User login
Immediate or delayed pushing in the second stage of labor?
ILLUSTRATIVE CASE
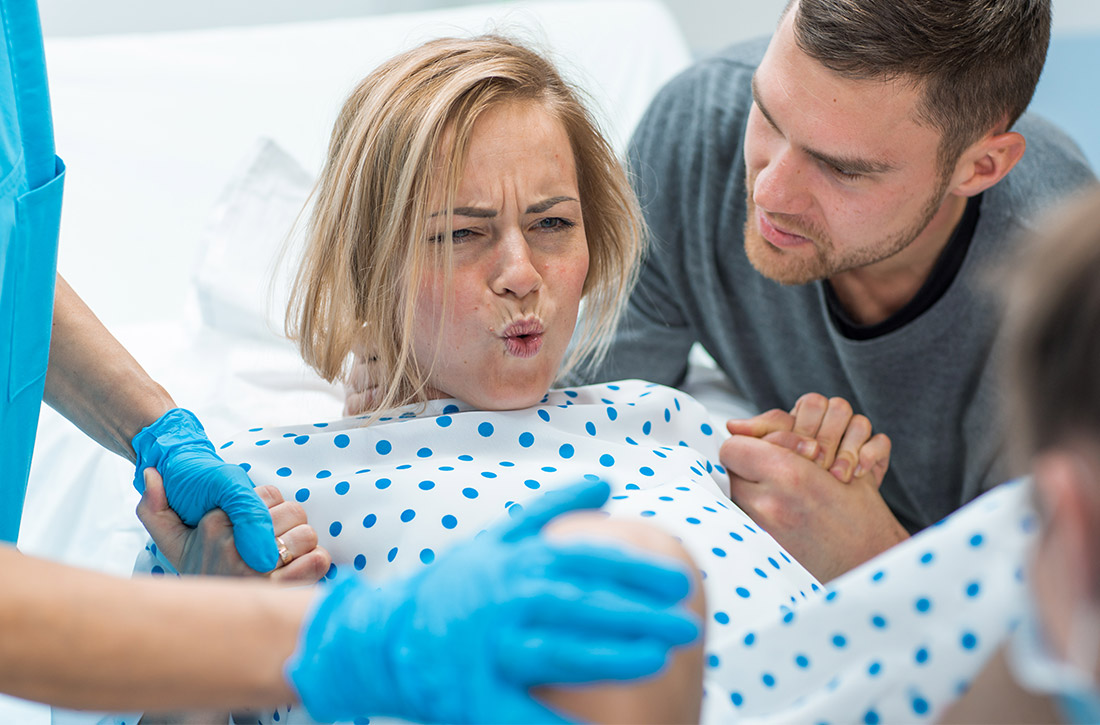
A 27-year-old G1P000 at term with an uncomplicated pregnancy has been laboring for 6 hours with an epidural in place and a reassuring fetal heart tracing. She is at –2 station with complete cervical dilation and effacement. Should she push now or delay pushing to allow for more descent?
More than 10,000 women give birth each day in the United States, yet few of our approaches to labor management are evidence based.2 For example, there are no clear guidelines on whether immediate pushing or delayed pushing (waiting 1-2 hours) in the second stage of labor (the time from complete cervical dilation to delivery of the fetus) leads to better outcomes.
A recent Cochrane review, which included very low- to moderate-quality trials of nulliparous and multiparous women using epidural analgesia showed that delayed pushing resulted in more vaginal deliveries, longer duration of second stage of labor, and shorter duration of pushing.3 But many of the trials included in this Cochrane review were noted to have study design limitations and significant heterogeneity.
A recent retrospective study found that delayed pushing resulted in longer duration of pushing and increased risks for cesarean section, operative vaginal delivery, and postpartum hemorrhage in nulliparous patients with and without epidurals.4 The World Health Organization recommends delayed pushing in women with epidural analgesia if time and fetal monitoring resources are available.5
STUDY SUMMARY
Does the timing of second stage pushing efforts affect outcomes?
This multicenter randomized controlled trial (RCT) evaluated the effect on spontaneous vaginal delivery of delayed pushing vs immediate pushing in 2404 term nulliparous women using epidural analgesia.1 Patients were ≥ 37 weeks’ gestation. Once patients achieved 10 cm of cervical dilation, they were randomized in a 1:1 ratio to either immediate pushing or to delayed (for 60 minutes) pushing (unless there was an irresistible urge to push or they were otherwise instructed by their provider).
