User login
COVID-19 pandemic hinders access to contraception
The pandemic has affected reproductive health because of barriers to contraception access, potentially increasing unwanted pregnancies, reported Tracy Kuo Lin, PhD, of the University of California, San Francisco, and associates.
During the pandemic, women have experienced an increased desire to avoid pregnancy, and when that desire is coupled with loss of income, accessing contraception becomes more difficult, Dr. Lin and colleagues observed in a cross-sectional survey published in the journal Contraception.
The study aimed to quantify the effect of COVID-19 on women’s economic status and reproductive health decisions related to childbearing and pregnancy. Women aged 18-49 who resided in the U.S. were targeted via Facebook and Instagram advertisements from May 16 to June 16, 2020. In all, 554 racially diverse respondents from 43 states were selected: 41% aged 18-24, 37% aged 25-34, and 23% aged 35-49.
Income losses affect nearly half of respondents
In determining risk of unwanted pregnancy, the researchers considered the influence of COVID-19 on a number of factors related to economic well-being as well as respondents’ sexual activity, intimate partner violence, overall desire for pregnancy, and access to contraception as issues affecting their interest in becoming pregnant and their ability to access medical care and contraception. Overall, 46% experienced a reduction in income, 43% reported no change, and 10% experienced an increase in income.
Difficulty in being able to afford food, transportation, and housing doubled among respondents from 8% to 16% as a result of the pandemic. The study authors cited education, race/ethnicity, federal poverty level, and change in income as predictors of inability to provide for these basic needs.
A total of 83% of respondents reported having sex within the past month; 54% of those had sex with someone they lived with, compared with 29% who had sex with someone they did not live with. The pandemic had no impact on sexual desire for 37% of respondents, compared with 32% who experienced a decrease in desire, and 29% who experienced more desire for sex. The presence of shelter-in-place orders had no effect on frequency of or desire for sex. Among the respondents, 4% noted intimate partner violence, which increased slightly from 3% before the pandemic.
Among respondents using contraception, the study authors noted that 17% reported greater difficulty accessing birth control during the pandemic compared with 4% who felt access had become easier. Of those citing increased difficulties, 9% noted increasing challenges getting to a pharmacy, 4% were less able to afford birth control, 3% said it had become harder to obtain a prescription, and 1% cited difficulties having long-acting reversible contraceptives removed.
Despite the pandemic’s overall impact on quality of life, 41% of respondents reported a stronger desire to become pregnant, compared with 25% who had a reduced desire, and 34% whose interest in pregnancy was unchanged by the pandemic.
More than one-third of respondents (37%) admitted that COVID-19 contributed to their fears of becoming pregnant while 13% indicated their fear of pregnancy stemmed from concerns over being able to afford the cost of having a child. Not surprisingly, the decrease in desire for pregnancy was twice as high in those who reported they were unable to afford food, transportation, and/or housing compared with those who saw no change in their ability to afford basic needs.
“In these uncertain economic times, it is of utmost importance to create policies that will ensure access to and comprehensive coverage of core sexual and reproductive health services,” Dr. Lin and colleagues urged. “By doing so, we safeguard people’s ability to make decisions that support their reproductive health goals.”
Will COVID-19 drive needed practice and policy changes?
“This study highlights the economic and reproductive health toll of COVID-19 and the pressing need for improved contraception access,” Eve Espey, MD, MPH, said in an interview.
“Ob.gyns. and other practitioners can use this information to consider evidence-based practice changes that incorporate telemedicine visits, extended refills on contraceptive methods, and a focus on postpartum and postabortion initiation of contraception,” noted Dr. Espey, of the University of New Mexico, Albuquerque. For women who are experiencing economic hardship, consulting with state-based programs that offer pharmacy access and online access to contraceptives may offer a reasonable alternative, she added.
The study was funded by the University of California, San Francisco’s National Center of Excellence in Women’s Health. Dr. Lin received funding from Lazarex Cancer Foundation. The remaining authors had no conflicts of interest and reported no disclosures.
The pandemic has affected reproductive health because of barriers to contraception access, potentially increasing unwanted pregnancies, reported Tracy Kuo Lin, PhD, of the University of California, San Francisco, and associates.
During the pandemic, women have experienced an increased desire to avoid pregnancy, and when that desire is coupled with loss of income, accessing contraception becomes more difficult, Dr. Lin and colleagues observed in a cross-sectional survey published in the journal Contraception.
The study aimed to quantify the effect of COVID-19 on women’s economic status and reproductive health decisions related to childbearing and pregnancy. Women aged 18-49 who resided in the U.S. were targeted via Facebook and Instagram advertisements from May 16 to June 16, 2020. In all, 554 racially diverse respondents from 43 states were selected: 41% aged 18-24, 37% aged 25-34, and 23% aged 35-49.
Income losses affect nearly half of respondents
In determining risk of unwanted pregnancy, the researchers considered the influence of COVID-19 on a number of factors related to economic well-being as well as respondents’ sexual activity, intimate partner violence, overall desire for pregnancy, and access to contraception as issues affecting their interest in becoming pregnant and their ability to access medical care and contraception. Overall, 46% experienced a reduction in income, 43% reported no change, and 10% experienced an increase in income.
Difficulty in being able to afford food, transportation, and housing doubled among respondents from 8% to 16% as a result of the pandemic. The study authors cited education, race/ethnicity, federal poverty level, and change in income as predictors of inability to provide for these basic needs.
A total of 83% of respondents reported having sex within the past month; 54% of those had sex with someone they lived with, compared with 29% who had sex with someone they did not live with. The pandemic had no impact on sexual desire for 37% of respondents, compared with 32% who experienced a decrease in desire, and 29% who experienced more desire for sex. The presence of shelter-in-place orders had no effect on frequency of or desire for sex. Among the respondents, 4% noted intimate partner violence, which increased slightly from 3% before the pandemic.
Among respondents using contraception, the study authors noted that 17% reported greater difficulty accessing birth control during the pandemic compared with 4% who felt access had become easier. Of those citing increased difficulties, 9% noted increasing challenges getting to a pharmacy, 4% were less able to afford birth control, 3% said it had become harder to obtain a prescription, and 1% cited difficulties having long-acting reversible contraceptives removed.
Despite the pandemic’s overall impact on quality of life, 41% of respondents reported a stronger desire to become pregnant, compared with 25% who had a reduced desire, and 34% whose interest in pregnancy was unchanged by the pandemic.
More than one-third of respondents (37%) admitted that COVID-19 contributed to their fears of becoming pregnant while 13% indicated their fear of pregnancy stemmed from concerns over being able to afford the cost of having a child. Not surprisingly, the decrease in desire for pregnancy was twice as high in those who reported they were unable to afford food, transportation, and/or housing compared with those who saw no change in their ability to afford basic needs.
“In these uncertain economic times, it is of utmost importance to create policies that will ensure access to and comprehensive coverage of core sexual and reproductive health services,” Dr. Lin and colleagues urged. “By doing so, we safeguard people’s ability to make decisions that support their reproductive health goals.”
Will COVID-19 drive needed practice and policy changes?
“This study highlights the economic and reproductive health toll of COVID-19 and the pressing need for improved contraception access,” Eve Espey, MD, MPH, said in an interview.
“Ob.gyns. and other practitioners can use this information to consider evidence-based practice changes that incorporate telemedicine visits, extended refills on contraceptive methods, and a focus on postpartum and postabortion initiation of contraception,” noted Dr. Espey, of the University of New Mexico, Albuquerque. For women who are experiencing economic hardship, consulting with state-based programs that offer pharmacy access and online access to contraceptives may offer a reasonable alternative, she added.
The study was funded by the University of California, San Francisco’s National Center of Excellence in Women’s Health. Dr. Lin received funding from Lazarex Cancer Foundation. The remaining authors had no conflicts of interest and reported no disclosures.
The pandemic has affected reproductive health because of barriers to contraception access, potentially increasing unwanted pregnancies, reported Tracy Kuo Lin, PhD, of the University of California, San Francisco, and associates.
During the pandemic, women have experienced an increased desire to avoid pregnancy, and when that desire is coupled with loss of income, accessing contraception becomes more difficult, Dr. Lin and colleagues observed in a cross-sectional survey published in the journal Contraception.
The study aimed to quantify the effect of COVID-19 on women’s economic status and reproductive health decisions related to childbearing and pregnancy. Women aged 18-49 who resided in the U.S. were targeted via Facebook and Instagram advertisements from May 16 to June 16, 2020. In all, 554 racially diverse respondents from 43 states were selected: 41% aged 18-24, 37% aged 25-34, and 23% aged 35-49.
Income losses affect nearly half of respondents
In determining risk of unwanted pregnancy, the researchers considered the influence of COVID-19 on a number of factors related to economic well-being as well as respondents’ sexual activity, intimate partner violence, overall desire for pregnancy, and access to contraception as issues affecting their interest in becoming pregnant and their ability to access medical care and contraception. Overall, 46% experienced a reduction in income, 43% reported no change, and 10% experienced an increase in income.
Difficulty in being able to afford food, transportation, and housing doubled among respondents from 8% to 16% as a result of the pandemic. The study authors cited education, race/ethnicity, federal poverty level, and change in income as predictors of inability to provide for these basic needs.
A total of 83% of respondents reported having sex within the past month; 54% of those had sex with someone they lived with, compared with 29% who had sex with someone they did not live with. The pandemic had no impact on sexual desire for 37% of respondents, compared with 32% who experienced a decrease in desire, and 29% who experienced more desire for sex. The presence of shelter-in-place orders had no effect on frequency of or desire for sex. Among the respondents, 4% noted intimate partner violence, which increased slightly from 3% before the pandemic.
Among respondents using contraception, the study authors noted that 17% reported greater difficulty accessing birth control during the pandemic compared with 4% who felt access had become easier. Of those citing increased difficulties, 9% noted increasing challenges getting to a pharmacy, 4% were less able to afford birth control, 3% said it had become harder to obtain a prescription, and 1% cited difficulties having long-acting reversible contraceptives removed.
Despite the pandemic’s overall impact on quality of life, 41% of respondents reported a stronger desire to become pregnant, compared with 25% who had a reduced desire, and 34% whose interest in pregnancy was unchanged by the pandemic.
More than one-third of respondents (37%) admitted that COVID-19 contributed to their fears of becoming pregnant while 13% indicated their fear of pregnancy stemmed from concerns over being able to afford the cost of having a child. Not surprisingly, the decrease in desire for pregnancy was twice as high in those who reported they were unable to afford food, transportation, and/or housing compared with those who saw no change in their ability to afford basic needs.
“In these uncertain economic times, it is of utmost importance to create policies that will ensure access to and comprehensive coverage of core sexual and reproductive health services,” Dr. Lin and colleagues urged. “By doing so, we safeguard people’s ability to make decisions that support their reproductive health goals.”
Will COVID-19 drive needed practice and policy changes?
“This study highlights the economic and reproductive health toll of COVID-19 and the pressing need for improved contraception access,” Eve Espey, MD, MPH, said in an interview.
“Ob.gyns. and other practitioners can use this information to consider evidence-based practice changes that incorporate telemedicine visits, extended refills on contraceptive methods, and a focus on postpartum and postabortion initiation of contraception,” noted Dr. Espey, of the University of New Mexico, Albuquerque. For women who are experiencing economic hardship, consulting with state-based programs that offer pharmacy access and online access to contraceptives may offer a reasonable alternative, she added.
The study was funded by the University of California, San Francisco’s National Center of Excellence in Women’s Health. Dr. Lin received funding from Lazarex Cancer Foundation. The remaining authors had no conflicts of interest and reported no disclosures.
FROM CONTRACEPTION
Study finds benefits of increasing length of NICU stay unclear
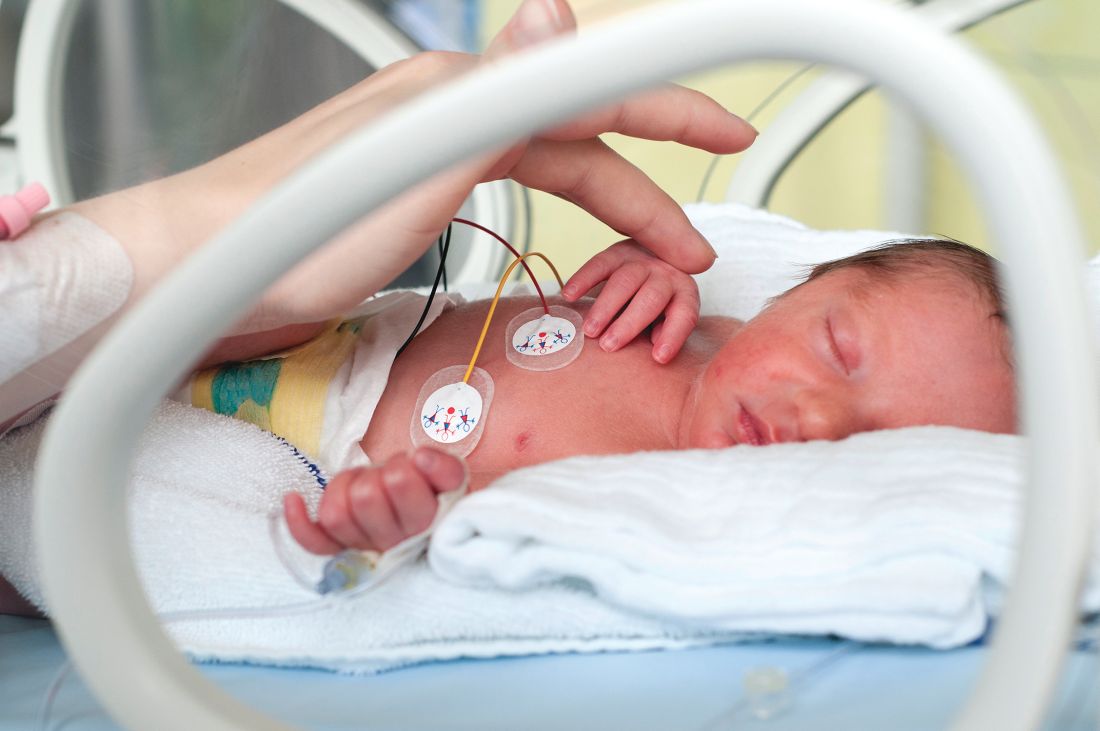
Gestational age and weight at discharge for infants aged 24-29 weeks increased steadily between 2005 and 2018, reported Erika M. Edwards, PhD, MPH, of the Vermont Oxford Network, Burlington, and associates.
Although they discussed several possible influencing factors, the authors were unable to explain the associated benefits, costs, and harms associated with increased age and weight at discharge, which remain undetermined. Infants are separated a week longer than they were at the beginning of the study period, the prolonged effects of which cannot be underestimated, Dr. Edwards and colleagues observed in a large cohort study in Pediatrics.
A total of 314,811 infants 24-29 weeks’ gestational age who were admitted to 824 neonatal ICUs (NICUs) throughout the United States survived to initial discharge. The median postmenstrual age at hospital discharge was 38.3 weeks. Over the 14-year period from 2005 to 2018, unadjusted postmenstrual age at discharge increased a median 9 days, compared with a median adjusted age of 8 days.
Of the 273,109 infants initially discharged from the hospital to home, median weight at discharge was 2,600 g. Over the 14 years from 2005 to 2018, median unadjusted discharge weight increased 360 g, compared with median adjusted weight, which was estimated to have increased 316 g.
Median unadjusted z scores for weight increased 0.22 standard units over the 14-year period, compared with median adjusted z scores for weight at discharge, which increased an estimated 0.19 standard units.
The proportion of infants who were consuming human milk at discharge increased over the study period from 40% in 2005 to 48% in 2018. The use of cardiorespiratory monitors and oxygen decreased from 49% to 26%, and 27% to 22% respectively. The number of infants who were never transferred to specialized care before discharge to home also improved, from 71% to 76%.
Despite the unknowns, good news for managing pediatricians?
In a separate interview, study author Dr. Edwards noted that “infants born very preterm, who are discharged home from the NICU today, are larger and more physiologically mature than they were in 2005. Pediatricians will likely find this news to be positive as it may be easier to manage care for a more physiologically mature [infant],” and it may reduce risk of readmission.
“Infants stayed, on average, 8 days longer in 2018 than they did in 2005. That is 8 days when they were not at home with their families. Despite efforts by NICU teams to increase family-centered care, the NICU is not the same as being at home. ... That extra time in the NICU cost [some families] an estimated $28,000. ... As health care costs continue to rise, we need to understand the true cost [behind] this increase,” added Dr. Edwards, noting that more research is needed to understand what may be driving the increase in NICU length of stay and the possible implications. More research to investigate whether babies did better after discharge also is needed.
Going forward, Dr. Edwards indicated that she and her colleagues are exploring ways to measure apnea of prematurity (AOP) and use of continuous pulse oximetry (CPO) as the subject of future studies. In our study, we showed that the number of infants discharged home on a cardiorespiratory monitor decreased, but we do not know if that is explained by differences in management of AOP and CPO. “Understanding the influence of AOP and CPO management on discharge age would be an important contribution [to future research].”
AOP may drive increase in postmenstrual age
In an accompanying editorial, Cody Arnold, MD, and Alexis S. Davis, MD, said: “We have focused on apnea of prematurity and discharge countdowns in this commentary because we believe that changes in related practices are likely the most important drivers of the increases in postmenstrual age” reported by the authors in this study. “Other factors, such as increasing availability of NICU beds or decreasing availability of home support services, may have contributed to longer length of stay. But these questions should be answered by research, not by speculation,” said Dr. Arnold, neonatologist, University of Texas Health Sciences Center, Houston, and Dr. Davis, clinical associate professor, Stanford (Calif.) University.
“Prospective research comparing alternative countdown strategies on the basis of readmission rates and other outpatient outcomes is overdue.” Additional research is needed operationally to clearly outline parameters for countdown events, countdown duration, indications for CPO, outpatient caffeine use, and parental shared decision-making.”
The study was funded by the Vermont Oxford Network. Dr. Edwards received a grant from the Vermont Oxford Network; several others also had ties to the Network. Dr. Arnold and Dr. Davis had no conflicts of interest and reported no disclosures.
