User login
The painful knee: Choosing the right imaging test
Radiography plays a key role in the initial evaluation of acute knee pain in adults. Yet conflicting studies and the absence of clear guidelines may leave the primary care physician uncertain as to which imaging test to order—ie, whether radiography is sufficient, and when computed tomography (CT) or magnetic resonance imaging (MRI) is needed. This article reviews the indications for radiologic examination of the knee and discusses indications for cross-sectional imaging studies. Imaging in oncology patients is not discussed here.
ACUTE KNEE PAIN: A TYPICAL SCENARIO
A 47-year-old woman presents to the emergency department with left knee pain after a motor vehicle accident that occurred the day before. The car she was driving hit a tree, and she hit her knee on the dashboard. She was wearing a seatbelt at the time of the accident. She says she was unable to walk immediately after the accident because of knee pain.
The initial examination in the emergency room reveals swelling and pain throughout the range of motion. The anterior drawer test and the Lachman test are negative (see below).
The patient is discharged home with a knee immobilizer, pain medication, and crutches, with instructions for a follow-up visit in the orthopedics clinic.
Five days later, she returns to the emergency department complaining of continuing knee pain. She says the knee gives way when she puts weight on it. The physical findings are unchanged, and she is discharged home with a follow-up appointment with orthopedics in 3 days.
At the follow-up visit, she complains of persistent knee pain in the medial aspect of the knee joint. Physical examination is difficult because of pain and swelling, and it reveals mild joint effusion with no gross instability. She has pain on the medial side with valgus stress, but there appears to be a hard end point. There is no posterior sag, and the Lachman test is negative.
Based on the physical examination and the patient’s complaints, she receives a diagnosis of medial collateral ligament strain and injury. She is given a hinged brace and is instructed to undergo a physical rehabilitation program.
Three weeks after the initial evaluation, she returns to the orthopedics clinic with continuing knee problems. Mild knee effusion persists, but she has less pain and swelling, allowing a more complete examination. The examination reveals less limitation of range of motion and a hint of positivity on the Lachman test. The knee is diffusely tender, and the pain seems out of proportion with the maneuvers used during the examination. She requests more pain medication. You suspect internal derangement of the knee. Which imaging test should you order to further evaluate this patient?
A SYSTEMATIC AND COST-EFFECTIVE APPROACH IS NEEDED
The case presented above represents a typical scenario for the presentation of acute knee pain and illustrates the diagnostic challenges.
Knee pain is a common reason for emergency room visits, and it accounts for approximately 1.9 million visits to primary care clinics annually.1 In the emergency department, most patients undergo plain radiography to assess for fracture, yet approximately 92% of radiographic studies do not show a fracture.2 Clearly, the evaluation of knee pain requires a systematic, accurate, and cost-effective approach.
Key elements of the physical examination
In acute knee pain, accurate diagnosis begins with a detailed history and physical examination.
The anterior drawer test is done to evaluate the anterior cruciate ligament. With the relaxed knee flexed to approximately 80° and the foot stabilized in a neutral position, the examiner grasps the proximal tibia in a firm yet gentle grip, and then applies anterior force, noting the degree of anterior displacement compared with the other knee.
The Lachman test, a variation of the anterior drawer test, is more definitive for the anterior cruciate ligament and is carried out with the knee in 15° of flexion and external rotation, in order to relax the iliotibial band. The upper hand grasps the distal thigh, and the lower hand, with the thumb on the tibial tubercle, pulls the tibia forward. The degree of anterior motion in millimeters is noted and compared with that on the other side, and the end point is graded as “soft” or “hard.” An end point is considered hard when a ligament abruptly halts the motion of the bone being tested against the stabilized bone. An end point is considered soft when the ligament is disrupted and the restraints are the more elastic secondary stabilizers.
Debate continues
Some authors contend that in skilled hands a thorough history, physical examination, and radiographic examination are sufficient to diagnose trauma-related intra-articular knee disorders.3 Others contend that MRI plays a key role in the initial evaluation. A number of studies4–8 have shown that using MRI in the initial evaluation not only identifies key lesions, but also may eliminate the need for an invasive diagnostic procedure (ie, arthroscopy).
For example, MRI can reveal fracture, stress fracture, insufficiency fracture, and transient patellar dislocation—conditions that may satisfactorily explain knee symptoms.
PLAIN RADIOGRAPHY STILL THE FIRST STEP IN KNEE EVALUATION
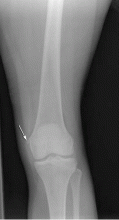
Radiography is the first step in the evaluation of knee pain. It is quick and inexpensive and can yield many diagnostic clues. It can readily reveal fractures, osteochondral defects, bony lesions, joint effusions, joint space narrowing, and bone misalignment.
In patients with knee trauma, supine anteroposterior and cross-table lateral radiographic images are generally obtained. In patients whose knee pain is not due to trauma, standing projections are done, as well as dedicated projection of the patellofemoral articulation. A standing series is most helpful for evaluating joint space and alignment.
Applying the Ottawa rules
When a patient presents to the emergency room with acute knee pain, the immediate concern is whether he or she has a fracture. The Ottawa knee rules9 for when to order radiography in adults with knee pain are highly sensitive for detecting a clinically important fracture. If any one of the five Ottawa criteria applies—ie, the patient is age 55 or older, has tenderness at the head of the fibula, has patellar tenderness, is unable to flex the knee to 90°, or is unable to bear weight—then radiography is indicated.