Outcome and results. The primary outcome was spontaneous vaginal delivery without the use of any operative support. The mean time to pushing after complete cervical dilation was 19 minutes in the immediate pushing group and 60 minutes in the delayed group. There was no difference in the rate of spontaneous vaginal delivery between the immediate and delayed pushing groups (86% vs 87%, respectively; P = .67). The immediate pushing group had a shorter duration of second stage of labor (102 minutes vs 134 minutes; mean difference [MD] = –32 minutes; 95% confidence interval [CI], –37 to –27; P < .001) and a slightly longer duration of active pushing (84 minutes vs 75 minutes; MD = 9.2 minutes; 95% CI, 6-13; P < .001).
There was no significant difference in operative vaginal or cesarean deliveries. Postpartum hemorrhage was lower in the immediate pushing group (2.3% vs 4%; risk ratio [RR] = 0.6; 95% CI, 0.3-0.9; P = .03; number needed to treat [NNT] = 58), as was chorioamnionitis (6.7% vs 9.1%; RR = 0.7; 95% CI, 0.66-0.90; P = .005; NNT = 40). There was no significant difference in neonatal morbidity between groups. And in subgroup analysis, there was no significant difference in rates of vaginal delivery based on fetal position (occiput anterior, posterior, or transverse) or station (defined as high [< 2 cm] or low [≥ 2 cm]) between groups. Recruitment was stopped early at 75% because there was no difference in the primary outcome and there was concern regarding an increased risk of hemorrhage in the delayed pushing group.
Continue to: WHAT'S NEW
WHAT’S NEW
There’s no good reason to delay pushing
Delaying pushing once the cervix is completely dilated is not indicated, even for nulliparous women receiving epidural analgesia, as it does not decrease the rate of spontaneous vaginal delivery. It does, however, increase the length of second stage labor and the risk of postpartum hemorrhage and chorioamnionitis.
CAVEATS
Study was stopped early, and groups were unblinded
This study was stopped early, so it is not known if it was underpowered for some of the secondary outcomes. Also, it was not possible to blind the groups, so it is not clear if any bias in patient management or diagnosis resulted.
CHALLENGES TO IMPLEMENTATION
Will current practice and culture pose obstacles?
Although the overt challenges to enacting a policy of immediate pushing are minimal, the inertia of current practice and culture could affect the implementation of this strategy.
ACKNOWLEDGEMENT
The PURLs Surveillance System was supported in part by Grant Number UL1RR024999 from the National Center For Research Resources, a Clinical Translational Science Award to the University of Chicago. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center For Research Resources or the National Institutes of Health.
1. Cahill AG, Srinivas SK, Tita ATN, et al. Effect of immediate vs delayed pushing on rates of spontaneous vaginal delivery among nulliparous women receiving neuraxial analgesia: a randomized clinical trial. JAMA. 2018;320:1444-1454.
2. Hamilton BE, Martin JA, Osterman MJK, et al. Births: provisional data for 2018. Vital Statistics Rapid Release. May 2019; Report No. 007. www.cdc.gov/nchs/data/vsrr/vsrr-007-508.pdf. Accessed April 22, 2020.
3. Lemos A, Amorim MM, Domales de Andrade A, et al. Pushing/bearing down methods for the second stage of labour. Cochrane Database Syst Rev. 2017;3:CD009124.
4. Yee LM, Sandoval G, Bailit J, et al. Maternal and neonatal outcomes with early compared with delayed pushing among nulliparous women. Obstet Gynecol. 2016;128:1039-1047.
5. WHO recommendations: intrapartum care for a positive childbirth experience. Geneva: World Health Organization; 2018. www.who.int/reproductivehealth/publications/intrapartum-care-guidelines/en/. Accessed April 22, 2020.
ILLUSTRATIVE CASE
A 27-year-old G1P000 at term with an uncomplicated pregnancy has been laboring for 6 hours with an epidural in place and a reassuring fetal heart tracing. She is at –2 station with complete cervical dilation and effacement. Should she push now or delay pushing to allow for more descent?
More than 10,000 women give birth each day in the United States, yet few of our approaches to labor management are evidence based.2 For example, there are no clear guidelines on whether immediate pushing or delayed pushing (waiting 1-2 hours) in the second stage of labor (the time from complete cervical dilation to delivery of the fetus) leads to better outcomes.
A recent Cochrane review, which included very low- to moderate-quality trials of nulliparous and multiparous women using epidural analgesia showed that delayed pushing resulted in more vaginal deliveries, longer duration of second stage of labor, and shorter duration of pushing.3 But many of the trials included in this Cochrane review were noted to have study design limitations and significant heterogeneity.