Gestational age and weight at discharge for infants aged 24-29 weeks increased steadily between 2005 and 2018, reported Erika M. Edwards, PhD, MPH, of the Vermont Oxford Network, Burlington, and associates.
Although they discussed several possible influencing factors, the authors were unable to explain the associated benefits, costs, and harms associated with increased age and weight at discharge, which remain undetermined. Infants are separated a week longer than they were at the beginning of the study period, the prolonged effects of which cannot be underestimated, Dr. Edwards and colleagues observed in a large cohort study in Pediatrics.
A total of 314,811 infants 24-29 weeks’ gestational age who were admitted to 824 neonatal ICUs (NICUs) throughout the United States survived to initial discharge. The median postmenstrual age at hospital discharge was 38.3 weeks. Over the 14-year period from 2005 to 2018, unadjusted postmenstrual age at discharge increased a median 9 days, compared with a median adjusted age of 8 days.
Of the 273,109 infants initially discharged from the hospital to home, median weight at discharge was 2,600 g. Over the 14 years from 2005 to 2018, median unadjusted discharge weight increased 360 g, compared with median adjusted weight, which was estimated to have increased 316 g.
Median unadjusted z scores for weight increased 0.22 standard units over the 14-year period, compared with median adjusted z scores for weight at discharge, which increased an estimated 0.19 standard units.
The proportion of infants who were consuming human milk at discharge increased over the study period from 40% in 2005 to 48% in 2018. The use of cardiorespiratory monitors and oxygen decreased from 49% to 26%, and 27% to 22% respectively. The number of infants who were never transferred to specialized care before discharge to home also improved, from 71% to 76%.
Despite the unknowns, good news for managing pediatricians?
In a separate interview, study author Dr. Edwards noted that “infants born very preterm, who are discharged home from the NICU today, are larger and more physiologically mature than they were in 2005. Pediatricians will likely find this news to be positive as it may be easier to manage care for a more physiologically mature [infant],” and it may reduce risk of readmission.
“Infants stayed, on average, 8 days longer in 2018 than they did in 2005. That is 8 days when they were not at home with their families. Despite efforts by NICU teams to increase family-centered care, the NICU is not the same as being at home. ... That extra time in the NICU cost [some families] an estimated $28,000. ... As health care costs continue to rise, we need to understand the true cost [behind] this increase,” added Dr. Edwards, noting that more research is needed to understand what may be driving the increase in NICU length of stay and the possible implications. More research to investigate whether babies did better after discharge also is needed.
Going forward, Dr. Edwards indicated that she and her colleagues are exploring ways to measure apnea of prematurity (AOP) and use of continuous pulse oximetry (CPO) as the subject of future studies. In our study, we showed that the number of infants discharged home on a cardiorespiratory monitor decreased, but we do not know if that is explained by differences in management of AOP and CPO. “Understanding the influence of AOP and CPO management on discharge age would be an important contribution [to future research].”
AOP may drive increase in postmenstrual age
In an accompanying editorial, Cody Arnold, MD, and Alexis S. Davis, MD, said: “We have focused on apnea of prematurity and discharge countdowns in this commentary because we believe that changes in related practices are likely the most important drivers of the increases in postmenstrual age” reported by the authors in this study. “Other factors, such as increasing availability of NICU beds or decreasing availability of home support services, may have contributed to longer length of stay. But these questions should be answered by research, not by speculation,” said Dr. Arnold, neonatologist, University of Texas Health Sciences Center, Houston, and Dr. Davis, clinical associate professor, Stanford (Calif.) University.
“Prospective research comparing alternative countdown strategies on the basis of readmission rates and other outpatient outcomes is overdue.” Additional research is needed operationally to clearly outline parameters for countdown events, countdown duration, indications for CPO, outpatient caffeine use, and parental shared decision-making.”
The study was funded by the Vermont Oxford Network. Dr. Edwards received a grant from the Vermont Oxford Network; several others also had ties to the Network. Dr. Arnold and Dr. Davis had no conflicts of interest and reported no disclosures.
Gestational age and weight at discharge for infants aged 24-29 weeks increased steadily between 2005 and 2018, reported Erika M. Edwards, PhD, MPH, of the Vermont Oxford Network, Burlington, and associates.
Although they discussed several possible influencing factors, the authors were unable to explain the associated benefits, costs, and harms associated with increased age and weight at discharge, which remain undetermined. Infants are separated a week longer than they were at the beginning of the study period, the prolonged effects of which cannot be underestimated, Dr. Edwards and colleagues observed in a large cohort study in Pediatrics.
A total of 314,811 infants 24-29 weeks’ gestational age who were admitted to 824 neonatal ICUs (NICUs) throughout the United States survived to initial discharge. The median postmenstrual age at hospital discharge was 38.3 weeks. Over the 14-year period from 2005 to 2018, unadjusted postmenstrual age at discharge increased a median 9 days, compared with a median adjusted age of 8 days.
Of the 273,109 infants initially discharged from the hospital to home, median weight at discharge was 2,600 g. Over the 14 years from 2005 to 2018, median unadjusted discharge weight increased 360 g, compared with median adjusted weight, which was estimated to have increased 316 g.
Median unadjusted z scores for weight increased 0.22 standard units over the 14-year period, compared with median adjusted z scores for weight at discharge, which increased an estimated 0.19 standard units.
The proportion of infants who were consuming human milk at discharge increased over the study period from 40% in 2005 to 48% in 2018. The use of cardiorespiratory monitors and oxygen decreased from 49% to 26%, and 27% to 22% respectively. The number of infants who were never transferred to specialized care before discharge to home also improved, from 71% to 76%.
Despite the unknowns, good news for managing pediatricians?
In a separate interview, study author Dr. Edwards noted that “infants born very preterm, who are discharged home from the NICU today, are larger and more physiologically mature than they were in 2005. Pediatricians will likely find this news to be positive as it may be easier to manage care for a more physiologically mature [infant],” and it may reduce risk of readmission.
“Infants stayed, on average, 8 days longer in 2018 than they did in 2005. That is 8 days when they were not at home with their families. Despite efforts by NICU teams to increase family-centered care, the NICU is not the same as being at home. ... That extra time in the NICU cost [some families] an estimated $28,000. ... As health care costs continue to rise, we need to understand the true cost [behind] this increase,” added Dr. Edwards, noting that more research is needed to understand what may be driving the increase in NICU length of stay and the possible implications. More research to investigate whether babies did better after discharge also is needed.
Going forward, Dr. Edwards indicated that she and her colleagues are exploring ways to measure apnea of prematurity (AOP) and use of continuous pulse oximetry (CPO) as the subject of future studies. In our study, we showed that the number of infants discharged home on a cardiorespiratory monitor decreased, but we do not know if that is explained by differences in management of AOP and CPO. “Understanding the influence of AOP and CPO management on discharge age would be an important contribution [to future research].”
AOP may drive increase in postmenstrual age
In an accompanying editorial, Cody Arnold, MD, and Alexis S. Davis, MD, said: “We have focused on apnea of prematurity and discharge countdowns in this commentary because we believe that changes in related practices are likely the most important drivers of the increases in postmenstrual age” reported by the authors in this study. “Other factors, such as increasing availability of NICU beds or decreasing availability of home support services, may have contributed to longer length of stay. But these questions should be answered by research, not by speculation,” said Dr. Arnold, neonatologist, University of Texas Health Sciences Center, Houston, and Dr. Davis, clinical associate professor, Stanford (Calif.) University.
“Prospective research comparing alternative countdown strategies on the basis of readmission rates and other outpatient outcomes is overdue.” Additional research is needed operationally to clearly outline parameters for countdown events, countdown duration, indications for CPO, outpatient caffeine use, and parental shared decision-making.”
The study was funded by the Vermont Oxford Network. Dr. Edwards received a grant from the Vermont Oxford Network; several others also had ties to the Network. Dr. Arnold and Dr. Davis had no conflicts of interest and reported no disclosures.
FROM PEDIATRICS
Pediatric minority patients less likely to undergo ED imaging
Significant racial and ethnic differences in diagnostic imaging rates exist among children receiving care in pediatric EDs across the United States, Jennifer R. Marin, MD, of the University of Pittsburgh Medical Center Children’s Hospital of Pittsburgh, and associates reported.
Specifically, visits with non-Hispanic Black and Hispanic patients less frequently included radiography, CT, ultrasonography, and MRI than those of non-Hispanic White patients. The findings persisted across most diagnostic groups, even when stratified according to insurance type, Dr. Marin and colleagues reported in a multicenter cross-sectional study in JAMA Network Open.
The authors collected administrative data from the Pediatric Health Information System on 44 tertiary care children’s hospitals in 17 major metropolitan areas across the United States. They evaluated a total of 13,087,522 ED visits by 6,230,911 patients that occurred between Jan. 1, 2016, and Dec. 31, 2019. Of these, 28.2% included at least one imaging study. Altogether, 33.5% were performed on non-Hispanic White children, compared with just 24.1% of non-Hispanic Black children (adjusted odds ratio, 0.82) and 26.1% of Hispanic children (aOR, 0.87). After adjusting for relevant confounding factors, non-Hispanic Black and Hispanic children were less likely to have any imaging at all during their visits.
“Our findings suggest that a child’s race and ethnicity may be independently associated with the decision to perform imaging during ED visits,” Dr. Marin and associates said, adding that “the differential use of diagnostic imaging by race/ethnicity may reflect underuse of imaging in non-Hispanic Black and Hispanic children, or alternatively, overuse in non-Hispanic White children.”
Overuse vs. underuse: Racial bias or parental anxiety?
Overuse of imaging carries its own risks, but underuse can lead to misdiagnosis, the need for additional care, and possibly worse outcomes in the long run, Dr. Marin and colleagues explained. “Although we were unable to discern underuse from overuse using an administrative database, it is likely that much of the imaging in White children is unnecessary.”
Higher parental anxiety was just one of the explanations the authors offered for excessive imaging in White children. Especially in cases of diagnostic imaging for head trauma, one survey of adult ED patients showed that the peace of mind CT offers with its more definitive diagnosis was worth the additional possible risk of radiation.
Language barriers in non–English-speaking patients may also affect likelihood of testing as part of an ED visit.
Implicit physician racial bias, which can be amplified under the stress of working in an ED, can affect patient interactions, treatment decisions and adherence, and ultimately overall health outcomes, the authors noted. The goal in ensuring parity is to routinely follow clinical guidelines and use objective scoring tools that minimize subjectivity. At the institutional level, internal quality assurance evaluations go a long way toward understanding and limiting bias.
Historically, White patients are more likely than minority patients to have a medical home, which can influence whether ED physicians order imaging studies and whether imaging of White patients may have been triggered by a primary care physician referral, Dr. Marin and associates said.
In an accompanying editorial, Anupam B. Kharbanda, MD, said these findings are “consistent with decades of previous research documenting inequalities in health care delivery ... [and] must be examined in the context of inequities within the social framework of a community.”
Going back to the drawing board
“Physicians, researchers, and health care leaders must partner with the communities they serve to develop and implement interventions to address these substantial inequities in care,” said Dr. Kharbanda, pediatric emergency medicine physician at Children’s Minnesota Hospital, Minneapolis. As previous studies have demonstrated, implicit bias and antiracism training are needed to help physicians develop empathy so they are better equipped to help patients and families in a multicultural environment. Partnering with community-based organizations to ensure that care is more community centered, as has been done successfully within the Kaiser Permanente health system, for example, and employing a more diverse workforce that mirrors the populations cared for will go a long way.
Citing a 1966 speech of the late Dr. Martin Luther King, Jr., in which he said: “Of all the forms of inequality, injustice in health care is the most shocking and inhumane,” Dr. Kharbanda urged clinicians to not only hear but believe these words and act on them by working in partnerships with the communities they serve.
In a separate interview, Walter Palmer, MD, pediatric emergency medicine fellow at Children’s National Medical Center, Washington, noted: “This study’s findings are disappointing and yet not at all unexpected, as the authors convincingly identify yet another step at which patients of color are treated unequally in the U.S. health care system. It highlights a frightening truth: That we are all at risk of letting invisible implicit biases impact our clinical decision-making process. This is especially true in the busy emergency department environment, where pressure to make swift decisions regarding diagnostic workup and management invites the influence of imperceptible biases. It is now incumbent upon us as health care providers to monitor our personal and departmental patterns of practice for areas in which we can improve racial health equity and become advocates for the children and families who entrust us with their care.”
The authors reported multiple financial disclosures. Dr. Kharbanda and Dr. Palmer had no conflicts of interest and reported no disclosures.
Significant racial and ethnic differences in diagnostic imaging rates exist among children receiving care in pediatric EDs across the United States, Jennifer R. Marin, MD, of the University of Pittsburgh Medical Center Children’s Hospital of Pittsburgh, and associates reported.
Specifically, visits with non-Hispanic Black and Hispanic patients less frequently included radiography, CT, ultrasonography, and MRI than those of non-Hispanic White patients. The findings persisted across most diagnostic groups, even when stratified according to insurance type, Dr. Marin and colleagues reported in a multicenter cross-sectional study in JAMA Network Open.
The authors collected administrative data from the Pediatric Health Information System on 44 tertiary care children’s hospitals in 17 major metropolitan areas across the United States. They evaluated a total of 13,087,522 ED visits by 6,230,911 patients that occurred between Jan. 1, 2016, and Dec. 31, 2019. Of these, 28.2% included at least one imaging study. Altogether, 33.5% were performed on non-Hispanic White children, compared with just 24.1% of non-Hispanic Black children (adjusted odds ratio, 0.82) and 26.1% of Hispanic children (aOR, 0.87). After adjusting for relevant confounding factors, non-Hispanic Black and Hispanic children were less likely to have any imaging at all during their visits.
“Our findings suggest that a child’s race and ethnicity may be independently associated with the decision to perform imaging during ED visits,” Dr. Marin and associates said, adding that “the differential use of diagnostic imaging by race/ethnicity may reflect underuse of imaging in non-Hispanic Black and Hispanic children, or alternatively, overuse in non-Hispanic White children.”
Overuse vs. underuse: Racial bias or parental anxiety?
Overuse of imaging carries its own risks, but underuse can lead to misdiagnosis, the need for additional care, and possibly worse outcomes in the long run, Dr. Marin and colleagues explained. “Although we were unable to discern underuse from overuse using an administrative database, it is likely that much of the imaging in White children is unnecessary.”
Higher parental anxiety was just one of the explanations the authors offered for excessive imaging in White children. Especially in cases of diagnostic imaging for head trauma, one survey of adult ED patients showed that the peace of mind CT offers with its more definitive diagnosis was worth the additional possible risk of radiation.
Language barriers in non–English-speaking patients may also affect likelihood of testing as part of an ED visit.
Implicit physician racial bias, which can be amplified under the stress of working in an ED, can affect patient interactions, treatment decisions and adherence, and ultimately overall health outcomes, the authors noted. The goal in ensuring parity is to routinely follow clinical guidelines and use objective scoring tools that minimize subjectivity. At the institutional level, internal quality assurance evaluations go a long way toward understanding and limiting bias.
Historically, White patients are more likely than minority patients to have a medical home, which can influence whether ED physicians order imaging studies and whether imaging of White patients may have been triggered by a primary care physician referral, Dr. Marin and associates said.
In an accompanying editorial, Anupam B. Kharbanda, MD, said these findings are “consistent with decades of previous research documenting inequalities in health care delivery ... [and] must be examined in the context of inequities within the social framework of a community.”
Going back to the drawing board
“Physicians, researchers, and health care leaders must partner with the communities they serve to develop and implement interventions to address these substantial inequities in care,” said Dr. Kharbanda, pediatric emergency medicine physician at Children’s Minnesota Hospital, Minneapolis. As previous studies have demonstrated, implicit bias and antiracism training are needed to help physicians develop empathy so they are better equipped to help patients and families in a multicultural environment. Partnering with community-based organizations to ensure that care is more community centered, as has been done successfully within the Kaiser Permanente health system, for example, and employing a more diverse workforce that mirrors the populations cared for will go a long way.
Citing a 1966 speech of the late Dr. Martin Luther King, Jr., in which he said: “Of all the forms of inequality, injustice in health care is the most shocking and inhumane,” Dr. Kharbanda urged clinicians to not only hear but believe these words and act on them by working in partnerships with the communities they serve.
In a separate interview, Walter Palmer, MD, pediatric emergency medicine fellow at Children’s National Medical Center, Washington, noted: “This study’s findings are disappointing and yet not at all unexpected, as the authors convincingly identify yet another step at which patients of color are treated unequally in the U.S. health care system. It highlights a frightening truth: That we are all at risk of letting invisible implicit biases impact our clinical decision-making process. This is especially true in the busy emergency department environment, where pressure to make swift decisions regarding diagnostic workup and management invites the influence of imperceptible biases. It is now incumbent upon us as health care providers to monitor our personal and departmental patterns of practice for areas in which we can improve racial health equity and become advocates for the children and families who entrust us with their care.”
The authors reported multiple financial disclosures. Dr. Kharbanda and Dr. Palmer had no conflicts of interest and reported no disclosures.
Significant racial and ethnic differences in diagnostic imaging rates exist among children receiving care in pediatric EDs across the United States, Jennifer R. Marin, MD, of the University of Pittsburgh Medical Center Children’s Hospital of Pittsburgh, and associates reported.
Specifically, visits with non-Hispanic Black and Hispanic patients less frequently included radiography, CT, ultrasonography, and MRI than those of non-Hispanic White patients. The findings persisted across most diagnostic groups, even when stratified according to insurance type, Dr. Marin and colleagues reported in a multicenter cross-sectional study in JAMA Network Open.
The authors collected administrative data from the Pediatric Health Information System on 44 tertiary care children’s hospitals in 17 major metropolitan areas across the United States. They evaluated a total of 13,087,522 ED visits by 6,230,911 patients that occurred between Jan. 1, 2016, and Dec. 31, 2019. Of these, 28.2% included at least one imaging study. Altogether, 33.5% were performed on non-Hispanic White children, compared with just 24.1% of non-Hispanic Black children (adjusted odds ratio, 0.82) and 26.1% of Hispanic children (aOR, 0.87). After adjusting for relevant confounding factors, non-Hispanic Black and Hispanic children were less likely to have any imaging at all during their visits.
