but that study only lasted a year.
Indeed, Dr. Anawalt noted, “[TRAVERSE] and its father study, the TTrials, were the first systematic studies to look at large groups of men getting testosterone versus placebo. We’re now starting to get real data on something that we’ve been prescribing for decades.”
At the ENDO symposium, Dr. Bhasin presented data showing significant improvements with testosterone compared to placebo in overall sexual activity (P = .011), sexual symptoms (P < .001), and sexual desire over one year, and maintained over two years in TRAVERSE. All were assessed by validated questionnaires.
“They confirmed that there’s an improvement in sexual function and that it’s sustained. That’s important because there had been doubt about that ... and it sounds like it’s clinically significant,” Dr. Anawalt said.
Testosterone therapy was also associated with lower rates of anemia among men who were not anemic at baseline, and lower incidence of anemia in those who were anemic to begin with. However, the rate of progression from prediabetes to diabetes didn’t differ significantly, nor did testosterone therapy improve glycemic control or remission in men who had diabetes at baseline, Dr. Bhasin reported.
‘Big surprise’ and a mystery: Testosterone increased fracture risk
The fracture data were presented by Peter J. Snyder, MD, of the University of Pennsylvania, who earlier in the session had received an Endocrine Society award for his work in the testosterone field.
“No prior trial of testosterone treatment of hypogonadal men has been large enough or long enough to assess its effect on fractures ... until the TRAVERSE trial,” he said.
The hypothesis going in was that testosterone would decrease the fracture incidence, since prior data had suggested it improves many parameters of bone quality in elderly men and in those with severe hypogonadism.
Instead, there were 91 confirmed and adjudicated clinical fractures in the testosterone group versus 64 in the placebo group, giving a hazard ratio of 1.43 (P = .03). The risk was seen across fracture types, increasing the likelihood that this finding was, in fact, real, Dr. Snyder said.
“We could speculate about a possible mechanism, but because we did not expect these results, we did not design the trial to evaluate a possible mechanism,” Dr. Snyder noted.
Dr. Anawalt told this news organization that the fracture finding “was a big surprise. None of us would have expected that there would be an increase in fractures.”
Clinically, Dr. Anawalt said it suggests consideration of expanding the use of anti-osteoporotic medication such as bisphosphonates to men with low testosterone and elevated fracture risk for whom clinicians may have assumed that just giving them testosterone replacement might also protect their bones.
“This begs the question should we reorient the way we’re thinking about these men.”
The study was funded by AbbVie, Acerus Pharmaceuticals Corporation/Aytu Biosciences, Allergan Sales, Endo Pharmaceuticals, and Upsher-Smith Laboratories. Dr. Bhasin has disclosed grants to his institution from Function Promoting Therapies and Metro International Biotech, and owns stock in XYone. Dr. Anawalt has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
This article was updated 6/19/23.
CHICAGO – , long-awaited results from a major clinical trial show.
Among over 5,000 men aged 45-80 years randomized to daily transdermal testosterone gel or matching placebo gel for an average of 22 months, no increased risk was seen for a first occurrence of any component of a composite of death from cardiovascular causes, nonfatal myocardial infarction, or nonfatal stroke.
There was also no increased risk for prostate cancer over the 33-month follow-up period. However, there were increases in rates of atrial fibrillation, acute kidney injury, and pulmonary embolism in the testosterone group.
In terms of efficacy, testosterone therapy was associated with improved sexual function over two years of treatment and correction, or prevention, of anemia, but had no effect on progression to diabetes or glycemic parameters.
And, an unexpected finding was a significant and unexplained 43% increase in fractures with testosterone therapy.
The TRAVERSE study was mandated by the Food and Drug Administration in 2015 in response to concerns and conflicting data regarding the cardiovascular safety of testosterone replacement therapy in men. It was conducted by a consortium of five manufacturers of testosterone replacement products, led by AbbVie.
The results were presented during a symposium at the annual meeting of the Endocrine Society. The mandated safety data were published online in the New England Journal of Medicine. The efficacy outcomes, undertaken opportunistically due to the trial’s large sample size and relatively long followup time, will be published later this year.
Taken together, the TRAVERSE findings are expected to transform the risk–benefit discussions with patients about the use of testosterone therapy for hypogonadism, study coauthor Shalender Bhasin, MD, told this news organization.