While studies have validated the ability of the Ottawa rules to detect important fractures in acute knee injury,2,10 fracture is the cause of only a small percentage of knee complaints in the primary care setting. More common causes include osteoarthritis, meniscal injury, ligamental injury, and crystal arthropathy, and these account for approximately half of all diagnoses. Sprain and strain account for most of the rest of knee injuries.1
Acute exacerbations of osteoarthritis
Osteoarthritis is a chronic problem, yet it is not unusual for a patient to present to the primary care physician with an acute exacerbation of joint pain. The clinical hallmarks include age over 50, stiffness lasting less than 30 minutes, bony enlargement and tenderness, and crepitus. The radiographic hallmarks, according to the Kellgren-Lawrence grading scale, are joint space narrowing, osteophytes, subchondral cysts, and sclerosis. These radiographic findings correlate well with clinical findings in these patients.11
Situations in which radiography is less helpful
In some cases the radiographic findings may not explain the patient’s clinical signs and symptoms. For example, in suspected crystalline and septic arthritis, the clinical presentation may include warmth, erythema, and effusion. Arthrocentesis would be indicated in such a patient. Indeed, in the case of suspected pseudogout, chondrocalcinosis may be radiographically evident. However, it is also present in many patients without symptoms or with osteoarthritis, so radiographic evidence does not provide a definite diagnosis.
While radiography may not always identify the cause of knee pain, it is useful in excluding serious problems such as fractures, advanced degenerative changes, and neoplasms, and it may help direct further management. Radiography is not useful in the evaluation of the cruciate and collateral ligaments, the menisci, and the hyaline cartilage of the knee and may fail to show an insufficiency or stress fracture. To evaluate these structures and associated soft tissues, MRI is preferable.
COMPUTED TOMOGRAPHY IN ACUTE KNEE PAIN
CURRENT USES OF MRI TO EVALUATE ACUTE KNEE PAIN
As mentioned above, MRI is useful in evaluating suspected meniscal and ligamentous injuries.
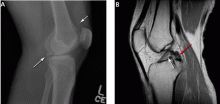
Figure 3 shows how T2-weighted MRI was used to evaluate for suspected meniscal injury in our 47-year-old female patient with left knee pain after a motor vehicle accident.
Still a matter of debate
MRI’s role in the diagnosis of knee pain is still a contentious issue.
Advantages of MRI are that it is noninvasive, it does not use ionizing radiation, it gives multiplanar images, and it provides images of soft-tissue structures, which other imaging methods cannot.12 It is a well-proven and widely accepted test. Its sensitivity for detecting meniscal and cruciate ligament injury ranges from 75% to 88%,1 and it can help in the evaluation of other injuries for which radiography is not useful, including synovitis, bone bruise, stress or insufficiency fracture, osteochondral defects, and osteonecrosis.
In addition, several studies show that using MRI to establish the diagnosis in acute knee pain can mean that 22% to 42% fewer arthroscopic procedures need to be performed.4–8 Authors of a prospective double-blind study8 recommended that MRI be used in patients with acute knee injury when the findings of the clinical history and examination by orthopedic surgeons prove equivocal.8 MRI evaluation is especially desirable for young, active patients who wish to resume activity as soon as possible.
A routine MRI examination consists of T1- and T2-weighted images in three planes, although the number of sequences and planes varies from hospital to hospital. The use of gadolinium contrast is indicated only when osteomyelitis, septic arthritis, or a mass is suspected.
Disadvantages of MRI include its cost: Medicare reimbursement for knee MRI is around $400, compared with $200 for knee CT and $50 for knee radiography with four views. Also, while studies have shown MRI to have a high sensitivity and specificity in the diagnosis of acute knee injury, some have reported a high false-positive rate for the detection of meniscal tear.13,14 MRI has also been shown to have a lower sensitivity than arthroscopy for lesions of the articular cartilage.13 Furthermore, MRI has been shown to reveal cartilage lesions, osteophytes, and meniscal abnormalities in asymptomatic study volunteers with no history of pain, trauma or knee disease.14 Therefore, findings on MRI must closely correlate with findings on the history and physical examination.
Additional indications for knee MRI
Cartilage can be assessed on routine MRI sequences of the knee. Since closed MRI systems have more powerful magnets than open systems, closed MRI systems provide greater anatomic detail.
MRI can identify other lesions, such as spontaneous osteonecrosis of the knee, usually seen in elderly women who may present with sudden knee pain. In such patients, MRI findings of focal replacement of the bone marrow and surrounding edema are specific for osteonecrosis.
Opinions vary as to whether bone marrow edema is always associated with pain. Sequential MRI studies have shown persistence of bone marrow edema for 2 years in patients with degenerative arthritis whose symptoms have waned. Bone marrow edema may be associated with pain but may be absent or inconsequential in the presence of pain.
Because fluid-sensitive T2-weighted MRI is exquisitely sensitive for mobile water protons (ie, in bone marrow edema), it is important that a cause for the edema-like signal be sought on the MRI scan, since this finding is nonspecific and may be associated with articular disease, trauma, osteonecrosis, infection, or bone tumors. Additionally, clinicians need to be aware that the findings on MRI depend on the quality of the study, and are influenced by technical factors such as magnet strength, imaging planes, and use of surface coils.
MRI should be used in patients in whom surgical treatment, ie, arthroscopy, is being considered. As discussed above, several studies have shown that a significant number of unnecessary arthroscopies may be prevented when preceded by an MRI examination.
Figure 5 shows the use of MRI in the evaluation of a 45-year-old man with left knee pain after a motorcycle accident.