“Our findings suggest that a child’s race and ethnicity may be independently associated with the decision to perform imaging during ED visits,” Dr. Marin and associates said, adding that “the differential use of diagnostic imaging by race/ethnicity may reflect underuse of imaging in non-Hispanic Black and Hispanic children, or alternatively, overuse in non-Hispanic White children.”
Overuse vs. underuse: Racial bias or parental anxiety?
Overuse of imaging carries its own risks, but underuse can lead to misdiagnosis, the need for additional care, and possibly worse outcomes in the long run, Dr. Marin and colleagues explained. “Although we were unable to discern underuse from overuse using an administrative database, it is likely that much of the imaging in White children is unnecessary.”
Higher parental anxiety was just one of the explanations the authors offered for excessive imaging in White children. Especially in cases of diagnostic imaging for head trauma, one survey of adult ED patients showed that the peace of mind CT offers with its more definitive diagnosis was worth the additional possible risk of radiation.
Language barriers in non–English-speaking patients may also affect likelihood of testing as part of an ED visit.
Implicit physician racial bias, which can be amplified under the stress of working in an ED, can affect patient interactions, treatment decisions and adherence, and ultimately overall health outcomes, the authors noted. The goal in ensuring parity is to routinely follow clinical guidelines and use objective scoring tools that minimize subjectivity. At the institutional level, internal quality assurance evaluations go a long way toward understanding and limiting bias.
Historically, White patients are more likely than minority patients to have a medical home, which can influence whether ED physicians order imaging studies and whether imaging of White patients may have been triggered by a primary care physician referral, Dr. Marin and associates said.
In an accompanying editorial, Anupam B. Kharbanda, MD, said these findings are “consistent with decades of previous research documenting inequalities in health care delivery ... [and] must be examined in the context of inequities within the social framework of a community.”
Going back to the drawing board
“Physicians, researchers, and health care leaders must partner with the communities they serve to develop and implement interventions to address these substantial inequities in care,” said Dr. Kharbanda, pediatric emergency medicine physician at Children’s Minnesota Hospital, Minneapolis. As previous studies have demonstrated, implicit bias and antiracism training are needed to help physicians develop empathy so they are better equipped to help patients and families in a multicultural environment. Partnering with community-based organizations to ensure that care is more community centered, as has been done successfully within the Kaiser Permanente health system, for example, and employing a more diverse workforce that mirrors the populations cared for will go a long way.
Citing a 1966 speech of the late Dr. Martin Luther King, Jr., in which he said: “Of all the forms of inequality, injustice in health care is the most shocking and inhumane,” Dr. Kharbanda urged clinicians to not only hear but believe these words and act on them by working in partnerships with the communities they serve.
In a separate interview, Walter Palmer, MD, pediatric emergency medicine fellow at Children’s National Medical Center, Washington, noted: “This study’s findings are disappointing and yet not at all unexpected, as the authors convincingly identify yet another step at which patients of color are treated unequally in the U.S. health care system. It highlights a frightening truth: That we are all at risk of letting invisible implicit biases impact our clinical decision-making process. This is especially true in the busy emergency department environment, where pressure to make swift decisions regarding diagnostic workup and management invites the influence of imperceptible biases. It is now incumbent upon us as health care providers to monitor our personal and departmental patterns of practice for areas in which we can improve racial health equity and become advocates for the children and families who entrust us with their care.”
The authors reported multiple financial disclosures. Dr. Kharbanda and Dr. Palmer had no conflicts of interest and reported no disclosures.
FROM JAMA NETWORK OPEN
Oral antibiotic treats most children with UTI
Oral antibiotic treatment for 7-10 days works for most feverish children with uncomplicated urinary tract infection (UTI), reported Tej K. Mattoo, MD, of Wayne State University, Detroit, and associates.
A good clinical assessment supported by laboratory results using a clean urine specimen is crucial to accurately diagnosing UTI in children, Dr. Mattoo and colleagues reported in a state-of-the-art review article in Pediatrics.
The authors set out to summarize the current literature on UTI in children with the goal of guiding clinical management. They provide a thorough summary of the research on a wide range of issues, including pathogenesis of acute pyelonephritis and renal scarring, risk factors for UTI and renal scarring, diagnosis and common errors in diagnosis, complications of UTI and post-UTI renal imaging, antibiotics, antimicrobial prophylaxis, surgical interventions, and prevention of recurrent UTIs.
What key steps make all the difference?
To help guide practicing physicians through this wealth of information, Dr. Mattoo noted in an interview that, although the review article offers “many takeaway messages,” there are several issues of crucial importance. Notably, urine collection in young children who are not yet toilet trained can present considerable challenges in achieving an accurate assessment. A contaminated urine specimen leads to unnecessary antibiotic treatment, and in some cases unwarranted hospitalization, intravenous lines, renal imaging, and follow-up investigations, Dr. Mattoo said.
Ureteral catheterization or suprapubic bladder aspiration are the preferred methods of specimen collection, especially in cases where specimens collected with a perineal bag are dipstick positive, the authors explained. Midstream collection (known as the Quick-Wee method) can also be used following stimulation of the suprapubic area with cold fluid-soaked gauze.
Also of considerable importance is distinguishing bladder infections from kidney infections whenever possible, Dr. Mattoo noted. The antibiotic treatment, complications, and follow-up plans can be different for each, he cautioned. The authors have provided a helpful table within the article to help make this differentiation.
Timing is crucial
Prescribing treatment with an antibiotic within 48 hours of fever onset is essential for the prevention of renal scarring, Dr. Mattoo advised. The key is to treat with the goal of avoiding long-term complications. Although there are some exceptions, most cases of UTI can be treated with oral antibiotics and do not require hospitalization.
Some children with first UTI need additional testing, such as renal imaging, to ensure that there are no underlying risk factors for UTI. These children, in particular, can be at an increased risk of recurrent UTI and renal scarring, Dr. Mattoo explained.
Antibiotic resistance is a major emerging problem in patients with UTI at all ages and we should use antibiotics only in patients who truly have a UTI that requires such treatment, he urged.
In an interview, Timothy Joos, MD, a Seattle internist and pediatrician in private practice, noted: “In the words of the British novelist Tom Holt, ‘There are few moments of clarity more profound than those that follow the emptying of an overcharged bladder. The world slows down, the focus sharpens, the brain comes back online. Huge nebulous difficulties prove on close calm examination to be merely cloud giants.’ Thank you to Drs. Mattoo, Nelson, and Shaikh for providing this clarity of current UTI diagnosis and management,” Dr. Joos said.
“It bears repeating that because of the rare prevalence of grade 4 to 5 vesicoureteral reflux in children with their first UTI, current guidelines recommend that a voiding cystourethrogram can be reserved for children with an abnormal ultrasound, atypical pathogen, complicated clinical course, or known renal scarring,” added Dr. Joos.
The authors had no relevant disclosures. Dr. Joos is a member of the Pediatric News editorial advisory board but had no other disclosures.
Oral antibiotic treatment for 7-10 days works for most feverish children with uncomplicated urinary tract infection (UTI), reported Tej K. Mattoo, MD, of Wayne State University, Detroit, and associates.
A good clinical assessment supported by laboratory results using a clean urine specimen is crucial to accurately diagnosing UTI in children, Dr. Mattoo and colleagues reported in a state-of-the-art review article in Pediatrics.
The authors set out to summarize the current literature on UTI in children with the goal of guiding clinical management. They provide a thorough summary of the research on a wide range of issues, including pathogenesis of acute pyelonephritis and renal scarring, risk factors for UTI and renal scarring, diagnosis and common errors in diagnosis, complications of UTI and post-UTI renal imaging, antibiotics, antimicrobial prophylaxis, surgical interventions, and prevention of recurrent UTIs.
What key steps make all the difference?
To help guide practicing physicians through this wealth of information, Dr. Mattoo noted in an interview that, although the review article offers “many takeaway messages,” there are several issues of crucial importance. Notably, urine collection in young children who are not yet toilet trained can present considerable challenges in achieving an accurate assessment. A contaminated urine specimen leads to unnecessary antibiotic treatment, and in some cases unwarranted hospitalization, intravenous lines, renal imaging, and follow-up investigations, Dr. Mattoo said.
Ureteral catheterization or suprapubic bladder aspiration are the preferred methods of specimen collection, especially in cases where specimens collected with a perineal bag are dipstick positive, the authors explained. Midstream collection (known as the Quick-Wee method) can also be used following stimulation of the suprapubic area with cold fluid-soaked gauze.
Also of considerable importance is distinguishing bladder infections from kidney infections whenever possible, Dr. Mattoo noted. The antibiotic treatment, complications, and follow-up plans can be different for each, he cautioned. The authors have provided a helpful table within the article to help make this differentiation.
Timing is crucial
Prescribing treatment with an antibiotic within 48 hours of fever onset is essential for the prevention of renal scarring, Dr. Mattoo advised. The key is to treat with the goal of avoiding long-term complications. Although there are some exceptions, most cases of UTI can be treated with oral antibiotics and do not require hospitalization.
Some children with first UTI need additional testing, such as renal imaging, to ensure that there are no underlying risk factors for UTI. These children, in particular, can be at an increased risk of recurrent UTI and renal scarring, Dr. Mattoo explained.
Antibiotic resistance is a major emerging problem in patients with UTI at all ages and we should use antibiotics only in patients who truly have a UTI that requires such treatment, he urged.
In an interview, Timothy Joos, MD, a Seattle internist and pediatrician in private practice, noted: “In the words of the British novelist Tom Holt, ‘There are few moments of clarity more profound than those that follow the emptying of an overcharged bladder. The world slows down, the focus sharpens, the brain comes back online. Huge nebulous difficulties prove on close calm examination to be merely cloud giants.’ Thank you to Drs. Mattoo, Nelson, and Shaikh for providing this clarity of current UTI diagnosis and management,” Dr. Joos said.
“It bears repeating that because of the rare prevalence of grade 4 to 5 vesicoureteral reflux in children with their first UTI, current guidelines recommend that a voiding cystourethrogram can be reserved for children with an abnormal ultrasound, atypical pathogen, complicated clinical course, or known renal scarring,” added Dr. Joos.
The authors had no relevant disclosures. Dr. Joos is a member of the Pediatric News editorial advisory board but had no other disclosures.
Oral antibiotic treatment for 7-10 days works for most feverish children with uncomplicated urinary tract infection (UTI), reported Tej K. Mattoo, MD, of Wayne State University, Detroit, and associates.
A good clinical assessment supported by laboratory results using a clean urine specimen is crucial to accurately diagnosing UTI in children, Dr. Mattoo and colleagues reported in a state-of-the-art review article in Pediatrics.
The authors set out to summarize the current literature on UTI in children with the goal of guiding clinical management. They provide a thorough summary of the research on a wide range of issues, including pathogenesis of acute pyelonephritis and renal scarring, risk factors for UTI and renal scarring, diagnosis and common errors in diagnosis, complications of UTI and post-UTI renal imaging, antibiotics, antimicrobial prophylaxis, surgical interventions, and prevention of recurrent UTIs.
What key steps make all the difference?
To help guide practicing physicians through this wealth of information, Dr. Mattoo noted in an interview that, although the review article offers “many takeaway messages,” there are several issues of crucial importance. Notably, urine collection in young children who are not yet toilet trained can present considerable challenges in achieving an accurate assessment. A contaminated urine specimen leads to unnecessary antibiotic treatment, and in some cases unwarranted hospitalization, intravenous lines, renal imaging, and follow-up investigations, Dr. Mattoo said.
Ureteral catheterization or suprapubic bladder aspiration are the preferred methods of specimen collection, especially in cases where specimens collected with a perineal bag are dipstick positive, the authors explained. Midstream collection (known as the Quick-Wee method) can also be used following stimulation of the suprapubic area with cold fluid-soaked gauze.
Also of considerable importance is distinguishing bladder infections from kidney infections whenever possible, Dr. Mattoo noted. The antibiotic treatment, complications, and follow-up plans can be different for each, he cautioned. The authors have provided a helpful table within the article to help make this differentiation.
Timing is crucial
Prescribing treatment with an antibiotic within 48 hours of fever onset is essential for the prevention of renal scarring, Dr. Mattoo advised. The key is to treat with the goal of avoiding long-term complications. Although there are some exceptions, most cases of UTI can be treated with oral antibiotics and do not require hospitalization.
Some children with first UTI need additional testing, such as renal imaging, to ensure that there are no underlying risk factors for UTI. These children, in particular, can be at an increased risk of recurrent UTI and renal scarring, Dr. Mattoo explained.
Antibiotic resistance is a major emerging problem in patients with UTI at all ages and we should use antibiotics only in patients who truly have a UTI that requires such treatment, he urged.
In an interview, Timothy Joos, MD, a Seattle internist and pediatrician in private practice, noted: “In the words of the British novelist Tom Holt, ‘There are few moments of clarity more profound than those that follow the emptying of an overcharged bladder. The world slows down, the focus sharpens, the brain comes back online. Huge nebulous difficulties prove on close calm examination to be merely cloud giants.’ Thank you to Drs. Mattoo, Nelson, and Shaikh for providing this clarity of current UTI diagnosis and management,” Dr. Joos said.
“It bears repeating that because of the rare prevalence of grade 4 to 5 vesicoureteral reflux in children with their first UTI, current guidelines recommend that a voiding cystourethrogram can be reserved for children with an abnormal ultrasound, atypical pathogen, complicated clinical course, or known renal scarring,” added Dr. Joos.
The authors had no relevant disclosures. Dr. Joos is a member of the Pediatric News editorial advisory board but had no other disclosures.
FROM PEDIATRICS
Menopause, not aging, may influence brain volume
Postmenopausal women not only have larger brain volume than women who are premenopausal, but they also experience larger reductions in brain volume over time, reported Ananthan Ambikairajah of the Centre for Research on Ageing, Health and Wellbeing, Australian National University, Canberra, and associates. Their report was published in Menopause.
In this large population-based cohort of 5,072 women aged 37-73 years, the goal of the study was to look at links between brain volume and measures of menstruation history, such as menopausal status, age at menopause, age at menarche, and the duration of a woman’s reproductive stage, but to do so within the context of how it relates to dementia prevalence. Citing a study in The Lancet Neurology, the authors noted that the age-standardized prevalence for dementia is 17% higher in women than in men, and they speculated that it may be important to look beyond age for answers.
What about menstrual history and Alzheimer’s disease?
According to the Framingham Study in Neurology, the remaining lifetime risk of Alzheimer’s disease (AD) is nearly double for a 65-year-old woman (12%) compared with a 65-year-old man (6.3%), leading Mr. Ambikairajah and associates to conclude that “menstruation history may also be particularly relevant, given that it is unique to female aging.” They further speculated, citing several related studies, that because AD pathology is initiated decades prior to the onset of clinical signs, menstruation history and its effects on brain health may, in fact, be reflected in brain volume.
Postmenopausal women had 0.82% and 1.33% larger total brain and hippocampal volume, respectively, compared with premenopausal women. Postmenopausal women had a 23% greater decrease in total brain volume but not in hippocampal volume over time, compared with premenopausal women.
As Braak and Braak illustrated in Acta Neuropathologica, chronic inflammation has been linked to brain shrinkage “consistent with the pattern of results in the present study,” Mr. Ambikairajah and colleagues noted, adding that longitudinal neuroimaging/biomarker studies are needed to explore this further.
What made this study unique was its ability to match pre- and postmenopausal women for age, a critically important attribute “given that aging and menopause both progress concurrently, which can make it difficult to determine the individual contribution of each for measures of brain health,” the authors explained.
In an interview, Constance Bohon, MD, an ob.gyn. in private practice and assistant clinical professor, George Washington University, Washington, observed: “The conclusion [in this study] is that an early age of menarche, delayed age of menopause and increased duration of the reproductive stage is negatively associated with brain volume.”
What of the neuroprotective effects of endogenous estrogen?
“Their findings are not consistent with a neuroprotective effect of endogenous estrogen exposure on brain volume,” she noted, adding that the study “did not assess the effect of exogenous estrogen on brain volume. Neither was the effect of exogenous or endogenous estrogen on cerebral blood flow assessed. In a study published in Obstetrics & Gynecology, the conclusion was that oophorectomy before the age of natural menopause is associated with a decrease in cognitive impairment and dementia. There was no assessment of brain volume or cerebral blood flow. Likewise in a report published in Neurobiology of Aging, Maki P and Resnick S M. concluded that estrogen helps maintain hippocampal and prefrontal function as women age,” observed Dr. Bohon, noting that the study did not assess brain volume.
“It is unclear whether the most predictive assessment for worsening cognition and dementia is the finding of decreased total brain volume, decreased hippocampal volume, or decreased cerebral blood flow. The effect of both endogenous and exogenous estrogen on the risk for dementia needs further evaluation,” she cautioned.
Mr. Ambikairajah cited one financial disclosure; the remaining contributors had no relevant disclosures.
Postmenopausal women not only have larger brain volume than women who are premenopausal, but they also experience larger reductions in brain volume over time, reported Ananthan Ambikairajah of the Centre for Research on Ageing, Health and Wellbeing, Australian National University, Canberra, and associates. Their report was published in Menopause.
In this large population-based cohort of 5,072 women aged 37-73 years, the goal of the study was to look at links between brain volume and measures of menstruation history, such as menopausal status, age at menopause, age at menarche, and the duration of a woman’s reproductive stage, but to do so within the context of how it relates to dementia prevalence. Citing a study in The Lancet Neurology, the authors noted that the age-standardized prevalence for dementia is 17% higher in women than in men, and they speculated that it may be important to look beyond age for answers.
What about menstrual history and Alzheimer’s disease?
According to the Framingham Study in Neurology, the remaining lifetime risk of Alzheimer’s disease (AD) is nearly double for a 65-year-old woman (12%) compared with a 65-year-old man (6.3%), leading Mr. Ambikairajah and associates to conclude that “menstruation history may also be particularly relevant, given that it is unique to female aging.” They further speculated, citing several related studies, that because AD pathology is initiated decades prior to the onset of clinical signs, menstruation history and its effects on brain health may, in fact, be reflected in brain volume.
