User login
FDA clears portable hematology analyzer
The U.S. Food and Drug Administration (FDA) has granted 510(k) clearance for PixCell Medical’s HemoScreen™.
This portable hematology analyzer is used to perform a complete blood count at the point of care.
HemoScreen requires a single drop of blood and uses disposable cartridges that provide automatic sample preparation.
HemoScreen can analyze 20 standard complete blood count parameters and produces results within 5 minutes.
Study results suggested that HemoScreen provides results comparable to those of another hematology analyzer, Sysmex XE-2100. This study was published in the Journal of Clinical Pathology in 2016.
“The HemoScreen delivers lab-accurate results,” said Avishay Bransky, PhD, chief executive officer of PixCell Medical.
He added that HemoScreen “would be especially useful” in physicians’ offices, emergency rooms, intensive care units, oncology clinics, and remote locations.
HemoScreen makes use of a technology called viscoelastic focusing, which employs microfluidics and machine vision algorithms to analyze cells.
The U.S. Food and Drug Administration (FDA) has granted 510(k) clearance for PixCell Medical’s HemoScreen™.
This portable hematology analyzer is used to perform a complete blood count at the point of care.
HemoScreen requires a single drop of blood and uses disposable cartridges that provide automatic sample preparation.
HemoScreen can analyze 20 standard complete blood count parameters and produces results within 5 minutes.
Study results suggested that HemoScreen provides results comparable to those of another hematology analyzer, Sysmex XE-2100. This study was published in the Journal of Clinical Pathology in 2016.
“The HemoScreen delivers lab-accurate results,” said Avishay Bransky, PhD, chief executive officer of PixCell Medical.
He added that HemoScreen “would be especially useful” in physicians’ offices, emergency rooms, intensive care units, oncology clinics, and remote locations.
HemoScreen makes use of a technology called viscoelastic focusing, which employs microfluidics and machine vision algorithms to analyze cells.
The U.S. Food and Drug Administration (FDA) has granted 510(k) clearance for PixCell Medical’s HemoScreen™.
This portable hematology analyzer is used to perform a complete blood count at the point of care.
HemoScreen requires a single drop of blood and uses disposable cartridges that provide automatic sample preparation.
HemoScreen can analyze 20 standard complete blood count parameters and produces results within 5 minutes.
Study results suggested that HemoScreen provides results comparable to those of another hematology analyzer, Sysmex XE-2100. This study was published in the Journal of Clinical Pathology in 2016.
“The HemoScreen delivers lab-accurate results,” said Avishay Bransky, PhD, chief executive officer of PixCell Medical.
He added that HemoScreen “would be especially useful” in physicians’ offices, emergency rooms, intensive care units, oncology clinics, and remote locations.
HemoScreen makes use of a technology called viscoelastic focusing, which employs microfluidics and machine vision algorithms to analyze cells.
Selinexor on fast track for DLBCL
The U.S. Food and Drug Administration (FDA) has granted fast track designation to selinexor for the treatment of diffuse large B-cell lymphoma (DLBCL).
The designation is for selinexor to treat DLBCL patients who have received at least two prior therapies and are not eligible for high-dose chemotherapy with stem cell rescue or chimeric antigen receptor T-cell therapy.
Selinexor is being studied in the phase 2b SADAL trial (NCT02227251), which is enrolling patients with relapsed or refractory DLBCL who have received two to five prior therapies and are not eligible for stem cell transplant.
Top-line results from this trial are scheduled to be presented at the 2018 ASH Annual Meeting (abstract 1677).
Selinexor is an oral selective inhibitor of nuclear export (SINE) compound being developed by Karyopharm Therapeutics Inc.
The company previously received fast track designation for selinexor to treat patients with penta-refractory multiple myeloma who have received at least three prior lines of therapy.
The FDA says its fast track program is designed to facilitate the development and expedite the review of products that are intended to treat serious conditions and have the potential to address unmet medical needs.
Fast track designation provides developers with greater access to the FDA as well as eligibility for accelerated approval, priority review, and rolling review.
“The receipt of fast track designation from the FDA for selinexor in relapsed DLBCL underscores the great unmet medical need for this aggressive form of lymphoma,” said Sharon Shacham, PhD, founder, president, and chief scientific officer of Karyopharm.
“Pending positive results from the phase 2b SADAL study, we plan to submit a second NDA [new drug application] to the FDA in the first half of 2019, with a request for accelerated approval, for oral selinexor as a potential new treatment for patients with relapsed or refractory DLBCL.”
Last month, the FDA accepted a new drug application for selinexor as a treatment for penta-refractory multiple myeloma. The agency granted the application priority review and set an action date of April 6, 2019.
The U.S. Food and Drug Administration (FDA) has granted fast track designation to selinexor for the treatment of diffuse large B-cell lymphoma (DLBCL).
The designation is for selinexor to treat DLBCL patients who have received at least two prior therapies and are not eligible for high-dose chemotherapy with stem cell rescue or chimeric antigen receptor T-cell therapy.
Selinexor is being studied in the phase 2b SADAL trial (NCT02227251), which is enrolling patients with relapsed or refractory DLBCL who have received two to five prior therapies and are not eligible for stem cell transplant.
Top-line results from this trial are scheduled to be presented at the 2018 ASH Annual Meeting (abstract 1677).
Selinexor is an oral selective inhibitor of nuclear export (SINE) compound being developed by Karyopharm Therapeutics Inc.
The company previously received fast track designation for selinexor to treat patients with penta-refractory multiple myeloma who have received at least three prior lines of therapy.
The FDA says its fast track program is designed to facilitate the development and expedite the review of products that are intended to treat serious conditions and have the potential to address unmet medical needs.
Fast track designation provides developers with greater access to the FDA as well as eligibility for accelerated approval, priority review, and rolling review.
“The receipt of fast track designation from the FDA for selinexor in relapsed DLBCL underscores the great unmet medical need for this aggressive form of lymphoma,” said Sharon Shacham, PhD, founder, president, and chief scientific officer of Karyopharm.
“Pending positive results from the phase 2b SADAL study, we plan to submit a second NDA [new drug application] to the FDA in the first half of 2019, with a request for accelerated approval, for oral selinexor as a potential new treatment for patients with relapsed or refractory DLBCL.”
Last month, the FDA accepted a new drug application for selinexor as a treatment for penta-refractory multiple myeloma. The agency granted the application priority review and set an action date of April 6, 2019.
The U.S. Food and Drug Administration (FDA) has granted fast track designation to selinexor for the treatment of diffuse large B-cell lymphoma (DLBCL).
The designation is for selinexor to treat DLBCL patients who have received at least two prior therapies and are not eligible for high-dose chemotherapy with stem cell rescue or chimeric antigen receptor T-cell therapy.
Selinexor is being studied in the phase 2b SADAL trial (NCT02227251), which is enrolling patients with relapsed or refractory DLBCL who have received two to five prior therapies and are not eligible for stem cell transplant.
Top-line results from this trial are scheduled to be presented at the 2018 ASH Annual Meeting (abstract 1677).
Selinexor is an oral selective inhibitor of nuclear export (SINE) compound being developed by Karyopharm Therapeutics Inc.
The company previously received fast track designation for selinexor to treat patients with penta-refractory multiple myeloma who have received at least three prior lines of therapy.
The FDA says its fast track program is designed to facilitate the development and expedite the review of products that are intended to treat serious conditions and have the potential to address unmet medical needs.
Fast track designation provides developers with greater access to the FDA as well as eligibility for accelerated approval, priority review, and rolling review.
“The receipt of fast track designation from the FDA for selinexor in relapsed DLBCL underscores the great unmet medical need for this aggressive form of lymphoma,” said Sharon Shacham, PhD, founder, president, and chief scientific officer of Karyopharm.
“Pending positive results from the phase 2b SADAL study, we plan to submit a second NDA [new drug application] to the FDA in the first half of 2019, with a request for accelerated approval, for oral selinexor as a potential new treatment for patients with relapsed or refractory DLBCL.”