A recent retrospective study found that delayed pushing resulted in longer duration of pushing and increased risks for cesarean section, operative vaginal delivery, and postpartum hemorrhage in nulliparous patients with and without epidurals.4 The World Health Organization recommends delayed pushing in women with epidural analgesia if time and fetal monitoring resources are available.5
STUDY SUMMARY
Does the timing of second stage pushing efforts affect outcomes?
This multicenter randomized controlled trial (RCT) evaluated the effect on spontaneous vaginal delivery of delayed pushing vs immediate pushing in 2404 term nulliparous women using epidural analgesia.1 Patients were ≥ 37 weeks’ gestation. Once patients achieved 10 cm of cervical dilation, they were randomized in a 1:1 ratio to either immediate pushing or to delayed (for 60 minutes) pushing (unless there was an irresistible urge to push or they were otherwise instructed by their provider).
Outcome and results. The primary outcome was spontaneous vaginal delivery without the use of any operative support. The mean time to pushing after complete cervical dilation was 19 minutes in the immediate pushing group and 60 minutes in the delayed group. There was no difference in the rate of spontaneous vaginal delivery between the immediate and delayed pushing groups (86% vs 87%, respectively; P = .67). The immediate pushing group had a shorter duration of second stage of labor (102 minutes vs 134 minutes; mean difference [MD] = –32 minutes; 95% confidence interval [CI], –37 to –27; P < .001) and a slightly longer duration of active pushing (84 minutes vs 75 minutes; MD = 9.2 minutes; 95% CI, 6-13; P < .001).
There was no significant difference in operative vaginal or cesarean deliveries. Postpartum hemorrhage was lower in the immediate pushing group (2.3% vs 4%; risk ratio [RR] = 0.6; 95% CI, 0.3-0.9; P = .03; number needed to treat [NNT] = 58), as was chorioamnionitis (6.7% vs 9.1%; RR = 0.7; 95% CI, 0.66-0.90; P = .005; NNT = 40). There was no significant difference in neonatal morbidity between groups. And in subgroup analysis, there was no significant difference in rates of vaginal delivery based on fetal position (occiput anterior, posterior, or transverse) or station (defined as high [< 2 cm] or low [≥ 2 cm]) between groups. Recruitment was stopped early at 75% because there was no difference in the primary outcome and there was concern regarding an increased risk of hemorrhage in the delayed pushing group.
Continue to: WHAT'S NEW
WHAT’S NEW
There’s no good reason to delay pushing
Delaying pushing once the cervix is completely dilated is not indicated, even for nulliparous women receiving epidural analgesia, as it does not decrease the rate of spontaneous vaginal delivery. It does, however, increase the length of second stage labor and the risk of postpartum hemorrhage and chorioamnionitis.
CAVEATS
Study was stopped early, and groups were unblinded
This study was stopped early, so it is not known if it was underpowered for some of the secondary outcomes. Also, it was not possible to blind the groups, so it is not clear if any bias in patient management or diagnosis resulted.
CHALLENGES TO IMPLEMENTATION
Will current practice and culture pose obstacles?
Although the overt challenges to enacting a policy of immediate pushing are minimal, the inertia of current practice and culture could affect the implementation of this strategy.
ACKNOWLEDGEMENT
The PURLs Surveillance System was supported in part by Grant Number UL1RR024999 from the National Center For Research Resources, a Clinical Translational Science Award to the University of Chicago. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center For Research Resources or the National Institutes of Health.
ILLUSTRATIVE CASE
A 27-year-old G1P000 at term with an uncomplicated pregnancy has been laboring for 6 hours with an epidural in place and a reassuring fetal heart tracing. She is at –2 station with complete cervical dilation and effacement. Should she push now or delay pushing to allow for more descent?
More than 10,000 women give birth each day in the United States, yet few of our approaches to labor management are evidence based.2 For example, there are no clear guidelines on whether immediate pushing or delayed pushing (waiting 1-2 hours) in the second stage of labor (the time from complete cervical dilation to delivery of the fetus) leads to better outcomes.
A recent Cochrane review, which included very low- to moderate-quality trials of nulliparous and multiparous women using epidural analgesia showed that delayed pushing resulted in more vaginal deliveries, longer duration of second stage of labor, and shorter duration of pushing.3 But many of the trials included in this Cochrane review were noted to have study design limitations and significant heterogeneity.