Postmenopausal women had 0.82% and 1.33% larger total brain and hippocampal volume, respectively, compared with premenopausal women. Postmenopausal women had a 23% greater decrease in total brain volume but not in hippocampal volume over time, compared with premenopausal women.
As Braak and Braak illustrated in Acta Neuropathologica, chronic inflammation has been linked to brain shrinkage “consistent with the pattern of results in the present study,” Mr. Ambikairajah and colleagues noted, adding that longitudinal neuroimaging/biomarker studies are needed to explore this further.
What made this study unique was its ability to match pre- and postmenopausal women for age, a critically important attribute “given that aging and menopause both progress concurrently, which can make it difficult to determine the individual contribution of each for measures of brain health,” the authors explained.
In an interview, Constance Bohon, MD, an ob.gyn. in private practice and assistant clinical professor, George Washington University, Washington, observed: “The conclusion [in this study] is that an early age of menarche, delayed age of menopause and increased duration of the reproductive stage is negatively associated with brain volume.”
What of the neuroprotective effects of endogenous estrogen?
“Their findings are not consistent with a neuroprotective effect of endogenous estrogen exposure on brain volume,” she noted, adding that the study “did not assess the effect of exogenous estrogen on brain volume. Neither was the effect of exogenous or endogenous estrogen on cerebral blood flow assessed. In a study published in Obstetrics & Gynecology, the conclusion was that oophorectomy before the age of natural menopause is associated with a decrease in cognitive impairment and dementia. There was no assessment of brain volume or cerebral blood flow. Likewise in a report published in Neurobiology of Aging, Maki P and Resnick S M. concluded that estrogen helps maintain hippocampal and prefrontal function as women age,” observed Dr. Bohon, noting that the study did not assess brain volume.
“It is unclear whether the most predictive assessment for worsening cognition and dementia is the finding of decreased total brain volume, decreased hippocampal volume, or decreased cerebral blood flow. The effect of both endogenous and exogenous estrogen on the risk for dementia needs further evaluation,” she cautioned.
Mr. Ambikairajah cited one financial disclosure; the remaining contributors had no relevant disclosures.
Postmenopausal women not only have larger brain volume than women who are premenopausal, but they also experience larger reductions in brain volume over time, reported Ananthan Ambikairajah of the Centre for Research on Ageing, Health and Wellbeing, Australian National University, Canberra, and associates. Their report was published in Menopause.
In this large population-based cohort of 5,072 women aged 37-73 years, the goal of the study was to look at links between brain volume and measures of menstruation history, such as menopausal status, age at menopause, age at menarche, and the duration of a woman’s reproductive stage, but to do so within the context of how it relates to dementia prevalence. Citing a study in The Lancet Neurology, the authors noted that the age-standardized prevalence for dementia is 17% higher in women than in men, and they speculated that it may be important to look beyond age for answers.
What about menstrual history and Alzheimer’s disease?
According to the Framingham Study in Neurology, the remaining lifetime risk of Alzheimer’s disease (AD) is nearly double for a 65-year-old woman (12%) compared with a 65-year-old man (6.3%), leading Mr. Ambikairajah and associates to conclude that “menstruation history may also be particularly relevant, given that it is unique to female aging.” They further speculated, citing several related studies, that because AD pathology is initiated decades prior to the onset of clinical signs, menstruation history and its effects on brain health may, in fact, be reflected in brain volume.
Postmenopausal women had 0.82% and 1.33% larger total brain and hippocampal volume, respectively, compared with premenopausal women. Postmenopausal women had a 23% greater decrease in total brain volume but not in hippocampal volume over time, compared with premenopausal women.
As Braak and Braak illustrated in Acta Neuropathologica, chronic inflammation has been linked to brain shrinkage “consistent with the pattern of results in the present study,” Mr. Ambikairajah and colleagues noted, adding that longitudinal neuroimaging/biomarker studies are needed to explore this further.
What made this study unique was its ability to match pre- and postmenopausal women for age, a critically important attribute “given that aging and menopause both progress concurrently, which can make it difficult to determine the individual contribution of each for measures of brain health,” the authors explained.
In an interview, Constance Bohon, MD, an ob.gyn. in private practice and assistant clinical professor, George Washington University, Washington, observed: “The conclusion [in this study] is that an early age of menarche, delayed age of menopause and increased duration of the reproductive stage is negatively associated with brain volume.”
What of the neuroprotective effects of endogenous estrogen?
“Their findings are not consistent with a neuroprotective effect of endogenous estrogen exposure on brain volume,” she noted, adding that the study “did not assess the effect of exogenous estrogen on brain volume. Neither was the effect of exogenous or endogenous estrogen on cerebral blood flow assessed. In a study published in Obstetrics & Gynecology, the conclusion was that oophorectomy before the age of natural menopause is associated with a decrease in cognitive impairment and dementia. There was no assessment of brain volume or cerebral blood flow. Likewise in a report published in Neurobiology of Aging, Maki P and Resnick S M. concluded that estrogen helps maintain hippocampal and prefrontal function as women age,” observed Dr. Bohon, noting that the study did not assess brain volume.
“It is unclear whether the most predictive assessment for worsening cognition and dementia is the finding of decreased total brain volume, decreased hippocampal volume, or decreased cerebral blood flow. The effect of both endogenous and exogenous estrogen on the risk for dementia needs further evaluation,” she cautioned.
Mr. Ambikairajah cited one financial disclosure; the remaining contributors had no relevant disclosures.
FROM MENOPAUSE
Peripartum maternal oxygen supplementation shows little benefit
Peripartum maternal oxygen supplementation does not yield a clinically relevant improvement in umbilical artery gas pH or other neonatal outcomes, reported Nandini Raghuraman, MD, MS, of the Washington University School of Medicine, St. Louis, MO, and her associates.
In a meta-analysis of 16 studies identified between Feb. 18 and April 3, 2020, the investigators sought to determine whether maternal oxygen supplementation during delivery leads to improved measures in umbilical artery (UA) gas and neonatal outcomes. Using data from randomized clinical trials, they compared peripartum oxygen supplementation with room air and examined the link between oxygen delivery during regular labor or planned cesarean delivery (CD) with UA gas measures and other neonatal outcomes.
Altogether, 1,078 patients were randomized to the oxygen group or the room air group. UA pH remained similar between the two groups even after the researchers factored in risk of bias, use of low-flow devices, or FIO2 below 60%, noted the authors. Oxygen supplementation also appeared to reduce rates of UA pH that were less than 7.2 and increase UA PaO2 relative to room air during scheduled cesarean deliveries, they added.
Considerable interstudy heterogeneity was found
Although marginally lower one-minute Apgar scores were observed in infants whose mothers received oxygen during cesarean delivery, the mean difference between oxygen and room air was less than a point and there were no other statistically significant differences in any secondary outcomes, the authors said. Considerable interstudy heterogeneity was noted across most of the study outcomes.
It is important to note that results pooled from all the studies reviewed indicated an increase in UA PaO2 but no notable differences in UA pH when oxygen was used. Citing multiple studies included in the review, the authors observed that UA PaO2 is a “poor estimator of neonatal morbidity” because, when evaluated in cord blood gas, it represents dissolved oxygen and is not an accurate indication of how much oxygen is bound to hemoglobin. For this reason, dissolved oxygen content by itself is not an indication of hypoxia or subpar tissue oxygenation.
“Prolonged tissue hypoxia leads to anaerobic metabolism, resulting in decreased pH, which is why UA pH ultimately serves as a better marker for prediction of neonatal morbidity. An intervention that increases the PaO2 without concomitantly increasing the pH has limited clinical benefit, particularly because hyperoxemia is associated with production of free radicals and oxidative cell damage in adults and neonates,” they explained.
With unproven benefits and potential for risk of harm, prolonged oxygen use should be limited
“A large, adequately powered trial is needed to investigate the effect of maternal oxygen supplementation in response to fetal heart rate tracings on short- and long-term neonatal morbidity,” the authors suggested. For the time being, they cautioned limiting prolonged oxygen use since the benefits are unproven and there is a potential risk of harm.
In a separate interview, Iris Krishna, MD, MPH, FACOG, Emory University, Atlanta, noted, “The use of maternal supplemental oxygen with the intent of improving fetal oxygenation is a common clinical practice. Previous studies on maternal oxygen supplementation during labor have yielded conflicting results; however, there is growing literature suggesting that maternal intrapartum supplemental oxygenation may not provide clinically significant benefit and there may even be potential harm to mother and baby.
“Unique to this meta-analysis is evaluation of maternal oxygen supplementation in the presence or absence of labor, hypothesizing that placental oxygen transfer may be affected by regular uterine contractions. The pooled results suggest that the use of maternal supplemental oxygenation does not result in clinically relevant fetal oxygenation in the presence or absence of labor when compared to room air. A limitation of this meta-analysis is that the use of oxygen in response to nonreassuring fetal tracing was not assessed, the most common clinical indication for maternal oxygen supplementation.
“This study further challenges the practice of maternal intrapartum supplemental oxygen and highlights that we have much to learn about the impact of this practice. More research is needed to assess optimal duration of oxygen supplementation, safety and efficacy of oxygen supplementation, appropriate clinical indications for oxygen supplementation, as well as the long-term neonatal outcomes of in utero hyperoxygenation.“
Dr. Raghuraman reported receiving multiple grants and acknowledged multiple funding sources. Her colleagues and Dr. Krishna had no conflicts of interest to report.
Peripartum maternal oxygen supplementation does not yield a clinically relevant improvement in umbilical artery gas pH or other neonatal outcomes, reported Nandini Raghuraman, MD, MS, of the Washington University School of Medicine, St. Louis, MO, and her associates.
In a meta-analysis of 16 studies identified between Feb. 18 and April 3, 2020, the investigators sought to determine whether maternal oxygen supplementation during delivery leads to improved measures in umbilical artery (UA) gas and neonatal outcomes. Using data from randomized clinical trials, they compared peripartum oxygen supplementation with room air and examined the link between oxygen delivery during regular labor or planned cesarean delivery (CD) with UA gas measures and other neonatal outcomes.
Altogether, 1,078 patients were randomized to the oxygen group or the room air group. UA pH remained similar between the two groups even after the researchers factored in risk of bias, use of low-flow devices, or FIO2 below 60%, noted the authors. Oxygen supplementation also appeared to reduce rates of UA pH that were less than 7.2 and increase UA PaO2 relative to room air during scheduled cesarean deliveries, they added.
Considerable interstudy heterogeneity was found
Although marginally lower one-minute Apgar scores were observed in infants whose mothers received oxygen during cesarean delivery, the mean difference between oxygen and room air was less than a point and there were no other statistically significant differences in any secondary outcomes, the authors said. Considerable interstudy heterogeneity was noted across most of the study outcomes.
It is important to note that results pooled from all the studies reviewed indicated an increase in UA PaO2 but no notable differences in UA pH when oxygen was used. Citing multiple studies included in the review, the authors observed that UA PaO2 is a “poor estimator of neonatal morbidity” because, when evaluated in cord blood gas, it represents dissolved oxygen and is not an accurate indication of how much oxygen is bound to hemoglobin. For this reason, dissolved oxygen content by itself is not an indication of hypoxia or subpar tissue oxygenation.
“Prolonged tissue hypoxia leads to anaerobic metabolism, resulting in decreased pH, which is why UA pH ultimately serves as a better marker for prediction of neonatal morbidity. An intervention that increases the PaO2 without concomitantly increasing the pH has limited clinical benefit, particularly because hyperoxemia is associated with production of free radicals and oxidative cell damage in adults and neonates,” they explained.
With unproven benefits and potential for risk of harm, prolonged oxygen use should be limited
“A large, adequately powered trial is needed to investigate the effect of maternal oxygen supplementation in response to fetal heart rate tracings on short- and long-term neonatal morbidity,” the authors suggested. For the time being, they cautioned limiting prolonged oxygen use since the benefits are unproven and there is a potential risk of harm.
In a separate interview, Iris Krishna, MD, MPH, FACOG, Emory University, Atlanta, noted, “The use of maternal supplemental oxygen with the intent of improving fetal oxygenation is a common clinical practice. Previous studies on maternal oxygen supplementation during labor have yielded conflicting results; however, there is growing literature suggesting that maternal intrapartum supplemental oxygenation may not provide clinically significant benefit and there may even be potential harm to mother and baby.
“Unique to this meta-analysis is evaluation of maternal oxygen supplementation in the presence or absence of labor, hypothesizing that placental oxygen transfer may be affected by regular uterine contractions. The pooled results suggest that the use of maternal supplemental oxygenation does not result in clinically relevant fetal oxygenation in the presence or absence of labor when compared to room air. A limitation of this meta-analysis is that the use of oxygen in response to nonreassuring fetal tracing was not assessed, the most common clinical indication for maternal oxygen supplementation.
“This study further challenges the practice of maternal intrapartum supplemental oxygen and highlights that we have much to learn about the impact of this practice. More research is needed to assess optimal duration of oxygen supplementation, safety and efficacy of oxygen supplementation, appropriate clinical indications for oxygen supplementation, as well as the long-term neonatal outcomes of in utero hyperoxygenation.“
Dr. Raghuraman reported receiving multiple grants and acknowledged multiple funding sources. Her colleagues and Dr. Krishna had no conflicts of interest to report.
Peripartum maternal oxygen supplementation does not yield a clinically relevant improvement in umbilical artery gas pH or other neonatal outcomes, reported Nandini Raghuraman, MD, MS, of the Washington University School of Medicine, St. Louis, MO, and her associates.
In a meta-analysis of 16 studies identified between Feb. 18 and April 3, 2020, the investigators sought to determine whether maternal oxygen supplementation during delivery leads to improved measures in umbilical artery (UA) gas and neonatal outcomes. Using data from randomized clinical trials, they compared peripartum oxygen supplementation with room air and examined the link between oxygen delivery during regular labor or planned cesarean delivery (CD) with UA gas measures and other neonatal outcomes.
Altogether, 1,078 patients were randomized to the oxygen group or the room air group. UA pH remained similar between the two groups even after the researchers factored in risk of bias, use of low-flow devices, or FIO2 below 60%, noted the authors. Oxygen supplementation also appeared to reduce rates of UA pH that were less than 7.2 and increase UA PaO2 relative to room air during scheduled cesarean deliveries, they added.
Considerable interstudy heterogeneity was found
Although marginally lower one-minute Apgar scores were observed in infants whose mothers received oxygen during cesarean delivery, the mean difference between oxygen and room air was less than a point and there were no other statistically significant differences in any secondary outcomes, the authors said. Considerable interstudy heterogeneity was noted across most of the study outcomes.
It is important to note that results pooled from all the studies reviewed indicated an increase in UA PaO2 but no notable differences in UA pH when oxygen was used. Citing multiple studies included in the review, the authors observed that UA PaO2 is a “poor estimator of neonatal morbidity” because, when evaluated in cord blood gas, it represents dissolved oxygen and is not an accurate indication of how much oxygen is bound to hemoglobin. For this reason, dissolved oxygen content by itself is not an indication of hypoxia or subpar tissue oxygenation.
“Prolonged tissue hypoxia leads to anaerobic metabolism, resulting in decreased pH, which is why UA pH ultimately serves as a better marker for prediction of neonatal morbidity. An intervention that increases the PaO2 without concomitantly increasing the pH has limited clinical benefit, particularly because hyperoxemia is associated with production of free radicals and oxidative cell damage in adults and neonates,” they explained.
With unproven benefits and potential for risk of harm, prolonged oxygen use should be limited
“A large, adequately powered trial is needed to investigate the effect of maternal oxygen supplementation in response to fetal heart rate tracings on short- and long-term neonatal morbidity,” the authors suggested. For the time being, they cautioned limiting prolonged oxygen use since the benefits are unproven and there is a potential risk of harm.
In a separate interview, Iris Krishna, MD, MPH, FACOG, Emory University, Atlanta, noted, “The use of maternal supplemental oxygen with the intent of improving fetal oxygenation is a common clinical practice. Previous studies on maternal oxygen supplementation during labor have yielded conflicting results; however, there is growing literature suggesting that maternal intrapartum supplemental oxygenation may not provide clinically significant benefit and there may even be potential harm to mother and baby.
“Unique to this meta-analysis is evaluation of maternal oxygen supplementation in the presence or absence of labor, hypothesizing that placental oxygen transfer may be affected by regular uterine contractions. The pooled results suggest that the use of maternal supplemental oxygenation does not result in clinically relevant fetal oxygenation in the presence or absence of labor when compared to room air. A limitation of this meta-analysis is that the use of oxygen in response to nonreassuring fetal tracing was not assessed, the most common clinical indication for maternal oxygen supplementation.
“This study further challenges the practice of maternal intrapartum supplemental oxygen and highlights that we have much to learn about the impact of this practice. More research is needed to assess optimal duration of oxygen supplementation, safety and efficacy of oxygen supplementation, appropriate clinical indications for oxygen supplementation, as well as the long-term neonatal outcomes of in utero hyperoxygenation.“
Dr. Raghuraman reported receiving multiple grants and acknowledged multiple funding sources. Her colleagues and Dr. Krishna had no conflicts of interest to report.
FROM JAMA PEDIATRICS
Early Head Start program boosts healthy eating, self-regulation
Home-based preventive interventions not only improve healthy eating habits and self-regulation in toddlers but also guide their parents toward better food presentation and response to picky behaviors, reported Robert L. Nix, PhD, of the University of Wisconsin, Madison, and his associates.
In a small, randomized controlled trial of 73 families with toddlers aged 18-36 months enrolled in home-based Early Head Start (EHS), the researchers evaluated four protective factors, including toddlers’ healthy eating habits, toddlers’ self-regulation, parents’ responsive feeding practices, and parents’ sensitive scaffolding. The study, conducted from April to October 2013, is the first clinical trial of Recipe 4 Success, a preschool-focused intervention created by administrators and home visitors of EHS that promotes healthy eating and self-regulation in toddlers living in poverty who may otherwise face weight challenges and obesity later in life. Integrating the intervention into EHS allowed the researchers to take full advantage of its national infrastructure and to make dissemination more efficient.