ULTRASONOGRAPHY HAS ONLY A LIMITED ROLE
Ultrasonography does not play a major role in the evaluation of acute knee pain in the United States, in part because the accuracy of the results depend much on the technical skills and experience of the operator.
Ultrasonography can be useful in evaluating for rupture of the quadriceps and patellar tendon, or to assess a repaired tendon after surgery,15 and it is a quick and reliable way to determine the presence of joint effusion and popliteal cyst. It is also used to guide needle placement for joint aspiration and injection.
- Jackson JL, O’Malley PG, Kroenke K. Evaluation of acute knee pain in primary care. Ann Intern Med 2003; 139:575–588.
- Steill IG, Greenberg GH, Wells GA, et al. Prospective validation of a decision rule for the use of radiographs in acute knee injuries. JAMA 1996; 275:611–615.
- O’Shea KJ, Murphy DP, Heekin RD, Herzwurm PJ. The diagnostic accuracy of history, physical examination, and radiographs in the evaluation of traumatic knee disorders. Am J Sports Med 1996; 24:164–167.
- Spiers AS, Meagher T, Ostlere SJ, Wilson DJ, Dodd CA. Can MRI of the knee affect arthroscopic practice? J Bone Joint Surg 1993; 75:49–52.
- Bui-Mansfield LT, Youngberg RA, Warme W, Pitcher JD, Nguyen PL. Potential cost savings of MR imaging obtained before arthroscopy of the knee: evaluation of 50 consecutive patients. AJR Am J Roentgenol 1997; 168:913–918.
- Rangger C, Klestil T, Kathrein A, Inderster A, Hamid L. Influence of magnetic resonance imaging on indications for arthroscopy of the knee. Clin Orthop Rel Res 1996; 330:133–142.
- Mackenzie R, Dixon AK, Keene GS, Hollingsworth W, Lomas DJ, Villar RN. Magnetic resonance imaging of the knee: assessment of effectiveness. Clin Radiol 1996; 51:245–250.
- Munshi M, Davidson M, MacDonald PB, Froese W, Sutherland K. The efficacy of magnetic resonance imaging in acute knee injuries. Clin J Sport Med 2000; 10:34–39.
- Steill IG, Wells GA, Hoag RH, et al. Implementation of the Ottawa knee rule for the use of radiography in acute knee injuries. JAMA 1997; 278:2075–2079.
- Tigges S, Pitts S, Mukundan S, Morrison D, Olson M, Shahriara A. External validation of the Ottawa knee rules in an urban trauma center in the United States. AJR Am J Roentgenol 1999; 172:1069–1071.
- Claessens AA, Schouten JS, van den Ouweland FA, Valkenburg HA. Do clinical findings associate with radiographic osteoarthritis of the knee? Ann Rheum Dis 1990; 49:771–774.
- Gries PE, Bardana DE, Holmstrom MC, Burks RT. Meniscal injury: basic science and evaluation. J Am Acad Orthop Surg 2002; 10:168–176.
- Gelb HJ, Glasgow SG, Sapega AA, Torg JS. Magnetic resonance imaging of knee disorders. Clinical value and cost-effectiveness in a sports medicine practice. Am J Sports Med 1996; 24:99–103.
- Beattie KA, Boulos P, Pui M, et al. Abnormalities identified in the knees of asymptomatic volunteers using peripheral magnetic resonance imaging. Osteoarthritis Cartilage 2005; 13:181–186.
- Ilan DI, Tejwani N, Keschner M, Leibman M. Quadriceps tendon rupture. J Am Acad Orthop Surg 2003; 11:192–200.
Radiography plays a key role in the initial evaluation of acute knee pain in adults. Yet conflicting studies and the absence of clear guidelines may leave the primary care physician uncertain as to which imaging test to order—ie, whether radiography is sufficient, and when computed tomography (CT) or magnetic resonance imaging (MRI) is needed. This article reviews the indications for radiologic examination of the knee and discusses indications for cross-sectional imaging studies. Imaging in oncology patients is not discussed here.
ACUTE KNEE PAIN: A TYPICAL SCENARIO
A 47-year-old woman presents to the emergency department with left knee pain after a motor vehicle accident that occurred the day before. The car she was driving hit a tree, and she hit her knee on the dashboard. She was wearing a seatbelt at the time of the accident. She says she was unable to walk immediately after the accident because of knee pain.
The initial examination in the emergency room reveals swelling and pain throughout the range of motion. The anterior drawer test and the Lachman test are negative (see below).
The patient is discharged home with a knee immobilizer, pain medication, and crutches, with instructions for a follow-up visit in the orthopedics clinic.
Five days later, she returns to the emergency department complaining of continuing knee pain. She says the knee gives way when she puts weight on it. The physical findings are unchanged, and she is discharged home with a follow-up appointment with orthopedics in 3 days.
At the follow-up visit, she complains of persistent knee pain in the medial aspect of the knee joint. Physical examination is difficult because of pain and swelling, and it reveals mild joint effusion with no gross instability. She has pain on the medial side with valgus stress, but there appears to be a hard end point. There is no posterior sag, and the Lachman test is negative.
Based on the physical examination and the patient’s complaints, she receives a diagnosis of medial collateral ligament strain and injury. She is given a hinged brace and is instructed to undergo a physical rehabilitation program.