“Testosterone deficiency doesn’t kill people as far as we know but it is really an important symptomatic condition that affects quality of life. Many middle-aged and older men seek assistance for these symptoms, so it’s an important condition and the treatment decisions are complicated,” said Dr. Bhasin, director of the research program in Men’s Health: Aging and Metabolism, at Brigham and Women’s Hospital in Boston.
These new data will be incorporated into future guidelines on testosterone therapy in men with hypoandrogenism, noted Dr. Bhasin, a coauthor of The Endocrine Society’s 2018 guidelines.
Findings apply only to men with bona fide testosterone deficiency
Asked to comment, endocrinologist Bradley D. Anawalt, MD, told this news organization that “the community of physicians who prescribe testosterone to men was waiting with bated breath” for the TRAVERSE results.
“Until now, we’ve had to say well, there might be a risk of strokes and heart attacks. This study does a lot to say that’s not a serious risk, in the first few years anyway, of testosterone therapy. We still need long-term follow-up in these patients, or others, to see what the long-term risks are, but it’s really reassuring,” added Dr. Anawalt, professor of medicine at the University of Washington, Seattle.
Both Dr. Bhasin and Dr. Anawalt said the TRAVERSE trial in men is similar in many ways to the Women’s Health Initiative (WHI). “[TRAVERSE] is not as big as [WHI], but it’s framed in a similar way to ask those safety questions and to weigh the risk and benefit,” Dr. Anawalt explained.
However, Dr. Anawalt stressed that the TRAVERSE safety data apply only to men with documented testosterone deficiency.
“It’s important to emphasize that this is a study of men with bona fide testosterone deficiency and symptoms. It doesn’t give carte blanche to prescribe to men with normal testosterone concentrations. It doesn’t tell us about the safety of that,” he noted.
Safety reassuring, but some concerns will require more investigation
TRAVERSE was a multicenter, randomized, double-blind, placebo-controlled noninferiority trial that enrolled 5246 men aged 45-80 years. Participants had pre-existing or were at high risk of cardiovascular disease, reported symptoms of hypogonadism, and had two fasting testosterone levels < 300 ng/dL. They were randomly assigned to receive daily transdermal 1.62% testosterone gel or placebo gel.
The primary safety endpoint event (first adjudicated major adverse cardiac event) occurred in 182 patients (7.0%) in the testosterone group and in 190 patients (7.3%) in the placebo group (hazard ratio, 0.96; P < .001 for noninferiority). Similar results were seen in sensitivity analyses.
Pulmonary embolism occurred in 0.9% of the testosterone group versus 0.5% of the placebo group, supporting current guidelines that testosterone should be used with caution in men who have had previous thromboembolic events, the authors note.
Prostate cancer occurred in 0.5% (n = 12) of patients in the testosterone group and 0.4% (n = 11) of patients in the placebo group, not a significant difference (P = .87).
There were, however, significant differences between the testosterone and placebo groups in terms of nonfatal arrhythmias warranting intervention (5.2% vs. 3.3%; P = .001), atrial fibrillation (3.5% vs. 2.4%; P = .02), and acute kidney injury (2.3% vs. 1.5%; P = .04).
“These adverse events were not expected,” the authors wrote.
Dr. Bhasin said that the team plans to investigate those cases further to look for possible risk factors, including whether COVID-19 played a role in these outcomes because the trial took place during the pandemic and some participants in both study groups contracted the virus.
Regarding acute kidney injury, Dr. Anawalt said: “I don’t know that I believe that ... It’s probably a statistical abnormality. It barely made ... significance.”
Finally, ‘real data on something we’ve been prescribing for decades’
Both Dr. Bhasin and Dr. Anawalt pointed out the deficiencies in the prior literature in terms of what has been known about testosterone’s effects. According to Dr. Bhasin, “In spite of all the folklore, there isn’t very much known about the efficacy of treatment beyond sexual function, and even there, the data are really limited. Most trials have been open-label and very small.”
He added that even among the few previous randomized clinical trials, only one, the TTrials series, had an adequate number of participants and used robust measures to assess sexual function, but that study only lasted a year.