Of the families selected to participate, all of whom were living below the Federal poverty threshold, 66 were retained through post treatment. Most participating parents were biological mothers; 61% were single; 29% were not high school graduates; just 11% were employed full time. The toddlers averaged 30.72 months; 44% were female. Roughly 48% of families were non-Hispanic White; 29% were Black; and 23% were Hispanic or Latinx, the investigators reported in Pediatrics. More than three-quarters of participants were enrolled in the Special Supplemental Nutrition Program for Women, Infants, and Children or the Supplemental Nutrition Assistance Program.
The program allowed parents to transform toddler eating habits quickly
The study, which was designed to evaluate for posttreatment differences in the primary outcomes, involved 10 consecutive weekly lessons implemented by regularly assigned EHS home visitors. Parents were required to adhere to feeding practices carefully targeted with sensitive, structured scaffolding designed to keep toddlers from becoming overwhelmed. Parents were guided to understand, for instance, that toddlers frequently need to be exposed to a new food 10-20 times before eating it, and that poor sleep can have a detrimental influence on emotional and behavioral controls that can progress to weight gain.
Parent recall of what food and drinks their toddlers consumed in the previous 24-hour period was collected by interviewers. The percentage of all meals that included a fruit and/or vegetable, a protein source, and the absence of sweets and junk food were noted. Toddler self-regulation was assessed in accordance with delay of gratification, task orientation, and emotional/behavioral control. Parents were asked to rate toddler ability to cease desired activities to comply with parental requests. Parental responsive feeding practices were also recorded to observe how they introduce unique healthy foods and how they responded to their toddlers’ reactions. Parental sensitive scaffolding was similarly observed for their ability to structure activities in a developmentally appropriate manner promoting self-regulation.
The researchers noted no statistically significant differences between families in the treatment and control groups, nor were there differences in outcome measures or covariates. Study findings showed that, compared with toddlers who continued to receive just EHS support, the toddlers randomly assigned to Recipe 4 Success were more likely to consume snacks and meals that contained fruits, vegetables, protein, and no sweets or junk food.
As the results of this study and others have shown, early food preferences offer the strongest indication of later diet and healthy eating habits throughout life. The program targeted in this study is significant in its ability to accelerate the adoption of better toddler eating habits in just a 10-week period.
Recipe 4 Success along with other successful preventive interventions for young children are most effective when parents drive the change. “In the present trial, the quality of parenting was most highly related to healthy eating habits and self-regulation at baseline,” the researchers noted.
Specifically, the authors attributed the success of the program to “targeting specific interrelated outcomes with an integrated, theoretically driven intervention model,” which allowed Recipe 4 Success to boost the effectiveness of EHS substantially “in just 10 weeks with a minimal increase in funding,” the authors added.
The authors noted several weaknesses as well as strengths of the study. Its primary weakness was a baseline-posttreatment design, which made it impossible to assert that intervention effects can be sustained. The study was also limited to English-speaking families. Given that most home visitors attended to families in both Recipe 4 Success and EHS, the researchers noted the possibility for contamination across conditions, but they added that this would have actually reduced the intervention effects. The study’s primary strength was the evidenced-based nature of the randomized control. That Recipe 4 Success was operated as an intervention only strengthen the benefits of normal EHS visits.
Patient parents who promote self-regulation have the best chance of success
“This small study emphasizes the importance of parent education and support in setting the toddlers’ palate for lifelong eating habits and self-regulation,” observed Silver Spring, MD, private practice pediatrician and associate clinical professor of pediatrics at George Washington University, Washington, Lillian M. Beard, MD, in a separate interview.
“With the goal of promoting eating habits and self-regulation, I try to guide parents’ choices of what they offer to their toddler. I applaud parents’ patience as I encourage them not to give in and quickly resort to offering salty or sweet snacks. I suggest that if during the course of a day, a palette of colorful healthy choices is offered, most toddlers will graze independently as they go about their play. The challenge is to really support the parent through this quirky stage of their child’s development,” she explained.
“The ultimate challenge today with so much food insecurity, COVID-19 related job losses, and shrinking dollars to feed families is that too many families are feeling a food crisis! A program such as Recipe 4 Success can provide invaluable education for families on how to best stretch their few dollars, with knowledge of which items to seek from their community food pantries, how to best utilize items from the State WIC programs and still seek nutrition tips from their pediatricians while avoiding expensive fast foods that only offer immediate satiety and gratification. The Recipe 4 Success educator, pediatrician, or any community educator can give recommendations about which fresh produce may be inexpensive, but nutritional,” Dr. Beard suggested.
Dr. Nix and colleagues as well as Dr. Beard had no conflicts of interest and no relevant financial disclosures.
Home-based preventive interventions not only improve healthy eating habits and self-regulation in toddlers but also guide their parents toward better food presentation and response to picky behaviors, reported Robert L. Nix, PhD, of the University of Wisconsin, Madison, and his associates.
In a small, randomized controlled trial of 73 families with toddlers aged 18-36 months enrolled in home-based Early Head Start (EHS), the researchers evaluated four protective factors, including toddlers’ healthy eating habits, toddlers’ self-regulation, parents’ responsive feeding practices, and parents’ sensitive scaffolding. The study, conducted from April to October 2013, is the first clinical trial of Recipe 4 Success, a preschool-focused intervention created by administrators and home visitors of EHS that promotes healthy eating and self-regulation in toddlers living in poverty who may otherwise face weight challenges and obesity later in life. Integrating the intervention into EHS allowed the researchers to take full advantage of its national infrastructure and to make dissemination more efficient.
Of the families selected to participate, all of whom were living below the Federal poverty threshold, 66 were retained through post treatment. Most participating parents were biological mothers; 61% were single; 29% were not high school graduates; just 11% were employed full time. The toddlers averaged 30.72 months; 44% were female. Roughly 48% of families were non-Hispanic White; 29% were Black; and 23% were Hispanic or Latinx, the investigators reported in Pediatrics. More than three-quarters of participants were enrolled in the Special Supplemental Nutrition Program for Women, Infants, and Children or the Supplemental Nutrition Assistance Program.
The program allowed parents to transform toddler eating habits quickly
The study, which was designed to evaluate for posttreatment differences in the primary outcomes, involved 10 consecutive weekly lessons implemented by regularly assigned EHS home visitors. Parents were required to adhere to feeding practices carefully targeted with sensitive, structured scaffolding designed to keep toddlers from becoming overwhelmed. Parents were guided to understand, for instance, that toddlers frequently need to be exposed to a new food 10-20 times before eating it, and that poor sleep can have a detrimental influence on emotional and behavioral controls that can progress to weight gain.
Parent recall of what food and drinks their toddlers consumed in the previous 24-hour period was collected by interviewers. The percentage of all meals that included a fruit and/or vegetable, a protein source, and the absence of sweets and junk food were noted. Toddler self-regulation was assessed in accordance with delay of gratification, task orientation, and emotional/behavioral control. Parents were asked to rate toddler ability to cease desired activities to comply with parental requests. Parental responsive feeding practices were also recorded to observe how they introduce unique healthy foods and how they responded to their toddlers’ reactions. Parental sensitive scaffolding was similarly observed for their ability to structure activities in a developmentally appropriate manner promoting self-regulation.
The researchers noted no statistically significant differences between families in the treatment and control groups, nor were there differences in outcome measures or covariates. Study findings showed that, compared with toddlers who continued to receive just EHS support, the toddlers randomly assigned to Recipe 4 Success were more likely to consume snacks and meals that contained fruits, vegetables, protein, and no sweets or junk food.
As the results of this study and others have shown, early food preferences offer the strongest indication of later diet and healthy eating habits throughout life. The program targeted in this study is significant in its ability to accelerate the adoption of better toddler eating habits in just a 10-week period.
Recipe 4 Success along with other successful preventive interventions for young children are most effective when parents drive the change. “In the present trial, the quality of parenting was most highly related to healthy eating habits and self-regulation at baseline,” the researchers noted.
Specifically, the authors attributed the success of the program to “targeting specific interrelated outcomes with an integrated, theoretically driven intervention model,” which allowed Recipe 4 Success to boost the effectiveness of EHS substantially “in just 10 weeks with a minimal increase in funding,” the authors added.
The authors noted several weaknesses as well as strengths of the study. Its primary weakness was a baseline-posttreatment design, which made it impossible to assert that intervention effects can be sustained. The study was also limited to English-speaking families. Given that most home visitors attended to families in both Recipe 4 Success and EHS, the researchers noted the possibility for contamination across conditions, but they added that this would have actually reduced the intervention effects. The study’s primary strength was the evidenced-based nature of the randomized control. That Recipe 4 Success was operated as an intervention only strengthen the benefits of normal EHS visits.
Patient parents who promote self-regulation have the best chance of success
“This small study emphasizes the importance of parent education and support in setting the toddlers’ palate for lifelong eating habits and self-regulation,” observed Silver Spring, MD, private practice pediatrician and associate clinical professor of pediatrics at George Washington University, Washington, Lillian M. Beard, MD, in a separate interview.
“With the goal of promoting eating habits and self-regulation, I try to guide parents’ choices of what they offer to their toddler. I applaud parents’ patience as I encourage them not to give in and quickly resort to offering salty or sweet snacks. I suggest that if during the course of a day, a palette of colorful healthy choices is offered, most toddlers will graze independently as they go about their play. The challenge is to really support the parent through this quirky stage of their child’s development,” she explained.
“The ultimate challenge today with so much food insecurity, COVID-19 related job losses, and shrinking dollars to feed families is that too many families are feeling a food crisis! A program such as Recipe 4 Success can provide invaluable education for families on how to best stretch their few dollars, with knowledge of which items to seek from their community food pantries, how to best utilize items from the State WIC programs and still seek nutrition tips from their pediatricians while avoiding expensive fast foods that only offer immediate satiety and gratification. The Recipe 4 Success educator, pediatrician, or any community educator can give recommendations about which fresh produce may be inexpensive, but nutritional,” Dr. Beard suggested.
Dr. Nix and colleagues as well as Dr. Beard had no conflicts of interest and no relevant financial disclosures.
Home-based preventive interventions not only improve healthy eating habits and self-regulation in toddlers but also guide their parents toward better food presentation and response to picky behaviors, reported Robert L. Nix, PhD, of the University of Wisconsin, Madison, and his associates.
In a small, randomized controlled trial of 73 families with toddlers aged 18-36 months enrolled in home-based Early Head Start (EHS), the researchers evaluated four protective factors, including toddlers’ healthy eating habits, toddlers’ self-regulation, parents’ responsive feeding practices, and parents’ sensitive scaffolding. The study, conducted from April to October 2013, is the first clinical trial of Recipe 4 Success, a preschool-focused intervention created by administrators and home visitors of EHS that promotes healthy eating and self-regulation in toddlers living in poverty who may otherwise face weight challenges and obesity later in life. Integrating the intervention into EHS allowed the researchers to take full advantage of its national infrastructure and to make dissemination more efficient.
Of the families selected to participate, all of whom were living below the Federal poverty threshold, 66 were retained through post treatment. Most participating parents were biological mothers; 61% were single; 29% were not high school graduates; just 11% were employed full time. The toddlers averaged 30.72 months; 44% were female. Roughly 48% of families were non-Hispanic White; 29% were Black; and 23% were Hispanic or Latinx, the investigators reported in Pediatrics. More than three-quarters of participants were enrolled in the Special Supplemental Nutrition Program for Women, Infants, and Children or the Supplemental Nutrition Assistance Program.
The program allowed parents to transform toddler eating habits quickly
The study, which was designed to evaluate for posttreatment differences in the primary outcomes, involved 10 consecutive weekly lessons implemented by regularly assigned EHS home visitors. Parents were required to adhere to feeding practices carefully targeted with sensitive, structured scaffolding designed to keep toddlers from becoming overwhelmed. Parents were guided to understand, for instance, that toddlers frequently need to be exposed to a new food 10-20 times before eating it, and that poor sleep can have a detrimental influence on emotional and behavioral controls that can progress to weight gain.
Parent recall of what food and drinks their toddlers consumed in the previous 24-hour period was collected by interviewers. The percentage of all meals that included a fruit and/or vegetable, a protein source, and the absence of sweets and junk food were noted. Toddler self-regulation was assessed in accordance with delay of gratification, task orientation, and emotional/behavioral control. Parents were asked to rate toddler ability to cease desired activities to comply with parental requests. Parental responsive feeding practices were also recorded to observe how they introduce unique healthy foods and how they responded to their toddlers’ reactions. Parental sensitive scaffolding was similarly observed for their ability to structure activities in a developmentally appropriate manner promoting self-regulation.
The researchers noted no statistically significant differences between families in the treatment and control groups, nor were there differences in outcome measures or covariates. Study findings showed that, compared with toddlers who continued to receive just EHS support, the toddlers randomly assigned to Recipe 4 Success were more likely to consume snacks and meals that contained fruits, vegetables, protein, and no sweets or junk food.
As the results of this study and others have shown, early food preferences offer the strongest indication of later diet and healthy eating habits throughout life. The program targeted in this study is significant in its ability to accelerate the adoption of better toddler eating habits in just a 10-week period.
Recipe 4 Success along with other successful preventive interventions for young children are most effective when parents drive the change. “In the present trial, the quality of parenting was most highly related to healthy eating habits and self-regulation at baseline,” the researchers noted.
Specifically, the authors attributed the success of the program to “targeting specific interrelated outcomes with an integrated, theoretically driven intervention model,” which allowed Recipe 4 Success to boost the effectiveness of EHS substantially “in just 10 weeks with a minimal increase in funding,” the authors added.
The authors noted several weaknesses as well as strengths of the study. Its primary weakness was a baseline-posttreatment design, which made it impossible to assert that intervention effects can be sustained. The study was also limited to English-speaking families. Given that most home visitors attended to families in both Recipe 4 Success and EHS, the researchers noted the possibility for contamination across conditions, but they added that this would have actually reduced the intervention effects. The study’s primary strength was the evidenced-based nature of the randomized control. That Recipe 4 Success was operated as an intervention only strengthen the benefits of normal EHS visits.
Patient parents who promote self-regulation have the best chance of success
“This small study emphasizes the importance of parent education and support in setting the toddlers’ palate for lifelong eating habits and self-regulation,” observed Silver Spring, MD, private practice pediatrician and associate clinical professor of pediatrics at George Washington University, Washington, Lillian M. Beard, MD, in a separate interview.
“With the goal of promoting eating habits and self-regulation, I try to guide parents’ choices of what they offer to their toddler. I applaud parents’ patience as I encourage them not to give in and quickly resort to offering salty or sweet snacks. I suggest that if during the course of a day, a palette of colorful healthy choices is offered, most toddlers will graze independently as they go about their play. The challenge is to really support the parent through this quirky stage of their child’s development,” she explained.
“The ultimate challenge today with so much food insecurity, COVID-19 related job losses, and shrinking dollars to feed families is that too many families are feeling a food crisis! A program such as Recipe 4 Success can provide invaluable education for families on how to best stretch their few dollars, with knowledge of which items to seek from their community food pantries, how to best utilize items from the State WIC programs and still seek nutrition tips from their pediatricians while avoiding expensive fast foods that only offer immediate satiety and gratification. The Recipe 4 Success educator, pediatrician, or any community educator can give recommendations about which fresh produce may be inexpensive, but nutritional,” Dr. Beard suggested.
Dr. Nix and colleagues as well as Dr. Beard had no conflicts of interest and no relevant financial disclosures.
FROM PEDIATRICS
Age at menarche signals potential cardiovascular health risk
“Increases in age at menarche are significantly associated with increases in cardiovascular health among women,” reported Yi Zheng, MPH, and colleagues at the University of Florida, Gainesville.
Mr. Zheng and colleagues conducted a cross-sectional analysis of 20,447 women aged 18 or older using data from a nationally representative sample of the 1999-2016 National Health and Nutrition Examinations Survey (NHANES). In all, 2,292 (11.2%) were determined to have ideal cardiovascular health (CVH).
Early menarche was confirmed to be related to increases in body mass index and greater incidence of type 2 diabetes, consistent with earlier studies, the authors confirmed. Those with nonideal CVH were more likely to have reported early menarche; those with ideal CVH were not only younger, but they also had college or graduate level education or above and higher poverty income ratio. Those with ideal CVH were also less likely to be to be of non-Hispanic Black heritage or to have been previously married.
BMI may be the missing link between early menarche and CVH
Unlike previous studies, the researchers found no significant link between early menarche and blood pressure, total cholesterol, smoking, physical activity, or diet using fully adjusted model data, leading them to conclude that “the associations between early menarche and CVH might be mainly driven by its associations with BMI.”
Mr. Zheng and colleagues suggested that future studies should evaluate the causal relationships between age at menarche and BMI and whether genetic factors and childhood lifestyle predispose women to early menarche and obesity.
“Our findings further highlighted that age at menarche may be used to identify high-risk population[s] and to guide targeted preventions to maintain and improve CVH,” the authors noted. Although they cited several strengths and limitations of the study, they emphasized that the wide use of Life’s Simple 7 factors (blood pressure, total cholesterol, glucose levels, smoking, BMI, physical activity, and diet) to measure CVH should “only be regarded as a surrogate construct, and future efforts are needed to better characterize CVH,” they cautioned.
The findings offer an opportunity to more closely track CVH in racial and ethnic groups
In a separate editorial, Ewa M. Gross-Sawicka, MD, PhD, and Eiran Z. Gorodeski, MD, MPH, both of the Harrington Heart and Vascular Institute, Cleveland, observed: “That the authors found African American women had the lowest overall CVH scores, even after adjusting for differences, highlights the importance of beginning cardiovascular health education earlier, especially for those in certain racial and ethnic groups.”
Dr. Gross-Sawicka and Dr. Gorodeski also raised several key questions that warrant further research: “1) Why do women who experience late menarche have improved cardiovascular health while those who experience early menarche have reduced cardiovascular health? 2) Why do the ‘beneficial’ effects of late menarche on CVH last 10 years longer than the ‘detrimental’ effects of early menarche? 3) Since both early and late menarche are associated with increased risk of cardiovascular disease, are women who experience menarche at an older age more cognizant of the cardiovascular risks compared with younger women and adjust their CVH accordingly?”