A recent retrospective study found that delayed pushing resulted in longer duration of pushing and increased risks for cesarean section, operative vaginal delivery, and postpartum hemorrhage in nulliparous patients with and without epidurals.4 The World Health Organization recommends delayed pushing in women with epidural analgesia if time and fetal monitoring resources are available.5
STUDY SUMMARY
Does the timing of second stage pushing efforts affect outcomes?
This multicenter randomized controlled trial (RCT) evaluated the effect on spontaneous vaginal delivery of delayed pushing vs immediate pushing in 2404 term nulliparous women using epidural analgesia.1 Patients were ≥ 37 weeks’ gestation. Once patients achieved 10 cm of cervical dilation, they were randomized in a 1:1 ratio to either immediate pushing or to delayed (for 60 minutes) pushing (unless there was an irresistible urge to push or they were otherwise instructed by their provider).
Outcome and results. The primary outcome was spontaneous vaginal delivery without the use of any operative support. The mean time to pushing after complete cervical dilation was 19 minutes in the immediate pushing group and 60 minutes in the delayed group. There was no difference in the rate of spontaneous vaginal delivery between the immediate and delayed pushing groups (86% vs 87%, respectively; P = .67). The immediate pushing group had a shorter duration of second stage of labor (102 minutes vs 134 minutes; mean difference [MD] = –32 minutes; 95% confidence interval [CI], –37 to –27; P < .001) and a slightly longer duration of active pushing (84 minutes vs 75 minutes; MD = 9.2 minutes; 95% CI, 6-13; P < .001).
There was no significant difference in operative vaginal or cesarean deliveries. Postpartum hemorrhage was lower in the immediate pushing group (2.3% vs 4%; risk ratio [RR] = 0.6; 95% CI, 0.3-0.9; P = .03; number needed to treat [NNT] = 58), as was chorioamnionitis (6.7% vs 9.1%; RR = 0.7; 95% CI, 0.66-0.90; P = .005; NNT = 40). There was no significant difference in neonatal morbidity between groups. And in subgroup analysis, there was no significant difference in rates of vaginal delivery based on fetal position (occiput anterior, posterior, or transverse) or station (defined as high [< 2 cm] or low [≥ 2 cm]) between groups. Recruitment was stopped early at 75% because there was no difference in the primary outcome and there was concern regarding an increased risk of hemorrhage in the delayed pushing group.
Continue to: WHAT'S NEW
WHAT’S NEW
There’s no good reason to delay pushing
Delaying pushing once the cervix is completely dilated is not indicated, even for nulliparous women receiving epidural analgesia, as it does not decrease the rate of spontaneous vaginal delivery. It does, however, increase the length of second stage labor and the risk of postpartum hemorrhage and chorioamnionitis.
CAVEATS
Study was stopped early, and groups were unblinded
This study was stopped early, so it is not known if it was underpowered for some of the secondary outcomes. Also, it was not possible to blind the groups, so it is not clear if any bias in patient management or diagnosis resulted.
CHALLENGES TO IMPLEMENTATION
Will current practice and culture pose obstacles?
Although the overt challenges to enacting a policy of immediate pushing are minimal, the inertia of current practice and culture could affect the implementation of this strategy.
ACKNOWLEDGEMENT
The PURLs Surveillance System was supported in part by Grant Number UL1RR024999 from the National Center For Research Resources, a Clinical Translational Science Award to the University of Chicago. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center For Research Resources or the National Institutes of Health.
1. Cahill AG, Srinivas SK, Tita ATN, et al. Effect of immediate vs delayed pushing on rates of spontaneous vaginal delivery among nulliparous women receiving neuraxial analgesia: a randomized clinical trial. JAMA. 2018;320:1444-1454.
2. Hamilton BE, Martin JA, Osterman MJK, et al. Births: provisional data for 2018. Vital Statistics Rapid Release. May 2019; Report No. 007. www.cdc.gov/nchs/data/vsrr/vsrr-007-508.pdf. Accessed April 22, 2020.
3. Lemos A, Amorim MM, Domales de Andrade A, et al. Pushing/bearing down methods for the second stage of labour. Cochrane Database Syst Rev. 2017;3:CD009124.
4. Yee LM, Sandoval G, Bailit J, et al. Maternal and neonatal outcomes with early compared with delayed pushing among nulliparous women. Obstet Gynecol. 2016;128:1039-1047.
5. WHO recommendations: intrapartum care for a positive childbirth experience. Geneva: World Health Organization; 2018. www.who.int/reproductivehealth/publications/intrapartum-care-guidelines/en/. Accessed April 22, 2020.