Last month, the FDA accepted a new drug application for selinexor as a treatment for penta-refractory multiple myeloma. The agency granted the application priority review and set an action date of April 6, 2019.
Quizartinib receives accelerated assessment for AML
The European Medicines Agency has granted accelerated assessment to the marketing authorization application (MAA) for the FLT3 inhibitor quizartinib.
With this MAA, Daiichi Sankyo Company, Ltd., is seeking authorization for quizartinib to treat adults with FLT3-ITD-positive, relapsed or refractory acute myeloid leukemia (AML).
Accelerated assessment is given to products expected to be of major interest for public health and therapeutic innovation, and it can reduce the review timeline from 210 days to 150 days.
Quizartinib also has orphan drug designation from the European Commission.
The MAA for quizartinib is based on the phase 3 QuANTUM-R study. Results from this trial were presented at the 23rd Congress of the European Hematology Association in June.
QuANTUM-R enrolled adults with FLT3-ITD AML (at least 3% FLT3-ITD allelic ratio) who had refractory disease or had relapsed within 6 months of their first complete response (CR).
Patients were randomized to receive once-daily treatment with quizartinib (n=245) or a salvage chemotherapy regimen (n=122)—low-dose cytarabine (LoDAC, n=29); combination mitoxantrone, etoposide, and cytarabine (MEC, n=40); or combination fludarabine, cytarabine, and idarubicin (FLAG-IDA, n=53).
Patients who responded to treatment could proceed to hematopoietic stem cell transplant (HSCT), and those in the quizartinib arm could resume quizartinib after HSCT.
In all, 241 patients received quizartinib, and 94 received salvage chemotherapy—LoDAC (n=22), MEC (n=25), and FLAG-IDA (n=47). Of the 28 patients in the chemotherapy group who were not treated, most withdrew consent.
Thirty-two percent of quizartinib-treated patients and 12% of the chemotherapy group went on to HSCT.
Efficacy
The median follow-up was 23.5 months. The efficacy results include all randomized patients.
The overall response rate was 69% in the quizartinib arm and 30% in the chemotherapy arm.
The composite CR rate was 48% in the quizartinib arm and 27% in the chemotherapy arm. This includes:
- The CR rate (4% and 1%, respectively)
- The rate of CR with incomplete platelet recovery (4% and 0%, respectively)
- The rate of CR with incomplete hematologic recovery (40% and 26%, respectively).
The median event-free survival was 6.0 weeks in the quizartinib arm and 3.7 weeks in the chemotherapy arm (hazard ratio=0.90, P=0.1071).
The median overall survival was 6.2 months in the quizartinib arm and 4.7 months in the chemotherapy arm (hazard ratio=0.76, P=0.0177). The 1-year overall survival rate was 27% and 20%, respectively.
Safety
The safety results include only patients who received their assigned treatment.
Grade 3 or higher hematologic treatment-emergent adverse events occurring in at least 5% of patients (in the quizartinib and chemotherapy groups, respectively) included:
- Thrombocytopenia (35% and 34%)
- Anemia (30% and 29%)
- Neutropenia (32% and 25%)
- Febrile neutropenia (31% and 21%)
- Leukopenia (17% and 16%).
Grade 3 or higher non-hematologic treatment-emergent adverse events occurring in at least 5% of patients (in the quizartinib and chemotherapy groups, respectively) included:
- Sepsis/septic shock (16% and 18%)
- Hypokalemia (12% and 9%)
- Pneumonia (12% and 9%)
- Fatigue (8% and 1%)
- Dyspnea (5% for both)
- Hypophosphatemia (5% for both).
The European Medicines Agency has granted accelerated assessment to the marketing authorization application (MAA) for the FLT3 inhibitor quizartinib.
With this MAA, Daiichi Sankyo Company, Ltd., is seeking authorization for quizartinib to treat adults with FLT3-ITD-positive, relapsed or refractory acute myeloid leukemia (AML).
Accelerated assessment is given to products expected to be of major interest for public health and therapeutic innovation, and it can reduce the review timeline from 210 days to 150 days.
Quizartinib also has orphan drug designation from the European Commission.
The MAA for quizartinib is based on the phase 3 QuANTUM-R study. Results from this trial were presented at the 23rd Congress of the European Hematology Association in June.
QuANTUM-R enrolled adults with FLT3-ITD AML (at least 3% FLT3-ITD allelic ratio) who had refractory disease or had relapsed within 6 months of their first complete response (CR).
Patients were randomized to receive once-daily treatment with quizartinib (n=245) or a salvage chemotherapy regimen (n=122)—low-dose cytarabine (LoDAC, n=29); combination mitoxantrone, etoposide, and cytarabine (MEC, n=40); or combination fludarabine, cytarabine, and idarubicin (FLAG-IDA, n=53).
Patients who responded to treatment could proceed to hematopoietic stem cell transplant (HSCT), and those in the quizartinib arm could resume quizartinib after HSCT.
In all, 241 patients received quizartinib, and 94 received salvage chemotherapy—LoDAC (n=22), MEC (n=25), and FLAG-IDA (n=47). Of the 28 patients in the chemotherapy group who were not treated, most withdrew consent.
Thirty-two percent of quizartinib-treated patients and 12% of the chemotherapy group went on to HSCT.
Efficacy
The median follow-up was 23.5 months. The efficacy results include all randomized patients.
The overall response rate was 69% in the quizartinib arm and 30% in the chemotherapy arm.
The composite CR rate was 48% in the quizartinib arm and 27% in the chemotherapy arm. This includes:
- The CR rate (4% and 1%, respectively)
- The rate of CR with incomplete platelet recovery (4% and 0%, respectively)
- The rate of CR with incomplete hematologic recovery (40% and 26%, respectively).
The median event-free survival was 6.0 weeks in the quizartinib arm and 3.7 weeks in the chemotherapy arm (hazard ratio=0.90, P=0.1071).
The median overall survival was 6.2 months in the quizartinib arm and 4.7 months in the chemotherapy arm (hazard ratio=0.76, P=0.0177). The 1-year overall survival rate was 27% and 20%, respectively.
Safety
The safety results include only patients who received their assigned treatment.
Grade 3 or higher hematologic treatment-emergent adverse events occurring in at least 5% of patients (in the quizartinib and chemotherapy groups, respectively) included:
- Thrombocytopenia (35% and 34%)
- Anemia (30% and 29%)
- Neutropenia (32% and 25%)
- Febrile neutropenia (31% and 21%)
- Leukopenia (17% and 16%).
Grade 3 or higher non-hematologic treatment-emergent adverse events occurring in at least 5% of patients (in the quizartinib and chemotherapy groups, respectively) included:
- Sepsis/septic shock (16% and 18%)
- Hypokalemia (12% and 9%)
- Pneumonia (12% and 9%)
- Fatigue (8% and 1%)
- Dyspnea (5% for both)
- Hypophosphatemia (5% for both).
The European Medicines Agency has granted accelerated assessment to the marketing authorization application (MAA) for the FLT3 inhibitor quizartinib.
With this MAA, Daiichi Sankyo Company, Ltd., is seeking authorization for quizartinib to treat adults with FLT3-ITD-positive, relapsed or refractory acute myeloid leukemia (AML).
Accelerated assessment is given to products expected to be of major interest for public health and therapeutic innovation, and it can reduce the review timeline from 210 days to 150 days.
Quizartinib also has orphan drug designation from the European Commission.
The MAA for quizartinib is based on the phase 3 QuANTUM-R study. Results from this trial were presented at the 23rd Congress of the European Hematology Association in June.
QuANTUM-R enrolled adults with FLT3-ITD AML (at least 3% FLT3-ITD allelic ratio) who had refractory disease or had relapsed within 6 months of their first complete response (CR).
Patients were randomized to receive once-daily treatment with quizartinib (n=245) or a salvage chemotherapy regimen (n=122)—low-dose cytarabine (LoDAC, n=29); combination mitoxantrone, etoposide, and cytarabine (MEC, n=40); or combination fludarabine, cytarabine, and idarubicin (FLAG-IDA, n=53).