A key point also worth further consideration: “It is unclear whether age at menarche is directly associated with CVH, or if this relationship is mediated by the association of age at menarche and BMI and/or hyperglycemia,” said Dr. Gross-Sawicka and Dr. Gorodeski.
In an interview, Jan Shifren, MD, director, Midlife Women’s Health Center, Massachusetts General Hospital, Boston, noted, “The principal finding is that early menarche is associated with worse cardiovascular health, which may reflect the adverse impact of obesity and glucose intolerance on CVH, as obesity also is a risk factor for early menarche. The association between early menarche and worse CVH was significant only in women aged 25-34 years, but not in older women, possibly as other risk factors become more important as women age. One of the most concerning findings in this study ... is that only 11% had ideal CVH based on a combination of behavioral and health factors. As cardiovascular disease is the leading cause of death for women, we must do a better job of optimizing [their] cardiovascular health. Clinicians need to focus on optimizing cardiovascular health for all of their midlife patients, whether or not they experienced early menarche!”
Mr. Zheng and colleagues, as well as Dr. Shifren and Dr. Grodeski, had no conflicts of interest to report. Dr. Gross-Sawicka has received funding from Abbott and Novartis.
“Increases in age at menarche are significantly associated with increases in cardiovascular health among women,” reported Yi Zheng, MPH, and colleagues at the University of Florida, Gainesville.
Mr. Zheng and colleagues conducted a cross-sectional analysis of 20,447 women aged 18 or older using data from a nationally representative sample of the 1999-2016 National Health and Nutrition Examinations Survey (NHANES). In all, 2,292 (11.2%) were determined to have ideal cardiovascular health (CVH).
Early menarche was confirmed to be related to increases in body mass index and greater incidence of type 2 diabetes, consistent with earlier studies, the authors confirmed. Those with nonideal CVH were more likely to have reported early menarche; those with ideal CVH were not only younger, but they also had college or graduate level education or above and higher poverty income ratio. Those with ideal CVH were also less likely to be to be of non-Hispanic Black heritage or to have been previously married.
BMI may be the missing link between early menarche and CVH
Unlike previous studies, the researchers found no significant link between early menarche and blood pressure, total cholesterol, smoking, physical activity, or diet using fully adjusted model data, leading them to conclude that “the associations between early menarche and CVH might be mainly driven by its associations with BMI.”
Mr. Zheng and colleagues suggested that future studies should evaluate the causal relationships between age at menarche and BMI and whether genetic factors and childhood lifestyle predispose women to early menarche and obesity.
“Our findings further highlighted that age at menarche may be used to identify high-risk population[s] and to guide targeted preventions to maintain and improve CVH,” the authors noted. Although they cited several strengths and limitations of the study, they emphasized that the wide use of Life’s Simple 7 factors (blood pressure, total cholesterol, glucose levels, smoking, BMI, physical activity, and diet) to measure CVH should “only be regarded as a surrogate construct, and future efforts are needed to better characterize CVH,” they cautioned.
The findings offer an opportunity to more closely track CVH in racial and ethnic groups
In a separate editorial, Ewa M. Gross-Sawicka, MD, PhD, and Eiran Z. Gorodeski, MD, MPH, both of the Harrington Heart and Vascular Institute, Cleveland, observed: “That the authors found African American women had the lowest overall CVH scores, even after adjusting for differences, highlights the importance of beginning cardiovascular health education earlier, especially for those in certain racial and ethnic groups.”
Dr. Gross-Sawicka and Dr. Gorodeski also raised several key questions that warrant further research: “1) Why do women who experience late menarche have improved cardiovascular health while those who experience early menarche have reduced cardiovascular health? 2) Why do the ‘beneficial’ effects of late menarche on CVH last 10 years longer than the ‘detrimental’ effects of early menarche? 3) Since both early and late menarche are associated with increased risk of cardiovascular disease, are women who experience menarche at an older age more cognizant of the cardiovascular risks compared with younger women and adjust their CVH accordingly?”
A key point also worth further consideration: “It is unclear whether age at menarche is directly associated with CVH, or if this relationship is mediated by the association of age at menarche and BMI and/or hyperglycemia,” said Dr. Gross-Sawicka and Dr. Gorodeski.
In an interview, Jan Shifren, MD, director, Midlife Women’s Health Center, Massachusetts General Hospital, Boston, noted, “The principal finding is that early menarche is associated with worse cardiovascular health, which may reflect the adverse impact of obesity and glucose intolerance on CVH, as obesity also is a risk factor for early menarche. The association between early menarche and worse CVH was significant only in women aged 25-34 years, but not in older women, possibly as other risk factors become more important as women age. One of the most concerning findings in this study ... is that only 11% had ideal CVH based on a combination of behavioral and health factors. As cardiovascular disease is the leading cause of death for women, we must do a better job of optimizing [their] cardiovascular health. Clinicians need to focus on optimizing cardiovascular health for all of their midlife patients, whether or not they experienced early menarche!”
Mr. Zheng and colleagues, as well as Dr. Shifren and Dr. Grodeski, had no conflicts of interest to report. Dr. Gross-Sawicka has received funding from Abbott and Novartis.
“Increases in age at menarche are significantly associated with increases in cardiovascular health among women,” reported Yi Zheng, MPH, and colleagues at the University of Florida, Gainesville.
Mr. Zheng and colleagues conducted a cross-sectional analysis of 20,447 women aged 18 or older using data from a nationally representative sample of the 1999-2016 National Health and Nutrition Examinations Survey (NHANES). In all, 2,292 (11.2%) were determined to have ideal cardiovascular health (CVH).
Early menarche was confirmed to be related to increases in body mass index and greater incidence of type 2 diabetes, consistent with earlier studies, the authors confirmed. Those with nonideal CVH were more likely to have reported early menarche; those with ideal CVH were not only younger, but they also had college or graduate level education or above and higher poverty income ratio. Those with ideal CVH were also less likely to be to be of non-Hispanic Black heritage or to have been previously married.
BMI may be the missing link between early menarche and CVH
Unlike previous studies, the researchers found no significant link between early menarche and blood pressure, total cholesterol, smoking, physical activity, or diet using fully adjusted model data, leading them to conclude that “the associations between early menarche and CVH might be mainly driven by its associations with BMI.”
Mr. Zheng and colleagues suggested that future studies should evaluate the causal relationships between age at menarche and BMI and whether genetic factors and childhood lifestyle predispose women to early menarche and obesity.
“Our findings further highlighted that age at menarche may be used to identify high-risk population[s] and to guide targeted preventions to maintain and improve CVH,” the authors noted. Although they cited several strengths and limitations of the study, they emphasized that the wide use of Life’s Simple 7 factors (blood pressure, total cholesterol, glucose levels, smoking, BMI, physical activity, and diet) to measure CVH should “only be regarded as a surrogate construct, and future efforts are needed to better characterize CVH,” they cautioned.
The findings offer an opportunity to more closely track CVH in racial and ethnic groups
In a separate editorial, Ewa M. Gross-Sawicka, MD, PhD, and Eiran Z. Gorodeski, MD, MPH, both of the Harrington Heart and Vascular Institute, Cleveland, observed: “That the authors found African American women had the lowest overall CVH scores, even after adjusting for differences, highlights the importance of beginning cardiovascular health education earlier, especially for those in certain racial and ethnic groups.”
Dr. Gross-Sawicka and Dr. Gorodeski also raised several key questions that warrant further research: “1) Why do women who experience late menarche have improved cardiovascular health while those who experience early menarche have reduced cardiovascular health? 2) Why do the ‘beneficial’ effects of late menarche on CVH last 10 years longer than the ‘detrimental’ effects of early menarche? 3) Since both early and late menarche are associated with increased risk of cardiovascular disease, are women who experience menarche at an older age more cognizant of the cardiovascular risks compared with younger women and adjust their CVH accordingly?”
A key point also worth further consideration: “It is unclear whether age at menarche is directly associated with CVH, or if this relationship is mediated by the association of age at menarche and BMI and/or hyperglycemia,” said Dr. Gross-Sawicka and Dr. Gorodeski.
In an interview, Jan Shifren, MD, director, Midlife Women’s Health Center, Massachusetts General Hospital, Boston, noted, “The principal finding is that early menarche is associated with worse cardiovascular health, which may reflect the adverse impact of obesity and glucose intolerance on CVH, as obesity also is a risk factor for early menarche. The association between early menarche and worse CVH was significant only in women aged 25-34 years, but not in older women, possibly as other risk factors become more important as women age. One of the most concerning findings in this study ... is that only 11% had ideal CVH based on a combination of behavioral and health factors. As cardiovascular disease is the leading cause of death for women, we must do a better job of optimizing [their] cardiovascular health. Clinicians need to focus on optimizing cardiovascular health for all of their midlife patients, whether or not they experienced early menarche!”
Mr. Zheng and colleagues, as well as Dr. Shifren and Dr. Grodeski, had no conflicts of interest to report. Dr. Gross-Sawicka has received funding from Abbott and Novartis.
FROM THE JOURNAL OF THE NORTH AMERICAN MENOPAUSE SOCIETY
Consensus bundle has potential to affect postpartum morbidity, mortality
Health care professionals miss an important opportunity if they do not use a holistic patient-centered approach in providing support to their postpartum patients, advised Alison M. Stuebe, MD, MSc, of the division of maternal-fetal medicine at the University of North Carolina at Chapel Hill, and colleagues.
Too often, the emphasis for health care professionals is on less common, highly morbid complications, while their patients’ needs are focused more on daily functioning.
More than half of maternal deaths occur not during delivery, but in the days, weeks, and months following birth. Many serious complications and management of less-emergent conditions such as flu-like symptoms go unnoticed or result in treatment delays. Routinely asking women who present for care whether they have been pregnant during the past year could go a long way in helping clinicians connect the dots for conditions they might not otherwise consider, suggested Dr. Stuebe and colleagues.
In response to what is becoming a growing burden of postpartum maternal morbidity and mortality in the United States, Dr. Stuebe and associates, in coordination with the Alliance of Innovation in Maternal Health, prepared a comprehensive consensus statement on postpartum care basics. The work came out of a day-long planning meeting of an interdisciplinary work group funded by AIMH to develop the maternal safety bundle, which established 28 goals across four phases – readiness, recognition and prevention, response, and reporting. Each phase is intended to occur as part of a coordinated effort between women experiencing pregnancy and their health care providers, with involvement from multiple clinical settings and health systems.
America needs to change the way it treats its new mothers
In a separate interview, Dr. Stuebe shared additional insights into the development of the consensus statement: “This article is part of a broader movement to change the way America treats new mothers. For too long, we’ve lavished attention on women in the weeks before birth and then left them alone to manage recovery, plunging hormones, sleepless nights, and new baby care. The goal of this article is to set out the ways that we can better support women in this critical transition period.
“We need to start during pregnancy, by working with women to plan for the fourth trimester and identify a care team that will support her and her baby. After birth, we need to adapt those plans and make sure she has the emotional and material support she needs to navigate the coming months. Many of these decisions are deeply personal, and we need to center the values and preferences of the woman and her family.”
Dr. Stuebe also spotlighted a new University of North Carolina–based program designed to support shared decision-making. Their Trimester Project team partnered with mothers to design NewMomHealth.com, the first national postpartum resource designed by and for new mothers, which is in the process of launching a culturally adapted Spanish-language site, saludmadre.com, in partnership with Urban Strategies.
Readiness prepares mothers, HCPs, and clinical settings for the fourth trimester
In the first phase, Readiness, there are three key parties involved: the woman experiencing pregnancy, the health care providers (HCPs) supporting her, and the clinical settings involved in her care. Each player has specific goals to achieve in this phase, women are responsible for four goals, health care providers have two goals, and clinical settings have five.
Prenatally, every woman should work with health care providers to develop a comprehensive, individualized postpartum care plan that designates a postpartum clinical “home” for addressing any care needed between birth and the “comprehensive postpartum visit.” The plan encourages the patient and her health care team give attention to social support, birth recovery, infant care and feeding plans, thoughts concerning future pregnancies, and specifically use of contraception, as well as any chronic health concerns and overall emotional well-being.
The plan should consist of a postpartum care team that includes friends and family and ensures that medical, material, and social support are available in the weeks following birth for both mother and baby.
The authors emphasized the importance for clinicians to develop a keen awareness of “reproductive justice,” which respects a woman’s right “to maintain personal bodily autonomy, have children, not have children, and parent the children we have in safe and sustainable communities.” They encouraged adopting a sensitivity to concerns deeply rooted in the history of family planning, which is perceived to have been “fraught by coercive tactics to incentivize sterilization and contraceptive implants among marginalized groups.” With this in mind, they urged clinicians to respectfully ask about the patient’s intentions before making any suggestions concerning future births and family planning preferences.
HCP readiness ensures that each woman “has a documented postpartum care plan and care team identified in the prenatal period.” HCPs are also responsible for developing and maintaining “a working knowledge of evidence-based evaluation and management of common issues facing the mother-infant dyad.”
Clinical setting readiness ensures that woman-centered postpartum care and education have been developed and optimized using adult learning principles whenever possible. Diversity of family structures, cultural traditions, and parenting practices are fully embraced. Dr. Stuebe and colleagues emphasized that traditional top-down teaching methods are ineffective and should be avoided.
Clinical setting readiness also ensures that systems are developed to pair families with community-based resources that provide medical follow-up as well as social and material support. Clinical protocols and reimbursement options should be available that give women easy access to preferred contraception. Systems should be in place that facilitate prompt, pertinent communication between in- and outpatient providers. Lastly, and perhaps most importantly, clinical setting readiness demands the development of protocols to screen and treat key postpartum concerns, such as depression, substance use disorders, family violence, and even incontinence in coordination with locally identified specialists.
Recognition and prevention promotes accountability and establishes key guidelines
Recognition and prevention require coordinated participation between women experiencing pregnancy and the clinical environments supporting their care. In this phase, women are responsible for three goals; clinical environments have four goals.
Women are to be identified and respected as the expert most knowledgeable of their own needs, cautioned the authors. They should also be empowered to trust their instincts, seeking care as early and as often as needed in the weeks after they give birth. Postpartum care needs to be viewed as an ongoing process, not just a singular encounter.
Women also need to take ownership for their postpartum care plan, reviewing and revising it as needed in coordination with their health care providers before maternity discharge is complete. Every plan should include a comprehensive list of warning signs and recommended action plans when faced with life-threatening complications, a list of resources for lactation support, and a “first-call” phone number that identifies the postpartum medical providers available to address breastfeeding issues and for postpartum care visits, including prescheduled dates and times.
Lastly, women are to take responsibility for attending their postpartum visit. Although new guidance suggests that the comprehensive visit take place no later than 12 weeks post partum, it also recognizes multiple visits may be required to address individual needs. All women should have contact with a maternal care provider within 3 weeks post partum, the American College of Obstetricians and Gynecologists recommends.
Responsibility for recognition and prevention in the clinical setting begins with determining guidelines for early postpartum visits, considering chronic conditions such as hypertension, diabetes, or substance abuse disorder and risk for postpartum conditions such as wound complications or postpartum depression, the authors wrote. Ongoing care between inpatient and outpatient settings as well as between maternal and infant care providers is coordinated to ensure health and well-being of both patients. Screening and treatment of common comorbidities such as mental health issues, smoking, and substance use as well as issues related to unstable housing and food insecurities are also addressed in the clinical environment. Lastly, clinicians are tasked with ensuring that every patient has selected a primary care provider for ongoing care.
Response ensures key parties and resources are connected at every step
In the response phase, clinical settings and health care providers are the key participants and they have two goals each.
Every clinical setting is tasked with implementing treatment protocols and providing needed care or facilitating referral in a timely fashion. The importance of a “warm hand-off” and “face-to-face introduction to the specialist to whom the patient is being referred” is encouraged. They are also responsible for keeping an updated inventory of community resources on hand for such unmet needs as 24-hour hotlines, food banks, diaper banks, lactation support groups, and home-visiting programs.
Every health care provider is tasked with developing strategies designed to reach women who do not attend their comprehensive postpartum visit. They are also responsible for assessing the severity of identified needs, and arranging immediate transportation to appropriate facilities in life-threatening circumstances. In nonacute cases, the woman and her care providers work with her to make appropriate decisions.
Reporting gives health systems the opportunity to assess and improve
Sole responsibility in the reporting phase falls to every health system. In this phase, they have a total of six goals.
Health systems are ideally organized to convene strategy-sharing sessions with inpatient as well as outpatient professionals to evaluate successes and opportunities for improvement. They are equally qualified to identify and monitor such quality measures as postpartum emergency department utilization and readmission rates. They are tasked with working toward quality metrics that compare postpartum outcomes and prenatal intentions, including patient receipt of preferred contraception or completion of planned breastfeeding duration.
Health systems are expected to conduct quality improvement measures designed to reduce postpartum morbidity when preventable. They are also the logical choice for maintaining a clearinghouse for resources, in collaboration with the community, that is designed to meet the postpartum needs of women.
Lastly, they play an important role in ensuring that reimbursement policies are structured such that they do not disincentivize postpartum visits.
The consensus bundle encourages change in the way America treats its new mothers
Angela Bianco, MD, maternal and fetal medicine specialist at Mount Sinai Hospital, New York, also interviewed separately, noted: “I think the fact that ACOG has created a postpartum bundle for providers to use for guidance is long overdue. The current prenatal care paradigm focuses on numerous/intensive prenatal visits but only a single postpartum visit. Many women report feeling ill-equipped to navigate the challenges that arise post delivery, including self-care, newborn care, and breastfeeding. In addition, most women experience the impact of dramatic hormonal fluctuations resulting in mood alterations. Add profound sleep deprivation to this and the result is often some degree of postpartum blues and/or depression. The importance of anticipatory guidance for our patients cannot be underestimated. Helping to facilitate potential social support structures be in place prior to the birth is optimal. Providers should reinforce the importance of access to a variety of tools, including digital apps, community support groups, and 24/7 web access services. Moving forward, it should be considered unconscionable to send a new mother home without ensuring the appropriate resources are in place. Postpartum care should be tailored to a woman’s needs and may require multiple visits and/or referrals.”