Indeed, Dr. Anawalt noted, “[TRAVERSE] and its father study, the TTrials, were the first systematic studies to look at large groups of men getting testosterone versus placebo. We’re now starting to get real data on something that we’ve been prescribing for decades.”
At the ENDO symposium, Dr. Bhasin presented data showing significant improvements with testosterone compared to placebo in overall sexual activity (P = .011), sexual symptoms (P < .001), and sexual desire over one year, and maintained over two years in TRAVERSE. All were assessed by validated questionnaires.
“They confirmed that there’s an improvement in sexual function and that it’s sustained. That’s important because there had been doubt about that ... and it sounds like it’s clinically significant,” Dr. Anawalt said.
Testosterone therapy was also associated with lower rates of anemia among men who were not anemic at baseline, and lower incidence of anemia in those who were anemic to begin with. However, the rate of progression from prediabetes to diabetes didn’t differ significantly, nor did testosterone therapy improve glycemic control or remission in men who had diabetes at baseline, Dr. Bhasin reported.
‘Big surprise’ and a mystery: Testosterone increased fracture risk
The fracture data were presented by Peter J. Snyder, MD, of the University of Pennsylvania, who earlier in the session had received an Endocrine Society award for his work in the testosterone field.
“No prior trial of testosterone treatment of hypogonadal men has been large enough or long enough to assess its effect on fractures ... until the TRAVERSE trial,” he said.
The hypothesis going in was that testosterone would decrease the fracture incidence, since prior data had suggested it improves many parameters of bone quality in elderly men and in those with severe hypogonadism.
Instead, there were 91 confirmed and adjudicated clinical fractures in the testosterone group versus 64 in the placebo group, giving a hazard ratio of 1.43 (P = .03). The risk was seen across fracture types, increasing the likelihood that this finding was, in fact, real, Dr. Snyder said.
“We could speculate about a possible mechanism, but because we did not expect these results, we did not design the trial to evaluate a possible mechanism,” Dr. Snyder noted.
Dr. Anawalt told this news organization that the fracture finding “was a big surprise. None of us would have expected that there would be an increase in fractures.”
Clinically, Dr. Anawalt said it suggests consideration of expanding the use of anti-osteoporotic medication such as bisphosphonates to men with low testosterone and elevated fracture risk for whom clinicians may have assumed that just giving them testosterone replacement might also protect their bones.
“This begs the question should we reorient the way we’re thinking about these men.”
The study was funded by AbbVie, Acerus Pharmaceuticals Corporation/Aytu Biosciences, Allergan Sales, Endo Pharmaceuticals, and Upsher-Smith Laboratories. Dr. Bhasin has disclosed grants to his institution from Function Promoting Therapies and Metro International Biotech, and owns stock in XYone. Dr. Anawalt has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
This article was updated 6/19/23.
AT ENDO 2023
FDA approves first-ever OTC erectile dysfunction gel
The gel, which can help users get an erection within 10 minutes, is already available without a prescription in Europe.
The Food and Drug Administration has approved the drug, called Eroxon, noting that it is a first-of-its-kind treatment. Eroxon is made by the British pharmaceutical company Futura Medical, which specializes in drugs that are given through the skin.
According to the product’s leaflet, Eroxon “stimulates blood flow in the penis through a unique physical cooling then warming effect, helping you get and keep an erection hard enough for sex.” The company said on the product’s website that 65% of people who used the drug were able to have sex.
A company spokesperson told CNN that the price of the product has not been set in the United States, but it costs the equivalent of about $31 in the United Kingdom. Futura Medical has not announced when it will be available in the United States.
Harvard Health reports that 30 million people in the United States have erectile dysfunction, which means a person cannot get an erection at all or one firm enough to have sex. The disorder is often linked to other physical or mental health problems, such as heart problems or clogged arteries.
Erectile dysfunction affects 1% of men in their 40s, 17% of men in their 60s, and nearly 50% of men who are age 75 or older, according to Harvard Health.
A version of this article originally appeared on WebMD.com.
The gel, which can help users get an erection within 10 minutes, is already available without a prescription in Europe.
The Food and Drug Administration has approved the drug, called Eroxon, noting that it is a first-of-its-kind treatment. Eroxon is made by the British pharmaceutical company Futura Medical, which specializes in drugs that are given through the skin.