Patients who responded to treatment could proceed to hematopoietic stem cell transplant (HSCT), and those in the quizartinib arm could resume quizartinib after HSCT.
In all, 241 patients received quizartinib, and 94 received salvage chemotherapy—LoDAC (n=22), MEC (n=25), and FLAG-IDA (n=47). Of the 28 patients in the chemotherapy group who were not treated, most withdrew consent.
Thirty-two percent of quizartinib-treated patients and 12% of the chemotherapy group went on to HSCT.
Efficacy
The median follow-up was 23.5 months. The efficacy results include all randomized patients.
The overall response rate was 69% in the quizartinib arm and 30% in the chemotherapy arm.
The composite CR rate was 48% in the quizartinib arm and 27% in the chemotherapy arm. This includes:
- The CR rate (4% and 1%, respectively)
- The rate of CR with incomplete platelet recovery (4% and 0%, respectively)
- The rate of CR with incomplete hematologic recovery (40% and 26%, respectively).
The median event-free survival was 6.0 weeks in the quizartinib arm and 3.7 weeks in the chemotherapy arm (hazard ratio=0.90, P=0.1071).
The median overall survival was 6.2 months in the quizartinib arm and 4.7 months in the chemotherapy arm (hazard ratio=0.76, P=0.0177). The 1-year overall survival rate was 27% and 20%, respectively.
Safety
The safety results include only patients who received their assigned treatment.
Grade 3 or higher hematologic treatment-emergent adverse events occurring in at least 5% of patients (in the quizartinib and chemotherapy groups, respectively) included:
- Thrombocytopenia (35% and 34%)
- Anemia (30% and 29%)
- Neutropenia (32% and 25%)
- Febrile neutropenia (31% and 21%)
- Leukopenia (17% and 16%).
Grade 3 or higher non-hematologic treatment-emergent adverse events occurring in at least 5% of patients (in the quizartinib and chemotherapy groups, respectively) included:
- Sepsis/septic shock (16% and 18%)
- Hypokalemia (12% and 9%)
- Pneumonia (12% and 9%)
- Fatigue (8% and 1%)
- Dyspnea (5% for both)
- Hypophosphatemia (5% for both).
Sandoz won’t seek U.S. approval for rituximab biosimilar
Sandoz has decided not to pursue U.S. approval for its rituximab product (GP2013), a proposed biosimiliar of Rituxan/Mabthera.
GP2013 (Rixathon, Riximyo) is already approved outside the U.S.
Sandoz was seeking U.S. approval of GP2013 for all the same indications as the reference product—B-cell non-Hodgkin lymphoma, chronic lymphocytic leukemia, rheumatoid arthritis, granulomatosis with polyangiitis, microscopic polyangiitis, and pemphigus vulgaris.
The U.S. Food and Drug Administration (FDA) had accepted the biologics license application (BLA) for GP2013 in September 2017.
In May of this year, the FDA issued a complete response letter saying it could not approve GP2013. The agency also requested additional information to complement the BLA submission for GP2013.
At the time of the complete response letter, Sandoz said it was still committed to bringing GP2013 to the U.S. market. Now, the company’s position has changed.
“We appreciate the important conversations with the FDA, which have provided specific requirements for our potential U.S. biosimilar rituximab, but believe the patient and marketplace needs in the U.S. will be satisfied before we can generate the data required,” said Stefan Hendriks, global head of biopharmaceuticals at Sandoz.
“We are disappointed to have to make this decision and stand behind the safety, efficacy, and quality of our medicine, which met the stringent criteria for approval in the European Union, Switzerland, Japan, New Zealand, and Australia.”
The BLA for GP2013 was supported, in part, by the ASSIST-FL trial (NCT01419665), in which researchers compared GP2013 to the reference product. Results from this trial were published in The Lancet Haematology in July 2017.
The phase 3 trial included adults with previously untreated, advanced stage follicular lymphoma. Patients received 8 cycles of cyclophosphamide, vincristine, and prednisone with either GP2013 or reference rituximab. Responders then received GP2013 or rituximab monotherapy as maintenance for up to 2 years.
At a median follow-up of 11.6 months, the overall response rate was 87% (271/311) in the GP2013 arm and 88% in the rituximab arm (274/313). Complete response rates were 15% (n=46) and 13% (n=42), respectively.
Rates of adverse events (AEs) were 93% in the GP2013 arm and 91% in the rituximab arm. Rates of serious AEs were 23% and 20%, respectively. The rate of discontinuation due to AEs was 7% in both arms.
The most common AE was neutropenia, which occurred in 26% of patients in the GP2013 arm and 30% of those in the rituximab arm in the combination phase. Rates of neutropenia in the maintenance phase were 10% and 6%, respectively.
Sandoz has decided not to pursue U.S. approval for its rituximab product (GP2013), a proposed biosimiliar of Rituxan/Mabthera.
GP2013 (Rixathon, Riximyo) is already approved outside the U.S.
Sandoz was seeking U.S. approval of GP2013 for all the same indications as the reference product—B-cell non-Hodgkin lymphoma, chronic lymphocytic leukemia, rheumatoid arthritis, granulomatosis with polyangiitis, microscopic polyangiitis, and pemphigus vulgaris.
The U.S. Food and Drug Administration (FDA) had accepted the biologics license application (BLA) for GP2013 in September 2017.
In May of this year, the FDA issued a complete response letter saying it could not approve GP2013. The agency also requested additional information to complement the BLA submission for GP2013.
At the time of the complete response letter, Sandoz said it was still committed to bringing GP2013 to the U.S. market. Now, the company’s position has changed.
“We appreciate the important conversations with the FDA, which have provided specific requirements for our potential U.S. biosimilar rituximab, but believe the patient and marketplace needs in the U.S. will be satisfied before we can generate the data required,” said Stefan Hendriks, global head of biopharmaceuticals at Sandoz.
“We are disappointed to have to make this decision and stand behind the safety, efficacy, and quality of our medicine, which met the stringent criteria for approval in the European Union, Switzerland, Japan, New Zealand, and Australia.”
The BLA for GP2013 was supported, in part, by the ASSIST-FL trial (NCT01419665), in which researchers compared GP2013 to the reference product. Results from this trial were published in The Lancet Haematology in July 2017.
The phase 3 trial included adults with previously untreated, advanced stage follicular lymphoma. Patients received 8 cycles of cyclophosphamide, vincristine, and prednisone with either GP2013 or reference rituximab. Responders then received GP2013 or rituximab monotherapy as maintenance for up to 2 years.
At a median follow-up of 11.6 months, the overall response rate was 87% (271/311) in the GP2013 arm and 88% in the rituximab arm (274/313). Complete response rates were 15% (n=46) and 13% (n=42), respectively.
Rates of adverse events (AEs) were 93% in the GP2013 arm and 91% in the rituximab arm. Rates of serious AEs were 23% and 20%, respectively. The rate of discontinuation due to AEs was 7% in both arms.
The most common AE was neutropenia, which occurred in 26% of patients in the GP2013 arm and 30% of those in the rituximab arm in the combination phase. Rates of neutropenia in the maintenance phase were 10% and 6%, respectively.
Sandoz has decided not to pursue U.S. approval for its rituximab product (GP2013), a proposed biosimiliar of Rituxan/Mabthera.
GP2013 (Rixathon, Riximyo) is already approved outside the U.S.
Sandoz was seeking U.S. approval of GP2013 for all the same indications as the reference product—B-cell non-Hodgkin lymphoma, chronic lymphocytic leukemia, rheumatoid arthritis, granulomatosis with polyangiitis, microscopic polyangiitis, and pemphigus vulgaris.
The U.S. Food and Drug Administration (FDA) had accepted the biologics license application (BLA) for GP2013 in September 2017.
In May of this year, the FDA issued a complete response letter saying it could not approve GP2013. The agency also requested additional information to complement the BLA submission for GP2013.
At the time of the complete response letter, Sandoz said it was still committed to bringing GP2013 to the U.S. market. Now, the company’s position has changed.