Dr. Stuebe and colleagues, as well as Dr. Bianco, disclosed receiving honoraria for various projects. Funding for the study was supported by the Alliance for Innovation on Maternal and Child Health, which is funded by a grant from the Health Resources and Services Administration.
Health care professionals miss an important opportunity if they do not use a holistic patient-centered approach in providing support to their postpartum patients, advised Alison M. Stuebe, MD, MSc, of the division of maternal-fetal medicine at the University of North Carolina at Chapel Hill, and colleagues.
Too often, the emphasis for health care professionals is on less common, highly morbid complications, while their patients’ needs are focused more on daily functioning.
More than half of maternal deaths occur not during delivery, but in the days, weeks, and months following birth. Many serious complications and management of less-emergent conditions such as flu-like symptoms go unnoticed or result in treatment delays. Routinely asking women who present for care whether they have been pregnant during the past year could go a long way in helping clinicians connect the dots for conditions they might not otherwise consider, suggested Dr. Stuebe and colleagues.
In response to what is becoming a growing burden of postpartum maternal morbidity and mortality in the United States, Dr. Stuebe and associates, in coordination with the Alliance of Innovation in Maternal Health, prepared a comprehensive consensus statement on postpartum care basics. The work came out of a day-long planning meeting of an interdisciplinary work group funded by AIMH to develop the maternal safety bundle, which established 28 goals across four phases – readiness, recognition and prevention, response, and reporting. Each phase is intended to occur as part of a coordinated effort between women experiencing pregnancy and their health care providers, with involvement from multiple clinical settings and health systems.
America needs to change the way it treats its new mothers
In a separate interview, Dr. Stuebe shared additional insights into the development of the consensus statement: “This article is part of a broader movement to change the way America treats new mothers. For too long, we’ve lavished attention on women in the weeks before birth and then left them alone to manage recovery, plunging hormones, sleepless nights, and new baby care. The goal of this article is to set out the ways that we can better support women in this critical transition period.
“We need to start during pregnancy, by working with women to plan for the fourth trimester and identify a care team that will support her and her baby. After birth, we need to adapt those plans and make sure she has the emotional and material support she needs to navigate the coming months. Many of these decisions are deeply personal, and we need to center the values and preferences of the woman and her family.”
Dr. Stuebe also spotlighted a new University of North Carolina–based program designed to support shared decision-making. Their Trimester Project team partnered with mothers to design NewMomHealth.com, the first national postpartum resource designed by and for new mothers, which is in the process of launching a culturally adapted Spanish-language site, saludmadre.com, in partnership with Urban Strategies.
Readiness prepares mothers, HCPs, and clinical settings for the fourth trimester
In the first phase, Readiness, there are three key parties involved: the woman experiencing pregnancy, the health care providers (HCPs) supporting her, and the clinical settings involved in her care. Each player has specific goals to achieve in this phase, women are responsible for four goals, health care providers have two goals, and clinical settings have five.
Prenatally, every woman should work with health care providers to develop a comprehensive, individualized postpartum care plan that designates a postpartum clinical “home” for addressing any care needed between birth and the “comprehensive postpartum visit.” The plan encourages the patient and her health care team give attention to social support, birth recovery, infant care and feeding plans, thoughts concerning future pregnancies, and specifically use of contraception, as well as any chronic health concerns and overall emotional well-being.
The plan should consist of a postpartum care team that includes friends and family and ensures that medical, material, and social support are available in the weeks following birth for both mother and baby.
The authors emphasized the importance for clinicians to develop a keen awareness of “reproductive justice,” which respects a woman’s right “to maintain personal bodily autonomy, have children, not have children, and parent the children we have in safe and sustainable communities.” They encouraged adopting a sensitivity to concerns deeply rooted in the history of family planning, which is perceived to have been “fraught by coercive tactics to incentivize sterilization and contraceptive implants among marginalized groups.” With this in mind, they urged clinicians to respectfully ask about the patient’s intentions before making any suggestions concerning future births and family planning preferences.
HCP readiness ensures that each woman “has a documented postpartum care plan and care team identified in the prenatal period.” HCPs are also responsible for developing and maintaining “a working knowledge of evidence-based evaluation and management of common issues facing the mother-infant dyad.”
Clinical setting readiness ensures that woman-centered postpartum care and education have been developed and optimized using adult learning principles whenever possible. Diversity of family structures, cultural traditions, and parenting practices are fully embraced. Dr. Stuebe and colleagues emphasized that traditional top-down teaching methods are ineffective and should be avoided.
Clinical setting readiness also ensures that systems are developed to pair families with community-based resources that provide medical follow-up as well as social and material support. Clinical protocols and reimbursement options should be available that give women easy access to preferred contraception. Systems should be in place that facilitate prompt, pertinent communication between in- and outpatient providers. Lastly, and perhaps most importantly, clinical setting readiness demands the development of protocols to screen and treat key postpartum concerns, such as depression, substance use disorders, family violence, and even incontinence in coordination with locally identified specialists.
Recognition and prevention promotes accountability and establishes key guidelines
Recognition and prevention require coordinated participation between women experiencing pregnancy and the clinical environments supporting their care. In this phase, women are responsible for three goals; clinical environments have four goals.
Women are to be identified and respected as the expert most knowledgeable of their own needs, cautioned the authors. They should also be empowered to trust their instincts, seeking care as early and as often as needed in the weeks after they give birth. Postpartum care needs to be viewed as an ongoing process, not just a singular encounter.
Women also need to take ownership for their postpartum care plan, reviewing and revising it as needed in coordination with their health care providers before maternity discharge is complete. Every plan should include a comprehensive list of warning signs and recommended action plans when faced with life-threatening complications, a list of resources for lactation support, and a “first-call” phone number that identifies the postpartum medical providers available to address breastfeeding issues and for postpartum care visits, including prescheduled dates and times.
Lastly, women are to take responsibility for attending their postpartum visit. Although new guidance suggests that the comprehensive visit take place no later than 12 weeks post partum, it also recognizes multiple visits may be required to address individual needs. All women should have contact with a maternal care provider within 3 weeks post partum, the American College of Obstetricians and Gynecologists recommends.
Responsibility for recognition and prevention in the clinical setting begins with determining guidelines for early postpartum visits, considering chronic conditions such as hypertension, diabetes, or substance abuse disorder and risk for postpartum conditions such as wound complications or postpartum depression, the authors wrote. Ongoing care between inpatient and outpatient settings as well as between maternal and infant care providers is coordinated to ensure health and well-being of both patients. Screening and treatment of common comorbidities such as mental health issues, smoking, and substance use as well as issues related to unstable housing and food insecurities are also addressed in the clinical environment. Lastly, clinicians are tasked with ensuring that every patient has selected a primary care provider for ongoing care.
Response ensures key parties and resources are connected at every step
In the response phase, clinical settings and health care providers are the key participants and they have two goals each.
Every clinical setting is tasked with implementing treatment protocols and providing needed care or facilitating referral in a timely fashion. The importance of a “warm hand-off” and “face-to-face introduction to the specialist to whom the patient is being referred” is encouraged. They are also responsible for keeping an updated inventory of community resources on hand for such unmet needs as 24-hour hotlines, food banks, diaper banks, lactation support groups, and home-visiting programs.
Every health care provider is tasked with developing strategies designed to reach women who do not attend their comprehensive postpartum visit. They are also responsible for assessing the severity of identified needs, and arranging immediate transportation to appropriate facilities in life-threatening circumstances. In nonacute cases, the woman and her care providers work with her to make appropriate decisions.
Reporting gives health systems the opportunity to assess and improve
Sole responsibility in the reporting phase falls to every health system. In this phase, they have a total of six goals.
Health systems are ideally organized to convene strategy-sharing sessions with inpatient as well as outpatient professionals to evaluate successes and opportunities for improvement. They are equally qualified to identify and monitor such quality measures as postpartum emergency department utilization and readmission rates. They are tasked with working toward quality metrics that compare postpartum outcomes and prenatal intentions, including patient receipt of preferred contraception or completion of planned breastfeeding duration.
Health systems are expected to conduct quality improvement measures designed to reduce postpartum morbidity when preventable. They are also the logical choice for maintaining a clearinghouse for resources, in collaboration with the community, that is designed to meet the postpartum needs of women.
Lastly, they play an important role in ensuring that reimbursement policies are structured such that they do not disincentivize postpartum visits.
The consensus bundle encourages change in the way America treats its new mothers
Angela Bianco, MD, maternal and fetal medicine specialist at Mount Sinai Hospital, New York, also interviewed separately, noted: “I think the fact that ACOG has created a postpartum bundle for providers to use for guidance is long overdue. The current prenatal care paradigm focuses on numerous/intensive prenatal visits but only a single postpartum visit. Many women report feeling ill-equipped to navigate the challenges that arise post delivery, including self-care, newborn care, and breastfeeding. In addition, most women experience the impact of dramatic hormonal fluctuations resulting in mood alterations. Add profound sleep deprivation to this and the result is often some degree of postpartum blues and/or depression. The importance of anticipatory guidance for our patients cannot be underestimated. Helping to facilitate potential social support structures be in place prior to the birth is optimal. Providers should reinforce the importance of access to a variety of tools, including digital apps, community support groups, and 24/7 web access services. Moving forward, it should be considered unconscionable to send a new mother home without ensuring the appropriate resources are in place. Postpartum care should be tailored to a woman’s needs and may require multiple visits and/or referrals.”
Dr. Stuebe and colleagues, as well as Dr. Bianco, disclosed receiving honoraria for various projects. Funding for the study was supported by the Alliance for Innovation on Maternal and Child Health, which is funded by a grant from the Health Resources and Services Administration.
Health care professionals miss an important opportunity if they do not use a holistic patient-centered approach in providing support to their postpartum patients, advised Alison M. Stuebe, MD, MSc, of the division of maternal-fetal medicine at the University of North Carolina at Chapel Hill, and colleagues.
Too often, the emphasis for health care professionals is on less common, highly morbid complications, while their patients’ needs are focused more on daily functioning.
More than half of maternal deaths occur not during delivery, but in the days, weeks, and months following birth. Many serious complications and management of less-emergent conditions such as flu-like symptoms go unnoticed or result in treatment delays. Routinely asking women who present for care whether they have been pregnant during the past year could go a long way in helping clinicians connect the dots for conditions they might not otherwise consider, suggested Dr. Stuebe and colleagues.
In response to what is becoming a growing burden of postpartum maternal morbidity and mortality in the United States, Dr. Stuebe and associates, in coordination with the Alliance of Innovation in Maternal Health, prepared a comprehensive consensus statement on postpartum care basics. The work came out of a day-long planning meeting of an interdisciplinary work group funded by AIMH to develop the maternal safety bundle, which established 28 goals across four phases – readiness, recognition and prevention, response, and reporting. Each phase is intended to occur as part of a coordinated effort between women experiencing pregnancy and their health care providers, with involvement from multiple clinical settings and health systems.
America needs to change the way it treats its new mothers
In a separate interview, Dr. Stuebe shared additional insights into the development of the consensus statement: “This article is part of a broader movement to change the way America treats new mothers. For too long, we’ve lavished attention on women in the weeks before birth and then left them alone to manage recovery, plunging hormones, sleepless nights, and new baby care. The goal of this article is to set out the ways that we can better support women in this critical transition period.
“We need to start during pregnancy, by working with women to plan for the fourth trimester and identify a care team that will support her and her baby. After birth, we need to adapt those plans and make sure she has the emotional and material support she needs to navigate the coming months. Many of these decisions are deeply personal, and we need to center the values and preferences of the woman and her family.”
Dr. Stuebe also spotlighted a new University of North Carolina–based program designed to support shared decision-making. Their Trimester Project team partnered with mothers to design NewMomHealth.com, the first national postpartum resource designed by and for new mothers, which is in the process of launching a culturally adapted Spanish-language site, saludmadre.com, in partnership with Urban Strategies.
Readiness prepares mothers, HCPs, and clinical settings for the fourth trimester
In the first phase, Readiness, there are three key parties involved: the woman experiencing pregnancy, the health care providers (HCPs) supporting her, and the clinical settings involved in her care. Each player has specific goals to achieve in this phase, women are responsible for four goals, health care providers have two goals, and clinical settings have five.
Prenatally, every woman should work with health care providers to develop a comprehensive, individualized postpartum care plan that designates a postpartum clinical “home” for addressing any care needed between birth and the “comprehensive postpartum visit.” The plan encourages the patient and her health care team give attention to social support, birth recovery, infant care and feeding plans, thoughts concerning future pregnancies, and specifically use of contraception, as well as any chronic health concerns and overall emotional well-being.
The plan should consist of a postpartum care team that includes friends and family and ensures that medical, material, and social support are available in the weeks following birth for both mother and baby.
The authors emphasized the importance for clinicians to develop a keen awareness of “reproductive justice,” which respects a woman’s right “to maintain personal bodily autonomy, have children, not have children, and parent the children we have in safe and sustainable communities.” They encouraged adopting a sensitivity to concerns deeply rooted in the history of family planning, which is perceived to have been “fraught by coercive tactics to incentivize sterilization and contraceptive implants among marginalized groups.” With this in mind, they urged clinicians to respectfully ask about the patient’s intentions before making any suggestions concerning future births and family planning preferences.
HCP readiness ensures that each woman “has a documented postpartum care plan and care team identified in the prenatal period.” HCPs are also responsible for developing and maintaining “a working knowledge of evidence-based evaluation and management of common issues facing the mother-infant dyad.”
Clinical setting readiness ensures that woman-centered postpartum care and education have been developed and optimized using adult learning principles whenever possible. Diversity of family structures, cultural traditions, and parenting practices are fully embraced. Dr. Stuebe and colleagues emphasized that traditional top-down teaching methods are ineffective and should be avoided.
Clinical setting readiness also ensures that systems are developed to pair families with community-based resources that provide medical follow-up as well as social and material support. Clinical protocols and reimbursement options should be available that give women easy access to preferred contraception. Systems should be in place that facilitate prompt, pertinent communication between in- and outpatient providers. Lastly, and perhaps most importantly, clinical setting readiness demands the development of protocols to screen and treat key postpartum concerns, such as depression, substance use disorders, family violence, and even incontinence in coordination with locally identified specialists.
Recognition and prevention promotes accountability and establishes key guidelines
Recognition and prevention require coordinated participation between women experiencing pregnancy and the clinical environments supporting their care. In this phase, women are responsible for three goals; clinical environments have four goals.
Women are to be identified and respected as the expert most knowledgeable of their own needs, cautioned the authors. They should also be empowered to trust their instincts, seeking care as early and as often as needed in the weeks after they give birth. Postpartum care needs to be viewed as an ongoing process, not just a singular encounter.
Women also need to take ownership for their postpartum care plan, reviewing and revising it as needed in coordination with their health care providers before maternity discharge is complete. Every plan should include a comprehensive list of warning signs and recommended action plans when faced with life-threatening complications, a list of resources for lactation support, and a “first-call” phone number that identifies the postpartum medical providers available to address breastfeeding issues and for postpartum care visits, including prescheduled dates and times.
Lastly, women are to take responsibility for attending their postpartum visit. Although new guidance suggests that the comprehensive visit take place no later than 12 weeks post partum, it also recognizes multiple visits may be required to address individual needs. All women should have contact with a maternal care provider within 3 weeks post partum, the American College of Obstetricians and Gynecologists recommends.
Responsibility for recognition and prevention in the clinical setting begins with determining guidelines for early postpartum visits, considering chronic conditions such as hypertension, diabetes, or substance abuse disorder and risk for postpartum conditions such as wound complications or postpartum depression, the authors wrote. Ongoing care between inpatient and outpatient settings as well as between maternal and infant care providers is coordinated to ensure health and well-being of both patients. Screening and treatment of common comorbidities such as mental health issues, smoking, and substance use as well as issues related to unstable housing and food insecurities are also addressed in the clinical environment. Lastly, clinicians are tasked with ensuring that every patient has selected a primary care provider for ongoing care.
Response ensures key parties and resources are connected at every step
In the response phase, clinical settings and health care providers are the key participants and they have two goals each.
Every clinical setting is tasked with implementing treatment protocols and providing needed care or facilitating referral in a timely fashion. The importance of a “warm hand-off” and “face-to-face introduction to the specialist to whom the patient is being referred” is encouraged. They are also responsible for keeping an updated inventory of community resources on hand for such unmet needs as 24-hour hotlines, food banks, diaper banks, lactation support groups, and home-visiting programs.
Every health care provider is tasked with developing strategies designed to reach women who do not attend their comprehensive postpartum visit. They are also responsible for assessing the severity of identified needs, and arranging immediate transportation to appropriate facilities in life-threatening circumstances. In nonacute cases, the woman and her care providers work with her to make appropriate decisions.
Reporting gives health systems the opportunity to assess and improve
Sole responsibility in the reporting phase falls to every health system. In this phase, they have a total of six goals.
Health systems are ideally organized to convene strategy-sharing sessions with inpatient as well as outpatient professionals to evaluate successes and opportunities for improvement. They are equally qualified to identify and monitor such quality measures as postpartum emergency department utilization and readmission rates. They are tasked with working toward quality metrics that compare postpartum outcomes and prenatal intentions, including patient receipt of preferred contraception or completion of planned breastfeeding duration.
Health systems are expected to conduct quality improvement measures designed to reduce postpartum morbidity when preventable. They are also the logical choice for maintaining a clearinghouse for resources, in collaboration with the community, that is designed to meet the postpartum needs of women.
Lastly, they play an important role in ensuring that reimbursement policies are structured such that they do not disincentivize postpartum visits.