Three weeks after the initial evaluation, she returns to the orthopedics clinic with continuing knee problems. Mild knee effusion persists, but she has less pain and swelling, allowing a more complete examination. The examination reveals less limitation of range of motion and a hint of positivity on the Lachman test. The knee is diffusely tender, and the pain seems out of proportion with the maneuvers used during the examination. She requests more pain medication. You suspect internal derangement of the knee. Which imaging test should you order to further evaluate this patient?
A SYSTEMATIC AND COST-EFFECTIVE APPROACH IS NEEDED
The case presented above represents a typical scenario for the presentation of acute knee pain and illustrates the diagnostic challenges.
Knee pain is a common reason for emergency room visits, and it accounts for approximately 1.9 million visits to primary care clinics annually.1 In the emergency department, most patients undergo plain radiography to assess for fracture, yet approximately 92% of radiographic studies do not show a fracture.2 Clearly, the evaluation of knee pain requires a systematic, accurate, and cost-effective approach.
Key elements of the physical examination
In acute knee pain, accurate diagnosis begins with a detailed history and physical examination.
The anterior drawer test is done to evaluate the anterior cruciate ligament. With the relaxed knee flexed to approximately 80° and the foot stabilized in a neutral position, the examiner grasps the proximal tibia in a firm yet gentle grip, and then applies anterior force, noting the degree of anterior displacement compared with the other knee.
The Lachman test, a variation of the anterior drawer test, is more definitive for the anterior cruciate ligament and is carried out with the knee in 15° of flexion and external rotation, in order to relax the iliotibial band. The upper hand grasps the distal thigh, and the lower hand, with the thumb on the tibial tubercle, pulls the tibia forward. The degree of anterior motion in millimeters is noted and compared with that on the other side, and the end point is graded as “soft” or “hard.” An end point is considered hard when a ligament abruptly halts the motion of the bone being tested against the stabilized bone. An end point is considered soft when the ligament is disrupted and the restraints are the more elastic secondary stabilizers.
Debate continues
Some authors contend that in skilled hands a thorough history, physical examination, and radiographic examination are sufficient to diagnose trauma-related intra-articular knee disorders.3 Others contend that MRI plays a key role in the initial evaluation. A number of studies4–8 have shown that using MRI in the initial evaluation not only identifies key lesions, but also may eliminate the need for an invasive diagnostic procedure (ie, arthroscopy).
For example, MRI can reveal fracture, stress fracture, insufficiency fracture, and transient patellar dislocation—conditions that may satisfactorily explain knee symptoms.
PLAIN RADIOGRAPHY STILL THE FIRST STEP IN KNEE EVALUATION
Radiography is the first step in the evaluation of knee pain. It is quick and inexpensive and can yield many diagnostic clues. It can readily reveal fractures, osteochondral defects, bony lesions, joint effusions, joint space narrowing, and bone misalignment.
In patients with knee trauma, supine anteroposterior and cross-table lateral radiographic images are generally obtained. In patients whose knee pain is not due to trauma, standing projections are done, as well as dedicated projection of the patellofemoral articulation. A standing series is most helpful for evaluating joint space and alignment.
Applying the Ottawa rules
When a patient presents to the emergency room with acute knee pain, the immediate concern is whether he or she has a fracture. The Ottawa knee rules9 for when to order radiography in adults with knee pain are highly sensitive for detecting a clinically important fracture. If any one of the five Ottawa criteria applies—ie, the patient is age 55 or older, has tenderness at the head of the fibula, has patellar tenderness, is unable to flex the knee to 90°, or is unable to bear weight—then radiography is indicated.
While studies have validated the ability of the Ottawa rules to detect important fractures in acute knee injury,2,10 fracture is the cause of only a small percentage of knee complaints in the primary care setting. More common causes include osteoarthritis, meniscal injury, ligamental injury, and crystal arthropathy, and these account for approximately half of all diagnoses. Sprain and strain account for most of the rest of knee injuries.1
Acute exacerbations of osteoarthritis
Osteoarthritis is a chronic problem, yet it is not unusual for a patient to present to the primary care physician with an acute exacerbation of joint pain. The clinical hallmarks include age over 50, stiffness lasting less than 30 minutes, bony enlargement and tenderness, and crepitus. The radiographic hallmarks, according to the Kellgren-Lawrence grading scale, are joint space narrowing, osteophytes, subchondral cysts, and sclerosis. These radiographic findings correlate well with clinical findings in these patients.11
Situations in which radiography is less helpful
In some cases the radiographic findings may not explain the patient’s clinical signs and symptoms. For example, in suspected crystalline and septic arthritis, the clinical presentation may include warmth, erythema, and effusion. Arthrocentesis would be indicated in such a patient. Indeed, in the case of suspected pseudogout, chondrocalcinosis may be radiographically evident. However, it is also present in many patients without symptoms or with osteoarthritis, so radiographic evidence does not provide a definite diagnosis.
While radiography may not always identify the cause of knee pain, it is useful in excluding serious problems such as fractures, advanced degenerative changes, and neoplasms, and it may help direct further management. Radiography is not useful in the evaluation of the cruciate and collateral ligaments, the menisci, and the hyaline cartilage of the knee and may fail to show an insufficiency or stress fracture. To evaluate these structures and associated soft tissues, MRI is preferable.
COMPUTED TOMOGRAPHY IN ACUTE KNEE PAIN
CURRENT USES OF MRI TO EVALUATE ACUTE KNEE PAIN
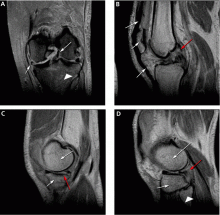
As mentioned above, MRI is useful in evaluating suspected meniscal and ligamentous injuries.