1. Cahill AG, Srinivas SK, Tita ATN, et al. Effect of immediate vs delayed pushing on rates of spontaneous vaginal delivery among nulliparous women receiving neuraxial analgesia: a randomized clinical trial. JAMA. 2018;320:1444-1454.
2. Hamilton BE, Martin JA, Osterman MJK, et al. Births: provisional data for 2018. Vital Statistics Rapid Release. May 2019; Report No. 007. www.cdc.gov/nchs/data/vsrr/vsrr-007-508.pdf. Accessed April 22, 2020.
3. Lemos A, Amorim MM, Domales de Andrade A, et al. Pushing/bearing down methods for the second stage of labour. Cochrane Database Syst Rev. 2017;3:CD009124.
4. Yee LM, Sandoval G, Bailit J, et al. Maternal and neonatal outcomes with early compared with delayed pushing among nulliparous women. Obstet Gynecol. 2016;128:1039-1047.
5. WHO recommendations: intrapartum care for a positive childbirth experience. Geneva: World Health Organization; 2018. www.who.int/reproductivehealth/publications/intrapartum-care-guidelines/en/. Accessed April 22, 2020.
PRACTICE CHANGER
Recommend immediate, rather than delayed, pushing in the second stage of labor for nulliparous women receiving epidural analgesia. The rate of spontaneous vaginal delivery is the same, and there is a lower risk of postpartum hemorrhage and chorioamnionitis.
STRENGTH OF RECOMMENDATION
B: Based on an individual randomized controlled trial. 1
Cahill AG, Srinivas SK, Tita ATN, et al. Effect of immediate vs delayed pushing on rates of spontaneous vaginal delivery among nulliparous women receiving neuraxial analgesia: a randomized clinical trial. JAMA. 2018;320:1444-1454.
What are the risks of long-term PPI use for GERD symptoms in patients > 65 years?
EVIDENCE SUMMARY
A 2017 meta-analysis of 16 RCTs examined the risk of cardiovascular events in 7540 adult patients taking PPIs for GERD (mean ages 45-55 years).1 The primary outcome was cardiovascular events—including acute myocardial infarction, myocardial ischemia, angina pectoris, cardiac failure, and coronary artery stenosis—and cardiac disorders.
Analysis of pooled data found that PPI use was associated with a 70% increase in cardiovascular risk (relative risk [RR] = 1.7; 95% confidence interval [CI], 1.13-2.56; number needed to harm [NNH] = 241) when compared with controls (placebo, H2 blocker, or surgery). A subgroup analysis found that PPI use for longer than 8 weeks was associated with an even higher risk of adverse cardiovascular events (6 trials, 2296 patients; RR = 2.33; 95% CI, 1.33-4.08; NNH = 67) when compared with controls. The meta-analysis wasn’t limited by heterogeneity (I2 = 0).
C difficile infection risk is higherfor PPI users
A 2016 meta-analysis of 23 observational studies (19 case-control, 4 retrospective cohort; 186,033 patients) examined the risk of hospital-acquired C difficile infections in adults prescribed PPI for any indication.2 PPI exposure varied from use at time of diagnosis or hospitalization to any use within 90 days. Of the 23 studies, 16 reported sufficient data to calculate the mean age for the patients which was 69.9 years.
The risk of C difficile infection was found to be higher with PPI use than no use (pooled odds ratio [OR] = 1.81; 95% CI, 1.52-2.14). Although a significant association was found across a large group, the results were limited by considerable heterogeneity (I2 = 82%).
Risk of community-acquired pneumonia also increases with PPI use
A 2015 systematic review and meta-analysis of 33 trials (18 case-control, 10 cohort, 4 RCTs, and 1 case-crossover study) examined the risk of CAP in adult patients prescribed PPI for any indication for durations ranging from less than 1 month to > 6 months.3 The systematic review was distilled to 26 studies because of overlapping study populations. These 26 studies included 226,769 cases of CAP among 6,351,656 patients. The primary outcome was development of CAP, the secondary outcome was hospitalization for CAP.
PPI use, compared with no use, was associated with an increased risk of developing CAP (pooled OR = 1.49; 95% CI, 1.16-1.92) and an increased risk of hospitalization for CAP (pooled OR = 1.61; 95% CI, 1.12-2.31).
In a subgroup analysis for age, patients older than 65 years were also found to have an increased risk of developing CAP with PPI use (11 trials, total number of patients not provided; OR = 1.33; 95% CI, 1.13-1.58). Despite the significant associations of PPI use with risk revealed in the primary, secondary, and subgroup analyses, the results were limited by marked heterogeneity, with an I2 > 99%.