“We appreciate the important conversations with the FDA, which have provided specific requirements for our potential U.S. biosimilar rituximab, but believe the patient and marketplace needs in the U.S. will be satisfied before we can generate the data required,” said Stefan Hendriks, global head of biopharmaceuticals at Sandoz.
“We are disappointed to have to make this decision and stand behind the safety, efficacy, and quality of our medicine, which met the stringent criteria for approval in the European Union, Switzerland, Japan, New Zealand, and Australia.”
The BLA for GP2013 was supported, in part, by the ASSIST-FL trial (NCT01419665), in which researchers compared GP2013 to the reference product. Results from this trial were published in The Lancet Haematology in July 2017.
The phase 3 trial included adults with previously untreated, advanced stage follicular lymphoma. Patients received 8 cycles of cyclophosphamide, vincristine, and prednisone with either GP2013 or reference rituximab. Responders then received GP2013 or rituximab monotherapy as maintenance for up to 2 years.
At a median follow-up of 11.6 months, the overall response rate was 87% (271/311) in the GP2013 arm and 88% in the rituximab arm (274/313). Complete response rates were 15% (n=46) and 13% (n=42), respectively.
Rates of adverse events (AEs) were 93% in the GP2013 arm and 91% in the rituximab arm. Rates of serious AEs were 23% and 20%, respectively. The rate of discontinuation due to AEs was 7% in both arms.
The most common AE was neutropenia, which occurred in 26% of patients in the GP2013 arm and 30% of those in the rituximab arm in the combination phase. Rates of neutropenia in the maintenance phase were 10% and 6%, respectively.
CPI-0610 receives fast track designation for MF
The U.S. Food and Drug Administration (FDA) has granted fast track designation to CPI-0610 for the treatment of myelofibrosis (MF).
CPI-0610 is a BET inhibitor being developed by Constellation Pharmaceuticals, Inc.
The company said results from preclinical studies and translational insights from the first-in-human study of CPI-0610 led to the prioritization of CPI-0610 as a potential treatment for MF.
The company is now enrolling patients in the phase 2 portion of the phase 1/2 MANIFEST trial (NCT02158858).
In this trial, researchers are testing CPI-0610 alone or in combination with ruxolitinib in the following patient groups:
- Transfusion-dependent or -independent MF patients who have previously received a JAK inhibitor and are ineligible for or cannot tolerate additional JAK inhibitor therapy, lost response to a JAK inhibitor, or are resistant or refractory to JAK inhibition
- MF patients who are transfusion-dependent or -independent whose disease is not being adequately controlled by ruxolitinib
- MF patients who are anemic and have not previously received a JAK inhibitor.
According to Constellation Pharmaceuticals, CPI-0610 demonstrated clinical activity in the first four patients treated on this trial, all of whom previously received a JAK inhibitor.
The researchers observed reductions in spleen volume and improvements in hemoglobin levels in patients who received monotherapy (n=2) or CPI-0610 plus ruxolitinib (n=2).
One patient treated with the combination experienced resolution of thrombocytosis and became transfusion-independent.
The company said proof-of-concept data from this trial are expected in mid-2019.
About fast track designation
The FDA’s fast track development program is designed to expedite clinical development and submission of applications for products with the potential to treat serious or life-threatening conditions and address unmet medical needs.
Fast track designation facilitates frequent interactions with the FDA review team, including meetings to discuss the product’s development plan and written communications about issues such as trial design and use of biomarkers.
Products that receive fast track designation may be eligible for accelerated approval and priority review if relevant criteria are met. Such products may also be eligible for rolling review, which allows a developer to submit individual sections of a product’s application for review as they are ready, rather than waiting until all sections are complete.
The U.S. Food and Drug Administration (FDA) has granted fast track designation to CPI-0610 for the treatment of myelofibrosis (MF).
CPI-0610 is a BET inhibitor being developed by Constellation Pharmaceuticals, Inc.
The company said results from preclinical studies and translational insights from the first-in-human study of CPI-0610 led to the prioritization of CPI-0610 as a potential treatment for MF.
The company is now enrolling patients in the phase 2 portion of the phase 1/2 MANIFEST trial (NCT02158858).
In this trial, researchers are testing CPI-0610 alone or in combination with ruxolitinib in the following patient groups:
- Transfusion-dependent or -independent MF patients who have previously received a JAK inhibitor and are ineligible for or cannot tolerate additional JAK inhibitor therapy, lost response to a JAK inhibitor, or are resistant or refractory to JAK inhibition
- MF patients who are transfusion-dependent or -independent whose disease is not being adequately controlled by ruxolitinib
- MF patients who are anemic and have not previously received a JAK inhibitor.
According to Constellation Pharmaceuticals, CPI-0610 demonstrated clinical activity in the first four patients treated on this trial, all of whom previously received a JAK inhibitor.
The researchers observed reductions in spleen volume and improvements in hemoglobin levels in patients who received monotherapy (n=2) or CPI-0610 plus ruxolitinib (n=2).
One patient treated with the combination experienced resolution of thrombocytosis and became transfusion-independent.
The company said proof-of-concept data from this trial are expected in mid-2019.
About fast track designation
The FDA’s fast track development program is designed to expedite clinical development and submission of applications for products with the potential to treat serious or life-threatening conditions and address unmet medical needs.
Fast track designation facilitates frequent interactions with the FDA review team, including meetings to discuss the product’s development plan and written communications about issues such as trial design and use of biomarkers.
Products that receive fast track designation may be eligible for accelerated approval and priority review if relevant criteria are met. Such products may also be eligible for rolling review, which allows a developer to submit individual sections of a product’s application for review as they are ready, rather than waiting until all sections are complete.
The U.S. Food and Drug Administration (FDA) has granted fast track designation to CPI-0610 for the treatment of myelofibrosis (MF).
CPI-0610 is a BET inhibitor being developed by Constellation Pharmaceuticals, Inc.
The company said results from preclinical studies and translational insights from the first-in-human study of CPI-0610 led to the prioritization of CPI-0610 as a potential treatment for MF.
The company is now enrolling patients in the phase 2 portion of the phase 1/2 MANIFEST trial (NCT02158858).
In this trial, researchers are testing CPI-0610 alone or in combination with ruxolitinib in the following patient groups:
- Transfusion-dependent or -independent MF patients who have previously received a JAK inhibitor and are ineligible for or cannot tolerate additional JAK inhibitor therapy, lost response to a JAK inhibitor, or are resistant or refractory to JAK inhibition
- MF patients who are transfusion-dependent or -independent whose disease is not being adequately controlled by ruxolitinib
- MF patients who are anemic and have not previously received a JAK inhibitor.
According to Constellation Pharmaceuticals, CPI-0610 demonstrated clinical activity in the first four patients treated on this trial, all of whom previously received a JAK inhibitor.
The researchers observed reductions in spleen volume and improvements in hemoglobin levels in patients who received monotherapy (n=2) or CPI-0610 plus ruxolitinib (n=2).
One patient treated with the combination experienced resolution of thrombocytosis and became transfusion-independent.
The company said proof-of-concept data from this trial are expected in mid-2019.
About fast track designation
The FDA’s fast track development program is designed to expedite clinical development and submission of applications for products with the potential to treat serious or life-threatening conditions and address unmet medical needs.
Fast track designation facilitates frequent interactions with the FDA review team, including meetings to discuss the product’s development plan and written communications about issues such as trial design and use of biomarkers.
Products that receive fast track designation may be eligible for accelerated approval and priority review if relevant criteria are met. Such products may also be eligible for rolling review, which allows a developer to submit individual sections of a product’s application for review as they are ready, rather than waiting until all sections are complete.
FDA and EC approve pegfilgrastim biosimilar
The U.S. Food and Drug Administration (FDA) and European Commission (EC) have approved Coherus BioSciences, Inc.’s pegfilgrastim-cbqv (Udenyca™), a biosimilar of Amgen’s pegfilgrastim product (Neulasta).