According to the product’s leaflet, Eroxon “stimulates blood flow in the penis through a unique physical cooling then warming effect, helping you get and keep an erection hard enough for sex.” The company said on the product’s website that 65% of people who used the drug were able to have sex.
A company spokesperson told CNN that the price of the product has not been set in the United States, but it costs the equivalent of about $31 in the United Kingdom. Futura Medical has not announced when it will be available in the United States.
Harvard Health reports that 30 million people in the United States have erectile dysfunction, which means a person cannot get an erection at all or one firm enough to have sex. The disorder is often linked to other physical or mental health problems, such as heart problems or clogged arteries.
Erectile dysfunction affects 1% of men in their 40s, 17% of men in their 60s, and nearly 50% of men who are age 75 or older, according to Harvard Health.
A version of this article originally appeared on WebMD.com.
The gel, which can help users get an erection within 10 minutes, is already available without a prescription in Europe.
The Food and Drug Administration has approved the drug, called Eroxon, noting that it is a first-of-its-kind treatment. Eroxon is made by the British pharmaceutical company Futura Medical, which specializes in drugs that are given through the skin.
According to the product’s leaflet, Eroxon “stimulates blood flow in the penis through a unique physical cooling then warming effect, helping you get and keep an erection hard enough for sex.” The company said on the product’s website that 65% of people who used the drug were able to have sex.
A company spokesperson told CNN that the price of the product has not been set in the United States, but it costs the equivalent of about $31 in the United Kingdom. Futura Medical has not announced when it will be available in the United States.
Harvard Health reports that 30 million people in the United States have erectile dysfunction, which means a person cannot get an erection at all or one firm enough to have sex. The disorder is often linked to other physical or mental health problems, such as heart problems or clogged arteries.
Erectile dysfunction affects 1% of men in their 40s, 17% of men in their 60s, and nearly 50% of men who are age 75 or older, according to Harvard Health.
A version of this article originally appeared on WebMD.com.
Breast cancer outcomes are worse for Black men
A new study finds that racial disparities in male breast cancer are persisting in the United States.
From 2000 to 2019, Black men were diagnosed at later ages than White males (median ages, 69 and 63 years, respectively) and were more likely to die from the disease (22.4% vs. 16.8%, respectively). Male breast cancer (MBC) was more likely to kill Black men in rural vs. urban areas (hazard ratio = 1.4; 95% confidence interval, 1.0-2.1; P less than .05). Among White males, in contrast, there was no difference on that front, according to the research, which was presented in a poster (Abstract No. 87P) at the European Society for Medical Oncology (ESMO) Breast Cancer annual congress.
It’s not clear why the disparities exist, said lead author Lekha Yadukumar, MBBS, an internal medicine resident at the Wright Center for Graduate Medical Education in Scranton, Penn., in an interview.
“Several potential factors may contribute to the higher rate of breast cancer diagnosis in older [Black] men, including the pathology of the disease, limited awareness about breast cancer, and potential barriers to accessibility,” she said. “The increased mortality among [Black men] may be linked to variations in tumor pathology and molecular biology. Social factors may also potentially impact survival rates, including [having] limited access to health care in rural areas and inadequate social support.”
Male breast cancer is rare, accounting for less than 1% of all breast cancer cases in the United States, according to the Breast Cancer Research Foundation. An estimated 2,700 men are diagnosed each year, and about 530 will die. Previous research has suggested Black men have worse outcomes than White men, but the data covered earlier years than the new study.
Methods and results
Dr. Yadukumar and colleagues retrospectively analyzed statistics from the Surveillance, Epidemiology, and End Results database for patients diagnosed with primary male breast cancer from 2000 to 2019 (n = 8,373; Black men, 1,111 [13.26%]; White men, 6,817 [81.41%]).
Median income didn’t affect mortality, whereas men in both racial groups were less likely to die if they were married vs. single/divorced (hazard ratio = 0.6; P less than .05).
Other studies have shown that “[Black American] men diagnosed with breast cancer experience longer time intervals before receiving treatment, encounter more severe disease manifestations, and exhibit lower rates of survivorship,” Dr. Yadukumar said. “Despite these findings, there remains a scarcity of genetic studies aimed at comprehending the underlying causes of these disparities. Moreover, there is a dearth of research investigating other factors that may influence survival outcomes among men with breast cancer.”