Figure 3 shows how T2-weighted MRI was used to evaluate for suspected meniscal injury in our 47-year-old female patient with left knee pain after a motor vehicle accident.
Still a matter of debate
MRI’s role in the diagnosis of knee pain is still a contentious issue.
Advantages of MRI are that it is noninvasive, it does not use ionizing radiation, it gives multiplanar images, and it provides images of soft-tissue structures, which other imaging methods cannot.12 It is a well-proven and widely accepted test. Its sensitivity for detecting meniscal and cruciate ligament injury ranges from 75% to 88%,1 and it can help in the evaluation of other injuries for which radiography is not useful, including synovitis, bone bruise, stress or insufficiency fracture, osteochondral defects, and osteonecrosis.
In addition, several studies show that using MRI to establish the diagnosis in acute knee pain can mean that 22% to 42% fewer arthroscopic procedures need to be performed.4–8 Authors of a prospective double-blind study8 recommended that MRI be used in patients with acute knee injury when the findings of the clinical history and examination by orthopedic surgeons prove equivocal.8 MRI evaluation is especially desirable for young, active patients who wish to resume activity as soon as possible.
A routine MRI examination consists of T1- and T2-weighted images in three planes, although the number of sequences and planes varies from hospital to hospital. The use of gadolinium contrast is indicated only when osteomyelitis, septic arthritis, or a mass is suspected.
Disadvantages of MRI include its cost: Medicare reimbursement for knee MRI is around $400, compared with $200 for knee CT and $50 for knee radiography with four views. Also, while studies have shown MRI to have a high sensitivity and specificity in the diagnosis of acute knee injury, some have reported a high false-positive rate for the detection of meniscal tear.13,14 MRI has also been shown to have a lower sensitivity than arthroscopy for lesions of the articular cartilage.13 Furthermore, MRI has been shown to reveal cartilage lesions, osteophytes, and meniscal abnormalities in asymptomatic study volunteers with no history of pain, trauma or knee disease.14 Therefore, findings on MRI must closely correlate with findings on the history and physical examination.
Additional indications for knee MRI
Cartilage can be assessed on routine MRI sequences of the knee. Since closed MRI systems have more powerful magnets than open systems, closed MRI systems provide greater anatomic detail.
MRI can identify other lesions, such as spontaneous osteonecrosis of the knee, usually seen in elderly women who may present with sudden knee pain. In such patients, MRI findings of focal replacement of the bone marrow and surrounding edema are specific for osteonecrosis.
Opinions vary as to whether bone marrow edema is always associated with pain. Sequential MRI studies have shown persistence of bone marrow edema for 2 years in patients with degenerative arthritis whose symptoms have waned. Bone marrow edema may be associated with pain but may be absent or inconsequential in the presence of pain.
Because fluid-sensitive T2-weighted MRI is exquisitely sensitive for mobile water protons (ie, in bone marrow edema), it is important that a cause for the edema-like signal be sought on the MRI scan, since this finding is nonspecific and may be associated with articular disease, trauma, osteonecrosis, infection, or bone tumors. Additionally, clinicians need to be aware that the findings on MRI depend on the quality of the study, and are influenced by technical factors such as magnet strength, imaging planes, and use of surface coils.
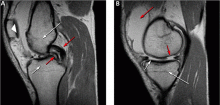
MRI should be used in patients in whom surgical treatment, ie, arthroscopy, is being considered. As discussed above, several studies have shown that a significant number of unnecessary arthroscopies may be prevented when preceded by an MRI examination.
Figure 5 shows the use of MRI in the evaluation of a 45-year-old man with left knee pain after a motorcycle accident.
ULTRASONOGRAPHY HAS ONLY A LIMITED ROLE
Ultrasonography does not play a major role in the evaluation of acute knee pain in the United States, in part because the accuracy of the results depend much on the technical skills and experience of the operator.
Ultrasonography can be useful in evaluating for rupture of the quadriceps and patellar tendon, or to assess a repaired tendon after surgery,15 and it is a quick and reliable way to determine the presence of joint effusion and popliteal cyst. It is also used to guide needle placement for joint aspiration and injection.
Radiography plays a key role in the initial evaluation of acute knee pain in adults. Yet conflicting studies and the absence of clear guidelines may leave the primary care physician uncertain as to which imaging test to order—ie, whether radiography is sufficient, and when computed tomography (CT) or magnetic resonance imaging (MRI) is needed. This article reviews the indications for radiologic examination of the knee and discusses indications for cross-sectional imaging studies. Imaging in oncology patients is not discussed here.
ACUTE KNEE PAIN: A TYPICAL SCENARIO
A 47-year-old woman presents to the emergency department with left knee pain after a motor vehicle accident that occurred the day before. The car she was driving hit a tree, and she hit her knee on the dashboard. She was wearing a seatbelt at the time of the accident. She says she was unable to walk immediately after the accident because of knee pain.
The initial examination in the emergency room reveals swelling and pain throughout the range of motion. The anterior drawer test and the Lachman test are negative (see below).
The patient is discharged home with a knee immobilizer, pain medication, and crutches, with instructions for a follow-up visit in the orthopedics clinic.
Five days later, she returns to the emergency department complaining of continuing knee pain. She says the knee gives way when she puts weight on it. The physical findings are unchanged, and she is discharged home with a follow-up appointment with orthopedics in 3 days.