Both agencies approved pegfilgrastim-cbqv (formerly CHS-1701) for cancer patients receiving myelosuppressive chemotherapy.
Pegfilgrastim-cbqv is FDA-approved “to decrease the incidence of infection, as manifested by febrile neutropenia, in patients with non-myeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia.”
The product is EC-approved to reduce “the duration of neutropenia and the incidence of febrile neutropenia in adult patients treated with cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukemia and myelodysplastic syndromes).”
The U.S. prescribing information for pegfilgrastim-cbqv is available at www.UDENYCA.com, and the European summary of product characteristics is available on the European Medicines Agency’s website.
The FDA and EC approvals of pegfilgrastim-cbqv were supported by analyses establishing biosimilarity as well as pharmacokinetic, pharmacodynamic, and immunogenicity studies of healthy subjects (NCT02650973, NCT02385851, and NCT02418104).
Results from one of these studies (NCT02650973) were presented at the 2017 ASCO Annual Meeting.
“Udenyca’s robust clinical package includes a dedicated immunogenicity similarity study in over 300 healthy subjects,” said Barbara Finck, MD, chief medical officer of Coherus BioSciences.
“In support of that study, and as part of our commitment to ensuring patient safety, we deployed a battery of sensitive immunogenicity assays. This effort not only supported the biosimilarity of Udenyca but also advanced the understanding of the immunogenic response of pegfilgrastim products.”
The U.S. Food and Drug Administration (FDA) and European Commission (EC) have approved Coherus BioSciences, Inc.’s pegfilgrastim-cbqv (Udenyca™), a biosimilar of Amgen’s pegfilgrastim product (Neulasta).
Both agencies approved pegfilgrastim-cbqv (formerly CHS-1701) for cancer patients receiving myelosuppressive chemotherapy.
Pegfilgrastim-cbqv is FDA-approved “to decrease the incidence of infection, as manifested by febrile neutropenia, in patients with non-myeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia.”
The product is EC-approved to reduce “the duration of neutropenia and the incidence of febrile neutropenia in adult patients treated with cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukemia and myelodysplastic syndromes).”
The U.S. prescribing information for pegfilgrastim-cbqv is available at www.UDENYCA.com, and the European summary of product characteristics is available on the European Medicines Agency’s website.
The FDA and EC approvals of pegfilgrastim-cbqv were supported by analyses establishing biosimilarity as well as pharmacokinetic, pharmacodynamic, and immunogenicity studies of healthy subjects (NCT02650973, NCT02385851, and NCT02418104).
Results from one of these studies (NCT02650973) were presented at the 2017 ASCO Annual Meeting.
“Udenyca’s robust clinical package includes a dedicated immunogenicity similarity study in over 300 healthy subjects,” said Barbara Finck, MD, chief medical officer of Coherus BioSciences.
“In support of that study, and as part of our commitment to ensuring patient safety, we deployed a battery of sensitive immunogenicity assays. This effort not only supported the biosimilarity of Udenyca but also advanced the understanding of the immunogenic response of pegfilgrastim products.”
The U.S. Food and Drug Administration (FDA) and European Commission (EC) have approved Coherus BioSciences, Inc.’s pegfilgrastim-cbqv (Udenyca™), a biosimilar of Amgen’s pegfilgrastim product (Neulasta).
Both agencies approved pegfilgrastim-cbqv (formerly CHS-1701) for cancer patients receiving myelosuppressive chemotherapy.
Pegfilgrastim-cbqv is FDA-approved “to decrease the incidence of infection, as manifested by febrile neutropenia, in patients with non-myeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia.”
The product is EC-approved to reduce “the duration of neutropenia and the incidence of febrile neutropenia in adult patients treated with cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukemia and myelodysplastic syndromes).”
The U.S. prescribing information for pegfilgrastim-cbqv is available at www.UDENYCA.com, and the European summary of product characteristics is available on the European Medicines Agency’s website.
The FDA and EC approvals of pegfilgrastim-cbqv were supported by analyses establishing biosimilarity as well as pharmacokinetic, pharmacodynamic, and immunogenicity studies of healthy subjects (NCT02650973, NCT02385851, and NCT02418104).
Results from one of these studies (NCT02650973) were presented at the 2017 ASCO Annual Meeting.
“Udenyca’s robust clinical package includes a dedicated immunogenicity similarity study in over 300 healthy subjects,” said Barbara Finck, MD, chief medical officer of Coherus BioSciences.
“In support of that study, and as part of our commitment to ensuring patient safety, we deployed a battery of sensitive immunogenicity assays. This effort not only supported the biosimilarity of Udenyca but also advanced the understanding of the immunogenic response of pegfilgrastim products.”
Breakthrough designation for pathogen-reduced cryoprecipitate
The U.S. Food and Drug Administration (FDA) has granted breakthrough device designation for pathogen-reduced cryoprecipitate manufactured from plasma treated with the INTERCEPT Blood System.
Cerus Corporation aims to seek FDA approval for this pathogen-reduced cryoprecipitate to treat massive hemorrhage.
“The proposed label indication for pathogen-reduced cryoprecipitate would be to control massive bleeding associated with fibrinogen deficiency,” said Laurence Corash, chief scientific officer of Cerus.
The proposed shelf life for pathogen-reduced cyroprecipitate is 5 days at room temperature.
The INTERCEPT Blood System is already FDA-approved for the inactivation of pathogens in platelets and plasma.
“Cryo[precipitate] is a natural extension to our current FDA-approved INTERCEPT Blood System for plasma,” said William “Obi” Greenman, president and chief executive officer of Cerus.
If the FDA granted approval, INTERCEPT-treated plasma could be manufactured into pathogen-reduced cryoprecipitate.
About breakthrough device designation
The FDA says it grants breakthrough designation to devices “that provide more effective treatment or diagnosis of life-threatening or irreversibly debilitating human diseases or conditions.”
Breakthrough designation is intended to expedite the development, assessment, and review of medical devices. The breakthrough devices program supersedes the FDA’s expedited access pathway and priority review programs.
The U.S. Food and Drug Administration (FDA) has granted breakthrough device designation for pathogen-reduced cryoprecipitate manufactured from plasma treated with the INTERCEPT Blood System.
Cerus Corporation aims to seek FDA approval for this pathogen-reduced cryoprecipitate to treat massive hemorrhage.
“The proposed label indication for pathogen-reduced cryoprecipitate would be to control massive bleeding associated with fibrinogen deficiency,” said Laurence Corash, chief scientific officer of Cerus.
The proposed shelf life for pathogen-reduced cyroprecipitate is 5 days at room temperature.
The INTERCEPT Blood System is already FDA-approved for the inactivation of pathogens in platelets and plasma.
“Cryo[precipitate] is a natural extension to our current FDA-approved INTERCEPT Blood System for plasma,” said William “Obi” Greenman, president and chief executive officer of Cerus.
If the FDA granted approval, INTERCEPT-treated plasma could be manufactured into pathogen-reduced cryoprecipitate.
About breakthrough device designation
The FDA says it grants breakthrough designation to devices “that provide more effective treatment or diagnosis of life-threatening or irreversibly debilitating human diseases or conditions.”
Breakthrough designation is intended to expedite the development, assessment, and review of medical devices. The breakthrough devices program supersedes the FDA’s expedited access pathway and priority review programs.
The U.S. Food and Drug Administration (FDA) has granted breakthrough device designation for pathogen-reduced cryoprecipitate manufactured from plasma treated with the INTERCEPT Blood System.
Cerus Corporation aims to seek FDA approval for this pathogen-reduced cryoprecipitate to treat massive hemorrhage.
“The proposed label indication for pathogen-reduced cryoprecipitate would be to control massive bleeding associated with fibrinogen deficiency,” said Laurence Corash, chief scientific officer of Cerus.
The proposed shelf life for pathogen-reduced cyroprecipitate is 5 days at room temperature.
The INTERCEPT Blood System is already FDA-approved for the inactivation of pathogens in platelets and plasma.