The consensus bundle encourages change in the way America treats its new mothers
Angela Bianco, MD, maternal and fetal medicine specialist at Mount Sinai Hospital, New York, also interviewed separately, noted: “I think the fact that ACOG has created a postpartum bundle for providers to use for guidance is long overdue. The current prenatal care paradigm focuses on numerous/intensive prenatal visits but only a single postpartum visit. Many women report feeling ill-equipped to navigate the challenges that arise post delivery, including self-care, newborn care, and breastfeeding. In addition, most women experience the impact of dramatic hormonal fluctuations resulting in mood alterations. Add profound sleep deprivation to this and the result is often some degree of postpartum blues and/or depression. The importance of anticipatory guidance for our patients cannot be underestimated. Helping to facilitate potential social support structures be in place prior to the birth is optimal. Providers should reinforce the importance of access to a variety of tools, including digital apps, community support groups, and 24/7 web access services. Moving forward, it should be considered unconscionable to send a new mother home without ensuring the appropriate resources are in place. Postpartum care should be tailored to a woman’s needs and may require multiple visits and/or referrals.”
Dr. Stuebe and colleagues, as well as Dr. Bianco, disclosed receiving honoraria for various projects. Funding for the study was supported by the Alliance for Innovation on Maternal and Child Health, which is funded by a grant from the Health Resources and Services Administration.
FROM OBSTETRICS AND GYNECOLOGY
Invasive bacterial infections uncommon in afebrile infants with diagnosed AOM
Outpatient management of most afebrile infants with acute otitis media who haven’t been tested for invasive bacterial infection may be reasonable given the low occurrence of adverse events, said Son H. McLaren, MD, MS, of Columbia University, New York, and colleagues.
Dr. McLaren and associates conducted an international cross-sectional study at 33 emergency departments participating in the Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics (AAP): 29 in the United States, 2 in Canada and 2 in Spain.
The researchers sought first to assess prevalence of invasive bacterial infections and adverse events tied to acute otitis media (AOM) in infants 90 days and younger. Those who were clinically diagnosed with AOM and presented without fever between January 2007 and December 2017 were included in the study. The presence of fever, they explained, “is a primary driver for more expanded testing and/or empirical treatment of invasive bacterial infection (IBI). Secondarily, they sought to characterize patterns of diagnostic testing and the factors associated with it specifically in this patient population.
Of 5,270 patients screened, 1,637 met study criteria. Included patients were a median age of 68 days. A total of 1,459 (89.1%) met AAP diagnostic criteria for AOM. The remaining 178 patients were examined and found to have more than one of these criteria: 113 had opacification of tympanic membrane, 57 had dull tympanic membrane, 25 had decreased visualization of middle ear structures, 9 had middle ear effusion, 8 had visible tympanic membrane perforation and 5 had decreased tympanic membrane mobility with insufflation. None of the 278 infants with blood cultures had bacteremia, nor were they diagnosed with bacterial meningitis. Two of 645 (0.3%) infants experienced adverse events, as evidenced with 30-day follow-up or history of hospitalization.
Dr. McLaren and colleagues observed that despite a low prevalence of IBI and AOM-associated adverse events, more than one-fifth of patients were prescribed diagnostic testing for IBI and subsequently hospitalized, a practice that appeared more common with younger patients.
Significant testing and hospitalizations persisted despite low prevalence of IBIs
Although diagnostic testing and hospitalizations differed by site, they were, in fact, “substantial in contrast to the low prevalence of IBIs and adverse events,” the researchers noted. “Our data may be used to help guide clinical management of afebrile infants with clinician-diagnosed AOM, who are not included in the current AAP AOM practice guideline,” the authors said. They speculated that this practice may be due, in part, to young-age risk of IBI and the concern for IBI in this population based on febrile infant population data and a general hesitance to begin antibiotics without first evaluating for IBI. They also cited a low prevalence ranging from 0.8% to 2.5% as evidence for low risk of IBI in afebrile infants with AOM.
Also of note, given that roughly three-fourths of infants included in the study were reported to have symptoms of upper respiratory infection that can lead to viral AOM, including these infants who could have a lower likelihood of IBI than those with known bacterial AOM, may have led the researchers to underestimate IBI prevalence. Because existing data do not allow for clear distinction of viral from bacterial AOM without tympanocentesis, and because more than 85% of older patients with clinically diagnosed AOM also have observed bacterial otopathogens, the authors clarify that “it is understandable why clinicians would manage infants with AOM conservatively, regardless of the presence of concurrent viral illnesses.” They also acknowledged that one major challenge in working with infants believed to have AOM is ensuring that it is actually present since it is so hard to diagnose.
Dr. McLaren and colleagues cited several study limitations: 1) completeness and accuracy of data couldn’t be ensured because of the retrospective study design; 2) because not all infants were tested for IBI, its prevalence may have been underestimated; 3) infants whose discharge codes did not include AOM may have been missed, although all infants with positive blood or cerebrospinal fluid cultures were screened for missed AOM diagnosis; and 4) it is important to consider that any issues associated with testing and hospitalization that were identified may have been the result of management decisions driven by factors that cannot be captured retrospectively or by a diagnosis of AOM.
The findings are not generalizable to infants aged younger than 28 days
Finally, the authors cautioned that because the number of infants younger than 28 days was quite small, and it is therefore infinitely more challenging to diagnose AOM for these patients, results of the study should be applied to infants older than 28 days and are not generalizable to febrile infants.
“This report will not resolve the significant challenge faced by clinicians in treating infants aged [younger than] 28 days who have the highest risk of occult bacteremia and systemic spread of a focal bacterial infection,” Joseph Ravera, MD, and M.W. Stevens, MD, of the University of Vermont, Burlington, noted in an accompanying editorial. Previous studies have identified this age group “to be at the highest risk for systemic bacterial involvement and the most difficult to risk stratify on the basis of physical examination findings and initial laboratory results,” they noted. That the subjects aged younger than 28 days in this study had nearly a 50% admission rate illustrates the clinical uncertainty pediatric emergency medicine providers are challenged with, they added. Just 100 (6%) of the 1,637 patients in the study sample were in this age category, which makes it difficult, given the lack of sufficient data, to generalize findings to the youngest infants.
“Despite a paucity of young infants and limitations inherent to the design, this study does contribute to the literature with a robust retrospective data set of afebrile infants between 1 and 3 months of age with an ED diagnosis of AOM ... It certainly provides a base of support for carefully designed prospective studies in which researchers aim to determine the best care for AOM in children under 6 months of age,” reflected Dr. Ravera and Dr. Stevens.
In a separate interview, Karalyn Kinsella, MD, private practice, Cheshire, Conn. noted, “What is confusing is the absence of documented symptoms for infants presenting to the emergency department, as the symptoms they presented with would influence our concern for IBI. Diagnosing AOM in infants under 90 days old is extremely uncommon as an outpatient pediatrician. Although the finding of AOM in an afebrile infant is very rare in the outpatient setting, this study assures us the risk of IBI is almost nonexistent. Therefore, further workup is unnecessary unless providers have clinical suspicions to the contrary.”
Dr. McLaren and colleagues as well as Dr. Ravera, Dr. Stevens, and Dr. Kinsella, had no conflicts of interest and no relevant financial disclosures.
Outpatient management of most afebrile infants with acute otitis media who haven’t been tested for invasive bacterial infection may be reasonable given the low occurrence of adverse events, said Son H. McLaren, MD, MS, of Columbia University, New York, and colleagues.
Dr. McLaren and associates conducted an international cross-sectional study at 33 emergency departments participating in the Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics (AAP): 29 in the United States, 2 in Canada and 2 in Spain.
The researchers sought first to assess prevalence of invasive bacterial infections and adverse events tied to acute otitis media (AOM) in infants 90 days and younger. Those who were clinically diagnosed with AOM and presented without fever between January 2007 and December 2017 were included in the study. The presence of fever, they explained, “is a primary driver for more expanded testing and/or empirical treatment of invasive bacterial infection (IBI). Secondarily, they sought to characterize patterns of diagnostic testing and the factors associated with it specifically in this patient population.
Of 5,270 patients screened, 1,637 met study criteria. Included patients were a median age of 68 days. A total of 1,459 (89.1%) met AAP diagnostic criteria for AOM. The remaining 178 patients were examined and found to have more than one of these criteria: 113 had opacification of tympanic membrane, 57 had dull tympanic membrane, 25 had decreased visualization of middle ear structures, 9 had middle ear effusion, 8 had visible tympanic membrane perforation and 5 had decreased tympanic membrane mobility with insufflation. None of the 278 infants with blood cultures had bacteremia, nor were they diagnosed with bacterial meningitis. Two of 645 (0.3%) infants experienced adverse events, as evidenced with 30-day follow-up or history of hospitalization.
Dr. McLaren and colleagues observed that despite a low prevalence of IBI and AOM-associated adverse events, more than one-fifth of patients were prescribed diagnostic testing for IBI and subsequently hospitalized, a practice that appeared more common with younger patients.
Significant testing and hospitalizations persisted despite low prevalence of IBIs
Although diagnostic testing and hospitalizations differed by site, they were, in fact, “substantial in contrast to the low prevalence of IBIs and adverse events,” the researchers noted. “Our data may be used to help guide clinical management of afebrile infants with clinician-diagnosed AOM, who are not included in the current AAP AOM practice guideline,” the authors said. They speculated that this practice may be due, in part, to young-age risk of IBI and the concern for IBI in this population based on febrile infant population data and a general hesitance to begin antibiotics without first evaluating for IBI. They also cited a low prevalence ranging from 0.8% to 2.5% as evidence for low risk of IBI in afebrile infants with AOM.
Also of note, given that roughly three-fourths of infants included in the study were reported to have symptoms of upper respiratory infection that can lead to viral AOM, including these infants who could have a lower likelihood of IBI than those with known bacterial AOM, may have led the researchers to underestimate IBI prevalence. Because existing data do not allow for clear distinction of viral from bacterial AOM without tympanocentesis, and because more than 85% of older patients with clinically diagnosed AOM also have observed bacterial otopathogens, the authors clarify that “it is understandable why clinicians would manage infants with AOM conservatively, regardless of the presence of concurrent viral illnesses.” They also acknowledged that one major challenge in working with infants believed to have AOM is ensuring that it is actually present since it is so hard to diagnose.
Dr. McLaren and colleagues cited several study limitations: 1) completeness and accuracy of data couldn’t be ensured because of the retrospective study design; 2) because not all infants were tested for IBI, its prevalence may have been underestimated; 3) infants whose discharge codes did not include AOM may have been missed, although all infants with positive blood or cerebrospinal fluid cultures were screened for missed AOM diagnosis; and 4) it is important to consider that any issues associated with testing and hospitalization that were identified may have been the result of management decisions driven by factors that cannot be captured retrospectively or by a diagnosis of AOM.
The findings are not generalizable to infants aged younger than 28 days
Finally, the authors cautioned that because the number of infants younger than 28 days was quite small, and it is therefore infinitely more challenging to diagnose AOM for these patients, results of the study should be applied to infants older than 28 days and are not generalizable to febrile infants.
“This report will not resolve the significant challenge faced by clinicians in treating infants aged [younger than] 28 days who have the highest risk of occult bacteremia and systemic spread of a focal bacterial infection,” Joseph Ravera, MD, and M.W. Stevens, MD, of the University of Vermont, Burlington, noted in an accompanying editorial. Previous studies have identified this age group “to be at the highest risk for systemic bacterial involvement and the most difficult to risk stratify on the basis of physical examination findings and initial laboratory results,” they noted. That the subjects aged younger than 28 days in this study had nearly a 50% admission rate illustrates the clinical uncertainty pediatric emergency medicine providers are challenged with, they added. Just 100 (6%) of the 1,637 patients in the study sample were in this age category, which makes it difficult, given the lack of sufficient data, to generalize findings to the youngest infants.
“Despite a paucity of young infants and limitations inherent to the design, this study does contribute to the literature with a robust retrospective data set of afebrile infants between 1 and 3 months of age with an ED diagnosis of AOM ... It certainly provides a base of support for carefully designed prospective studies in which researchers aim to determine the best care for AOM in children under 6 months of age,” reflected Dr. Ravera and Dr. Stevens.
In a separate interview, Karalyn Kinsella, MD, private practice, Cheshire, Conn. noted, “What is confusing is the absence of documented symptoms for infants presenting to the emergency department, as the symptoms they presented with would influence our concern for IBI. Diagnosing AOM in infants under 90 days old is extremely uncommon as an outpatient pediatrician. Although the finding of AOM in an afebrile infant is very rare in the outpatient setting, this study assures us the risk of IBI is almost nonexistent. Therefore, further workup is unnecessary unless providers have clinical suspicions to the contrary.”
Dr. McLaren and colleagues as well as Dr. Ravera, Dr. Stevens, and Dr. Kinsella, had no conflicts of interest and no relevant financial disclosures.
Outpatient management of most afebrile infants with acute otitis media who haven’t been tested for invasive bacterial infection may be reasonable given the low occurrence of adverse events, said Son H. McLaren, MD, MS, of Columbia University, New York, and colleagues.
Dr. McLaren and associates conducted an international cross-sectional study at 33 emergency departments participating in the Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics (AAP): 29 in the United States, 2 in Canada and 2 in Spain.
The researchers sought first to assess prevalence of invasive bacterial infections and adverse events tied to acute otitis media (AOM) in infants 90 days and younger. Those who were clinically diagnosed with AOM and presented without fever between January 2007 and December 2017 were included in the study. The presence of fever, they explained, “is a primary driver for more expanded testing and/or empirical treatment of invasive bacterial infection (IBI). Secondarily, they sought to characterize patterns of diagnostic testing and the factors associated with it specifically in this patient population.
Of 5,270 patients screened, 1,637 met study criteria. Included patients were a median age of 68 days. A total of 1,459 (89.1%) met AAP diagnostic criteria for AOM. The remaining 178 patients were examined and found to have more than one of these criteria: 113 had opacification of tympanic membrane, 57 had dull tympanic membrane, 25 had decreased visualization of middle ear structures, 9 had middle ear effusion, 8 had visible tympanic membrane perforation and 5 had decreased tympanic membrane mobility with insufflation. None of the 278 infants with blood cultures had bacteremia, nor were they diagnosed with bacterial meningitis. Two of 645 (0.3%) infants experienced adverse events, as evidenced with 30-day follow-up or history of hospitalization.
Dr. McLaren and colleagues observed that despite a low prevalence of IBI and AOM-associated adverse events, more than one-fifth of patients were prescribed diagnostic testing for IBI and subsequently hospitalized, a practice that appeared more common with younger patients.
Significant testing and hospitalizations persisted despite low prevalence of IBIs
Although diagnostic testing and hospitalizations differed by site, they were, in fact, “substantial in contrast to the low prevalence of IBIs and adverse events,” the researchers noted. “Our data may be used to help guide clinical management of afebrile infants with clinician-diagnosed AOM, who are not included in the current AAP AOM practice guideline,” the authors said. They speculated that this practice may be due, in part, to young-age risk of IBI and the concern for IBI in this population based on febrile infant population data and a general hesitance to begin antibiotics without first evaluating for IBI. They also cited a low prevalence ranging from 0.8% to 2.5% as evidence for low risk of IBI in afebrile infants with AOM.
Also of note, given that roughly three-fourths of infants included in the study were reported to have symptoms of upper respiratory infection that can lead to viral AOM, including these infants who could have a lower likelihood of IBI than those with known bacterial AOM, may have led the researchers to underestimate IBI prevalence. Because existing data do not allow for clear distinction of viral from bacterial AOM without tympanocentesis, and because more than 85% of older patients with clinically diagnosed AOM also have observed bacterial otopathogens, the authors clarify that “it is understandable why clinicians would manage infants with AOM conservatively, regardless of the presence of concurrent viral illnesses.” They also acknowledged that one major challenge in working with infants believed to have AOM is ensuring that it is actually present since it is so hard to diagnose.
Dr. McLaren and colleagues cited several study limitations: 1) completeness and accuracy of data couldn’t be ensured because of the retrospective study design; 2) because not all infants were tested for IBI, its prevalence may have been underestimated; 3) infants whose discharge codes did not include AOM may have been missed, although all infants with positive blood or cerebrospinal fluid cultures were screened for missed AOM diagnosis; and 4) it is important to consider that any issues associated with testing and hospitalization that were identified may have been the result of management decisions driven by factors that cannot be captured retrospectively or by a diagnosis of AOM.
The findings are not generalizable to infants aged younger than 28 days
Finally, the authors cautioned that because the number of infants younger than 28 days was quite small, and it is therefore infinitely more challenging to diagnose AOM for these patients, results of the study should be applied to infants older than 28 days and are not generalizable to febrile infants.
“This report will not resolve the significant challenge faced by clinicians in treating infants aged [younger than] 28 days who have the highest risk of occult bacteremia and systemic spread of a focal bacterial infection,” Joseph Ravera, MD, and M.W. Stevens, MD, of the University of Vermont, Burlington, noted in an accompanying editorial. Previous studies have identified this age group “to be at the highest risk for systemic bacterial involvement and the most difficult to risk stratify on the basis of physical examination findings and initial laboratory results,” they noted. That the subjects aged younger than 28 days in this study had nearly a 50% admission rate illustrates the clinical uncertainty pediatric emergency medicine providers are challenged with, they added. Just 100 (6%) of the 1,637 patients in the study sample were in this age category, which makes it difficult, given the lack of sufficient data, to generalize findings to the youngest infants.
“Despite a paucity of young infants and limitations inherent to the design, this study does contribute to the literature with a robust retrospective data set of afebrile infants between 1 and 3 months of age with an ED diagnosis of AOM ... It certainly provides a base of support for carefully designed prospective studies in which researchers aim to determine the best care for AOM in children under 6 months of age,” reflected Dr. Ravera and Dr. Stevens.
In a separate interview, Karalyn Kinsella, MD, private practice, Cheshire, Conn. noted, “What is confusing is the absence of documented symptoms for infants presenting to the emergency department, as the symptoms they presented with would influence our concern for IBI. Diagnosing AOM in infants under 90 days old is extremely uncommon as an outpatient pediatrician. Although the finding of AOM in an afebrile infant is very rare in the outpatient setting, this study assures us the risk of IBI is almost nonexistent. Therefore, further workup is unnecessary unless providers have clinical suspicions to the contrary.”
Dr. McLaren and colleagues as well as Dr. Ravera, Dr. Stevens, and Dr. Kinsella, had no conflicts of interest and no relevant financial disclosures.
FROM PEDIATRICS