Continue to: Hip and vertebral fracture risks associated with PPIs
Hip and vertebral fracture riskis associated with PPIs
A 2011 systematic review and meta-analysis investigated the risk of fracture in adult patients taking PPIs for any indication.4 The analysis included 10 observational studies (4 cohort, 6 case-control) with a total of 223,210 fracture cases. The authors examined the incidence of hip, vertebral, and wrist or forearm fractures.
No significant association was found between PPI use and wrist or forearm fracture (3 studies; pooled OR = 1.09; 95% CI, 0.95-1.24). A modest association was noted between PPI use and both hip fractures (9 trials; OR = 1.25; 95% CI, 1.14-1.37) and vertebral fractures (4 trials; OR = 1.5; 95% CI, 1.32-1.72).
Subgroup analysis didn’t reveal evidence of an effect of duration of PPI use on fracture. Investigators didn’t conduct subgroup analysis of different patient ages. Final results were limited by significant heterogeneity with an I2 of 86%.
RECOMMENDATIONS
A 2015 American Geriatrics Society Beers Criteria update recommends limiting PPI use because of increased risk of C difficile infections and fractures. It also recommends against using PPIs for longer than 8 weeks except for high-risk patients (such as patients taking oral corticosteroids or chronic nonsteroidal anti-inflammatory drug users), patients with Barrett’s esophagitis, or patients who need maintenance after failure of a drug discontinuation trial or H2 blockers (quality of evidence, high; SOR, strong).5
Editor’s take
1. Sun S, Cui Z, Zhou M, et al. Proton pump inhibitor monotherapy and the risk of cardiovascular events in patients with gastro-esophageal reflux disease: a meta-analysis. Neurogastroenterol Motil. 2017;29:e12926.
2. Arriola V, Tischendorf J, Musuuza J, et al. Assessing the risk of hospital-acquired clostridium difficile infection with proton pump inhibitor use: a meta-analysis. Infect Control Hosp Epidemiol. 2016;37:1408-1417.
3. Lambert AA, Lam JO, Paik JJ, et al. Risk of community-acquired pneumonia with outpatient proton-pump inhibitor therapy: a systematic review and meta-analysis. PLoS One. 2015;10:e0128004.
4. Ngamruengphong S, Leontiadis GI, Radhi S, et al. Proton pump inhibitors and risk of fracture: a systematic review and meta-analysis of observational studies. Am J Gastroenterol. 2011;106:1209-1218.
5. American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2015;63:2227-2246.
EVIDENCE SUMMARY
A 2017 meta-analysis of 16 RCTs examined the risk of cardiovascular events in 7540 adult patients taking PPIs for GERD (mean ages 45-55 years).1 The primary outcome was cardiovascular events—including acute myocardial infarction, myocardial ischemia, angina pectoris, cardiac failure, and coronary artery stenosis—and cardiac disorders.
Analysis of pooled data found that PPI use was associated with a 70% increase in cardiovascular risk (relative risk [RR] = 1.7; 95% confidence interval [CI], 1.13-2.56; number needed to harm [NNH] = 241) when compared with controls (placebo, H2 blocker, or surgery). A subgroup analysis found that PPI use for longer than 8 weeks was associated with an even higher risk of adverse cardiovascular events (6 trials, 2296 patients; RR = 2.33; 95% CI, 1.33-4.08; NNH = 67) when compared with controls. The meta-analysis wasn’t limited by heterogeneity (I2 = 0).
C difficile infection risk is higherfor PPI users
A 2016 meta-analysis of 23 observational studies (19 case-control, 4 retrospective cohort; 186,033 patients) examined the risk of hospital-acquired C difficile infections in adults prescribed PPI for any indication.2 PPI exposure varied from use at time of diagnosis or hospitalization to any use within 90 days. Of the 23 studies, 16 reported sufficient data to calculate the mean age for the patients which was 69.9 years.
The risk of C difficile infection was found to be higher with PPI use than no use (pooled odds ratio [OR] = 1.81; 95% CI, 1.52-2.14). Although a significant association was found across a large group, the results were limited by considerable heterogeneity (I2 = 82%).
Risk of community-acquired pneumonia also increases with PPI use
A 2015 systematic review and meta-analysis of 33 trials (18 case-control, 10 cohort, 4 RCTs, and 1 case-crossover study) examined the risk of CAP in adult patients prescribed PPI for any indication for durations ranging from less than 1 month to > 6 months.3 The systematic review was distilled to 26 studies because of overlapping study populations. These 26 studies included 226,769 cases of CAP among 6,351,656 patients. The primary outcome was development of CAP, the secondary outcome was hospitalization for CAP.