At the follow-up visit, she complains of persistent knee pain in the medial aspect of the knee joint. Physical examination is difficult because of pain and swelling, and it reveals mild joint effusion with no gross instability. She has pain on the medial side with valgus stress, but there appears to be a hard end point. There is no posterior sag, and the Lachman test is negative.
Based on the physical examination and the patient’s complaints, she receives a diagnosis of medial collateral ligament strain and injury. She is given a hinged brace and is instructed to undergo a physical rehabilitation program.
Three weeks after the initial evaluation, she returns to the orthopedics clinic with continuing knee problems. Mild knee effusion persists, but she has less pain and swelling, allowing a more complete examination. The examination reveals less limitation of range of motion and a hint of positivity on the Lachman test. The knee is diffusely tender, and the pain seems out of proportion with the maneuvers used during the examination. She requests more pain medication. You suspect internal derangement of the knee. Which imaging test should you order to further evaluate this patient?
A SYSTEMATIC AND COST-EFFECTIVE APPROACH IS NEEDED
The case presented above represents a typical scenario for the presentation of acute knee pain and illustrates the diagnostic challenges.
Knee pain is a common reason for emergency room visits, and it accounts for approximately 1.9 million visits to primary care clinics annually.1 In the emergency department, most patients undergo plain radiography to assess for fracture, yet approximately 92% of radiographic studies do not show a fracture.2 Clearly, the evaluation of knee pain requires a systematic, accurate, and cost-effective approach.
Key elements of the physical examination
In acute knee pain, accurate diagnosis begins with a detailed history and physical examination.
The anterior drawer test is done to evaluate the anterior cruciate ligament. With the relaxed knee flexed to approximately 80° and the foot stabilized in a neutral position, the examiner grasps the proximal tibia in a firm yet gentle grip, and then applies anterior force, noting the degree of anterior displacement compared with the other knee.
The Lachman test, a variation of the anterior drawer test, is more definitive for the anterior cruciate ligament and is carried out with the knee in 15° of flexion and external rotation, in order to relax the iliotibial band. The upper hand grasps the distal thigh, and the lower hand, with the thumb on the tibial tubercle, pulls the tibia forward. The degree of anterior motion in millimeters is noted and compared with that on the other side, and the end point is graded as “soft” or “hard.” An end point is considered hard when a ligament abruptly halts the motion of the bone being tested against the stabilized bone. An end point is considered soft when the ligament is disrupted and the restraints are the more elastic secondary stabilizers.
Debate continues
Some authors contend that in skilled hands a thorough history, physical examination, and radiographic examination are sufficient to diagnose trauma-related intra-articular knee disorders.3 Others contend that MRI plays a key role in the initial evaluation. A number of studies4–8 have shown that using MRI in the initial evaluation not only identifies key lesions, but also may eliminate the need for an invasive diagnostic procedure (ie, arthroscopy).
For example, MRI can reveal fracture, stress fracture, insufficiency fracture, and transient patellar dislocation—conditions that may satisfactorily explain knee symptoms.
PLAIN RADIOGRAPHY STILL THE FIRST STEP IN KNEE EVALUATION
Radiography is the first step in the evaluation of knee pain. It is quick and inexpensive and can yield many diagnostic clues. It can readily reveal fractures, osteochondral defects, bony lesions, joint effusions, joint space narrowing, and bone misalignment.
In patients with knee trauma, supine anteroposterior and cross-table lateral radiographic images are generally obtained. In patients whose knee pain is not due to trauma, standing projections are done, as well as dedicated projection of the patellofemoral articulation. A standing series is most helpful for evaluating joint space and alignment.
Applying the Ottawa rules
When a patient presents to the emergency room with acute knee pain, the immediate concern is whether he or she has a fracture. The Ottawa knee rules9 for when to order radiography in adults with knee pain are highly sensitive for detecting a clinically important fracture. If any one of the five Ottawa criteria applies—ie, the patient is age 55 or older, has tenderness at the head of the fibula, has patellar tenderness, is unable to flex the knee to 90°, or is unable to bear weight—then radiography is indicated.
While studies have validated the ability of the Ottawa rules to detect important fractures in acute knee injury,2,10 fracture is the cause of only a small percentage of knee complaints in the primary care setting. More common causes include osteoarthritis, meniscal injury, ligamental injury, and crystal arthropathy, and these account for approximately half of all diagnoses. Sprain and strain account for most of the rest of knee injuries.1
Acute exacerbations of osteoarthritis
Osteoarthritis is a chronic problem, yet it is not unusual for a patient to present to the primary care physician with an acute exacerbation of joint pain. The clinical hallmarks include age over 50, stiffness lasting less than 30 minutes, bony enlargement and tenderness, and crepitus. The radiographic hallmarks, according to the Kellgren-Lawrence grading scale, are joint space narrowing, osteophytes, subchondral cysts, and sclerosis. These radiographic findings correlate well with clinical findings in these patients.11
Situations in which radiography is less helpful
In some cases the radiographic findings may not explain the patient’s clinical signs and symptoms. For example, in suspected crystalline and septic arthritis, the clinical presentation may include warmth, erythema, and effusion. Arthrocentesis would be indicated in such a patient. Indeed, in the case of suspected pseudogout, chondrocalcinosis may be radiographically evident. However, it is also present in many patients without symptoms or with osteoarthritis, so radiographic evidence does not provide a definite diagnosis.
While radiography may not always identify the cause of knee pain, it is useful in excluding serious problems such as fractures, advanced degenerative changes, and neoplasms, and it may help direct further management. Radiography is not useful in the evaluation of the cruciate and collateral ligaments, the menisci, and the hyaline cartilage of the knee and may fail to show an insufficiency or stress fracture. To evaluate these structures and associated soft tissues, MRI is preferable.