Findings reflect the disparities in female breast cancer
In an interview, Duke University, Durham, N.C., oncologist Arif Kamal, MD, MBA, MHS, the chief patient officer at the American Cancer Society, said the study is impressive since the number of patients is large for a rare cancer and the population is diverse. Plus, the findings reflect the disparities in female breast cancer, he noted.
“We know that Black women’s mortality is worse vs. White women in breast cancer, and we believe that most of that has nothing to do with cancer screening,” said Dr. Kamal, who was not involved in the new study. “When the clock starts from diagnosis onwards, you start to see less introduction to clinical trials and standard care medications and more time to treatment, surgery, and radiation,” he said.
“You see similar disparities as related to mortality in Black vs. White men,” he noted.
The new findings about higher death rates for Black men, especially in rural areas, suggest that “distance matters, and race matters,” he said. In rural areas, it can be hard to access pathologists, radiologists, and surgeons with more experience with breast cancer, he said.
But, he noted, the study finds that income doesn’t appear to be a factor.
In the big picture, he said, the results suggest that when it comes to barriers to better outcomes, “things that are systemic don’t make exceptions because you are a man vs. a woman.”
No study funding was reported. The study authors and Dr. Kamal have no relevant financial disclosures.
A new study finds that racial disparities in male breast cancer are persisting in the United States.
From 2000 to 2019, Black men were diagnosed at later ages than White males (median ages, 69 and 63 years, respectively) and were more likely to die from the disease (22.4% vs. 16.8%, respectively). Male breast cancer (MBC) was more likely to kill Black men in rural vs. urban areas (hazard ratio = 1.4; 95% confidence interval, 1.0-2.1; P less than .05). Among White males, in contrast, there was no difference on that front, according to the research, which was presented in a poster (Abstract No. 87P) at the European Society for Medical Oncology (ESMO) Breast Cancer annual congress.
It’s not clear why the disparities exist, said lead author Lekha Yadukumar, MBBS, an internal medicine resident at the Wright Center for Graduate Medical Education in Scranton, Penn., in an interview.
“Several potential factors may contribute to the higher rate of breast cancer diagnosis in older [Black] men, including the pathology of the disease, limited awareness about breast cancer, and potential barriers to accessibility,” she said. “The increased mortality among [Black men] may be linked to variations in tumor pathology and molecular biology. Social factors may also potentially impact survival rates, including [having] limited access to health care in rural areas and inadequate social support.”
Male breast cancer is rare, accounting for less than 1% of all breast cancer cases in the United States, according to the Breast Cancer Research Foundation. An estimated 2,700 men are diagnosed each year, and about 530 will die. Previous research has suggested Black men have worse outcomes than White men, but the data covered earlier years than the new study.
Methods and results
Dr. Yadukumar and colleagues retrospectively analyzed statistics from the Surveillance, Epidemiology, and End Results database for patients diagnosed with primary male breast cancer from 2000 to 2019 (n = 8,373; Black men, 1,111 [13.26%]; White men, 6,817 [81.41%]).
Median income didn’t affect mortality, whereas men in both racial groups were less likely to die if they were married vs. single/divorced (hazard ratio = 0.6; P less than .05).
Other studies have shown that “[Black American] men diagnosed with breast cancer experience longer time intervals before receiving treatment, encounter more severe disease manifestations, and exhibit lower rates of survivorship,” Dr. Yadukumar said. “Despite these findings, there remains a scarcity of genetic studies aimed at comprehending the underlying causes of these disparities. Moreover, there is a dearth of research investigating other factors that may influence survival outcomes among men with breast cancer.”
Findings reflect the disparities in female breast cancer
In an interview, Duke University, Durham, N.C., oncologist Arif Kamal, MD, MBA, MHS, the chief patient officer at the American Cancer Society, said the study is impressive since the number of patients is large for a rare cancer and the population is diverse. Plus, the findings reflect the disparities in female breast cancer, he noted.
“We know that Black women’s mortality is worse vs. White women in breast cancer, and we believe that most of that has nothing to do with cancer screening,” said Dr. Kamal, who was not involved in the new study. “When the clock starts from diagnosis onwards, you start to see less introduction to clinical trials and standard care medications and more time to treatment, surgery, and radiation,” he said.