“Cryo[precipitate] is a natural extension to our current FDA-approved INTERCEPT Blood System for plasma,” said William “Obi” Greenman, president and chief executive officer of Cerus.
If the FDA granted approval, INTERCEPT-treated plasma could be manufactured into pathogen-reduced cryoprecipitate.
About breakthrough device designation
The FDA says it grants breakthrough designation to devices “that provide more effective treatment or diagnosis of life-threatening or irreversibly debilitating human diseases or conditions.”
Breakthrough designation is intended to expedite the development, assessment, and review of medical devices. The breakthrough devices program supersedes the FDA’s expedited access pathway and priority review programs.
Health Canada approves pralatrexate for rel/ref PTCL
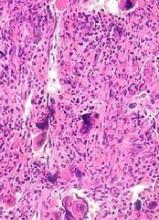
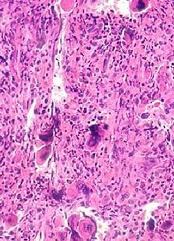
Health Canada has granted conditional approval for pralatrexate (Folotyn®) to treat relapsed or refractory peripheral T-cell lymphoma (PTCL).
Pralatrexate received a Notice of Compliance with Conditions (NOC/c), which is an approval granted on the basis of promising evidence of clinical effectiveness that must be verified in additional clinical trials.
To be approved under Health Canada’s NOC/c policy, a product must be intended for the treatment, prevention, or diagnosis of a serious, life-threatening, or severely debilitating illness.
In addition, the product must have demonstrated promising benefit, be of high quality, have an acceptable safety profile based on a benefit/risk assessment, and either respond to a serious unmet need or provide a significant improvement over existing therapies.
The NOC/c for pralatrexate is based on response rates in the single-arm, phase 2 PROPEL trial. Results from PROPEL were published in the Journal of Clinical Oncology in 2011.
The trial enrolled 115 patients with relapsed or refractory PTCL who had received a median of three (range, 1-12) prior systemic therapies.
The patients received pralatrexate once weekly at a dose of 30 mg/m2 for 6 weeks in 7-week cycles until disease progression or unacceptable toxicity.
In the 109 evaluable patients, the response rate was 29% (32/109). The complete response rate was 11% (n=12), and the partial response rate was 18% (n=20).
The median duration of response was 10.1 months, the median progression-free survival was 3.5 months, and the median overall survival was 14.5 months.
The most common adverse events (AEs) were mucositis (71%), thrombocytopenia (41%), nausea (41%), fatigue (36%), pyrexia (34%), anemia (34%), constipation (34%), edema (31%), cough (29%), epistaxis (26%), vomiting (25%), neutropenia (25%), and diarrhea (23%).
The most common grade 3/4 AEs were thrombocytopenia (32%), mucositis (22%), neutropenia (22%), and anemia (18%).
The product monograph for pralatrexate contains a boxed warning highlighting the risk of AEs associated with pralatrexate use, including dermatologic reactions, bone marrow suppression, infection, mucosal inflammation, tumor lysis syndrome, potential fetal harm, and pulmonary toxicity.
The product monograph is available for download from the website of Servier Canada, the company marketing pralatrexate in Canada.
Health Canada has granted conditional approval for pralatrexate (Folotyn®) to treat relapsed or refractory peripheral T-cell lymphoma (PTCL).
Pralatrexate received a Notice of Compliance with Conditions (NOC/c), which is an approval granted on the basis of promising evidence of clinical effectiveness that must be verified in additional clinical trials.
To be approved under Health Canada’s NOC/c policy, a product must be intended for the treatment, prevention, or diagnosis of a serious, life-threatening, or severely debilitating illness.
In addition, the product must have demonstrated promising benefit, be of high quality, have an acceptable safety profile based on a benefit/risk assessment, and either respond to a serious unmet need or provide a significant improvement over existing therapies.
The NOC/c for pralatrexate is based on response rates in the single-arm, phase 2 PROPEL trial. Results from PROPEL were published in the Journal of Clinical Oncology in 2011.
The trial enrolled 115 patients with relapsed or refractory PTCL who had received a median of three (range, 1-12) prior systemic therapies.
The patients received pralatrexate once weekly at a dose of 30 mg/m2 for 6 weeks in 7-week cycles until disease progression or unacceptable toxicity.
In the 109 evaluable patients, the response rate was 29% (32/109). The complete response rate was 11% (n=12), and the partial response rate was 18% (n=20).
The median duration of response was 10.1 months, the median progression-free survival was 3.5 months, and the median overall survival was 14.5 months.
The most common adverse events (AEs) were mucositis (71%), thrombocytopenia (41%), nausea (41%), fatigue (36%), pyrexia (34%), anemia (34%), constipation (34%), edema (31%), cough (29%), epistaxis (26%), vomiting (25%), neutropenia (25%), and diarrhea (23%).
The most common grade 3/4 AEs were thrombocytopenia (32%), mucositis (22%), neutropenia (22%), and anemia (18%).
The product monograph for pralatrexate contains a boxed warning highlighting the risk of AEs associated with pralatrexate use, including dermatologic reactions, bone marrow suppression, infection, mucosal inflammation, tumor lysis syndrome, potential fetal harm, and pulmonary toxicity.
The product monograph is available for download from the website of Servier Canada, the company marketing pralatrexate in Canada.
Health Canada has granted conditional approval for pralatrexate (Folotyn®) to treat relapsed or refractory peripheral T-cell lymphoma (PTCL).
Pralatrexate received a Notice of Compliance with Conditions (NOC/c), which is an approval granted on the basis of promising evidence of clinical effectiveness that must be verified in additional clinical trials.
To be approved under Health Canada’s NOC/c policy, a product must be intended for the treatment, prevention, or diagnosis of a serious, life-threatening, or severely debilitating illness.
In addition, the product must have demonstrated promising benefit, be of high quality, have an acceptable safety profile based on a benefit/risk assessment, and either respond to a serious unmet need or provide a significant improvement over existing therapies.
The NOC/c for pralatrexate is based on response rates in the single-arm, phase 2 PROPEL trial. Results from PROPEL were published in the Journal of Clinical Oncology in 2011.
The trial enrolled 115 patients with relapsed or refractory PTCL who had received a median of three (range, 1-12) prior systemic therapies.
The patients received pralatrexate once weekly at a dose of 30 mg/m2 for 6 weeks in 7-week cycles until disease progression or unacceptable toxicity.
In the 109 evaluable patients, the response rate was 29% (32/109). The complete response rate was 11% (n=12), and the partial response rate was 18% (n=20).
The median duration of response was 10.1 months, the median progression-free survival was 3.5 months, and the median overall survival was 14.5 months.
The most common adverse events (AEs) were mucositis (71%), thrombocytopenia (41%), nausea (41%), fatigue (36%), pyrexia (34%), anemia (34%), constipation (34%), edema (31%), cough (29%), epistaxis (26%), vomiting (25%), neutropenia (25%), and diarrhea (23%).
The most common grade 3/4 AEs were thrombocytopenia (32%), mucositis (22%), neutropenia (22%), and anemia (18%).
The product monograph for pralatrexate contains a boxed warning highlighting the risk of AEs associated with pralatrexate use, including dermatologic reactions, bone marrow suppression, infection, mucosal inflammation, tumor lysis syndrome, potential fetal harm, and pulmonary toxicity.
The product monograph is available for download from the website of Servier Canada, the company marketing pralatrexate in Canada.
EC approves venetoclax in combo with rituximab
The European Commission (EC) has approved a new indication for venetoclax (Venclyxto®).
The drug is now approved for use in combination with rituximab to treat patients with relapsed/refractory chronic lymphocytic leukemia (CLL) who have received at least one prior therapy.
The approval is valid in all member states of the European Union as well as Iceland, Liechtenstein, and Norway.
The EC’s approval is based on results from the phase 3 MURANO trial, which were published in The New England Journal of Medicine in March.
The trial included 389 CLL patients who were randomized to receive venetoclax plus rituximab (VEN+R) or bendamustine plus rituximab (B+R). The median follow-up was 23.8 months.