COMPUTED TOMOGRAPHY IN ACUTE KNEE PAIN
CURRENT USES OF MRI TO EVALUATE ACUTE KNEE PAIN
As mentioned above, MRI is useful in evaluating suspected meniscal and ligamentous injuries.
Figure 3 shows how T2-weighted MRI was used to evaluate for suspected meniscal injury in our 47-year-old female patient with left knee pain after a motor vehicle accident.
Still a matter of debate
MRI’s role in the diagnosis of knee pain is still a contentious issue.
Advantages of MRI are that it is noninvasive, it does not use ionizing radiation, it gives multiplanar images, and it provides images of soft-tissue structures, which other imaging methods cannot.12 It is a well-proven and widely accepted test. Its sensitivity for detecting meniscal and cruciate ligament injury ranges from 75% to 88%,1 and it can help in the evaluation of other injuries for which radiography is not useful, including synovitis, bone bruise, stress or insufficiency fracture, osteochondral defects, and osteonecrosis.
In addition, several studies show that using MRI to establish the diagnosis in acute knee pain can mean that 22% to 42% fewer arthroscopic procedures need to be performed.4–8 Authors of a prospective double-blind study8 recommended that MRI be used in patients with acute knee injury when the findings of the clinical history and examination by orthopedic surgeons prove equivocal.8 MRI evaluation is especially desirable for young, active patients who wish to resume activity as soon as possible.
A routine MRI examination consists of T1- and T2-weighted images in three planes, although the number of sequences and planes varies from hospital to hospital. The use of gadolinium contrast is indicated only when osteomyelitis, septic arthritis, or a mass is suspected.
Disadvantages of MRI include its cost: Medicare reimbursement for knee MRI is around $400, compared with $200 for knee CT and $50 for knee radiography with four views. Also, while studies have shown MRI to have a high sensitivity and specificity in the diagnosis of acute knee injury, some have reported a high false-positive rate for the detection of meniscal tear.13,14 MRI has also been shown to have a lower sensitivity than arthroscopy for lesions of the articular cartilage.13 Furthermore, MRI has been shown to reveal cartilage lesions, osteophytes, and meniscal abnormalities in asymptomatic study volunteers with no history of pain, trauma or knee disease.14 Therefore, findings on MRI must closely correlate with findings on the history and physical examination.
Additional indications for knee MRI
Cartilage can be assessed on routine MRI sequences of the knee. Since closed MRI systems have more powerful magnets than open systems, closed MRI systems provide greater anatomic detail.
MRI can identify other lesions, such as spontaneous osteonecrosis of the knee, usually seen in elderly women who may present with sudden knee pain. In such patients, MRI findings of focal replacement of the bone marrow and surrounding edema are specific for osteonecrosis.
Opinions vary as to whether bone marrow edema is always associated with pain. Sequential MRI studies have shown persistence of bone marrow edema for 2 years in patients with degenerative arthritis whose symptoms have waned. Bone marrow edema may be associated with pain but may be absent or inconsequential in the presence of pain.
Because fluid-sensitive T2-weighted MRI is exquisitely sensitive for mobile water protons (ie, in bone marrow edema), it is important that a cause for the edema-like signal be sought on the MRI scan, since this finding is nonspecific and may be associated with articular disease, trauma, osteonecrosis, infection, or bone tumors. Additionally, clinicians need to be aware that the findings on MRI depend on the quality of the study, and are influenced by technical factors such as magnet strength, imaging planes, and use of surface coils.
MRI should be used in patients in whom surgical treatment, ie, arthroscopy, is being considered. As discussed above, several studies have shown that a significant number of unnecessary arthroscopies may be prevented when preceded by an MRI examination.
Figure 5 shows the use of MRI in the evaluation of a 45-year-old man with left knee pain after a motorcycle accident.
ULTRASONOGRAPHY HAS ONLY A LIMITED ROLE
Ultrasonography does not play a major role in the evaluation of acute knee pain in the United States, in part because the accuracy of the results depend much on the technical skills and experience of the operator.
Ultrasonography can be useful in evaluating for rupture of the quadriceps and patellar tendon, or to assess a repaired tendon after surgery,15 and it is a quick and reliable way to determine the presence of joint effusion and popliteal cyst. It is also used to guide needle placement for joint aspiration and injection.
- Jackson JL, O’Malley PG, Kroenke K. Evaluation of acute knee pain in primary care. Ann Intern Med 2003; 139:575–588.
- Steill IG, Greenberg GH, Wells GA, et al. Prospective validation of a decision rule for the use of radiographs in acute knee injuries. JAMA 1996; 275:611–615.
- O’Shea KJ, Murphy DP, Heekin RD, Herzwurm PJ. The diagnostic accuracy of history, physical examination, and radiographs in the evaluation of traumatic knee disorders. Am J Sports Med 1996; 24:164–167.
- Spiers AS, Meagher T, Ostlere SJ, Wilson DJ, Dodd CA. Can MRI of the knee affect arthroscopic practice? J Bone Joint Surg 1993; 75:49–52.
- Bui-Mansfield LT, Youngberg RA, Warme W, Pitcher JD, Nguyen PL. Potential cost savings of MR imaging obtained before arthroscopy of the knee: evaluation of 50 consecutive patients. AJR Am J Roentgenol 1997; 168:913–918.