PPI use, compared with no use, was associated with an increased risk of developing CAP (pooled OR = 1.49; 95% CI, 1.16-1.92) and an increased risk of hospitalization for CAP (pooled OR = 1.61; 95% CI, 1.12-2.31).
In a subgroup analysis for age, patients older than 65 years were also found to have an increased risk of developing CAP with PPI use (11 trials, total number of patients not provided; OR = 1.33; 95% CI, 1.13-1.58). Despite the significant associations of PPI use with risk revealed in the primary, secondary, and subgroup analyses, the results were limited by marked heterogeneity, with an I2 > 99%.
Continue to: Hip and vertebral fracture risks associated with PPIs
Hip and vertebral fracture riskis associated with PPIs
A 2011 systematic review and meta-analysis investigated the risk of fracture in adult patients taking PPIs for any indication.4 The analysis included 10 observational studies (4 cohort, 6 case-control) with a total of 223,210 fracture cases. The authors examined the incidence of hip, vertebral, and wrist or forearm fractures.
No significant association was found between PPI use and wrist or forearm fracture (3 studies; pooled OR = 1.09; 95% CI, 0.95-1.24). A modest association was noted between PPI use and both hip fractures (9 trials; OR = 1.25; 95% CI, 1.14-1.37) and vertebral fractures (4 trials; OR = 1.5; 95% CI, 1.32-1.72).
Subgroup analysis didn’t reveal evidence of an effect of duration of PPI use on fracture. Investigators didn’t conduct subgroup analysis of different patient ages. Final results were limited by significant heterogeneity with an I2 of 86%.
RECOMMENDATIONS
A 2015 American Geriatrics Society Beers Criteria update recommends limiting PPI use because of increased risk of C difficile infections and fractures. It also recommends against using PPIs for longer than 8 weeks except for high-risk patients (such as patients taking oral corticosteroids or chronic nonsteroidal anti-inflammatory drug users), patients with Barrett’s esophagitis, or patients who need maintenance after failure of a drug discontinuation trial or H2 blockers (quality of evidence, high; SOR, strong).5
Editor’s take
EVIDENCE SUMMARY
A 2017 meta-analysis of 16 RCTs examined the risk of cardiovascular events in 7540 adult patients taking PPIs for GERD (mean ages 45-55 years).1 The primary outcome was cardiovascular events—including acute myocardial infarction, myocardial ischemia, angina pectoris, cardiac failure, and coronary artery stenosis—and cardiac disorders.
Analysis of pooled data found that PPI use was associated with a 70% increase in cardiovascular risk (relative risk [RR] = 1.7; 95% confidence interval [CI], 1.13-2.56; number needed to harm [NNH] = 241) when compared with controls (placebo, H2 blocker, or surgery). A subgroup analysis found that PPI use for longer than 8 weeks was associated with an even higher risk of adverse cardiovascular events (6 trials, 2296 patients; RR = 2.33; 95% CI, 1.33-4.08; NNH = 67) when compared with controls. The meta-analysis wasn’t limited by heterogeneity (I2 = 0).
C difficile infection risk is higherfor PPI users
A 2016 meta-analysis of 23 observational studies (19 case-control, 4 retrospective cohort; 186,033 patients) examined the risk of hospital-acquired C difficile infections in adults prescribed PPI for any indication.2 PPI exposure varied from use at time of diagnosis or hospitalization to any use within 90 days. Of the 23 studies, 16 reported sufficient data to calculate the mean age for the patients which was 69.9 years.
The risk of C difficile infection was found to be higher with PPI use than no use (pooled odds ratio [OR] = 1.81; 95% CI, 1.52-2.14). Although a significant association was found across a large group, the results were limited by considerable heterogeneity (I2 = 82%).
Risk of community-acquired pneumonia also increases with PPI use
A 2015 systematic review and meta-analysis of 33 trials (18 case-control, 10 cohort, 4 RCTs, and 1 case-crossover study) examined the risk of CAP in adult patients prescribed PPI for any indication for durations ranging from less than 1 month to > 6 months.3 The systematic review was distilled to 26 studies because of overlapping study populations. These 26 studies included 226,769 cases of CAP among 6,351,656 patients. The primary outcome was development of CAP, the secondary outcome was hospitalization for CAP.
PPI use, compared with no use, was associated with an increased risk of developing CAP (pooled OR = 1.49; 95% CI, 1.16-1.92) and an increased risk of hospitalization for CAP (pooled OR = 1.61; 95% CI, 1.12-2.31).