“You see similar disparities as related to mortality in Black vs. White men,” he noted.
The new findings about higher death rates for Black men, especially in rural areas, suggest that “distance matters, and race matters,” he said. In rural areas, it can be hard to access pathologists, radiologists, and surgeons with more experience with breast cancer, he said.
But, he noted, the study finds that income doesn’t appear to be a factor.
In the big picture, he said, the results suggest that when it comes to barriers to better outcomes, “things that are systemic don’t make exceptions because you are a man vs. a woman.”
No study funding was reported. The study authors and Dr. Kamal have no relevant financial disclosures.
A new study finds that racial disparities in male breast cancer are persisting in the United States.
From 2000 to 2019, Black men were diagnosed at later ages than White males (median ages, 69 and 63 years, respectively) and were more likely to die from the disease (22.4% vs. 16.8%, respectively). Male breast cancer (MBC) was more likely to kill Black men in rural vs. urban areas (hazard ratio = 1.4; 95% confidence interval, 1.0-2.1; P less than .05). Among White males, in contrast, there was no difference on that front, according to the research, which was presented in a poster (Abstract No. 87P) at the European Society for Medical Oncology (ESMO) Breast Cancer annual congress.
It’s not clear why the disparities exist, said lead author Lekha Yadukumar, MBBS, an internal medicine resident at the Wright Center for Graduate Medical Education in Scranton, Penn., in an interview.
“Several potential factors may contribute to the higher rate of breast cancer diagnosis in older [Black] men, including the pathology of the disease, limited awareness about breast cancer, and potential barriers to accessibility,” she said. “The increased mortality among [Black men] may be linked to variations in tumor pathology and molecular biology. Social factors may also potentially impact survival rates, including [having] limited access to health care in rural areas and inadequate social support.”
Male breast cancer is rare, accounting for less than 1% of all breast cancer cases in the United States, according to the Breast Cancer Research Foundation. An estimated 2,700 men are diagnosed each year, and about 530 will die. Previous research has suggested Black men have worse outcomes than White men, but the data covered earlier years than the new study.
Methods and results
Dr. Yadukumar and colleagues retrospectively analyzed statistics from the Surveillance, Epidemiology, and End Results database for patients diagnosed with primary male breast cancer from 2000 to 2019 (n = 8,373; Black men, 1,111 [13.26%]; White men, 6,817 [81.41%]).
Median income didn’t affect mortality, whereas men in both racial groups were less likely to die if they were married vs. single/divorced (hazard ratio = 0.6; P less than .05).
Other studies have shown that “[Black American] men diagnosed with breast cancer experience longer time intervals before receiving treatment, encounter more severe disease manifestations, and exhibit lower rates of survivorship,” Dr. Yadukumar said. “Despite these findings, there remains a scarcity of genetic studies aimed at comprehending the underlying causes of these disparities. Moreover, there is a dearth of research investigating other factors that may influence survival outcomes among men with breast cancer.”
Findings reflect the disparities in female breast cancer
In an interview, Duke University, Durham, N.C., oncologist Arif Kamal, MD, MBA, MHS, the chief patient officer at the American Cancer Society, said the study is impressive since the number of patients is large for a rare cancer and the population is diverse. Plus, the findings reflect the disparities in female breast cancer, he noted.
“We know that Black women’s mortality is worse vs. White women in breast cancer, and we believe that most of that has nothing to do with cancer screening,” said Dr. Kamal, who was not involved in the new study. “When the clock starts from diagnosis onwards, you start to see less introduction to clinical trials and standard care medications and more time to treatment, surgery, and radiation,” he said.
“You see similar disparities as related to mortality in Black vs. White men,” he noted.
The new findings about higher death rates for Black men, especially in rural areas, suggest that “distance matters, and race matters,” he said. In rural areas, it can be hard to access pathologists, radiologists, and surgeons with more experience with breast cancer, he said.
But, he noted, the study finds that income doesn’t appear to be a factor.
In the big picture, he said, the results suggest that when it comes to barriers to better outcomes, “things that are systemic don’t make exceptions because you are a man vs. a woman.”
No study funding was reported. The study authors and Dr. Kamal have no relevant financial disclosures.
FROM ESMO BREAST CANCER 2023