- Rangger C, Klestil T, Kathrein A, Inderster A, Hamid L. Influence of magnetic resonance imaging on indications for arthroscopy of the knee. Clin Orthop Rel Res 1996; 330:133–142.
- Mackenzie R, Dixon AK, Keene GS, Hollingsworth W, Lomas DJ, Villar RN. Magnetic resonance imaging of the knee: assessment of effectiveness. Clin Radiol 1996; 51:245–250.
- Munshi M, Davidson M, MacDonald PB, Froese W, Sutherland K. The efficacy of magnetic resonance imaging in acute knee injuries. Clin J Sport Med 2000; 10:34–39.
- Steill IG, Wells GA, Hoag RH, et al. Implementation of the Ottawa knee rule for the use of radiography in acute knee injuries. JAMA 1997; 278:2075–2079.
- Tigges S, Pitts S, Mukundan S, Morrison D, Olson M, Shahriara A. External validation of the Ottawa knee rules in an urban trauma center in the United States. AJR Am J Roentgenol 1999; 172:1069–1071.
- Claessens AA, Schouten JS, van den Ouweland FA, Valkenburg HA. Do clinical findings associate with radiographic osteoarthritis of the knee? Ann Rheum Dis 1990; 49:771–774.
- Gries PE, Bardana DE, Holmstrom MC, Burks RT. Meniscal injury: basic science and evaluation. J Am Acad Orthop Surg 2002; 10:168–176.
- Gelb HJ, Glasgow SG, Sapega AA, Torg JS. Magnetic resonance imaging of knee disorders. Clinical value and cost-effectiveness in a sports medicine practice. Am J Sports Med 1996; 24:99–103.
- Beattie KA, Boulos P, Pui M, et al. Abnormalities identified in the knees of asymptomatic volunteers using peripheral magnetic resonance imaging. Osteoarthritis Cartilage 2005; 13:181–186.
- Ilan DI, Tejwani N, Keschner M, Leibman M. Quadriceps tendon rupture. J Am Acad Orthop Surg 2003; 11:192–200.
- Jackson JL, O’Malley PG, Kroenke K. Evaluation of acute knee pain in primary care. Ann Intern Med 2003; 139:575–588.
- Steill IG, Greenberg GH, Wells GA, et al. Prospective validation of a decision rule for the use of radiographs in acute knee injuries. JAMA 1996; 275:611–615.
- O’Shea KJ, Murphy DP, Heekin RD, Herzwurm PJ. The diagnostic accuracy of history, physical examination, and radiographs in the evaluation of traumatic knee disorders. Am J Sports Med 1996; 24:164–167.
- Spiers AS, Meagher T, Ostlere SJ, Wilson DJ, Dodd CA. Can MRI of the knee affect arthroscopic practice? J Bone Joint Surg 1993; 75:49–52.
- Bui-Mansfield LT, Youngberg RA, Warme W, Pitcher JD, Nguyen PL. Potential cost savings of MR imaging obtained before arthroscopy of the knee: evaluation of 50 consecutive patients. AJR Am J Roentgenol 1997; 168:913–918.
- Rangger C, Klestil T, Kathrein A, Inderster A, Hamid L. Influence of magnetic resonance imaging on indications for arthroscopy of the knee. Clin Orthop Rel Res 1996; 330:133–142.
- Mackenzie R, Dixon AK, Keene GS, Hollingsworth W, Lomas DJ, Villar RN. Magnetic resonance imaging of the knee: assessment of effectiveness. Clin Radiol 1996; 51:245–250.
- Munshi M, Davidson M, MacDonald PB, Froese W, Sutherland K. The efficacy of magnetic resonance imaging in acute knee injuries. Clin J Sport Med 2000; 10:34–39.
- Steill IG, Wells GA, Hoag RH, et al. Implementation of the Ottawa knee rule for the use of radiography in acute knee injuries. JAMA 1997; 278:2075–2079.
- Tigges S, Pitts S, Mukundan S, Morrison D, Olson M, Shahriara A. External validation of the Ottawa knee rules in an urban trauma center in the United States. AJR Am J Roentgenol 1999; 172:1069–1071.
- Claessens AA, Schouten JS, van den Ouweland FA, Valkenburg HA. Do clinical findings associate with radiographic osteoarthritis of the knee? Ann Rheum Dis 1990; 49:771–774.
- Gries PE, Bardana DE, Holmstrom MC, Burks RT. Meniscal injury: basic science and evaluation. J Am Acad Orthop Surg 2002; 10:168–176.
- Gelb HJ, Glasgow SG, Sapega AA, Torg JS. Magnetic resonance imaging of knee disorders. Clinical value and cost-effectiveness in a sports medicine practice. Am J Sports Med 1996; 24:99–103.
- Beattie KA, Boulos P, Pui M, et al. Abnormalities identified in the knees of asymptomatic volunteers using peripheral magnetic resonance imaging. Osteoarthritis Cartilage 2005; 13:181–186.
- Ilan DI, Tejwani N, Keschner M, Leibman M. Quadriceps tendon rupture. J Am Acad Orthop Surg 2003; 11:192–200.
KEY POINTS
- In the emergency department, most patients undergo plain radiography to assess for fracture, yet more than 90% of these studies do not show a fracture.
- CT is useful in patients with knee trauma but normal radiographs.
- MRI is the imaging modality for internal derangement of the knee.
- Ultrasonography’s role in the evaluation of acute knee pain is generally limited to assessment of the extensor mechanism, joint effusion, and popliteal cyst.