In a subgroup analysis for age, patients older than 65 years were also found to have an increased risk of developing CAP with PPI use (11 trials, total number of patients not provided; OR = 1.33; 95% CI, 1.13-1.58). Despite the significant associations of PPI use with risk revealed in the primary, secondary, and subgroup analyses, the results were limited by marked heterogeneity, with an I2 > 99%.
Continue to: Hip and vertebral fracture risks associated with PPIs
Hip and vertebral fracture riskis associated with PPIs
A 2011 systematic review and meta-analysis investigated the risk of fracture in adult patients taking PPIs for any indication.4 The analysis included 10 observational studies (4 cohort, 6 case-control) with a total of 223,210 fracture cases. The authors examined the incidence of hip, vertebral, and wrist or forearm fractures.
No significant association was found between PPI use and wrist or forearm fracture (3 studies; pooled OR = 1.09; 95% CI, 0.95-1.24). A modest association was noted between PPI use and both hip fractures (9 trials; OR = 1.25; 95% CI, 1.14-1.37) and vertebral fractures (4 trials; OR = 1.5; 95% CI, 1.32-1.72).
Subgroup analysis didn’t reveal evidence of an effect of duration of PPI use on fracture. Investigators didn’t conduct subgroup analysis of different patient ages. Final results were limited by significant heterogeneity with an I2 of 86%.
RECOMMENDATIONS
A 2015 American Geriatrics Society Beers Criteria update recommends limiting PPI use because of increased risk of C difficile infections and fractures. It also recommends against using PPIs for longer than 8 weeks except for high-risk patients (such as patients taking oral corticosteroids or chronic nonsteroidal anti-inflammatory drug users), patients with Barrett’s esophagitis, or patients who need maintenance after failure of a drug discontinuation trial or H2 blockers (quality of evidence, high; SOR, strong).5
Editor’s take
1. Sun S, Cui Z, Zhou M, et al. Proton pump inhibitor monotherapy and the risk of cardiovascular events in patients with gastro-esophageal reflux disease: a meta-analysis. Neurogastroenterol Motil. 2017;29:e12926.
2. Arriola V, Tischendorf J, Musuuza J, et al. Assessing the risk of hospital-acquired clostridium difficile infection with proton pump inhibitor use: a meta-analysis. Infect Control Hosp Epidemiol. 2016;37:1408-1417.
3. Lambert AA, Lam JO, Paik JJ, et al. Risk of community-acquired pneumonia with outpatient proton-pump inhibitor therapy: a systematic review and meta-analysis. PLoS One. 2015;10:e0128004.
4. Ngamruengphong S, Leontiadis GI, Radhi S, et al. Proton pump inhibitors and risk of fracture: a systematic review and meta-analysis of observational studies. Am J Gastroenterol. 2011;106:1209-1218.
5. American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2015;63:2227-2246.
1. Sun S, Cui Z, Zhou M, et al. Proton pump inhibitor monotherapy and the risk of cardiovascular events in patients with gastro-esophageal reflux disease: a meta-analysis. Neurogastroenterol Motil. 2017;29:e12926.
2. Arriola V, Tischendorf J, Musuuza J, et al. Assessing the risk of hospital-acquired clostridium difficile infection with proton pump inhibitor use: a meta-analysis. Infect Control Hosp Epidemiol. 2016;37:1408-1417.
3. Lambert AA, Lam JO, Paik JJ, et al. Risk of community-acquired pneumonia with outpatient proton-pump inhibitor therapy: a systematic review and meta-analysis. PLoS One. 2015;10:e0128004.
4. Ngamruengphong S, Leontiadis GI, Radhi S, et al. Proton pump inhibitors and risk of fracture: a systematic review and meta-analysis of observational studies. Am J Gastroenterol. 2011;106:1209-1218.
5. American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2015;63:2227-2246.
EVIDENCE-BASED ANSWER:
The use of proton pump inhibitors (PPIs) to control gastroesophageal reflux disease (GERD) is significantly associated with an increased risk of cardiovascular events such as acute myocardial infarction and myocardial ischemia, especially with treatment longer than 8 weeks (strength of recommendation [SOR]: A, systematic review of randomized, controlled trials [RCTs]). This summary is based on data extrapolated from studies on all adults because there is limited evidence that specifically addresses patients older than 65 years.
Adults taking PPIs also appear to be at increased risk of Clostridium difficile infection, community-acquired pneumonia (CAP; with use for < 30 days), and fracture (SOR: B, systematic reviews of heterogeneous prospective and retrospective observational studies).