According to an independent review committee, the overall response rate was 92.3% in the VEN+R arm and 72.3% in the B+R arm. The investigator-assessed overall response rates were 93.3% and 67.7%, respectively.
According to investigators, the median progression-free survival (PFS) was not reached in the VEN+R arm and was 17.0 months in the B+R arm (hazard ratio [HR]=0.17; P<0.0001).
According to the independent review committee, the median PFS was not reached in the VEN+R arm and was 18.1 months in the B+R arm (HR=0.20; P<0.0001).
Investigators said the 2-year PFS rate was 84.9% in the VEN+R arm and 36.3% in the B+R arm.
They said the 2-year overall survival rates were 91.9% and 86.6%, respectively (HR=0.48; P<0.0001). The median overall survival was not reached in either arm.
Grade 3/4 adverse events (AEs) with at least a 2% difference in incidence between the treatment arms (in the VEN+R and B+R arms, respectively) included:
- Neutropenia (57.7% and 38.8%)
- Infections and infestations (17.5% and 21.8%)
- Anemia (10.8% and 13.8%)
- Thrombocytopenia (5.7% and 10.1%)
- Febrile neutropenia (3.6% and 9.6%)
- Pneumonia (5.2% and 8.0%)
- Infusion-related reactions (1.5% and 5.3%)
- Tumor lysis syndrome (3.1% and 1.1%)
- Hypotension (0% and 2.7%)
- Hyperglycemia (2.1% and 0%)
- Hypogammaglobulinemia (2.1% and 0%).
Serious AEs with at least a 2% difference in incidence between the arms (in the VEN+R and B+R arms, respectively) were:
- Pneumonia (8.2% and 8.0%)
- Febrile neutropenia (3.6% and 8.5%)
- Pyrexia (2.6% and 6.9%)
- Anemia (1.5% and 2.7%)
- Infusion-related reactions (0.5% and 3.2%)
- Sepsis (0.5% and 2.1%)
- Tumor lysis syndrome (2.1% and 0.5%)
- Hypotension (0% and 2.7%).
Fatal AEs occurred in 5.2% of patients in the VEN+R arm and 5.9% in the B+R arm.
Fatal AEs in the VEN+R arm included pneumonia (n=3), sepsis (n=1), thrombocytopenia (n=1), cardiac failure (n=1), myocardial infarction (n=1), sudden cardiac death (n=1), colorectal cancer (n=1), status epilepticus (n=1), and acute respiratory failure (n=1). Two cases of pneumonia occurred in the setting of progression/Richter’s transformation.
The European Commission (EC) has approved a new indication for venetoclax (Venclyxto®).
The drug is now approved for use in combination with rituximab to treat patients with relapsed/refractory chronic lymphocytic leukemia (CLL) who have received at least one prior therapy.
The approval is valid in all member states of the European Union as well as Iceland, Liechtenstein, and Norway.
The EC’s approval is based on results from the phase 3 MURANO trial, which were published in The New England Journal of Medicine in March.
The trial included 389 CLL patients who were randomized to receive venetoclax plus rituximab (VEN+R) or bendamustine plus rituximab (B+R). The median follow-up was 23.8 months.
According to an independent review committee, the overall response rate was 92.3% in the VEN+R arm and 72.3% in the B+R arm. The investigator-assessed overall response rates were 93.3% and 67.7%, respectively.
According to investigators, the median progression-free survival (PFS) was not reached in the VEN+R arm and was 17.0 months in the B+R arm (hazard ratio [HR]=0.17; P<0.0001).
According to the independent review committee, the median PFS was not reached in the VEN+R arm and was 18.1 months in the B+R arm (HR=0.20; P<0.0001).
Investigators said the 2-year PFS rate was 84.9% in the VEN+R arm and 36.3% in the B+R arm.
They said the 2-year overall survival rates were 91.9% and 86.6%, respectively (HR=0.48; P<0.0001). The median overall survival was not reached in either arm.
Grade 3/4 adverse events (AEs) with at least a 2% difference in incidence between the treatment arms (in the VEN+R and B+R arms, respectively) included:
- Neutropenia (57.7% and 38.8%)
- Infections and infestations (17.5% and 21.8%)
- Anemia (10.8% and 13.8%)
- Thrombocytopenia (5.7% and 10.1%)
- Febrile neutropenia (3.6% and 9.6%)
- Pneumonia (5.2% and 8.0%)
- Infusion-related reactions (1.5% and 5.3%)
- Tumor lysis syndrome (3.1% and 1.1%)
- Hypotension (0% and 2.7%)
- Hyperglycemia (2.1% and 0%)
- Hypogammaglobulinemia (2.1% and 0%).
Serious AEs with at least a 2% difference in incidence between the arms (in the VEN+R and B+R arms, respectively) were:
- Pneumonia (8.2% and 8.0%)
- Febrile neutropenia (3.6% and 8.5%)
- Pyrexia (2.6% and 6.9%)
- Anemia (1.5% and 2.7%)
- Infusion-related reactions (0.5% and 3.2%)
- Sepsis (0.5% and 2.1%)
- Tumor lysis syndrome (2.1% and 0.5%)
- Hypotension (0% and 2.7%).
Fatal AEs occurred in 5.2% of patients in the VEN+R arm and 5.9% in the B+R arm.
Fatal AEs in the VEN+R arm included pneumonia (n=3), sepsis (n=1), thrombocytopenia (n=1), cardiac failure (n=1), myocardial infarction (n=1), sudden cardiac death (n=1), colorectal cancer (n=1), status epilepticus (n=1), and acute respiratory failure (n=1). Two cases of pneumonia occurred in the setting of progression/Richter’s transformation.
The European Commission (EC) has approved a new indication for venetoclax (Venclyxto®).
The drug is now approved for use in combination with rituximab to treat patients with relapsed/refractory chronic lymphocytic leukemia (CLL) who have received at least one prior therapy.
The approval is valid in all member states of the European Union as well as Iceland, Liechtenstein, and Norway.
The EC’s approval is based on results from the phase 3 MURANO trial, which were published in The New England Journal of Medicine in March.
The trial included 389 CLL patients who were randomized to receive venetoclax plus rituximab (VEN+R) or bendamustine plus rituximab (B+R). The median follow-up was 23.8 months.
According to an independent review committee, the overall response rate was 92.3% in the VEN+R arm and 72.3% in the B+R arm. The investigator-assessed overall response rates were 93.3% and 67.7%, respectively.
According to investigators, the median progression-free survival (PFS) was not reached in the VEN+R arm and was 17.0 months in the B+R arm (hazard ratio [HR]=0.17; P<0.0001).
According to the independent review committee, the median PFS was not reached in the VEN+R arm and was 18.1 months in the B+R arm (HR=0.20; P<0.0001).
Investigators said the 2-year PFS rate was 84.9% in the VEN+R arm and 36.3% in the B+R arm.
They said the 2-year overall survival rates were 91.9% and 86.6%, respectively (HR=0.48; P<0.0001). The median overall survival was not reached in either arm.
Grade 3/4 adverse events (AEs) with at least a 2% difference in incidence between the treatment arms (in the VEN+R and B+R arms, respectively) included:
- Neutropenia (57.7% and 38.8%)
- Infections and infestations (17.5% and 21.8%)
- Anemia (10.8% and 13.8%)
- Thrombocytopenia (5.7% and 10.1%)
- Febrile neutropenia (3.6% and 9.6%)
- Pneumonia (5.2% and 8.0%)
- Infusion-related reactions (1.5% and 5.3%)
- Tumor lysis syndrome (3.1% and 1.1%)
- Hypotension (0% and 2.7%)
- Hyperglycemia (2.1% and 0%)
- Hypogammaglobulinemia (2.1% and 0%).
Serious AEs with at least a 2% difference in incidence between the arms (in the VEN+R and B+R arms, respectively) were:
- Pneumonia (8.2% and 8.0%)
- Febrile neutropenia (3.6% and 8.5%)
- Pyrexia (2.6% and 6.9%)
- Anemia (1.5% and 2.7%)
- Infusion-related reactions (0.5% and 3.2%)
- Sepsis (0.5% and 2.1%)
- Tumor lysis syndrome (2.1% and 0.5%)
- Hypotension (0% and 2.7%).
Fatal AEs occurred in 5.2% of patients in the VEN+R arm and 5.9% in the B+R arm.
Fatal AEs in the VEN+R arm included pneumonia (n=3), sepsis (n=1), thrombocytopenia (n=1), cardiac failure (n=1), myocardial infarction (n=1), sudden cardiac death (n=1), colorectal cancer (n=1), status epilepticus (n=1), and acute respiratory failure (n=1). Two cases of pneumonia occurred in the setting of progression/Richter’s transformation.
Test strips for warfarin monitoring recalled due to serious risks
The U.S. Food and Drug Administration (FDA) announced a Class I recall of test strips used with medical devices that monitor warfarin levels, which means use of these strips may cause serious injuries or death.
Roche Diagnostics has recalled certain test strip lots used with its CoaguChek test meter devices.
The recall involves more than 1.1 million packages of CoaguChek XS PT Test Strips that were distributed nationwide from January 12, 2018, to October 29, 2018.
The test strips are used with the CoaguChek XS plus, CoaguChek XS Pro, CoaguChek XS professional, CoaguChek XS PST, and CoaguChek Vantus test meter devices.
The FDA said patients and healthcare professionals should not rely on these test meter devices to monitor warfarin levels if they’re using test strips affected by the recall. Instead, patients should have blood drawn from a vein and have their levels measured by a laboratory test or use an alternative meter device.
“These strips are widely used, and we are working diligently to warn healthcare providers and the public about the dangers associated with this recall,” said Jeffrey Shuren, MD, director of the FDA’s Center for Devices and Radiological Health.
“Using faulty strips can lead to serious errors in medication dosage that could cause serious harm or death in some patients. We are also working with the company on the swift removal of the recalled strips and to ensure the new corrected strips are distributed to patients and healthcare providers as quickly as possible.”
The FDA’s warning concerning the CoaguChek XS PT Test Strips is based on medical device reports submitted by Roche Diagnostics indicating that the test strips may provide results that are higher than the actual international normalized ratio (INR).
As a result of incorrect INR results, some patients may be prescribed an insufficient warfarin dose or instructed to interrupt warfarin use, which may increase the risk of thrombosis.
Approximately 90 medical device reports and two serious patient injuries involving strokes were reported to the FDA.
Roche Diagnostics attributes the cause of the problem to a recent recalibration of the test strips to a different international standard.
The company plans to provide new batches of recalibrated test strips, based on the previous international standard, to their customers by the end of November.
The FDA reviewed validation data submitted by the company for these recalibrated strips.
Patients who are using CoaguChek meters should contact their healthcare provider to get information about alternative test methods and to address questions regarding their individual testing schedule. Patients should also contact their self-testing service providers to find out when they will be getting their corrected test strips.
For questions about the recall or to report adverse reactions or quality problems, contact Roche Diagnostics Point of Care Technical Service at 1-800-428-4674.
Adverse reactions can also be reported to the FDA through MedWatch, the agency’s voluntary reporting program.
The U.S. Food and Drug Administration (FDA) announced a Class I recall of test strips used with medical devices that monitor warfarin levels, which means use of these strips may cause serious injuries or death.
Roche Diagnostics has recalled certain test strip lots used with its CoaguChek test meter devices.
The recall involves more than 1.1 million packages of CoaguChek XS PT Test Strips that were distributed nationwide from January 12, 2018, to October 29, 2018.
The test strips are used with the CoaguChek XS plus, CoaguChek XS Pro, CoaguChek XS professional, CoaguChek XS PST, and CoaguChek Vantus test meter devices.
The FDA said patients and healthcare professionals should not rely on these test meter devices to monitor warfarin levels if they’re using test strips affected by the recall. Instead, patients should have blood drawn from a vein and have their levels measured by a laboratory test or use an alternative meter device.
“These strips are widely used, and we are working diligently to warn healthcare providers and the public about the dangers associated with this recall,” said Jeffrey Shuren, MD, director of the FDA’s Center for Devices and Radiological Health.
“Using faulty strips can lead to serious errors in medication dosage that could cause serious harm or death in some patients. We are also working with the company on the swift removal of the recalled strips and to ensure the new corrected strips are distributed to patients and healthcare providers as quickly as possible.”
The FDA’s warning concerning the CoaguChek XS PT Test Strips is based on medical device reports submitted by Roche Diagnostics indicating that the test strips may provide results that are higher than the actual international normalized ratio (INR).
As a result of incorrect INR results, some patients may be prescribed an insufficient warfarin dose or instructed to interrupt warfarin use, which may increase the risk of thrombosis.
Approximately 90 medical device reports and two serious patient injuries involving strokes were reported to the FDA.
Roche Diagnostics attributes the cause of the problem to a recent recalibration of the test strips to a different international standard.
The company plans to provide new batches of recalibrated test strips, based on the previous international standard, to their customers by the end of November.
The FDA reviewed validation data submitted by the company for these recalibrated strips.
Patients who are using CoaguChek meters should contact their healthcare provider to get information about alternative test methods and to address questions regarding their individual testing schedule. Patients should also contact their self-testing service providers to find out when they will be getting their corrected test strips.
For questions about the recall or to report adverse reactions or quality problems, contact Roche Diagnostics Point of Care Technical Service at 1-800-428-4674.
Adverse reactions can also be reported to the FDA through MedWatch, the agency’s voluntary reporting program.
The U.S. Food and Drug Administration (FDA) announced a Class I recall of test strips used with medical devices that monitor warfarin levels, which means use of these strips may cause serious injuries or death.
Roche Diagnostics has recalled certain test strip lots used with its CoaguChek test meter devices.
The recall involves more than 1.1 million packages of CoaguChek XS PT Test Strips that were distributed nationwide from January 12, 2018, to October 29, 2018.
The test strips are used with the CoaguChek XS plus, CoaguChek XS Pro, CoaguChek XS professional, CoaguChek XS PST, and CoaguChek Vantus test meter devices.
The FDA said patients and healthcare professionals should not rely on these test meter devices to monitor warfarin levels if they’re using test strips affected by the recall. Instead, patients should have blood drawn from a vein and have their levels measured by a laboratory test or use an alternative meter device.
“These strips are widely used, and we are working diligently to warn healthcare providers and the public about the dangers associated with this recall,” said Jeffrey Shuren, MD, director of the FDA’s Center for Devices and Radiological Health.
“Using faulty strips can lead to serious errors in medication dosage that could cause serious harm or death in some patients. We are also working with the company on the swift removal of the recalled strips and to ensure the new corrected strips are distributed to patients and healthcare providers as quickly as possible.”
The FDA’s warning concerning the CoaguChek XS PT Test Strips is based on medical device reports submitted by Roche Diagnostics indicating that the test strips may provide results that are higher than the actual international normalized ratio (INR).
As a result of incorrect INR results, some patients may be prescribed an insufficient warfarin dose or instructed to interrupt warfarin use, which may increase the risk of thrombosis.
Approximately 90 medical device reports and two serious patient injuries involving strokes were reported to the FDA.
Roche Diagnostics attributes the cause of the problem to a recent recalibration of the test strips to a different international standard.
The company plans to provide new batches of recalibrated test strips, based on the previous international standard, to their customers by the end of November.
The FDA reviewed validation data submitted by the company for these recalibrated strips.
Patients who are using CoaguChek meters should contact their healthcare provider to get information about alternative test methods and to address questions regarding their individual testing schedule. Patients should also contact their self-testing service providers to find out when they will be getting their corrected test strips.
For questions about the recall or to report adverse reactions or quality problems, contact Roche Diagnostics Point of Care Technical Service at 1-800-428-4674.
Adverse reactions can also be reported to the FDA through MedWatch, the agency’s voluntary reporting program.